In the realm of spinal health, a quiet yet pervasive process unfolds over time: disc desiccation and loss of disc height. Often synonymous with the natural aging process, these changes within the intervertebral discs can sometimes be mistaken as inevitable causes of pain. But the relationship between disc desiccation, disc height reduction, and the onset of pain is far more intricate. Understanding this distinction opens doors to more precise evaluation and treatment approaches for patients experiencing back pain, especially when guided by experts like Dr. Sylvain Desforges, whose extensive clinical experience spans over three decades in osteopathic and alternative spinal care.
Disc desiccation describes the gradual dehydration of the spinal discs, reducing their ability to function as shock absorbers and structural supports within the spine. Loss of disc height frequently accompanies this dehydration, influencing spinal alignment and potentially leading to nerve irritation. However, many individuals with significant disc desiccation live without pain, while others suffer severe discomfort, highlighting the complexity of spinal pathologies. This article delves into the multifaceted aspects of disc desiccation and height loss, scrutinizes the fine line between physiological aging and pathological pain, and explores available treatment strategies embracing scientific rigor and patient-centered care, with particular attention to innovations like neurovertebral decompression and dynamic spinal implants.
Disc Anatomy and the Role of Hydration in Spine Functionality
The intervertebral discs serve as critical components in maintaining spinal stability and flexibility. Each disc comprises two distinct yet interdependent parts: the densely fibrous annulus fibrosus and the gel-like nucleus pulposus. The nucleus is predominantly hydrated, containing up to 80% water at birth, which gradually decreases with age. This moisture is essential because it allows the disc to evenly distribute mechanical loads and absorb shocks during daily activities.
In healthy spinal conditions, discs contribute approximately 25% of the spine’s total height, a factor crucial to preserving the natural curvatures that enable efficient movement and load-bearing. The annulus fibrosus encloses the nucleus and anchors the disc to adjacent vertebrae, maintaining spinal alignment and consensual motion between vertebral segments.
When hydration diminishes—a process termed disc desiccation—the nucleus loses its gel-like properties, becoming less resilient while the annulus may develop microtears or fissures. This structural compromise alters the disc’s mechanical function and height, affecting overall spinal biomechanics. This initial degeneration lays the foundation for subsequent structural changes that can manifest as pain or neurological symptoms in some patients.
Key Functions of Spinal Discs Dependent on Hydration
- Shock Absorption: Maintains cushioning effect during movements and weight-bearing.
- Load Distribution: Evenly disperses forces throughout the spinal column.
- Spinal Height Maintenance: Preserves normal intervertebral spacing critical for nerve root passage.
- Flexibility and Mobility: Enables controlled motion between vertebrae.
| Disc Component | Function | Hydration Level at Birth | Effect of Desiccation |
|---|---|---|---|
| Annulus Fibrosus | Structural containment and vertebral attachment | Approximately 65% | Microfissures and reduced integrity |
| Nucleus Pulposus | Shock absorption and load distribution | 80% | Dehydration leading to loss of elasticity |
Thus, preserving disc hydration remains a pivotal goal in spinal health management, underscoring the importance of interventions that can halt or reverse desiccation effects during early degenerative stages.
Distinguishing Natural Ageing from Pathological Disc Degeneration and Pain
Disc desiccation and loss of disc height are almost universal signs of spinal aging. Research shows that, by middle age, many individuals exhibit magnetic resonance imaging (MRI) changes consistent with disc degeneration, yet remain symptom-free. This phenomenon invites careful scrutiny into the relationship between spinal structural changes and pain manifestation.
Natural aging brings the gradual dehydration of discs, loss of elasticity, and subtle changes in spinal mechanics. However, these changes do not always culminate in pain. In contrast, pathological disc degeneration occurs when factors accelerate or exacerbate disc deterioration, leading to biomechanical instability, nerve irritation, and chronic discomfort.
Factors Contributing to Pathological Degeneration
- Excess Weight and Obesity: Increased spinal load accelerates wear on discs.
- Occupational Strain: Repetitive heavy lifting or spinal compression in certain jobs.
- Inactivity and Sedentary Lifestyle: Reduces disc nutrition due to impaired diffusion from lack of spinal movement.
- Smoking and Poor Nutrition: Impede disc cell metabolism and repair mechanisms.
- Genetic Predispositions: Influence susceptibility to early degeneration.
- Previous Spinal Trauma: Can precipitate accelerated disc damage or herniation.
Thus, while disc desiccation technically accompanies the aging process, distinguishing when it becomes a clinical problem is essential for tailoring treatment. This precision is a hallmark of Dr. Sylvain Desforges’ approach, where comprehensive evaluations integrate patient history, lifestyle factors, and advanced imaging.
| Type of Disc Degeneration | Characteristics | Relation to Pain | Typical Clinical Signs |
|---|---|---|---|
| Physiological Age-Related Degeneration | Moderate loss of hydration, some disc height reduction | Often asymptomatic | Mild stiffness, minimal pain |
| Pathological Degeneration | Accelerated dehydration, severe height loss, annular tears | Frequently symptomatic | Persistent pain, neurological symptoms, reduced mobility |
Recognizing these nuances ensures patients receive personalized care plans designed around their unique biomechanical and symptomatic profiles.
Clinical Manifestations of Disc Desiccation and Associated Pain Syndromes
The symptoms of disc desiccation vary significantly, ranging from no symptoms to severe pain and neurological impairments. The variability depends on the extent of dehydration, disc height loss, and whether surrounding neural structures are affected.
Patients might initially notice:
- Stiffness: Especially in the lumbar or cervical regions after periods of inactivity.
- Localized Pain: Mild to moderate ache or discomfort exacerbated by movement.
- Radicular Pain: Radiating sensations due to nerve root irritation, often extending to limbs.
- Neurological Symptoms: Numbness, tingling, or muscle weakness in the extremities.
- Height Loss Consequences: Reduced disc height can lead to foraminal narrowing, increasing the risk of nerve compression.
Importantly, clinical presentations are influenced by patient-specific factors such as age, anatomy, physical activity, and concurrent spinal conditions like facet arthropathy or spondylolisthesis.
Common Symptom Clusters Observed in Patients
| Symptom | Description | Potential Underlying Cause |
|---|---|---|
| Localized Back or Neck Pain | Dull, chronic pain worsened with flexion or extension | Disc dehydration and annular fissures |
| Radiculopathy | Shooting or burning pain radiating down extremities | Nerve root compression from disc height loss or herniation |
| Stiffness and Reduced Mobility | Decreased spinal flexibility, especially after rest | Loss of disc hydration impacting disc elasticity |
| Neurological Deficits | Weakness or numbness indicating nerve involvement | Chronic nerve root impingement |
Dr. Desforges’ extensive clinical expertise is particularly valuable in helping patients navigate these symptoms. His approach emphasizes comprehensive evaluation, where a differential diagnosis considers other factors and conditions that may mimic or exacerbate pain associated with disc desiccation.
Innovative Diagnostic Approaches to Assess Disc Desiccation and Height Loss
Accurate diagnosis of disc desiccation and associated loss of disc height is fundamental to formulating effective treatment plans. Advanced imaging technologies continue to improve the sensitivity and specificity of spinal evaluations.
- Magnetic Resonance Imaging (MRI): The gold standard for detecting disc hydration levels, annular integrity, and nerve involvement without radiation exposure.
- CT Scans: Provide detailed bone imaging to assess secondary changes such as osteophytes or foraminal stenosis.
- X-Ray Imaging: Useful for assessing gross disc height loss and spinal alignment changes.
- Dynamic Radiographs: Evaluate spinal movement and instability, important for surgical planning.
Beyond conventional imaging, newer technological advancements refine assessment sensitivity. These include T2 mapping MRI, which quantifies water content changes within discs, and functional imaging techniques identifying early metabolic alterations. Experts like Dr. Desforges integrate these tools to improve precision in distinguishing symptomatic from asymptomatic disc degeneration.
| Diagnostic Tool | Application | Strengths | Limitations |
|---|---|---|---|
| MRI | Disc hydration, nerve root evaluation | Non-invasive, high-resolution soft tissue imaging | Cost, availability, contraindications in some patients |
| CT Scan | Bone detail, osteophyte detection | Excellent bone visualization | Radiation exposure, less soft tissue detail |
| X-Ray | Disc height assessment, spinal curvature | Widely available, low cost | Limited soft tissue information |
| T2 Mapping MRI | Quantitative disc hydration measurement | Early degeneration detection | Specialized equipment, research settings |
This range of diagnostic modalities facilitates personalized approaches, carefully balancing the risks and benefits of further interventions.
Conservative Management and Non-Surgical Therapies for Disc Desiccation
Most patients with disc desiccation benefit from conservative treatment initially, emphasizing non-invasive approaches that mitigate pain, improve mobility, and support spinal health. Dr. Sylvain Desforges advocates personalized conservative therapies rooted in scientific evidence and patient comfort.
- Targeted Physical Therapy: Programs that enhance core and paraspinal muscle strength to reduce disc load and restore spinal alignment.
- Spinal Decompression Therapy: Advanced non-surgical technologies such as neurovertebral decompression systems alleviate pressure on discs and nerves.
- Pharmacological Measures: Use of NSAIDs, analgesics, and muscle relaxants for symptomatic relief, with careful monitoring of side effects.
- Postural Education and Ergonomics: To avoid repetitive strain and promote optimal spine mechanics in daily activities.
- Analgesic and Anti-inflammatory Injections: Including corticosteroid epidural injections for nerve root inflammation when indicated.
Effectiveness depends on early intervention and patient adherence. Dr. Desforges’ practice leverages multidisciplinary coordination and continuous patient education to optimize outcomes.
| Conservative Treatment | Purpose | Expected Outcome | Limitations |
|---|---|---|---|
| Physical Therapy | Strengthen musculature, improve mobility | Reduced pain, enhanced function | Requires patient commitment |
| Spinal Decompression | Relieve neural pressure | Pain alleviation, improved disc hydration | Variable response; supplemental treatment |
| Medications | Pain and inflammation control | Symptom relief | Does not alter disease progression |
| Injections | Reduce nerve inflammation | Temporary pain relief | Limited duration; repeat treatments needed |

Surgical Innovations for Advanced Disc Desiccation and Height Loss
For patients unresponsive to conservative care or experiencing severe symptoms, surgical options remain critical. The landscape of spine surgery has evolved considerably, embracing technologies from leading manufacturers including Medtronic, Stryker, Zimmer Biomet, NuVasive, Depuy Synthes, Globus Medical, Orthofix, SpineWave, Aesculap, and Baxter.
Artificial Disc Replacement (ADR) replaces the damaged disc with a prosthesis designed to maintain motion, potentially preserving adjacent segment mobility.
Spinal Fusion involves stabilizing the affected vertebral segment by fusing adjacent bones, using instrumentation and bone graft materials, which may impact spine flexibility but reduces pain from instability.
Emerging technologies focus on dynamic implants that adapt to spinal movements, minimally invasive surgery techniques lowering recovery times, and integrated laser therapies minimizing tissue trauma.
- Advantages of ADR: Maintains segment motion; may reduce adjacent segment degeneration.
- Advantages of Fusion: Provides definitive stabilization; effective in multi-level degeneration.
- Minimally Invasive Approaches: Reduced blood loss, quicker recovery.
- Use of High-Tech Implants: Enhanced biomechanical compatibility and durability.
| Surgical Technique | Indication | Benefits | Recovery Time |
|---|---|---|---|
| Artificial Disc Replacement | Severe disc degeneration with preserved facet joints | Motion preservation, pain relief | 8-12 weeks |
| Spinal Fusion | Instability, multi-level degeneration | Segment stabilization, pain reduction | 3-6 months |
| Minimally Invasive Decompression | Nerve compression, stenosis | Less tissue damage, faster recovery | 4-8 weeks |
Dr. Desforges rigorously ensures surgical candidacy evaluations comply with stringent Quebec and Canadian medical regulations and emphasizes exploring conservative avenues before surgery.
Personalized Patient Care: Evaluation and Continuous Support
Disc desiccation and associated height loss demand a nuanced and personalized approach due to varied presentations and progression rates. Dr. Sylvain Desforges employs comprehensive evaluations to capture each patient’s unique condition, considering clinical findings, imaging results, lifestyle, and goals. Importantly, he clarifies that his role is to conduct thorough assessments, not medical diagnosis, empowering patients with clear understanding and agency in their care.
Patient education is a cornerstone, with all information communicated in accessible language that demystifies complex medical terms and treatment pathways. This transparency fosters a collaborative dynamic where patients are motivated to actively engage in conservative management techniques or deliberate on surgical options as appropriate.
- Detailed spinal evaluations with advanced imaging review.
- Customized treatment plan integrating osteopathy, rehabilitation, and modern technology.
- Ongoing monitoring and adjustment of therapies according to patient progress.
- Emphasis on ethical standards, scientific rigor, and patient safety throughout care.
| Aspect | Implementation at TAGMED | Benefit to Patient |
|---|---|---|
| Comprehensive Evaluation | Multimodal clinical and imaging assessment | Accurate condition characterization for tailored care |
| Personalized Treatment Planning | Individualized osteopathic and decompression therapies | Optimized symptom management and function restoration |
| Continuous Support | Regular follow-ups and patient education | Increased treatment adherence and patient empowerment |
| Compliance and Ethics | Strict adherence to Quebec and Canadian medical standards | Safe, effective, and trustworthy care delivery |
This patient-first model is a hallmark of care under Dr. Desforges’ guidance, blending compassion with innovation and expertise.

Integrating Advanced Technologies in Spinal Care: Neurovertebral Decompression and Dynamic Implants
As disc desiccation progresses, restoration of disc function and spinal alignment is vital to preserve quality of life. Technological innovations have revolutionized treatment paradigms, offering new hope to patients with degenerative disc changes.
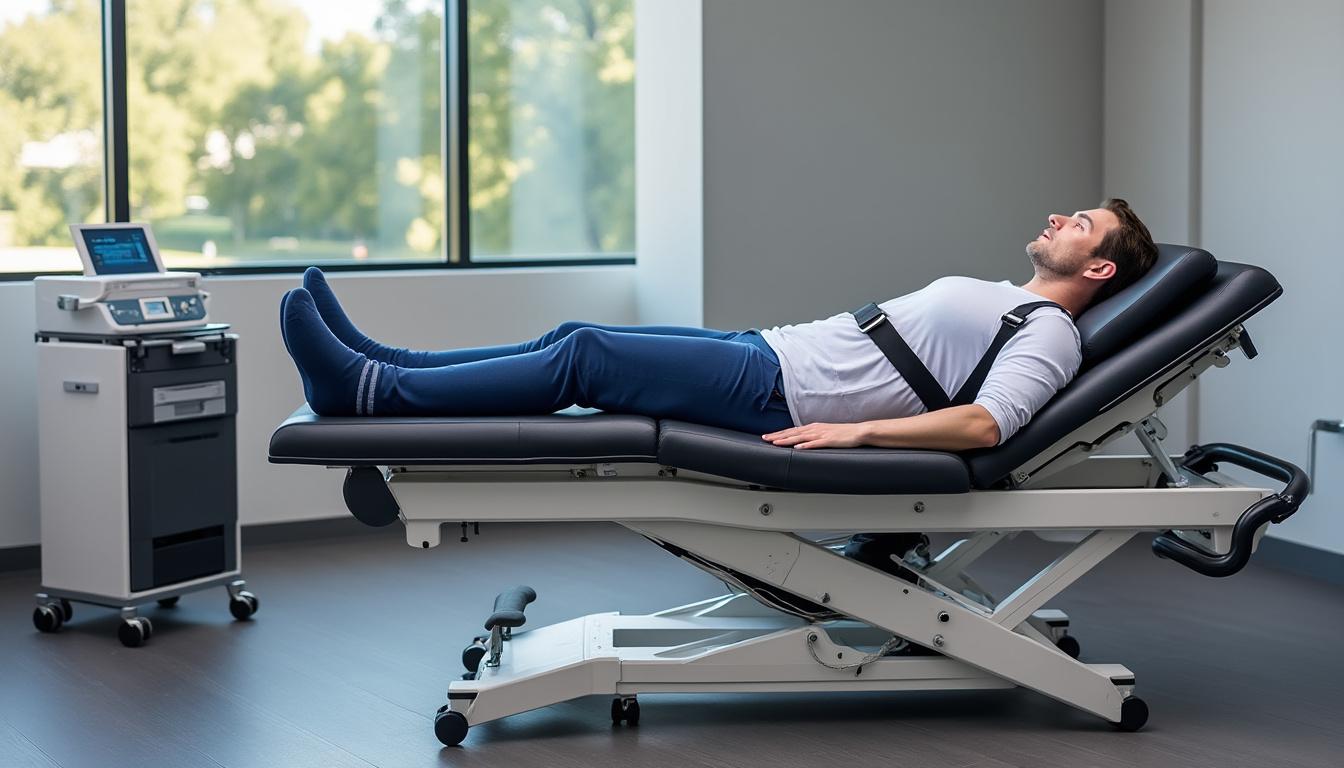
Neurovertebral decompression therapy employs motorized spinal decompression tables to gently elongate the spine, reducing intradiscal pressure and promoting nutrient transport into the disc matrix. This non-invasive technique is particularly effective for early-stage disc desiccation and herniations.
Dynamic spinal implants represent another leap forward. Unlike rigid fusion devices, these implants maintain segmental motion, reduce adjacent segment degeneration, and provide improved biomechanical behavior consistent with natural disc function. Companies such as Medtronic, NuVasive, and Zimmer Biomet have led advancements in this area, integrating biomaterials compatible with long-term implantation and functional restoration.
- Reduced nerve compression and inflammation
- Preservation of spinal mobility and flexibility
- Potential for disc height restoration through biomechanical support
- Shorter recovery periods compared to conventional surgery
| Technology | Purpose | Benefits | Leading Manufacturers |
|---|---|---|---|
| Neurovertebral Decompression | Reduce intradiscal pressure, promote healing | Non-invasive, supports disc hydration restoration | SpineWave, Orthofix |
| Dynamic Spinal Implants | Maintain motion while stabilizing spine | Protect adjacent discs, promote functional biomechanics | Medtronic, NuVasive, Zimmer Biomet |
| Laser Therapy | Reduce inflammation and facilitate tissue repair | Minimally invasive, adjunct to other therapies | Aesculap, Baxter |
Ongoing clinical studies continue to evaluate long-term outcomes, refining protocols that integrate these technologies with customized conservative and surgical care strategies.
Empowering Patients Through Education and Transparent Communication
One of the pillars of effective spinal care is clear and accessible education. Dr. Sylvain Desforges prioritizes demystifying disc desiccation and spinal degenerative processes, presenting complex scientific concepts in approachable terms. This empowers patients while fostering a collaborative decision-making environment.
- Explain disc anatomy and pathology simply: Using analogies like “shock absorbers” and “cushions” to relate disc function.
- Clarify that pain is multifactorial: Highlighting that disc desiccation alone does not equate to pain.
- Outline the benefits and limitations of treatments: Helping patients set realistic expectations.
- Encourage questions and ongoing dialogue: Advancing personalized care plans based on patient feedback.
This educational approach reduces anxiety, enhances adherence, and motivates patients to take ownership of their spinal health journey, whether through conservative care or surgical options when warranted.
| Educational Focus | Approach | Patient Outcome |
|---|---|---|
| Anatomy and Function | Accessible analogies and visual aids | Improved understanding and engagement |
| Pain Mechanisms | Emphasize multifactorial nature | Reduced fear, realistic expectations |
| Treatment Pathways | Clear, evidence-based explanations | Informed decision-making |
| Patient Communication | Open dialogue and question encouragement | Enhanced adherence and satisfaction |
Practical Steps to Maintain Disc Health and Slow Desiccation
Preventative strategies remain integral to promoting spinal longevity and mitigating degenerative changes. Dr. Sylvain Desforges highlights lifestyle factors that individuals can adopt to protect disc health.
- Maintain hydration: Drinking adequate fluids supports overall tissue health.
- Engage in regular low-impact exercise: Activities like swimming, walking, and pilates stimulate disc nutrition and strengthen core musculature.
- Practice proper body mechanics: Use ergonomic lifting techniques to avoid excessive stress on discs.
- Manage body weight: Reducing excess weight helps minimize undue spinal loading.
- Avoid smoking: Smoking impairs microcirculation, jeopardizing disc nutrition and repair.
- Balanced diet rich in nutrients: Foods providing antioxidants and collagen-building nutrients support disc matrix integrity.
Implementing these steps not only slows progression of disc desiccation but also complements therapeutic interventions for existing spinal conditions.
| Preventative Measure | Benefit to Spinal Disc Health | Recommended Implementation |
|---|---|---|
| Hydration | Supports cellular function and disc fluid content | At least 2 liters of water daily |
| Low-impact Exercise | Stimulates nutrient diffusion and strengthens muscles | 30 minutes, 5 times per week |
| Proper Lifting Technique | Prevents disc overload and injury | Bend knees, keep back straight, avoid twisting |
| Weight Management | Reduces spinal load and mechanical stress | Target BMI within healthy range |
| Smoking Cessation | Enhances circulation and healing potential | Complete cessation recommended |
| Nutrition | Provides essential building blocks for disc tissue | Balanced diet with vitamins C, D, and collagen peptides |
Is disc desiccation always associated with pain?
No, disc desiccation is often a natural part of aging and may not cause any pain. Many people with desiccated discs live symptom-free; pain usually arises when associated with nerve compression or other spinal pathologies.
Can disc height loss be reversed?
In early stages of disc degeneration, conservative treatments like spinal decompression and physical therapy can help improve disc function and hydration, potentially slowing or partially reversing height loss. Advanced degeneration usually requires surgical intervention.
What innovations exist in spinal implants for disc height preservation?
Dynamic spinal implants from leading manufacturers such as Medtronic and NuVasive allow preservation of spinal motion and reduce adjacent segment degeneration, offering an alternative to traditional rigid fusion implants.
How important is physical activity in managing disc desiccation?
Regular low-impact physical activity is crucial as it promotes disc nutrition through movement-induced fluid exchange and strengthens supporting musculature, reducing pain and functional decline.
What should a patient expect from a comprehensive spinal evaluation?
A detailed assessment includes clinical examination, advanced imaging review, patient history, and functional analysis. This holistic approach guides personalized treatment recommendations and ensures clarity about the condition and management options.

