Understanding Disc Herniation in the Southwest: The Top 3 Warning Signs and Neurovertebral Decompression Treatments
November 3, 2025
Understanding Disc Herniation in Mercier–Hochelaga-Maisonneuve: A Beginner’s Patient Guide to Neurovertebral Decompression Therapy
November 3, 2025As spinal surgery advances through 2025, the landscape of implant technology is witnessing groundbreaking transformations. Innovations such as the TOPS System, Intraspine, and ESP implants are revolutionizing treatment paradigms by prioritizing motion preservation and individualized patient care. These pioneering technologies, supported by leading global medical device companies including Medtronic, Zimmer Biomet, and Stryker, offer dynamic alternatives to traditional spinal fusion, reducing postoperative complications and enhancing long-term spinal function. The convergence of advanced biomaterials, minimally invasive techniques, and refined surgical navigation heralds a new era for patients, especially those from regions like Quebec, who seek sophisticated solutions beyond conventional methods.
Central to this evolution is the shift from rigid spinal fusions that historically immobilize spinal segments, to motion-preserving implants designed to maintain physiological movements. This paradigm enables better preservation of adjacent segment health and minimizes degenerative changes. Global coordinated care pathways facilitate seamless access for international patients, including a comprehensive approach from initial evaluation through surgery and follow-up rehabilitation. Supported by expert clinician networks and technological progress in robotics and navigation, these innovations not only mitigate risks but also redefine patient recovery trajectories.
Understanding the TOPS System: Revolutionizing Lumbar Spine Surgery with Motion Preservation
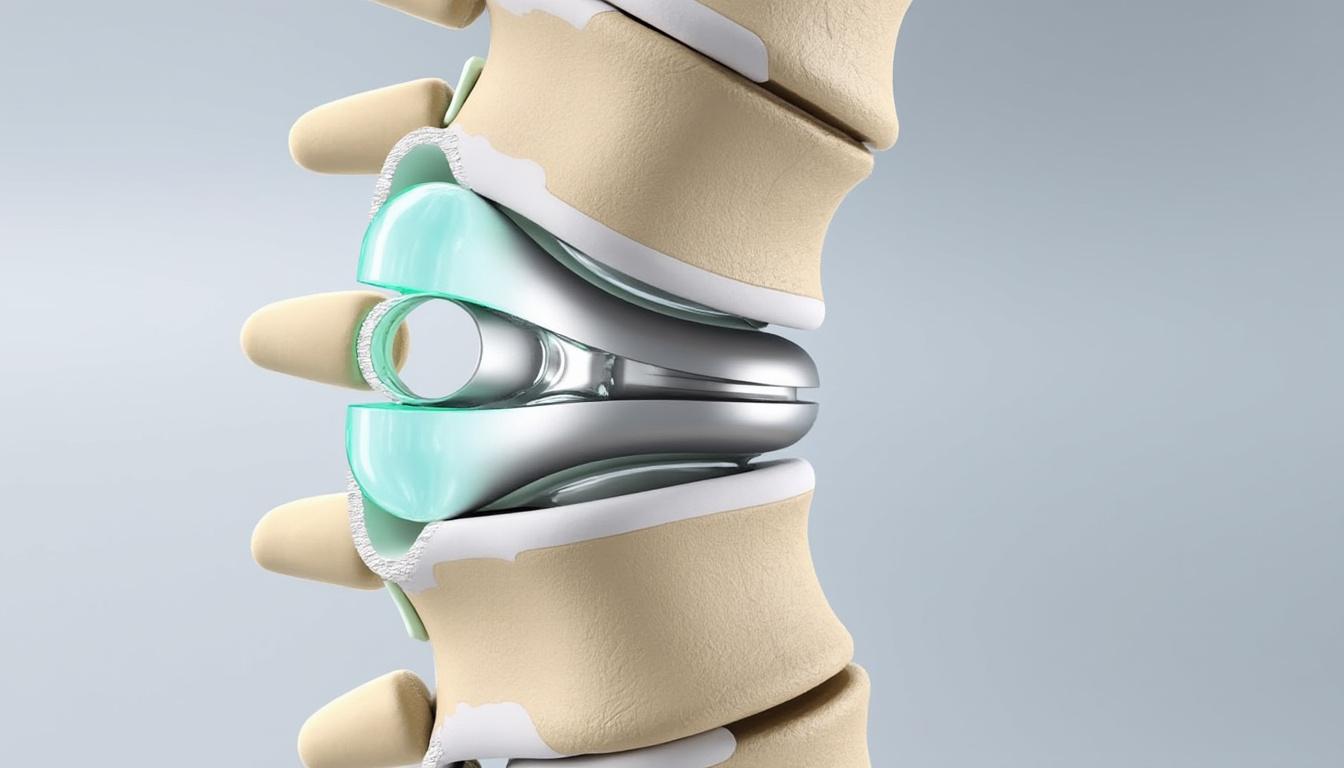
The TOPS (Total Posterior Solution) System marks a significant departure from traditional lumbar fusion methods. Unlike fusion that eliminates intervertebral motion to stabilize a spinal segment, the TOPS implant offers a multidirectional stabilization mechanism while preserving the spine’s natural range of motion. Engineered with biocompatible titanium and high-grade stainless steel, this sophisticated device controls flexion, extension, axial rotation, and lateral bending, reducing the risk of adjacent segment disease typically associated with rigid fusion.
Developed with input from industry leaders such as DePuy Synthes and Zimmer Biomet, the TOPS implant addresses common pathologies including lumbar spinal stenosis, spondylolisthesis, and facet joint arthrosis. Clinical trials, notably the pivotal FDA study involving over 300 patients, have demonstrated favorable outcomes in terms of pain relief, functional improvement, and reduced revision surgery rates compared to fusion. The system integrates seamlessly with minimally invasive surgical approaches enhanced by advanced peroperative navigation systems, which optimize implant placement and reduce tissue trauma.
- Preservation of natural spinal biomechanics: Enables physiological motion postoperatively.
- Reduction of postoperative pain: Balanced load distribution lowers stress on adjacent vertebrae.
- Enhanced implant durability: Utilizes high-quality titanium alloys ensuring long-term stability.
- Minimally invasive implantation: Advanced surgical techniques limit tissue damage and accelerate recovery.
| Criteria | Traditional Fusion | TOPS System |
|---|---|---|
| Postoperative Mobility | Immobilization of segment | Maintains functional spinal movement |
| Risk of Adjacent Segment Degeneration | High risk due to rigidity | Reduced with dynamic stabilization |
| Postoperative Pain Levels | Variable, often significant | Usually lower due to load balance |
| Recovery Duration | Extended | Typically faster recovery |
For patients in regions like Quebec, preoperative evaluation is often supervised by specialists such as Dr. Sylvain Desforges at the Clinique TAGMED. Once surgical candidacy is confirmed, coordinated pathways such as SOS Tourisme Médical enable efficient patient transfer to expert surgical centers in France, ensuring a seamless and high-quality care continuum. Advanced guidance throughout the surgical journey and postoperative rehabilitation optimizes outcomes, offering a modern alternative to lumbar fusion with tangible quality-of-life improvements.

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…
Intraspine and ESP Implants: Dynamic Alternatives for Lumbar Stability and Mobility
Alongside the TOPS System, dynamic interlaminar implants such as Intraspine and ESP (Elastic Spine Pad) have emerged as compelling options for patients with moderate lumbar instability or mild spinal stenosis. These devices aim to provide controlled segmental stabilization while preserving essential spinal motion, reducing the drawbacks linked to traditional fusion approaches.
The Intraspine implant, designed by companies like NuVasive and Implant Direct, is positioned between the spinous processes, delivering mechanical support to the lumbar segment without rigid fixation. This modality allows the preservation of flexion-extension movements, while minimizing facet joint overload. Its minimally invasive implantation technique ensures reduced operative time and faster discharge, making it attractive for patients seeking a less aggressive intervention.
In contrast, the ESP implant leverages high-density polyethylene components that function as shock-absorbing cushions within the spinal segment. Developed with the expertise of Spineart and LDR Medical, ESP’s biomimetic properties help dissipate forces during spinal loading, mitigating pain and potential degenerative changes. Clinical evidence suggests improvements in neurogenic symptomatology and a lower incidence of adjacent level degeneration.
- Maintained segmental mobility: Dynamic stabilization allowing physiological spinal movements.
- Reduced surgical trauma: Minimally invasive insertion reduces operative risks and hospital stay.
- Satisfactory pain relief: Addresses neurogenic pain through mechanical decompression and stability.
- Customized application: Implants are selected based on individual anatomical and pathological characteristics.
| Feature | Intraspine | ESP |
|---|---|---|
| Implant Positioning | Interspinous space | Polyethylene cushioning inside spinal segment |
| Flexibility | Controlled vertebral movement | Shock absorption and biomimetic flexibility |
| Surgical Approach | Minimally invasive | Minimally invasive to standard |
| Indications | Moderate instability, mild stenosis | Neurogenic pain, prevention post decompression |
Patients seeking these treatments from Canada are often referred via platforms like Franchir to renowned surgical centers in Toulouse, Bordeaux, or Le Mans, where surgeons utilize cutting-edge technologies such as the KARL STORZ navigation system. This ensures that each operation is executed with precision and safety, enhancing patient outcomes and satisfaction. Postoperative care through clinics like Neurothérapie Montréal further supports functional recovery and monitors implant performance.

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Minimally Invasive Spine Surgery and its Synergy with Advanced Implants
Minimally invasive surgical (MIS) techniques have become integral to the success of modern spinal implants. By reducing tissue disruption and minimizing blood loss, MIS contributes directly to enhanced recovery profiles when combined with dynamic devices like TOPS, Intraspine, and ESP. In France, centers within the SOS Tourisme Médical network leverage innovations like endoscopic spine surgery, which digitally visualizes the operative field, allowing for precise decompression and implant placement through minimal incisions.
The advantages of MIS include less postoperative pain, shorter hospital stays, and quicker return to preoperative function. Studies published in journals focusing on spine innovations highlight that robotic-assisted navigation systems guide surgeons to optimal implant positioning, dramatically reducing the margin of error and enhancing patient safety. Companies such as Globus Medical and Alphatec Spine are pioneering integrated implant and robotic solutions that synergize perfectly with these implants’ dynamic properties.
- Enhanced surgical precision: Utilization of robotics and navigation reduces complications.
- Reduced postoperative discomfort: Smaller incisions and less muscle disruption.
- Shortened hospitalization duration: Faster mobilization and decreased morbidity.
- Improved patient satisfaction: Positive impact on quality of life and functional outcomes.
| Aspect | Traditional Surgery | Minimally Invasive Surgery with Advanced Implants |
|---|---|---|
| Tissue Damage | Extensive muscle and tissue disruption | Minimal muscle trauma |
| Blood Loss | Higher volumes | Significantly reduced |
| Hospital Stay | Several days | Typically 1-2 days |
| Recovery Time | Weeks to months | Days to weeks |
Such technical advances are critical to the tailored approaches used in treating Quebec patients, where access to precision surgery amplifies the benefits of dynamic spinal implants, ultimately improving patient journey experiences and healthcare resource utilization.

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…
International Surgical Pathways: Coordinating Care Between Canada and France
The increasingly global nature of advanced spinal surgery demands streamlined international care models. For residents in Quebec and broader Canada, partnerships like SOS Tourisme Médical and Franchir have established efficient patient routing to world-renowned spinal centers across France. These coordinated efforts facilitate every stage of care, from rigorous preoperative evaluations, including specialized neurovertebral decompression therapies at centers like Clinique TAGMED, to seamless surgical scheduling and logistical support.
This international framework addresses common challenges of cross-border medical travel with detailed attention to patient safety, comfort, and postoperative monitoring. Neurothérapie Montréal exemplifies advanced rehabilitation services ensuring continuity of care following discharge from French institutions. Additionally, established medical device infrastructure involving renowned brands like Medtronic and Zimmer Biomet ensures high-quality implant availability throughout the patient journey.
- Comprehensive pre-surgical evaluation: Conservative management overseen by specialized clinicians avoids premature surgery.
- Efficient surgical scheduling and logistics: Coordination of travel, accommodations, and operating room access with French centers.
- Robust postoperative follow-up: Telemedicine and in-person therapies for rehabilitation and monitoring.
- Access to certified implant technologies: Use of CE-marked devices adhering to international standards.
| Care Phase | Responsible Entity | Goals |
|---|---|---|
| Preoperative Evaluation | Dr. Sylvain Desforges / Clinique TAGMED | Assessment and conservative treatment trial |
| Surgical Orientation & Logistics | SOS Tourisme Médical / Franchir | Organize surgery and patient itinerary |
| Surgical Intervention | French Specialized Spine Centers | Application of advanced surgical and implant technologies |
| Postoperative Management | Neurothérapie Montréal | Rehabilitation and remote patient monitoring |
Through such synchronized international cooperation, patients benefit from minimized wait times, optimized treatment timing, and enhanced access to cutting-edge care beyond local healthcare system limitations. This model serves as a template for expanding access to evolving spinal implant technologies globally.

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
Advanced Materials and Technological Innovations Shaping the Future of Spinal Implants
Material science continues to propel implant innovation with the adoption of nanomaterials, biodegradable polymers, and 3D bio-printed custom implants now gaining traction. These advancements aim to enhance implant biocompatibility, reduce permanent foreign body presence, and tailor solutions to patient-specific anatomy.
Nanomaterials incorporated within titanium or composite frameworks dramatically improve mechanical strength while decreasing implant weight, reducing load on vertebral bodies. Simultaneously, the emergence of 3D bio-printing allows anatomically precise implants molded to individual spinal segments, minimizing fit-related complications and improving osseous integration. The integration of biodegradable polymers provides temporary stabilization with gradual tissue integration, minimizing long-term inflammation and foreign body reactions.
On the technological front, robotics and AI-driven surgical planning platforms are streamlining spine surgeries. Companies such as Globus Medical and Alphatec Spine are at the forefront, providing robotic systems that enhance implant trajectory accuracy, intraoperative feedback, and patient-specific adjustments. The adoption of wireless connected implants introduces possibilities for postoperative real-time monitoring, enabling responsive therapeutic adaptations aimed at maintaining spinal health dynamically over time.
- Nanomaterials: Increased strength and reduced implant weight.
- 3D bio-printing: Precise anatomical customization.
- Biodegradable polymers: Temporary scaffolding with reduced immune response.
- Robotics & AI: Enhanced surgical accuracy and efficiency.
- Connected implants: Real-time postoperative surveillance and intervention.
| Innovation | Expected Benefit | Potential Impact on Spine Surgery |
|---|---|---|
| Nanomaterials | Mechanical reinforcement, lightness | Longer implant longevity and reduced vertebral stress |
| Bio-printed implants | Custom anatomical adaptation | Minimized complications through perfect fit |
| Biodegradable Polymers | Reduced chronic foreign body presence | Lower inflammation and improved tissue integration |
| Robotics & AI | Precision and personalized surgery | Minimized surgical errors and accelerated recovery |
| Connected systems | Continuous postoperative monitoring | Dynamic treatment adjustments to patient needs |
As these innovations intersect, the future of spinal implants will be marked by patient-tailored devices and procedures that improve longevity, function, and clinical outcomes. The integration of high-tech robotic platforms and connected implant monitoring will empower surgeons in managing complex spinal disorders more effectively than ever before.


International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…
Expert-Led Insights on Patient Selection and Surgical Decision-Making with TOPS, Intraspine, and ESP
The decision to proceed with surgical intervention versus conservative management remains pivotal. Specialists underscore the importance of a thorough assessment protocol where patients undergo careful evaluation, including at facilities such as Clinique TAGMED with therapies like neurovertebral decompression, to optimize outcomes and avoid unnecessary surgery.
The innovative implants TOPS, Intraspine, and ESP offer diversified options tailored to pathology severity and patient anatomy. The clinical advantage lies in their motion-preserving designs that permit dynamic stabilization instead of rigid fixation, potentially reducing chronic pain and improving postoperative mobility.
Key selection criteria for these implants include symptom chronicity, imaging findings, segmental instability degree, and patient lifestyle requirements. For example, TOPS is often indicated for patients with degenerative lumbar stenosis combined with spondylolisthesis, where preserving multiple plane movement is crucial. Intraspine or ESP implants may be preferred in cases with moderate instability or mild to moderate stenosis where less invasive and flexible solutions suffice.
- Comprehensive clinical and radiological evaluation.
- Preliminary conservative treatment trial (3–6 months).
- Consideration of patient activity levels and expectations.
- Precise matching of implant choice to pathology severity.
- Integration with minimally invasive techniques for faster recovery.
| Implant | Primary Indication | Patient Benefit Focus |
|---|---|---|
| TOPS | Degenerative stenosis and spondylolisthesis | Motion preservation and multi-plane stability |
| Intraspine | Moderate instability and mild stenosis | Segmental support with controlled flexibility |
| ESP | Neurogenic pain, post decompression prevention | Shock absorption and symptom relief |
Surgeons utilize refined diagnostic frameworks and clinical scoring systems to match implants to individualized treatment plans. The combination of technological sophistication and clinical expertise enhances decision-making, particularly important for Canadian and Quebec patients benefiting from advanced transatlantic care coordination.

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
Clinical Outcomes and Long-Term Benefits Demonstrated in Advanced Implant Use
Longitudinal studies confirm that motion-preserving implants such as TOPS, Intraspine, and ESP deliver superior patient outcomes compared to traditional fusion in specific clinical contexts. Patients report improved functional status, lower opioid use postoperatively, and better maintenance of spinal mobility.
For instance, published clinical data reveal that TOPS recipients experience higher rates of return to work and daily activities without recurrent pain. Additionally, these implants demonstrate lower revision surgery requirements, attributable to decreased adjacent segment degeneration. Similar findings apply to Intraspine and ESP implants, which reduce neurogenic pain symptoms effectively while preserving spinal dynamics.
- Enhanced functional performance documented over 2–5 years.
- Reduced incidence of adjacent segment disease.
- Improved patient satisfaction and quality of life metrics.
- Lower complication and reoperation rates.
- Support for faster rehabilitation and return to active lifestyle.
| Outcome Measure | TOPS System | Traditional Lumbar Fusion |
|---|---|---|
| Functional Mobility | Maintained in multiple planes | Reduced due to rigidity |
| Postoperative Pain Intensity | Lower scores reported | Moderate to high pain levels |
| Adjacent Segment Disease Rate | Significantly reduced | Higher incidence |
| Revision Surgery Rate | Lower | Higher |
| Return to Work Timeline | Typically within months | Often delayed |
These clinical advantages corroborate the strategic shift toward dynamic spinal stabilization supported by manufacturers like Medtronic and Zimmer Biomet. Patient testimonials and surgeon reports emphasize enhanced comfort, trust in implant durability, and broad applicability of these devices across diverse degenerative spinal conditions.

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…
Future Directions in Spinal Implant Technology: Integration of AI, Robotics, and Smart Devices
The integration of artificial intelligence and robotics within spinal surgery opens unprecedented avenues for elevating implant performance and surgical accuracy. Emerging platforms now utilize real-time imaging, AI-guided implant positioning, and smart-connected implants capable of continuous biomechanical monitoring. This dynamic feedback loop allows personalized adjustments in therapy and early complication detection, substantially augmenting patient safety and outcomes.
Companies like Alphatec Spine and Globus Medical are pioneering AI-based robotic assistance tools that support surgeons through augmented reality overlays and predictive analytics, reducing operation times and improving precision. The use of wireless-enabled implants signals a future where spinal health can be tracked seamlessly postoperatively outside hospital settings, enabling proactive care adjustments tailored to individual biomechanical demands.
- AI-driven surgical planning and intraoperative guidance.
- Robotic-assisted implant placement with enhanced accuracy.
- Wireless-connected implants for continuous postoperative monitoring.
- Predictive analytics for early detection of implant complications.
- Enhanced patient engagement through digital health platforms.
| Technological Advancement | Benefit | Clinical Impact |
|---|---|---|
| AI Surgical Systems | Precision and operative efficiency | Reduced complications and improved recovery |
| Robotic Navigation | Optimal implant positioning | Better biomechanical outcomes |
| Connected Implants | Real-time monitoring | Personalized postoperative care |
These forward-looking advancements epitomize the fusion of engineering innovation and clinical expertise, promising a new standard in spinal surgery that emphasizes precision, personalization, and improved patient outcomes. Canadian patients, collaborating with international centers, stand to benefit immensely from these evolving technologies.
Comparison of Pioneering Spinal Implants
| Feature | TOPS | Intraspine | ESP |
|---|
What are the main advantages of the TOPS implant compared to traditional fusion?
The TOPS System stabilizes the spine while preserving physiological motion, reducing postoperative pain and adjacent segment degeneration, resulting in better long-term quality of life.
How is the surgical pathway organized for Quebec patients considering these innovative implants?
Initial evaluation and conservative treatments are supervised by Dr. Sylvain Desforges at Clinique TAGMED. SOS Tourisme Médical and Franchir coordinate surgical orientation and logistics in France, with postoperative follow-up managed by Neurothérapie Montréal.
What are the primary indications for dynamic implants like Intraspine and ESP?
These implants are indicated for moderate spinal instabilities, mild to moderate spinal stenosis, and situations requiring stabilization without excessive rigidity, aiming to preserve spinal mobility.
Are the materials used in TOPS implants biocompatible and durable?
Yes, TOPS implants primarily use medical-grade titanium, specialized stainless steel, and high-density polyethylene, ensuring excellent biological tolerance and mechanical stability over time.
Can surgery be avoided through conservative treatments?
A conservative treatment protocol lasting 3 to 6 months, such as neurovertebral decompression at Clinique TAGMED, is essential before considering surgery and may sometimes alleviate symptoms sufficiently.

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…