Herniated Disc and Sciatica: TAGMED’s Approach in Laval
October 23, 2025
Innovative implants: insights from an expert on TOPS™, Intraspine®, and ESP
October 25, 2025In Brief:
Spinal decompression therapy offers non-invasive relief for herniated discs and nerve pain without surgery.
By reducing disc and nerve pressure, it targets symptoms like radiating pain, numbness, and mobility impairment.
The process involves computer-controlled traction to gently elongate the spine and promote disc healing over multiple sessions.
Ideal for patients with mild to moderate cases, it is inappropriate for those with certain contraindications such as severe osteoporosis or tumors.
Compared to surgery, spinal decompression therapy is associated with lower risk, no downtime, and evidence-based outcomes, but requires expert evaluation for best results.
Spinal decompression therapy has emerged as a transformative solution for individuals struggling with relentless back pain from herniated discs, sciatica, and related spinal challenges. In 2025, as innovative approaches become the cornerstone of modern rehabilitative medicine, more patients and practitioners are seeking gentle, non-surgical options that restore function without the risks or long recovery times of traditional surgery. This growing demand is fueled not just by technology but by real-world outcomes—patients regaining lost mobility, returning to sports, and resuming daily life where pain once stood in the way.
Within this context, leading clinics such as Clinique TAGMED and medical experts like Dr. Sylvain Desforges are at the forefront, employing state-of-the-art equipment and evidence-based protocols to tailor care. This article takes you through every angle of spinal decompression therapy, from how it works at a physiological level, to whom it best serves, and how it compares to surgical alternatives. Along the way, we’ll examine anecdotes, recent research, and practical checklists—offering invaluable insight for those considering their next steps towards lasting relief and healing.
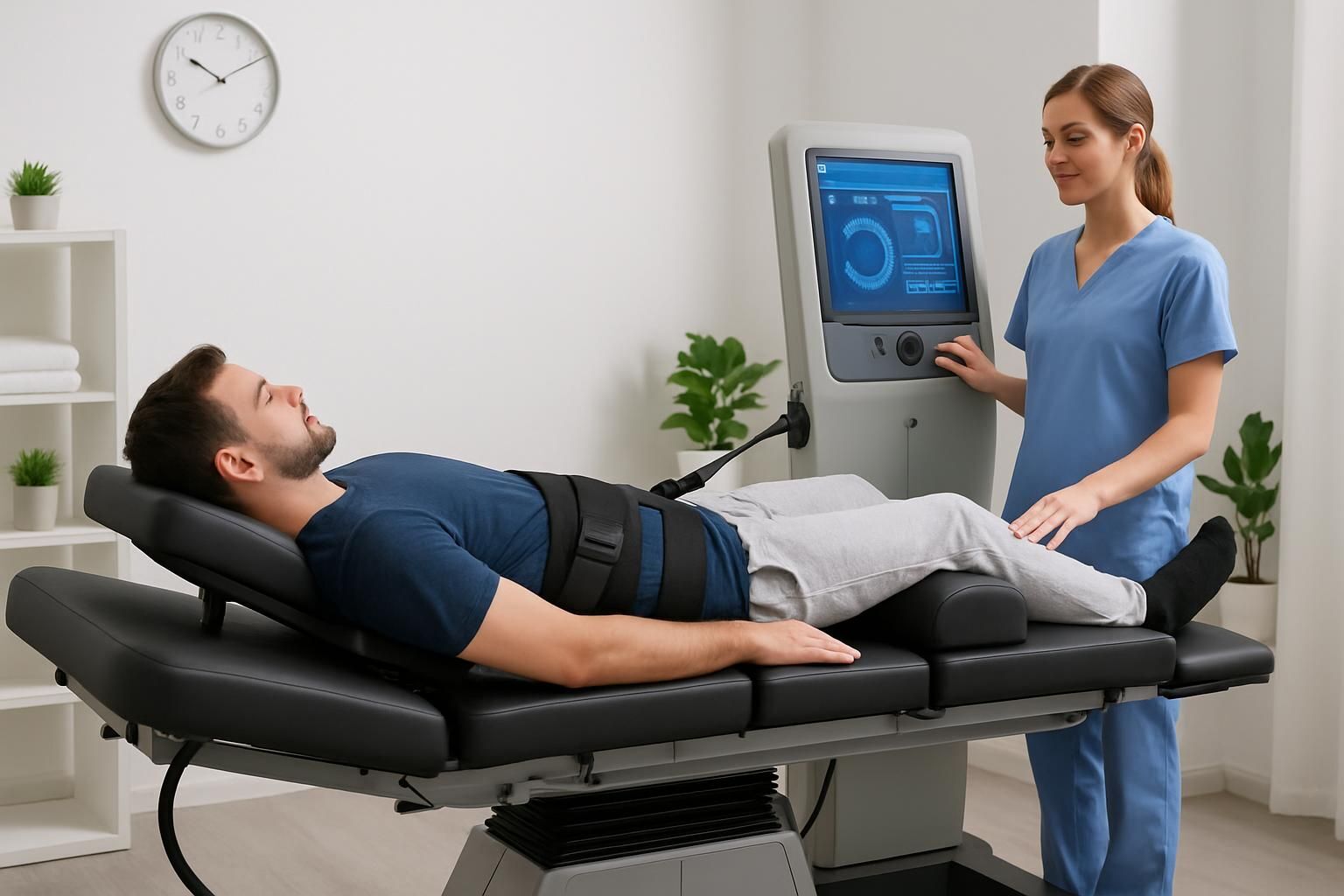
Understanding Spinal Decompression Therapy for Herniated Discs: Non-Invasive Relief Explained
What Is Spinal Decompression Therapy? Benefits and Mechanisms for Herniated Discs
Spinal decompression therapy is a specialized, non-surgical treatment engineered to alleviate the compressive forces exerted on spinal discs and nerves, particularly in cases of herniated discs. Unlike conventional surgical approaches, this therapy is non-invasive, relying instead on precisely calibrated mechanical traction. The primary objective is to gently stretch the spine, generating negative pressure within affected discs.
Through this process, a vacuum-like effect encourages bulging or herniated material to retract—relieving pressure on nerves and adjacent structures. Additionally, the therapy enhances nutrient, water, and oxygen influx into the discs, promoting cellular regeneration, rehydration, and healing. This makes it especially beneficial not only for pain relief but also for supporting the body’s natural repair mechanisms. Learn more from this comprehensive guide by Dr. Jonathan Wise which sheds light on its principles and benefits.
Mechanism | Therapeutic Benefit |
|---|---|
Spinal elongation with traction | Reduces pressure on herniated discs and nerves |
Disc retraction | Relieves nerve irritation and radiating pain |
Improved nutrient delivery | Promotes healing and slows degeneration |
Customizable settings for individualized care
Minimal discomfort compared to invasive procedures
Targets chronic and acute pain linked to disc injuries
For individuals seeking relief from persistent back pain, spinal decompression therapy is an avenue worth exploring, especially before considering surgery.
How Non-Surgical Spinal Decompression Reduces Disc and Nerve Pressure
The science behind spinal decompression therapy hinges on the principle of decompressive traction applied to the spine. Using a sophisticated, computer-controlled table, patients are gently positioned and harnessed to precisely control the angle and force of spinal stretching. This accuracy is crucial, as it allows the therapy to target the specific discs involved—be it lumbar or cervical.
By creating negative intradiscal pressure, the method draws herniated or bulging material back toward the disc’s center. This not only relieves the root cause of most pain—nerve compression and chemical inflammation—but also fosters rehydration and the influx of healing factors. Stories from clinics like Deuk Spine Institute illustrate patients who, after just a few weeks, report significant reductions in pain and dramatic gains in mobility.
Negative pressure pulls herniated material away from nerves
Reduced inflammation equals less swelling and discomfort
Optimal healing environment allows for sustainable recovery
The approach provides a targeted alternative for managing chronic disc and nerve pain, offering hope where medication may only mask symptoms.
Laval Lumbar Herniated Disc Solutions for Seniors
The prevalence of lumbar herniated discs among seniors in Laval has led to a growing demand for advanced, non-invasive, and effective solutions that offer relief without the risks associated with surgery. This shift towards conservative care is particularly pertinent as…

Candiac Back Pain Relief for Herniated Disc Sufferers
Back pain stemming from herniated discs remains a challenging and widespread issue impacting many individuals in Candiac and the surrounding Quebec regions. This condition often leads to persistent discomfort, restricted mobility, and diminished quality of life for sufferers. In the…
Symptoms and Conditions Treated by Spinal Decompression: Relief for Herniated Discs, Sciatica, and More
Recognizing Herniated Disc Symptoms and Related Functional Impairments
A herniated disc can present with a spectrum of symptoms that disrupt daily life—ranging from sharp, radiating leg or arm pain, to persistent numbness, tingling, or burning sensations. Muscle weakness, diminished reflexes, and restricted mobility are also common, especially when discs press on or irritate nerve roots.
Lifestyle factors such as prolonged poor posture, sedentary habits, lifting injuries, obesity, or even genetic predisposition can all contribute to disc vulnerability. According to disc herniation resources from MedPlus Centers, timely evaluation of symptoms—such as reduced grip strength, sciatica, or sudden difficulty walking—is essential for effective intervention and the prevention of further injury.
Sudden or chronic localized back pain
Numbness or tingling in extremities
Muscle weakness or loss of motor coordination
Diminished range of motion or flexibility
Early identification and comprehensive management with spinal decompression therapy can restore function and mitigate long-term impacts.
Spinal Decompression for Degenerative Disc Disease, Sciatica, and Spinal Stenosis
While best known for treating herniated discs, spinal decompression therapy is effective for other chronic spinal ailments such as degenerative disc disease, sciatica, and certain forms of spinal stenosis. These conditions often coexist and manifest with overlapping pain profiles—numbness, difficulty with mobility, and persistent inflammation.
For instance, patients with degenerative changes may experience a gradual loss of disc height and flexibility, intensifying pressure on adjacent nerves. Application of decompressive traction directly addresses these biomechanical issues, as highlighted in the WellConsulted therapy guide.
Condition | Symptoms Improved | Therapy Role |
|---|---|---|
Herniated Disc | Radiating pain, numbness, weakness | Disc pressure reduction & healing |
Degenerative Disc Disease | Stiffness, chronic discomfort, instability | Restores height & function |
Sciatica | Leg/hip pain, tingling | Relieves nerve root pressure |
Spinal Stenosis | Limited walking, back & leg pain | Widening of spinal canal space |
A multifaceted approach—combining lifestyle guidance with regular spinal decompression sessions—can result in meaningful improvements for patients who previously relied only on medication.
La Prairie Chronic Neck Pain Recovery Without Medication
Chronic neck pain continues to be a widespread and challenging condition that impacts millions globally, with significant effects on daily functioning and quality of life. Not confined to any particular age or occupation, it manifests from diverse causes such as…

Mirabel Lumbar Disc Protrusion Treatment Success Rates
The management of lumbar disc protrusion remains a critical focus in spinal health research and clinical care, especially within the dynamic context of Mirabel and surrounding regions. As low back pain continues to affect a significant portion of the adult…
Step-by-Step: The Non-Surgical Spinal Decompression Treatment Process
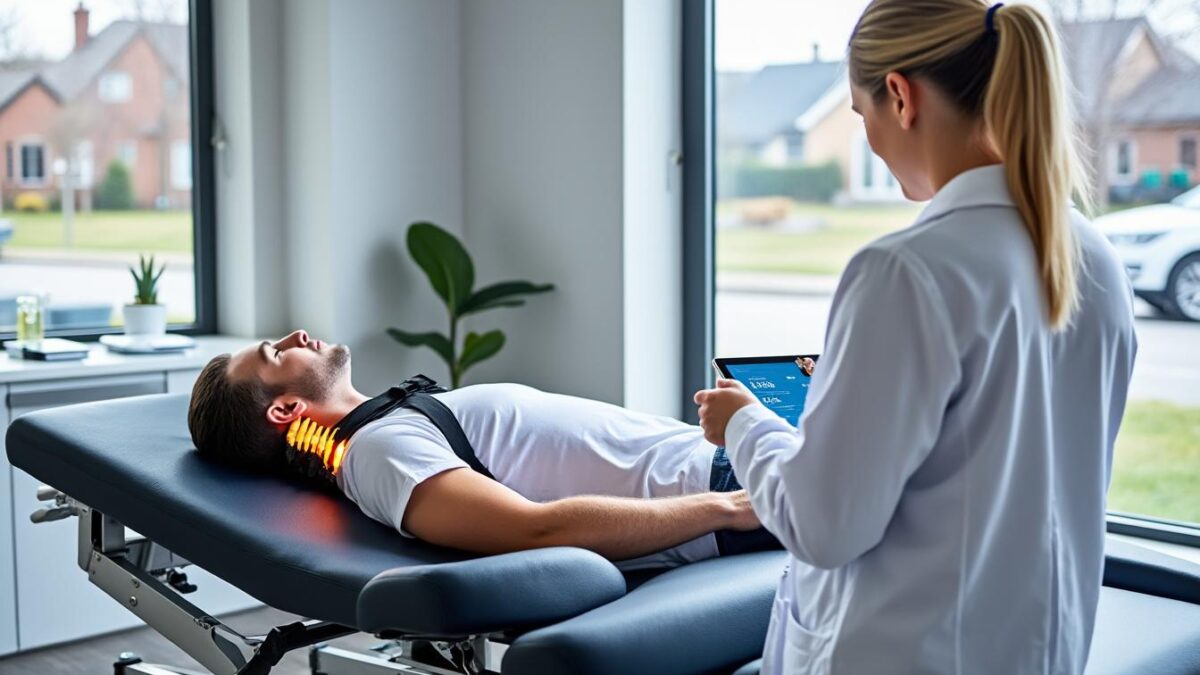
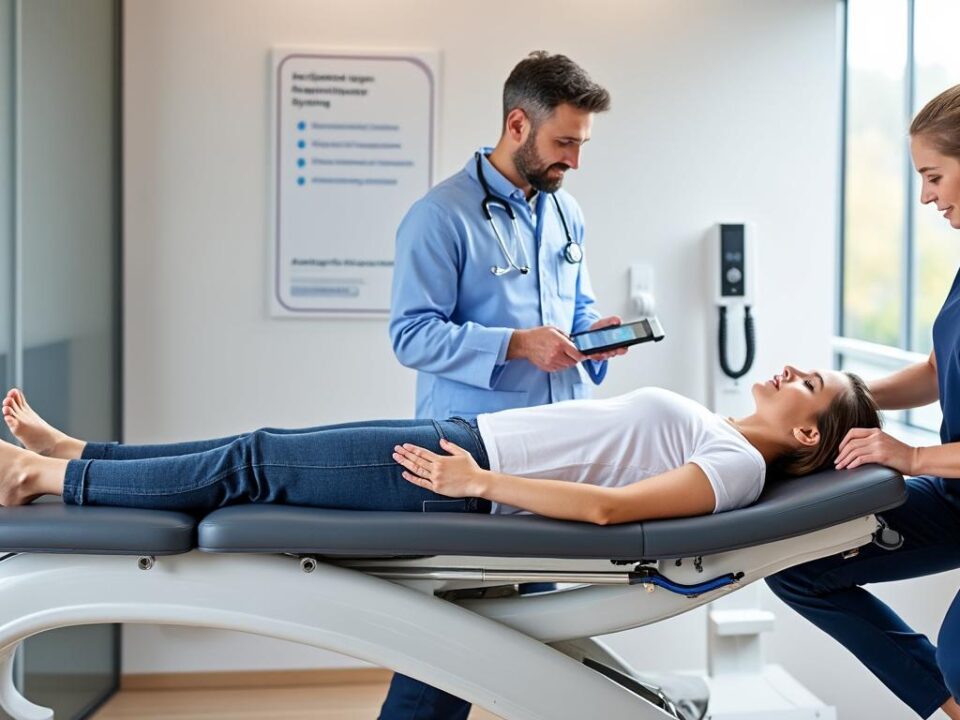
What to Expect During Spinal Decompression Sessions: Table Positioning, Traction, and Duration
Patients embarking on spinal decompression therapy are typically greeted by a high-tech, motorized table, controlled by an operating specialist. After a thorough safety briefing, patients are gently strapped in—either face-up or face-down depending on the spinal region treated. The session begins with careful adjustment of the traction force and angle, allowing for personalized pressure on target discs.
Most therapy protocols consist of sessions lasting 20-30 minutes, repeated 2-4 times per week for a course of several weeks. The entire process is closely monitored to ensure patient comfort, and automated systems precisely modulate the cycles of traction and relaxation. More on advanced technology can be explored at Spinal Decompression Therapy Technology.
Initial assessment and individualized therapy plan
Progressive adjustment according to symptom relief
Continuous feedback to maximize safety and healing
The ultimate aim is to reduce pressure on compressed discs, relieve pain, and facilitate gradual tissue healing—without the risks tied to invasive procedures.
Patient Experience and Typical Progression of Symptom Relief
Most patients find spinal decompression therapy sessions to be relaxing—the gentle stretching can even elicit a sense of relief during treatment. While a minority may feel mild soreness, this generally subsides as healing progresses. Over several weeks, many report a steady decrease in pain, improved flexibility, and a sensation of renewed mobility.
Clinical anecdotes frequently reference individuals—like a retired runner who visited Clinique TAGMED—who transitioned from daily pain to renewed activity within three months. The key lies in the cumulative effect of therapy: consistent traction reduces swelling and pressure, while repeated sessions allow discs time to recover and rehydrate.
Typical Progression | Expected Changes |
|---|---|
After 1-2 sessions | Slight pain reduction, increased comfort when sitting/standing |
After 5-8 sessions | Noticeable decrease in radiating pain, improved flexibility |
After full course (12-20 sessions) | Significant restoration of mobility, diminished numbness, confidence in daily activity |
Vaudreuil-Dorion Sciatica Recovery Through Non-Invasive Care
In the vibrant community of Vaudreuil-Dorion, many individuals grapple with debilitating sciatica, a condition characterized by sharp, radiating pain originating in the lower back and traveling down the legs. This ailment significantly disrupts daily life, impeding mobility and diminishing overall…

Saint-Eustache Neck Herniation Solutions Using Decompression
Neck pain, often stemming from conditions like herniated disc and cervical spine disorders, is a widespread affliction impacting millions globally. Residents of Saint-Eustache facing such challenges now have access to innovative, non-surgical treatment options that tackle the root causes of…
Ideal Candidates, Contraindications, and Alternatives to Spinal Decompression Therapy
Who Is an Ideal Candidate for Non-Surgical Spinal Decompression?
Spinal decompression therapy is most suitable for individuals with mild to moderate herniated disc symptoms or chronic nerve-related discomfort who have seen limited success with rest, medication, or physical therapy. Patients should have reasonable disc integrity and no evidence of severe instability or complex neurological deficits.
Nerve pain due to disc herniation, sciatica, or degenerative disc problems
Absence of acute spinal trauma or infections
Desire to avoid surgical intervention
Motivation for active participation in recovery
Collaborative evaluation by an experienced practitioner—like Dr. Sylvain Desforges—ensures the optimal treatment protocol for each situation.
Contraindications: When Spinal Decompression Therapy Is Not Recommended
Despite its versatility, spinal decompression therapy is unsuitable for certain groups. Those with spinal fractures, metastatic tumors, recent surgical implants or severe osteoporosis are generally advised against it. Pregnant women and individuals with advanced nerve compromise should also seek alternative strategies.
For a full overview of contraindications and safety considerations, the medically-reviewed information at SOS Herniated Disc is a trusted resource. Proper screening is crucial to avoid adverse outcomes.
Spinal instability or hardware in place
Active cancer or spinal infection
Advanced osteoporosis or metabolic bone diseases
Contraindication | Reason |
|---|---|
Recent spinal fractures | Risk of worsening injury |
Severe nerve compression with loss of function | May need urgent surgery instead |
Pregnancy | Unsuitable due to mechanical stress |
Alternative and Minimally Invasive Treatments for Herniated Discs
If spinal decompression therapy is contraindicated or proves ineffective, emerging alternatives may offer relief. Minimally invasive procedures—such as laser-assisted disc repair, microdiscectomy, or percutaneous endoscopic techniques—prioritize preserving native disc structure and promote shorter recovery times compared to traditional surgery.
More detailed information on these alternatives is available via the Loucil Chiropractic therapy guide and the spinal decompression special report. Conservative measures like focused physical therapy, posture training, and ergonomic modification can also empower patients in their long-term healing journey.

Mascouche Lower Back Injury Rehabilitation Without Surgery
Lower back injuries are a prevalent challenge that impacts countless individuals in Mascouche and beyond, often resulting in debilitating pain and disrupted daily life. Despite the common perception that surgery is the inevitable recourse for such spinal issues, many patients…

Saint-Jérôme Cervical Disc Herniation Recovery in Weeks
Cervical disc herniation poses a significant challenge for many residents in Saint-Jérôme seeking fast and effective relief from neck pain and restricted movement. This condition, involving the displacement or rupture of the cushioning discs located between the cervical vertebrae, can…
Comparing Non-Surgical Spinal Decompression, Surgical Options, and Effectiveness: Evidence and Best Practices
Surgical Spinal Decompression for Herniated Discs: Procedures, Risks, and Recovery
Surgical intervention is typically reserved for severe or unresponsive herniated disc cases that threaten neurological function or persist despite months of conservative care. Principal operations include laminectomy (removal of part of the bony vertebra to open the canal), microdiscectomy (extraction of herniated disc material), and spinal fusion (permanent joining of vertebrae).
While these can bring dramatic pain relief, they carry increased risks—bleeding, infection, nerve injury, and protracted recovery. Surgical procedures also necessitate anesthesia and hospital stays, and may sometimes lead to chronic instability or the need for additional interventions. A useful procedural breakdown can be found in the Spine Together surgical decompression guide.
Procedure | Goal | Main Risks | Typical Recovery |
|---|---|---|---|
Laminectomy | Expand spinal canal, relieve nerve pressure | Instability, infection, blood loss | 4-8 weeks or more |
Microdiscectomy | Remove herniated disc fragments | Nerve root injury, scar tissue | Up to 6 weeks |
Spinal Fusion | Prevent movement at painful segment | Hardware issues, adjacent disc degeneration | Several months |
Clinical Evidence on the Effectiveness of Spinal Decompression Therapy
Numerous clinical studies, including those referenced at SOS Herniated Disc and Back Pain Westchester, support the effectiveness of spinal decompression therapy in reducing pain and restoring function for a substantial number of patients with herniated disc symptoms. Outcomes can vary by age, degree of disc damage, and adherence to the full treatment plan.
Significant pain relief for many after multiple sessions
Reduced reliance on opioids and other pain medications
Improved quality of life and restored mobility
Importantly, data continues to evolve, and further long-term studies are required to refine patient selection and optimize outcomes.
Advantages of Non-Surgical Spinal Decompression Over Surgical Intervention
Spinal decompression therapy offers compelling advantages: no incisions, anesthesia, or extended hospital stays. Risks are markedly lower, and most patients return to their routine activities immediately. Modern clinics leverage advanced digital platforms, integrating patient feedback for highly tailored regimens.
According to the Today’s Woman guide, treatment plans are flexible and personalized, making them accessible to a wider demographic. For those who meet the therapeutic criteria, the therapy provides a safer, cost-effective bridge between passive management and invasive procedures.
No downtime; return to daily life after each session
Customizable to target individual anatomical needs
Lower cost and fewer complications compared to surgery
Consultation with trusted healthcare professionals remains vital—to ensure the therapy aligns with your unique health profile and maximizes the chance for lasting healing and recovery.
Can spinal decompression therapy completely cure a herniated disc?
While spinal decompression therapy is highly effective at relieving pain and promoting disc healing in many cases, it may not fully cure the underlying disc pathology in every patient. Its primary goal is to reduce disc and nerve pressure, alleviate symptoms, and delay or avoid the need for surgery.
How soon can I expect pain relief during spinal decompression?
Some patients notice improved comfort after just a few therapy sessions, while others may require several weeks for noticeable changes. Consistency and completion of the prescribed treatment plan enhance the odds of lasting relief.
Is the therapy covered by insurance?
Coverage varies depending on insurance carrier and plan specifics. Certain providers may cover spinal decompression therapy for specific diagnoses—learn more about insurance considerations and the process at SOS Herniated Disc.
What are common side effects of spinal decompression therapy?
Mild muscle soreness or temporary stiffness may occur in the early phase of therapy, but serious complications are rare when appropriately screened and supervised.
How do I choose a provider for spinal decompression?
Select a clinic with specialized credentials, experience in treating spinal disc issues, and a reputation for personalized, patient-centered care. Seek out feedback from other patients and verify credentials through reputable associations or boards.