Lumbar radiculopathy, particularly involving the L4–L5 and L5–S1 spinal levels, remains a prevalent and impactful cause of low back pain in adults under 45. This condition, resulting from nerve root irritation or compression, frequently leads to radiating pain, sensory changes, and muscle weakness that can significantly impair daily activities and quality of life. In clinical settings, managing lumbar radiculopathy effectively demands precise evaluation and classification, adherence to current evidence-based guidelines, and personalized, patient-centric care pathways.
Accurate differentiation between referred pain and true radiculopathy is essential for tailoring treatment strategies and optimizing recovery. Advances in non-invasive therapies, combined with new technologies such as spinal decompression devices, neural mobilization techniques, and state-of-the-art clinical guidelines, help clinicians provide comprehensive support to patients while minimizing unnecessary interventions. Expert evaluation, such as that offered by Dr. Sylvain Desforges—recognized for his integrative and innovative approach to spinal care—underscores the importance of combining scientific rigor with empathy and education.
This article explores the complex patterns of lumbar radiculopathy at the L4–L5 and L5–S1 segments, covering key diagnostic features, the role of advanced clinical assessment frameworks, evidence-based management approaches, and technological innovations that support effective non-surgical relief. Each section expands understanding through detailed explanations, clinical examples, and practical recommendations aimed at patients and healthcare providers alike.
Understanding Lumbar Radiculopathy: Causes and Clinical Importance
Lumbar radiculopathy occurs when nerve roots exiting the lumbar spine are compressed or irritated, typically at the L4–L5 or L5–S1 vertebral levels. The resulting neurological symptoms reflect the affected nerve roots’ anatomical pathways and functionality. This compression can arise from several structural issues:
- Intervertebral Disc Herniation: A protrusion of disc material into the spinal canal or nerve foramen, which directly impinges on nerve roots causing pain and neurological deficits.
- Foraminal or Lateral Recess Stenosis: Narrowing of the bony canals through which nerves exit, often secondary to osteoarthritis or degenerative disc changes.
- Facet Joint Hypertrophy: Enlargement of facet joints leading to reduced space and nerve compression.
- Spondylolisthesis: Forward slippage of a vertebral body causing mechanical narrowing of the nerve exit points.
The prevalence of lumbar radiculopathy underscores its clinical significance. Low back pain, with radicular symptoms, is among the leading causes of disability and healthcare resource utilization worldwide, particularly in working-age populations. For patients, the pain patterns typically indicate irritation of key nerve roots, such as the L5 or S1, which constitute major components of the sciatic nerve. Symptoms commonly manifest as sharp or burning pain radiating down the buttock and leg, extending below the knee in a dermatomal fashion consistent with nerve root anatomy.
An accurate clinical presentation is essential for avoiding misdiagnosis and guiding correct therapeutic decisions. For instance, the term “sciatica” is often broadly used but lacks precise clinical specificity and can obscure the identification of true radiculopathy involving these segments. Thus, expert evaluation using detailed neurologic examination combined with patient history remains paramount.
| Cause of Nerve Compression | Description | Impact on L4–L5 / L5–S1 |
|---|---|---|
| Disc Herniation | Protrusion of nucleus pulposus compressing nerve roots | Common at L4-L5 and L5-S1, compresses L5 and S1 roots respectively, causing dermatomal pain |
| Foraminal Stenosis | Bony narrowing of the foramen where nerves exit | Leads to chronic nerve root irritation and radicular symptoms |
| Facet Joint Hypertrophy | Degenerative enlargement of the facet joints | Contributes to narrowing of nerve pathways and pain |
| Spondylolisthesis | Anterior displacement of vertebra, often at L5-S1 | Reduces foraminal space, potentially compressing nerve roots |
Clinicians must consider these structural causes during patient evaluation, as recognizing the precise etiology directs optimal management strategies. Dr. Sylvain Desforges, with over 30 years in osteopathic and spinal care, integrates this diagnostic rigor with cutting-edge assessments to deliver personalized, scientific treatment pathways focused on recovery without unnecessary surgery.
Discerning Radiating Pain versus Referred Pain: Applying the ICF Framework
Central to managing lumbar radiculopathy is the accurate classification of pain types leveraging the International Classification of Functioning, Disability, and Health (ICF) framework. Distinguishing low back pain with referred pain from low back pain with radiating pain (radiculopathy) shapes both diagnosis and therapeutic approaches.
Characteristics of Referred Pain
Referred pain arises from tissues innervated by the spine but does not specifically follow the nerve root distribution. It often presents as:
- Pain localized to the lower back or proximal lower limb, usually above the knee.
- Absent or minimal neurological signs such as weakness or reflex changes.
- Symptoms that can be centralized—that is, decreased or moved proximally via repeated directional exercises.
Characteristics of Radiating Pain (Radiculopathy)
True radiculopathy involves nerve root irritation causing pain that radiates in a dermatomal pattern below the knee. Its features include:
- Sharp, burning, or stabbing pain along an identifiable nerve root distribution (e.g., L5 or S1 dermatome).
- Neurological findings such as sensory deficits, muscle weakness, or reflex abnormalities consistent with the affected root.
- Positive neural tension tests including the straight-leg raise (SLR), crossed SLR, or slump test which reproduce symptoms.
- Less frequent symptom centralization; symptoms might exacerbate with certain actions.
Clinicians, including Dr. Desforges, stress the importance of integrating patient history with these exam findings for proper classification, which ultimately guides intervention selection. For example, patients with referred pain often respond well to mechanical directional preference exercises, while radiculopathy sufferers may require additional neural mobilizations and graded activity plans tailored to nerve irritability levels.
| Feature | Referred Pain | Radiating Pain (Radiculopathy) |
|---|---|---|
| Pain Location | Lower back or proximal leg, above knee | Lower back and leg, below knee in dermatomal pattern |
| Neurological Signs | Typically absent or minimal | Present: sensory loss, weakness, reflex changes |
| Neural Tension Tests | Negative or non-provocative | Positive straight-leg raise, slump tests |
| Response to Repeated Movements | Centralization of pain | Symptoms often peripheralize or remain unchanged |
This detailed classification helps avoid inappropriate use of imaging or overly aggressive interventions, especially in early stages when conservative care tends to be most effective.
Diagnostic Protocols and Evaluations for L4–L5 and L5–S1 Radiculopathy
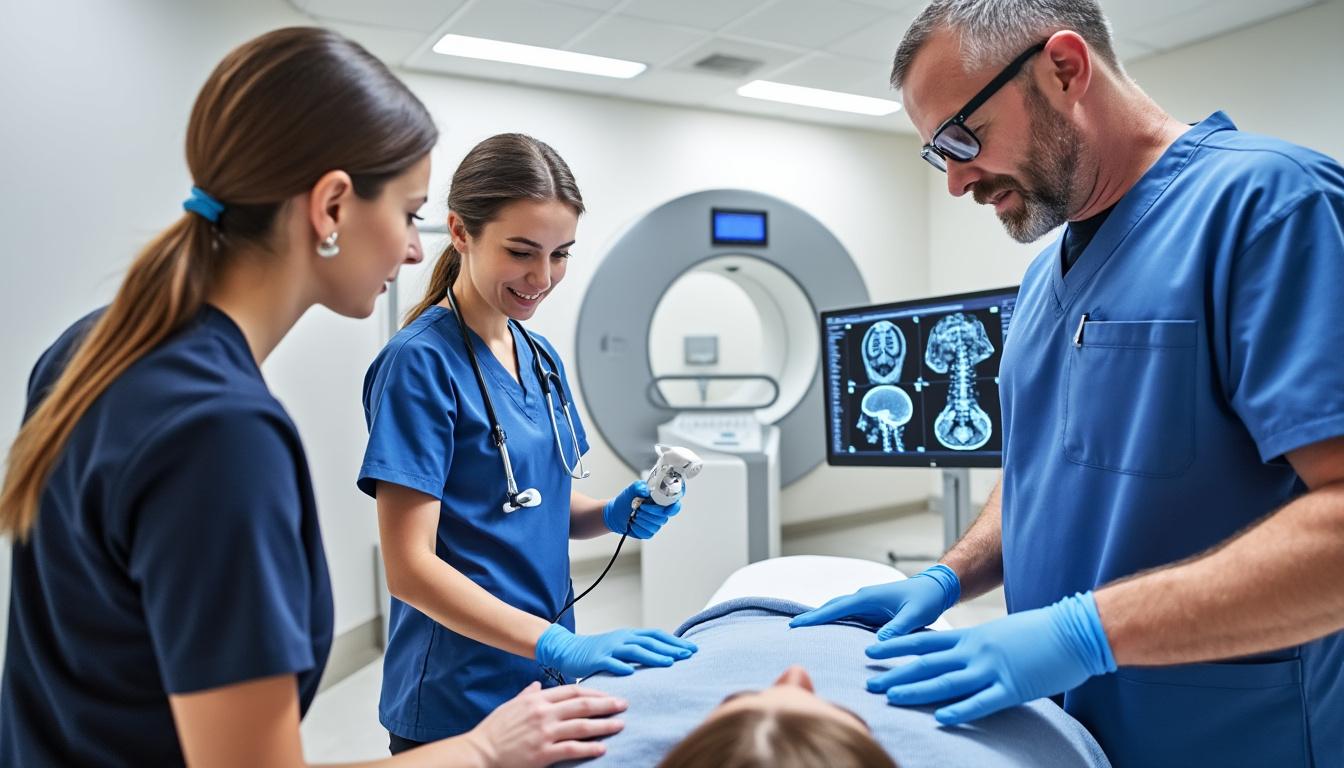
The expert evaluation of lumbar radiculopathy involves a comprehensive clinical exam, imaging when indicated, and sometimes electrodiagnostic studies to delineate nerve root involvement. Dr. Sylvain Desforges emphasizes a multidimensional approach grounded in scientific rigor and ethical care standards.
Physical Examination Essentials
- Neurological Assessment: Testing dermatomal sensory areas (e.g., medial ankle for L4, dorsum of foot for L5, lateral foot for S1).
- Muscle Strength (Myotomes): Assessing weakness such as knee extension (L4), dorsiflexion or great toe extension (L5), and plantar flexion (S1).
- Reflex Evaluation: Checking reflexes corresponding to nerve roots—patellar (L4), medial hamstring (L5), and Achilles (S1).
- Provocative Testing: Straight-leg raise (SLR) between 30°–70°, crossed SLR, and slump tests to reproduce radicular symptoms.
Imaging and Electrodiagnostics
Imaging is reserved for patients showing neurological deficits persisting over four to six weeks or those with suspected serious underlying pathology. Magnetic resonance imaging (MRI) is the modality of choice to visualize disc herniations, foraminal stenosis, or spondylolisthesis. Computed tomography (CT) and myelography are alternatives when MRI is contraindicated.
Electromyography (EMG) and nerve conduction studies may help confirm nerve root dysfunction and differentiate from peripheral neuropathies or other neuropathic conditions but are ideally performed after symptoms persist beyond two weeks for accuracy.
| Diagnostic Tool | Indication | Limitations |
|---|---|---|
| Physical Exam | Initial evaluation; detects neurological signs | Requires clinician expertise for accuracy |
| MRI | Persistent or worsening symptoms; red flag suspicion | May show incidental findings; not always correlated with symptoms |
| EMG/Nerve Conduction | Confirm nerve root involvement; differentiate mimics | Limited sensitivity if done too early |
By integrating these diagnostic modalities with a patient-centered clinical evaluation, Dr. Desforges ensures each individual receives a comprehensive assessment fostering safer and more targeted treatment plans.
Evidence-Based Treatment Strategies for Lumbar Radiculopathy at L4–L5 and L5–S1
Effective relief of lumbar radiculopathy symptoms requires a tailored approach respecting the patient’s symptom classification, acuity, and functional limitations. Clinical guidelines from recent research emphasize conservative care as the primary focus, reserving surgical intervention for select severe cases.
Non-Surgical Interventions
- Patient Education: Empowering patients with understanding about their condition reduces fear-avoidance behaviors and promotes active participation.
- Exercise Therapy:
- For referred pain: Directional preference exercises designed to centralize symptoms (e.g., prone press-ups for extension preference, knee-to-chest stretches for flexion preference).
- For radiculopathy: Graded activity, motor control exercises, and cautious neural mobilization to restore nerve and spinal function.
- For referred pain: Directional preference exercises designed to centralize symptoms (e.g., prone press-ups for extension preference, knee-to-chest stretches for flexion preference).
- For radiculopathy: Graded activity, motor control exercises, and cautious neural mobilization to restore nerve and spinal function.
- Neural Mobilization: Techniques like gentle sciatic nerve gliding can reduce neural tension and pain when applied appropriately, especially in subacute and chronic stages.
- Physical Modalities:
- Use of Biofreeze and devices such as Theragun and TENS 7000 may provide adjunctive symptom relief.
- Bracing options like DonJoy and Mueller braces may support lumbar stability during recovery phases.
- Use of Biofreeze and devices such as Theragun and TENS 7000 may provide adjunctive symptom relief.
- Bracing options like DonJoy and Mueller braces may support lumbar stability during recovery phases.
Pharmacologic and Interventional Treatments
Medications such as NSAIDs and acetaminophen support pain reduction, while gabapentin or low-dose tricyclic antidepressants can address neuropathic components. Oral corticosteroids may be considered selectively to accelerate symptom relief in acute radiculopathy, following evidence-based protocols.
When conservative care fails or if neurological deficits progress, epidural steroid injections or surgical decompression may be necessary. Criteria for surgery include refractory intractable pain, progressive weakness, or signs of cauda equina syndrome.
| Treatment Type | Indications | Benefits and Limitations |
|---|---|---|
| Exercise Therapy | All stages of referred or radiating pain | Improves function and reduces pain; requires patient adherence |
| Neural Mobilization | Subacute and chronic radiculopathy | Relieves nerve tension; must be performed cautiously |
| Pharmacologic Agents | Supportive for symptom control | Modest pain relief; potential side effects |
| Surgical Decompression | Progressive neurological deficits or intractable pain | Effective for severe cases; surgical risks apply |
Throughout the care process, adherence to personalized rehabilitation strategies that incorporate both innovative technologies—such as spinal decompression systems used at Clinique TAGMED—and patient education sets the foundation for successful outcomes, as championed by experts like Dr. Desforges.
The Role of Advanced Technologies in Managing Lumbar Radiculopathy
Technological innovation continues to transform the management of lumbar radiculopathy, especially around the levels L4–L5 and L5–S1. Dr. Sylvain Desforges is recognized for integrating such tools with clinical expertise to optimize patient outcomes.
Modern technologies that play key roles include:
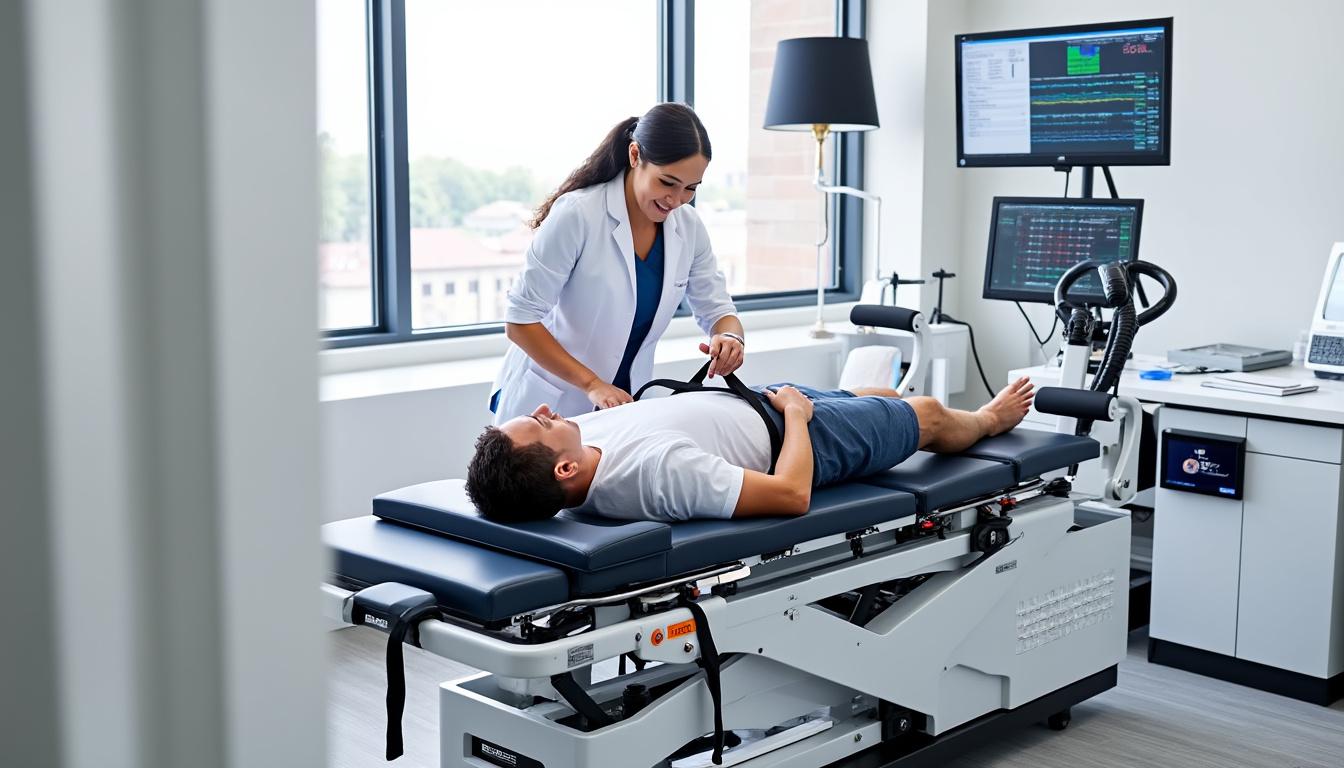
- Neurovertebral Decompression Therapy: Utilizes precision spinal decompression tables to reduce disc pressure and relieve nerve root compression non-surgically.
- Laser Therapy: Low-level laser therapy enhances tissue healing and pain reduction through photobiomodulation effects.
- Dynamic Spinal Implants: Minimally invasive devices designed to stabilize vertebral segments while preserving motion and reducing adjacent segment degeneration.
- Electrical Stimulation and Neuromodulation: Technologies like the TENS 7000 system provide targeted pain relief by modulating neural pathways.
- Advanced Bracing Devices: Brands such as DonJoy and Mueller deliver customized spinal support during recovery periods, complemented by ergonomic products like Tempur-Pedic cushions to enhance comfort.
The integration of these approaches emphasizes a patient-centered, multidisciplinary model focused on minimizing invasive procedures and improving quality of life. Each patient’s care is tailored based on detailed evaluations and evidence-based protocols, reflecting Dr. Desforges’ dedication to both innovation and safety under Quebec medical regulations.
| Technology | Function | Clinical Benefit |
|---|---|---|
| Neurovertebral Decompression | Relieves nerve compression via spinal traction | Non-surgical pain relief and functional restoration |
| Laser Therapy | Promotes tissue repair and reduces inflammation | Faster recovery and decreased pain |
| Dynamic Implants | Stabilizes spine preserving mobility | Reduces need for fusion surgery |
| TENS 7000 | Electrical nerve stimulation for analgesia | Adjunctive pain control |
| DonJoy and Mueller Bracing | Spinal support and protection | Improved patient comfort and stability |

Classification and Treatment Tailoring Based on Symptom Acuity
Symptom acuity is a pivotal factor influencing treatment strategies for lumbar radiculopathy. Understanding whether symptoms are acute, subacute, or chronic guides care intensity, patient education, and rehabilitation progression.
Stages of Symptom Acuity and Corresponding Care Principles
- Acute (Less than one month, high irritability):
- Symptoms often highly sensitive; neural mobilization generally avoided initially.
- Focus on education, gentle activity modification, and pain control.
- Bed rest limited to short durations (24-48 hours) with semi-Fowler positioning may relieve acute pain.
- Symptoms often highly sensitive; neural mobilization generally avoided initially.
- Focus on education, gentle activity modification, and pain control.
- Bed rest limited to short durations (24-48 hours) with semi-Fowler positioning may relieve acute pain.
- Subacute (Two to three months, moderate irritability):
- Incremental introduction of graded activity and gentle neural mobilization.
- Emphasis on centralization exercises and motor control.
- Close clinical monitoring for symptom changes.
- Incremental introduction of graded activity and gentle neural mobilization.
- Emphasis on centralization exercises and motor control.
- Close clinical monitoring for symptom changes.
- Chronic (More than three months, lower irritability):
- Progressive strengthening and endurance training.
- Advanced neural mobilization and functional retraining.
- Address psychological factors like fear-avoidance and pain catastrophizing.
- Progressive strengthening and endurance training.
- Advanced neural mobilization and functional retraining.
- Address psychological factors like fear-avoidance and pain catastrophizing.
| Symptom Phase | Treatment Focus | Precautions |
|---|---|---|
| Acute | Education, pain management, activity modification | Avoid aggressive neural mobilization; monitor irritability |
| Subacute | Graded activity, gentle neural mobilization, motor control | Progress carefully; avoid symptom aggravation |
| Chronic | Endurance training, advanced mobilization, psychological support | Address long-term disability and fear avoidance |
Dr. Desforges’ clinical practice reflects this graduated model, adjusting therapeutic intensity based on individual patient tolerance and response to care, thus fostering safer, more effective rehabilitation journeys.
Integrating Movement Coordination and Mobility Training in Lumbar Radiculopathy Care
Movement coordination deficits and mobility impairments commonly co-exist with lumbar radiculopathy symptoms. Addressing these through targeted rehabilitation enhances functional recovery and reduces the risk of recurrence.
Typical interventions include:
- Core Stabilization Exercises: Such as abdominal bracing, supine marching, bird-dogs, and planks to enhance trunk control and spinal support.
- Progressive Mobility Work: Mobilizations of lumbar and thoracic segments to restore joint range and alleviate stiffness.
- Functional Training: Task-specific strengthening like lunges and bridging to improve endurance relevant to daily activities and occupational demands.
In cases with hypomobility, manual therapy techniques including mobilization or manipulation may precede exercise therapy. These manual interventions should be combined with immediate reinforcement of motor control drills to maximize sustained benefits.
| Rehabilitation Component | Purpose | Example Exercises |
|---|---|---|
| Core Stabilization | Enhance trunk support and reduce spine strain | Abdominal bracing, supine marching, bird-dogs, planks |
| Mobility Exercises | Restore joint range and flexibility | Spinal mobilization, flexion and extension stretches |
| Functional Strengthening | Improve endurance and task-specific control | Lunges, bridging, step-down drills |
This layered approach, championed in evidence-based pathways and endorsed by leaders like Dr. Sylvain Desforges, empowers patients to regain independence and prevents long-term impairments common with untreated lumbar radiculopathy.
Patient Education and Lifestyle Adjustments for Long-Term Relief
Education is a cornerstone of lumbar radiculopathy management. Understanding the condition, realistic expectations, self-management strategies, and lifestyle modifications profoundly impact recovery speeds and reduce relapse risk.
Essential educational content should encompass:
- Nature of Radiculopathy: Explanation of nerve root irritation and its symptom manifestation, emphasizing the difference between referred and radiating pain.
- Activity Guidance: Encouragement to maintain safe, tolerated activities and avoid prolonged bed rest beyond brief acute phases.
- Use of Supportive Aids: Guidance on appropriate use of braces such as DonJoy or Mueller, and ergonomic adjustments including Tempur-Pedic seating for spinal alignment.
- Pain Management Techniques: Introduction to adjunctive therapies such as Biofreeze topical analgesics and tools like Theragun for muscular relaxation.
- When to Seek Further Care: Clear red-flag warning signs and criteria for escalating care to specialist consultation or medical intervention.
Patients report that comprehensible education reduces anxiety and fosters active engagement in rehabilitation programs. Clinicians like Dr. Desforges prioritize this accessible, jargon-free communication, collaborating with patients to customize understanding according to their unique experiences.
| Educational Topic | Recommendation | Patient Benefit |
|---|---|---|
| Understanding Radiculopathy | Explain nerve root involvement and symptom patterns | Reduces fear and misconceptions |
| Activity Levels | Promote safe movement and avoid prolonged rest | Prevents deconditioning and supports recovery |
| Supportive Devices | Proper use of braces and ergonomic aids | Enhances comfort and stability |
| Pain Management Tools | Instruction on adjunctive therapies like Biofreeze and Theragun | Improves symptom control |
| Red Flags Awareness | Educate on symptoms warranting urgent care | Ensures timely medical response |
What differentiates lumbar radiculopathy from general low back pain?
Lumbar radiculopathy involves nerve root irritation or compression causing radiating leg pain, sensory changes, and motor weakness, whereas general low back pain may not involve nerve symptoms and usually remains localized.
When should imaging be considered for lumbar radiculopathy?
Imaging, such as MRI, is recommended when neurological deficits persist beyond four to six weeks, symptoms worsen, or red flags like cauda equina syndrome are present.
How does neurovertebral decompression therapy aid lumbar radiculopathy?
It reduces pressure on spinal discs and nerve roots through controlled spinal traction, promoting pain relief and functional recovery without surgery.
Are there effective non-surgical treatments for lumbar radiculopathy?
Yes. Exercise therapy tailored to symptom classification, neural mobilization, patient education, physical modalities like Biofreeze, and activity modification form the cornerstone of non-surgical management.
What lifestyle changes help prevent lumbar radiculopathy recurrence?
Maintaining an active lifestyle, practicing proper body mechanics, using supportive devices appropriately, and managing stress through education and ergonomics reduce recurrence risk.

