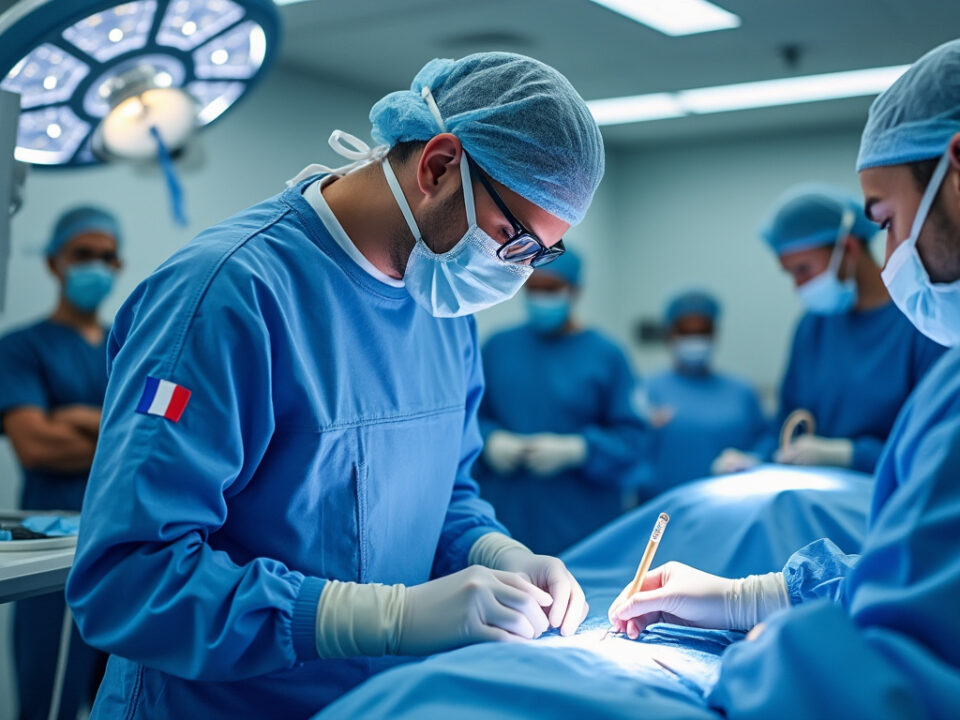
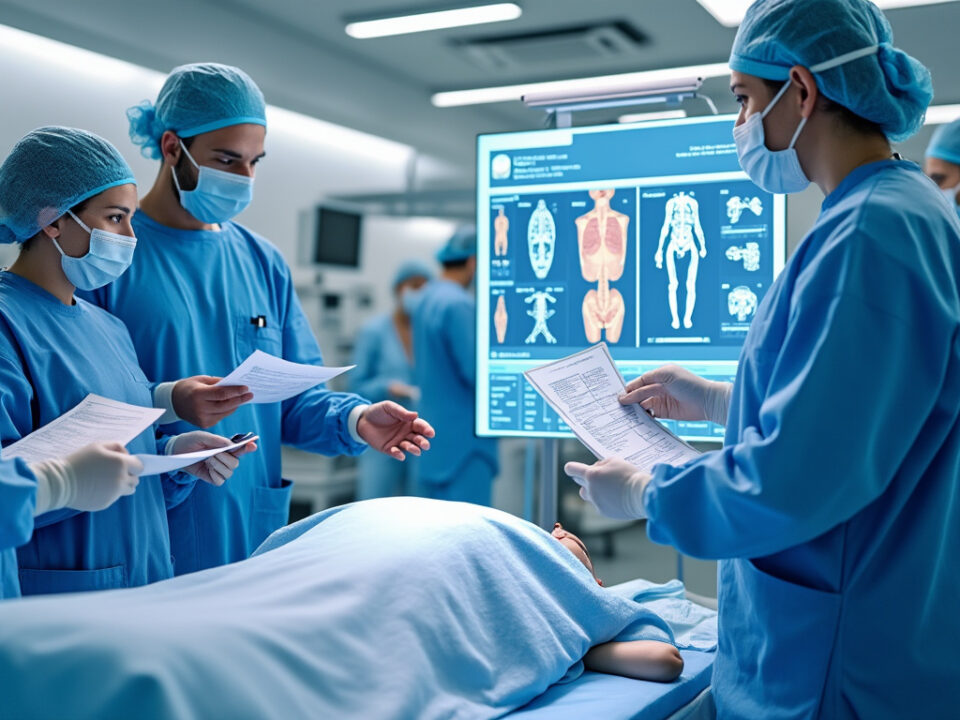
Top implant: the modern alternative to lumbar fusion
August 14, 2025
Understanding the eligibility criteria for back surgery: indications, benefits, and limitations
August 14, 2025In an era where spinal surgeries become increasingly refined, the focus is shifting not only towards the surgical procedure itself but equally on the post-operative trajectory that shapes patient recovery and quality of life. Among emerging therapies, repetitive Transcranial Magnetic Stimulation (rTMS) stands out as a groundbreaking adjunct to traditional post-surgical management. Initially renowned for its applications in psychiatric disorders, rTMS is now revealing a range of hidden benefits when integrated after spinal surgery. Particularly for patients navigating the complex recovery pathways between advanced medical systems, such as Quebec and France, rTMS introduces a new era of NeuroAdvantage by accelerating recovery rates, mitigating persistent neuropathic pain, and enhancing mental wellbeing. This combination of surgical innovation and neuromodulation forges a powerful SurgicalSynergy that elevates the entire continuum of care. The evolving protocols and collaborative international efforts bring forth a RenewalWave in rehabilitation, offering patients a reinforced PostOpPulse of hope and functionality that extends far beyond the operating room.
Enhanced Pain Management and Reduction of Neuropathic Symptoms with rTMS After Spinal Surgery
Neuropathic pain following spinal surgery remains one of the most challenging complications to address. Patients often grapple with persistent discomfort linked to nerve irritation or damage, which can limit mobility and prolong convalescence. Here the role of rTMS is noteworthy. By delivering controlled magnetic pulses mainly to the motor cortex (M1), rTMS modulates neural circuits involved with pain perception and transmission, a mechanism well documented in clinical research.
Several randomized controlled trials have confirmed the efficacy of rTMS in diminishing neuropathic pain post-operatively. For example, stimulation frequencies around 20 Hz on the cortex motor areas have resulted in significant pain relief for nearly half of treated patients, with effects extending up to several months, thereby representing a sustainable alternative to traditional pharmacologic therapies that often carry unpleasant side effects or limited effectiveness.
Managing chronic postoperative pain is crucial for enhancing patient autonomy and reducing reliance on opioid and non-opioid analgesics. The advantage of a non-invasive rTMS approach is that it aligns with contemporary goals of minimizing medication burden while promoting natural neuroplastic changes. This approach contributes to a significant RecoveryBoost by enabling patients to participate more effectively in physical rehabilitation and daily activities.
- Targeted neuromodulation of the motor cortex reduces nociceptive signaling.
- Non-invasive and safe approach, with minimal side effects such as transient headaches.
- Reduces dependence on medications, thus lowering risks of adverse drug reactions.
- Supports long-term pain relief, improving overall quality of life.
- Integrates seamlessly with multidisciplinary postoperative care.
| Aspect | Role of rTMS | Benefit to Patient |
|---|---|---|
| Neuropathic pain post-surgery | Repeated stimulation of motor cortex (20 Hz) | Significant pain reduction, reduced medication intake |
| Prevention of post-laminectomy syndrome | Regular rTMS sessions during follow-up | Attenuation of symptoms, better recovery outcomes |
The integration of rTMS for managing neuropathic pain represents a fundamental shift that enhances the patient’s SilentStrength, allowing for earlier and more confident engagement in rehabilitation, which is essential for improving surgical outcomes.

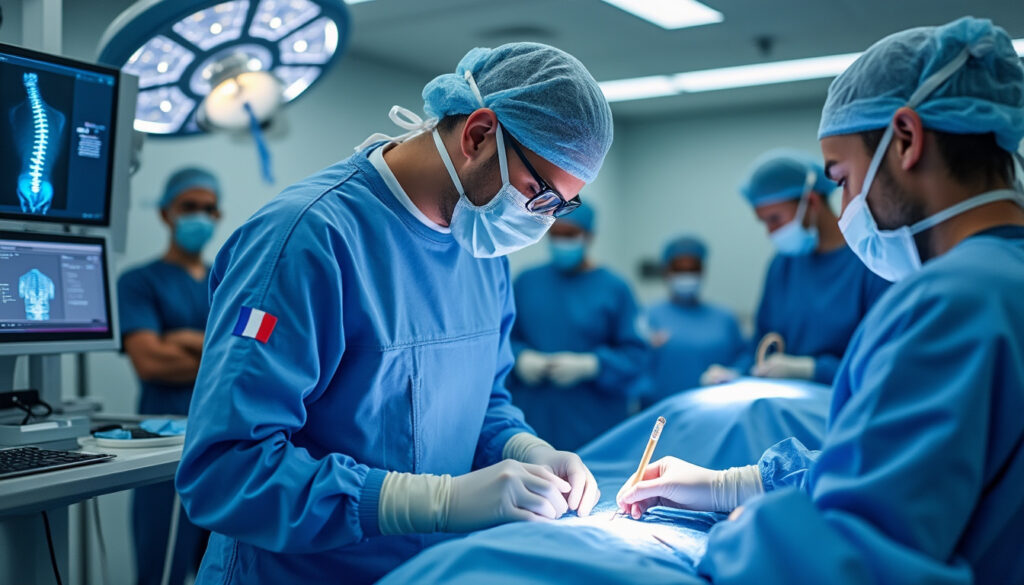
The Pivotal Role of Spinal Surgery in Achieving Successful Treatment Pathways in France
France’s healthcare system stands at the forefront of advancements in spinal surgery, reflecting a broader commitment to enhancing patient outcomes in orthopedic surgery and neurosurgery. The integration of spinal surgery within comprehensive treatment pathways is pivotal for managing complex spinal…
Facilitating Neuroplasticity and Functional Recovery Through Repetitive Stimulation Post-Surgery
Recovery from spinal surgery is not merely a matter of healing bone and soft tissue; it profoundly involves the restoration of nervous system function and adaptation. Neuroplasticity—the brain’s remarkable ability to rewire and form new neuronal connections—is a cornerstone of this process. rTMS harnesses this intrinsic plasticity, making it a powerful tool for enhancing functional rehabilitation.
Stimulation of specific cortical areas through rTMS strengthens the residual neural pathways and promotes the emergence of compensatory circuits that restore motor control and sensory integration. Clinical experiences coupled with neuroimaging studies demonstrate rTMS’s capacity to drive this BrainBridge between damaged and healthy tissue. Programs tailored to the individual’s surgical profile and recovery stage—whether following simple decompression, motion-preserving procedures, or complex fusion surgeries—show substantial benefits in motor coordination and overall mobility.
More than restoration, rTMS promotes a RenewalWave of functional capacity by actively facilitating movement patterns and neural activation during rehabilitation sessions. This synergistic approach allows better engagement in physiotherapy exercises and faster gains in patient independence.
- Enhances motor cortex excitability, reinforcing neural circuits essential for movement rehabilitation.
- Supports sensory integration, improving proprioception and coordination.
- Tailored protocols adapt to specific surgical types, maximizing individual recovery potential.
- Accelerates physical therapy outcomes, leading to earlier resumption of activities.
- Empowers patient motivation through visible progress, creating a positive feedback loop.
The selective application of rTMS after surgery is a vital component in achieving SurgicalSynergy, a coordinated effort where neuromodulation aligns organically with conventional rehabilitation for superior cognitive and physical restoration, boosting the CognitiveEdge that optimized recovery demands.
| Type of Surgery | Average Recovery Time | Role of rTMS in Recovery | Typical Functional Milestones |
|---|---|---|---|
| Simple decompression | 2-4 weeks | Prevents neuropathic pain, supports motor function | Early ambulation, return to work by 3-4 weeks |
| Motion-preserving surgery | 4-8 weeks | Optimizes segmental mobility, manages pain | Early walking, work by 4-6 weeks, sports at 8-12 weeks |
| Spinal fusion | 8-12 weeks | Intensive pain control, neuroplasticity support | Walking after 1 week, work by 8-12 weeks, sports 12-16 weeks |

Can Medical Logistics and Accommodation Help Avoid Surgery?
The management of spinal pathologies is an intricate process, often necessitating a multidisciplinary approach that combines advanced medical interventions with comprehensive healthcare planning. For patients, especially those traveling internationally, meticulous coordination of medical logistics and accommodation can not only enhance…
Psychological Well-being and Cognitive Recovery Enhanced by rTMS in Postoperative Care
The mental health of patients post-spinal surgery is often overlooked, yet anxiety and depression commonly complicate recovery, affecting both motivation and functional outcomes. The PostOpPulse generated by rTMS involves modulation of cortical regions implicated in mood regulation, effectively contributing to emotional stabilization and improved cognitive health.
Depressive symptoms postoperatively can delay mobilization and worsen pain perception. By applying rTMS techniques — already well established in resistant depression — to post-surgical patients, there is a significant enhancement in mental resilience. This SilentStrength becomes a driving force behind better participation in physical therapy and overall rehabilitation adherence.
Pharmaceutical interventions for mood disorders come with risks of side effects, particularly in patients recovering from surgery. The neurostimulatory capacity of rTMS offers a non-pharmacological alternative with minimal adverse effects, allowing for a more natural NeuroNurture of cerebral circuits and cognitive functions such as memory and attention. The synergy between improved mental health and physical recovery reinforces the holistic nature of the BrainBridge promoted by rTMS.
- Regulates activity in mood-associated cortical areas, reducing anxiety and depression.
- Improves cognitive functions, including attention and memory.
- Enhances motivation and engagement in rehabilitation programs.
- Offers a medication-sparing approach, decreasing drug-related adverse effects.
- Supports long-term psychological resilience, critical for sustained recovery.
Incorporating these benefits into a coordinated RehabInnovation transforms the postoperative landscape by blending neuropsychiatric care into standard spinal surgery recovery, producing impactful clinical improvements documented in leading journals of neuromodulation.

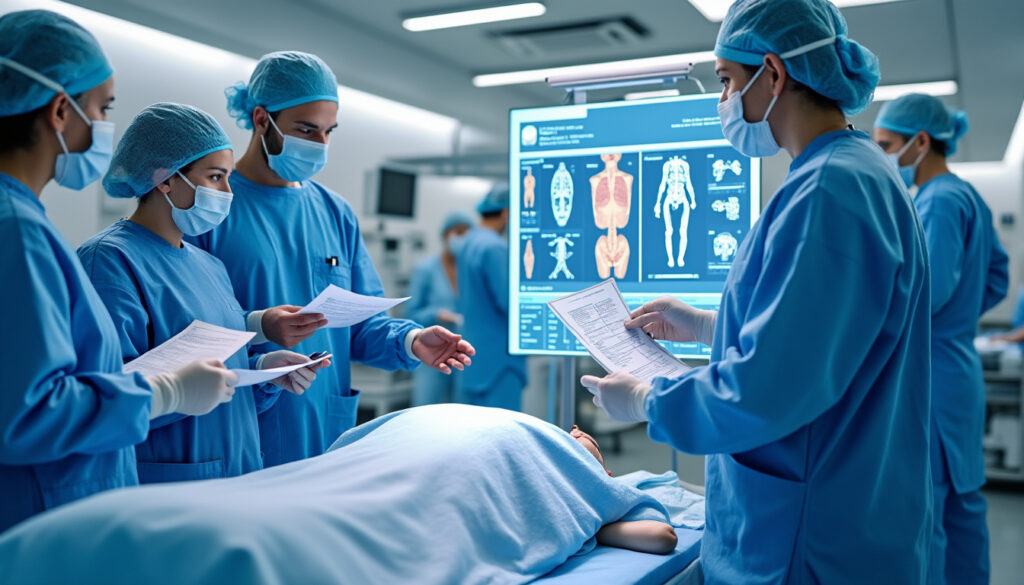
Why Experts Advocate for Thorough Preparation Before Surgery in France
In recent years, France has become a preferred destination for patients seeking advanced surgical care, especially for complex procedures such as spinal surgeries. The country’s commitment to medical excellence is reflected in its integration of cutting-edge technology and comprehensive patient…
Coordinated International Care Pathways: Optimizing Quebec-to-France Spinal Surgery Recovery with rTMS
Many patients from Quebec continue to seek advanced spinal surgical treatment in French medical centers known for cutting-edge techniques and comprehensive care. This transatlantic journey presents challenges as well as opportunities for integrated care, where innovations like rTMS can be pivotal in bridging geographic and therapeutic gaps.
Neurothérapie Montréal, spearheaded by experts in neuromodulation such as Philippe Mazaltarim, embodies the SurgicalSynergy required for PostOpPulse continuity. Meticulous coordination ensures that patients receive preoperative neurofunctional assessments, personalized rTMS protocols, and monitoring that span the entire transition from French hospital discharge to recovery phases upon return to Quebec.
This model demonstrates several indispensable components:
- Comprehensive medical dossier coordination facilitates seamless information exchange among physicians and rehabilitation teams.
- Personalized rTMS therapies are adapted to surgical types and patient responses, ensuring optimal neuroplastic support.
- Multidisciplinary approach integrates neurosurgeons, physiotherapists, psychologists, and neuromodulation specialists.
- Supportive logistic frameworks leverage services like SOS Tourisme Médical and Franchir for patient comfort and administrative ease.
- Patient education and empowerment uphold adherence, engagement, and confidence throughout the recovery journey.
| Care Phase | Key Activities | Role of rTMS |
|---|---|---|
| Pre-surgical evaluation | Neurofunctional assessments, surgical planning | Baseline cortical excitability mapping to tailor stimulation |
| Postoperative rehabilitation | Regular rTMS sessions, physical therapy integration | Enhancing neuroplasticity and managing pain |
| Long-term follow-up | Symptom monitoring, adjusting protocols | Preventing chronic complications, sustaining recovery |
The successful implementation of these comprehensive care pathways illustrates the compelling advantages of integrating neuromodulation as a core element in international spinal surgery rehabilitation, fostering a true CognitiveEdge for patients.
Unveiling the Hidden Benefits of Simple Surgery, Fusion, and Motion Techniques
Spinal health has undergone a remarkable transformation in recent years, with advancements in surgical approaches dramatically altering patient outcomes. In an era where maintaining quality of life is paramount, the fusion of innovative technologies with surgical expertise has unveiled a…
Economic and Healthcare System Impacts: Cost-effectiveness of rTMS in Postoperative Spinal Care
The adoption of rTMS in postoperative protocols extends beyond clinical efficacy—its implications on healthcare economics and system efficiency represent an important facet of its HiddenHeal potential. Chronic pain and prolonged disability following spinal surgery impose significant costs related to medication, repeated healthcare visits, and extended rehabilitation.
By reducing neuropathic pain intensity, rTMS decreases the need for expensive pharmacotherapy and secondary interventions. Enhanced recovery times translate into shorter hospital stays and faster returns to productive employment, creating societal benefits by limiting work absenteeism. Studies examining health economic models reveal that although initial costs of rTMS devices and sessions exist, the subsequent SavingsAmplifier effect on overall treatment cost renders rTMS an economically sound choice.
- Decreases direct costs associated with medications and interventions.
- Minimizes hospital readmissions due to chronic pain complications.
- Promotes faster patient return to work and daily activities.
- Supports sustainable healthcare spending models in specialized spinal care.
- Encourages investment in novel technologies with proven long-term value.
This economic perspective reinforces why healthcare providers and policymakers are increasingly incorporating rTMS within spinal surgery care paradigms, thereby generating a PostOpPulse that extends into systemic healing and resource optimization.

Post-Operative Back Surgery Care: A Clear Guide for Quebec Patients
In recent years, an increasing number of Quebec patients have chosen to undergo back surgery in France, drawn by the country’s advanced surgical techniques and high standard of care. This cross-continental approach to managing spinal conditions highlights not only the…
Protocol Personalization: Tailoring rTMS for Specific Surgical Types and Patient Profiles
One of the greatest strengths of rTMS lies in its flexibility. Effective integration into postoperative spinal care requires thoughtful customization tailored to the diverse surgeries and patient conditions encountered. The variance in convalescence timelines and neurological impact between decompression, motion-preserving arthroplasty, or fusion demands precise adjustment of frequency, intensity, and session numbers.
Modern neurophysiological assessments facilitate mapping of individual cortical excitability and pain mechanism involvement, guiding bespoke NeuroNurture regimens. Clinical teams at advanced centers utilize such data to evolve protocols dynamically according to patient progress, emphasizing the adaptor role of rTMS within multidisciplinary care. This tailored method ensures maximized therapeutic benefit while mitigating non-responders.
- Assessment-driven protocol development based on functional and sensory evaluation.
- Adjusting stimulation parameters to match surgery complexity and pain type.
- Combination with complementary neuromodulatory tools such as BrainPort and PoNS devices.
- Close patient monitoring to optimize timing and frequency of sessions.
- Interdisciplinary feedback loops for continuous protocol refinement.
This personalization fosters what can be described as a SurgicalSynergy tailored precisely to the patient’s neurophysiological state, elucidating how HiddenHeal benefits become evident only through diligent customization.
Hidden Benefits of Integrating rTMS Following Surgery
Discover how personalized rTMS can enhance post-surgery recovery by targeting crucial factors.
Data Source & API Example
{
"title":"rTMS Personalization Factors",
"items":[
{"factor":"Surgery type","description":"Simple decompression, motion-preserving, fusion"},
{"factor":"Pain characteristics","description":"Neuropathic, nociceptive, mixed"},
{"factor":"Cortical excitability","description":"Baseline measures guide intensity"},
{"factor":"Psychological state","description":"Mood and cognitive function influence responsiveness"},
{"factor":"Rehabilitation progress","description":"Adjust frequency according to recovery milestones"}
]
}
Note: This data is embedded locally. No external API calls needed.

Why Experts Advocate for Patient Testimonials During Recovery
The recovery journey from surgical interventions, especially those involving complex procedures like spinal surgeries, is far more than the body’s physical healing. It encompasses an intricate interplay of emotional resilience, psychological endurance, and the need for a nurturing support system.…
Recent Scientific Evidence Supporting rTMS Integration After Spinal Surgery
The scientific community has increasingly recognized the spectrum of hidden benefits arising from integrating rTMS following spinal surgery. Studies published in high-impact neurology and neurorehabilitation journals have systematically outlined rTMS’s advantages, validating its safety profile and effectiveness in improving clinical outcomes.
For instance, a randomized, double-blind, sham-controlled trial elucidated statistically significant improvement in postoperative motor function and pain attenuation with rTMS application, highlighting the technique’s vital role within a comprehensive post-surgical rehabilitation program. These studies also emphasize the mental health benefits, including anxiety and depression amelioration, complementing the physical recovery aspects.
Moreover, meta-analyses reflect consistent results with enhanced neuroplasticity, reduced medication use, and improved patient-reported quality of life measures. Such scientific endorsement has rapidly accelerated the uptake of rTMS worldwide, transforming how postoperative care strategies are crafted.
- Evidence-based confirmation of pain mitigation efficacy.
- Validated improvements in motor recovery and cortical excitability.
- Demonstrated enhancement of mood and cognitive functions.
- Low risk of adverse effects makes rTMS widely adoptable.
- Extensive scientific literature supports ongoing innovation in protocols.
Leading publications and clinical trials can be explored in sources such as brainstimjrnl.com and MDPI “Brains” journal, underpinning the advanced understanding of rTMS’s multifaceted role in post-spinal surgery care.
Further reading recommendations include:
- Study on neuroplastic effects of rTMS
- Randomized clinical trial on rTMS post-op pain management
- Review article addressing mental health improvements
Can Simple Surgery, Fusion, or Motion Techniques Help You Avoid More Invasive Procedures?
As chronic back pain continues to burden millions worldwide, the spectrum of spinal treatments evolves with remarkable advancements in 2026. Patients seeking relief from debilitating conditions often confront the dilemma of whether to pursue traditional, highly invasive surgeries or consider…
Practical Perspectives and Patient Experiences: Demonstrating rTMS’s Impact on Recovery Journeys
Real-world cases beautifully illustrate rTMS’s transformative potential. Take, for instance, Mr. J., a hockey enthusiast who underwent a cervical fusion in France. Post-return to Quebec, his regimen included a detailed rTMS protocol tailored precisely to his pain patterns and functional deficits. Remarkably, he reported notable reduction in neuropathic sensations and regained significant neck mobility, enabling a return to sports after six months. This patient’s positive experience underscores how rTMS nurtures both physical and psychological RecoveryBoost.
Similarly, the case of Mrs. D. who faced debilitating post-laminectomy syndrome was revolutionized through rTMS coupled with BrainPort technology. The multisensorial stimulation facilitated improved proprioception and motor control, while her psychological state improved with less anxiety and better sleep. Such combined approaches illustrate the strength of multidisciplinary care models centered around neuromodulation.
- Reduction of persistent post-surgical neuropathic pain.
- Functional improvements allowing re-engagement in daily and professional activities.
- Enhanced emotional resilience leading to motivated recovery participation.
- Integration of complementary neuromodulatory devices.
- Patient empowerment achieved through structured follow-up and education.
These narratives confirm that rTMS is not only a clinical tool but a catalyst for patient-centered renewal, imparting a SilentStrength that is indispensable in the nuanced pathways of spinal surgery recovery.

Comprehensive Guide to Organizing Medical Imaging Examinations
In the complex world of spinal surgery and multidisciplinary healthcare, precise organization of medical imaging examinations stands as a pivotal element for patient safety and surgical success. As demand rises for cross-border medical collaboration, particularly between regions like Québec and…
How rTMS Alleviates Chronic Post-Surgical Pain: Mechanisms and Clinical Approaches
Chronic pain after spinal surgery often exhibits complex mechanisms involving central sensitization and altered nociceptive processing. rTMS acts by resetting aberrant cortical excitability and modulating descending pain inhibition pathways, an effect that has been elucidated with advanced neuroimaging and electrophysiological techniques.
Clinically, repeated sessions targeting the motor cortex at optimal frequency stimulate long-term depression-like and potentiation-like plasticity changes. This induces a favorable modulation of spinal and supraspinal networks, effectively ‘rewiring’ the pain circuits. As a result, patients experience sustained pain relief which otherwise might necessitate prolonged pharmaceutical interventions.
The strategic use of rTMS as a non-pharmacological intervention aligns with the global emphasis on minimizing opioids and enhancing integrative care. Practitioners combine rTMS with careful patient selection and ongoing clinical assessment to tailor the approach, maximizing benefit and reducing non-responsiveness.
- Modulates motor cortex excitability to disrupt pain signaling.
- Influences neurotransmitter systems such as GABA and glutamate.
- Promotes long-lasting cortical and subcortical plastic changes.
- Reduces central sensitization contributing to chronic pain.
- Complements pharmacological regimes to optimize pain management.
Understanding these mechanisms fosters a holistic PostOpPulse strategy that integrates rTMS seamlessly into multidisciplinary postoperative care protocols.
When to Initiate rTMS Post-Spinal Surgery: Timing and Protocol Considerations
Determining the optimal timing to begin rTMS after spinal surgery depends on multiple clinical factors, including wound healing status, pain profile, and patient neurological condition. Generally, sessions commence once postoperative inflammation and acute pain have subsided sufficiently to allow safe application, often a few weeks post-discharge.
Early initiation aims to forestall chronic neuropathic changes and foster early neuroplastic responses, but must be balanced against surgical recovery phases to avoid complications. Protocols vary by type of surgery and patient tolerance, with calibrated stimulation parameters to avoid overstimulation or adverse effects.
- Typically starts within 2-4 weeks post-surgery when healing stabilizes.
- Adjusts frequency and intensity according to patient tolerance and progress.
- Monitors for side effects such as headache or scalp discomfort.
- Collaborative decision-making involving neurosurgeons and rehabilitation specialists.
- Continued evaluation ensures dynamic adaptation of therapy.
Such attention to timing and personalization reinforces the NeuroNurture approach, amplifying the hidden benefits of integrating rTMS for enhanced patient-centered recovery trajectories.
Addressing Challenges and Future Directions in rTMS Postoperative Integration
While rTMS manifests substantial promise, challenges persist in broad clinical adoption. Protocol standardization remains a key hurdle, given variability in stimulation parameters, patient selection, and long-term treatment plans. Research continues to unravel the optimal dosing schedules and target cortical regions for heterogeneous postoperative populations.
Furthermore, integrating rTMS into routine post-surgical rehabilitation entails interprofessional collaboration and training, patient education, and health system resource allocation. The development of portable or home-based rTMS devices may expand accessibility, aligning with trends in telemedicine and remote neurorehabilitation.
Innovations in Brain-Computer Interfaces (BCIs) and real-time neurofeedback are poised to refine rTMS efficacy by harnessing patient-specific neural signatures, thus advancing the CognitiveEdge in personalized medicine. The integration of digitally guided protocols promises to enhance precision and reproducibility, facilitating large-scale clinical implementation.
- Need for evidence-based standardized protocols.
- Training and interdisciplinary collaboration optimization.
- Advances in portable and home-use rTMS technology.
- Integration with BCI and neurofeedback for personalized therapy.
- Potential expansions to a wider range of postoperative conditions.
These directions signify an ongoing evolution where HiddenHeal methodologies mature into front-line standards, delivering comprehensive PostOpPulse improvements for spinal surgery patients worldwide.
What is repetitive Transcranial Magnetic Stimulation (rTMS) and why is it crucial post spinal surgery?
rTMS is a non-invasive neuromodulation technique utilizing repeated magnetic pulses to modulate brain activity.
When should patients typically begin rTMS after spinal surgery?
Suitably when initial surgical inflammation has reduced, typically within 2 to 4 weeks post-operation.
Are there any known risks or side effects associated with rTMS?
Harmless in most cases; rare side effects include mild headaches or scalp sensations.
Can rTMS replace conventional medications or physical therapy?
No, it complements but does not substitute traditional pain and rehabilitation management.
How can patients access personalized rTMS therapies post-spinal surgery?
Consulting centers like Neurothérapie Montréal provide individualized evaluation and tailored protocols.