The diagnosis of a herniated disc requires a meticulous approach that combines a detailed medical history, thorough physical examination, and, when necessary, advanced diagnostic tests. Herniated discs remain a prevalent cause of back and neck pain, affecting millions each year worldwide. Given the critical role spinal health plays in overall mobility and quality of life, accurate diagnosis is the first crucial step towards effective treatment and management.
In clinical settings such as Dr. Sylvain Desforges’ TAGMED Clinics in Québec, emphasis is placed on non-invasive, evidence-based methods, reflecting his 30+ years of expertise in spinal care. By adopting a comprehensive evaluation strategy, patients receive personalized insights into the precise nature of their spinal disorder, supporting targeted interventions that can significantly alleviate symptoms without resorting to surgery. The diagnostic process also considers neurological function, as nerve involvement often underlies the symptoms experienced by patients with herniated discs.
Thorough Medical History: The Foundation for Accurate Herniated Disc Diagnosis
The foundation of diagnosing a herniated disc begins with collecting an extensive medical history. A health care professional, such as Dr. Sylvain Desforges, asks about the onset, nature, and triggers of the patient’s symptoms to identify patterns that suggest nerve root irritation or spinal pathology.
- Symptom onset and progression: Patients are asked when the pain began, whether it was sudden or gradual, and how symptoms have evolved.
- Character and localization of pain: Descriptions include whether the pain is sharp, dull, constant, or intermittent, and whether it radiates down the arms or legs.
- Aggravating and relieving factors: Activities such as lifting, twisting, or prolonged sitting might worsen symptoms, while rest or specific postures may alleviate them.
- History of trauma or injury: Prior accidents or strains affecting the back are key information for differential diagnosis.
- Neurological symptoms: Patients report any numbness, tingling, weakness, or bowel/bladder function changes that suggest nerve involvement.
- Psychological factors: Given the impact of chronic pain on mental health, information about anxiety or depression aids in holistic care planning.
This detailed history is essential to differentiate herniated disc symptoms from other causes of back pain like muscular strain or spinal infections. Understanding individual patient experiences allows for tailored evaluations and treatment plans.
| Medical History Detail | Purpose for Herniated Disc Diagnosis |
|---|---|
| Symptom Timeline | Identifies acute or chronic nature |
| Pain Characteristics | Distinguishes disc-related pain from other etiologies |
| Activity Impact | Correlates symptoms with mechanical stressors |
| Neurological Complaints | Indicates potential nerve root compression |
| Psychological Assessment | Enhances treatment personalization |
For patients seeking expert evaluation, understanding that a comprehensive history combined with carefully considered physical and diagnostic tests leads to a more accurate diagnosis can empower them to engage meaningfully with their providers. Dr. Desforges’ practice highlights the importance of a compassionate and detailed listening approach to ensure every patient’s unique situation is appropriately understood and managed.
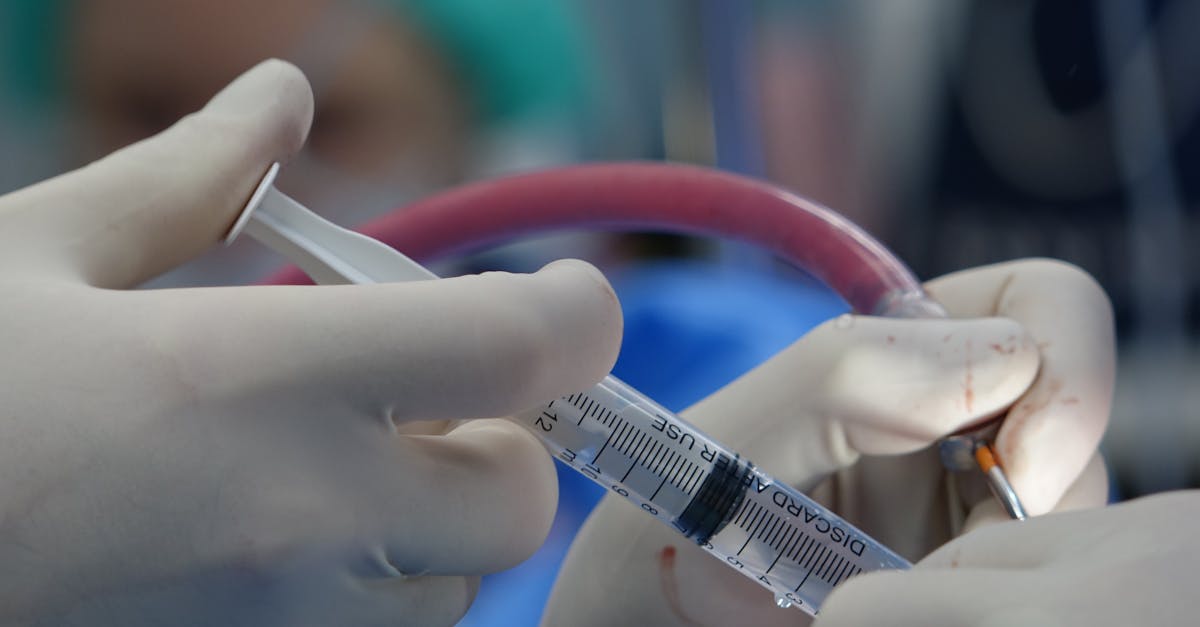
Physical Examination Techniques to Assess Herniated Disc Symptoms
Following the medical history, a physical exam is pivotal for evaluating the presence and impact of a herniated disc. This exam typically includes palpation and movement assessments, complemented by neurological testing to examine nerve function.
- Tenderness Evaluation: The clinician checks the back for areas that elicit pain when touched or pressed, helping localize symptomatic regions.
- Range of Motion Assessment: Patients perform movements such as bending forward, backward, and side to side to detect limitations or symptom provocation.
- Straight Leg Raise (Lasegue) Test: The patient lies flat while the leg is raised without bending the knee. Pain radiating down the leg during this maneuver often indicates sciatic nerve irritation from a lumbar herniated disc.
- Crossed Straight Leg Raise Test (Fajersztajn sign): Raising the unaffected leg causes pain in the opposite leg, suggesting nerve root compression.
- Neurological Reflex Testing: Tendon reflexes such as the patellar or Achilles reflex are assessed to identify diminished or absent responses linked to specific nerve roots.
- Muscle Strength and Sensation: Strength tests of lower extremity muscles and sensory evaluation to pinpricks, light touches, or vibration help map affected nerves.
Such comprehensive assessments demand skilled interpretation, with Dr. Desforges bringing his decades-long clinical experience to ensure precise evaluation. Variation in patient responses requires personalized analysis rather than a one-size-fits-all approach, recognizing the complexity of spinal nerve interactions.
| Physical Test | Purpose | Expected Finding if Herniated Disc Present |
|---|---|---|
| Tenderness Check | Pinpoints painful regions on the spine | Localized pain on palpation |
| Range of Motion | Assesses spinal flexibility and symptom triggers | Reduced motion with pain at extremes |
| Straight Leg Raise Test | Detects sciatic nerve irritation | Radiating leg pain between 30-70 degrees of elevation |
| Crossed Leg Raise Test | Confirms nerve root involvement | Pain in contralateral leg on raising unaffected leg |
| Reflexes Testing | Identifies affected nerve roots | Diminished or absent tendon reflexes |
| Muscle Strength | Evaluates nerve motor function | Weakness in specific muscle groups |
Mastering these physical tests is essential for non-surgical spinal care experts. Patients benefit from accurate localization and assessment of their symptoms, guiding subsequent treatment steps such as conservative management or advanced diagnostics.
Advanced Imaging Modalities Crucial for Confirming Herniated Disc Diagnosis
While clinical examination suffices in many cases, advanced imaging drastically improves diagnostic accuracy and surgical planning. As part of Dr. Sylvain Desforges’ protocol at TAGMED, cutting-edge technologies from providers such as Siemens Healthineers, Philips Healthcare, and GE Healthcare are integrated to capture high-resolution spinal images.
- Magnetic Resonance Imaging (MRI): Regarded as the gold standard, MRI uses magnetic fields and radio waves to visualize soft tissues, intervertebral discs, and nerves. Its superior contrast resolution reveals the precise location and size of herniations.
- Computed Tomography (CT) Scan: CT provides detailed cross-sectional images of bone and soft tissues, often performed with myelography to visualize nerve root compression through injected contrast into cerebrospinal fluid.
- X-rays: Though X-rays do not show discs directly, they exclude other spinal abnormalities such as fractures, infections, tumors, or vertebral misalignment that could mimic or complicate a herniated disc diagnosis.
- Myelogram: Injection of dye into the spinal canal followed by imaging highlights nerve impingement, beneficial when MRI is contraindicated or unclear.
The significance of these imaging techniques lies in their ability to corroborate physical findings and help tailor treatment strategies. For instance, MRI results guide the application of non-surgical spinal decompression therapy or determine surgical necessity. Moreover, advanced imaging is indispensable before any invasive intervention for safety and precision.
| Imaging Modality | Visualizes | Clinical Use in Herniated Disc |
|---|---|---|
| MRI | Discs, nerves, spinal cord, soft tissues | Localization of herniation and nerve impact |
| CT Scan | Bones, soft tissues with contrast | Evaluation when MRI not possible; detail bone structures |
| X-ray | Bones only | Rule out fractures, alignment issues, tumors |
| Myelogram | Nerve roots and spinal canal with dye | Detect nerve compression in complex cases |
Patients interested in detailed diagnostics can explore more information about advanced imaging through sources such as NYU Langone Health’s guide and Barricaid’s blog on diagnostic tests. Expert use of these technologies in clinics like TAGMED assures high standards of safety and efficacy.
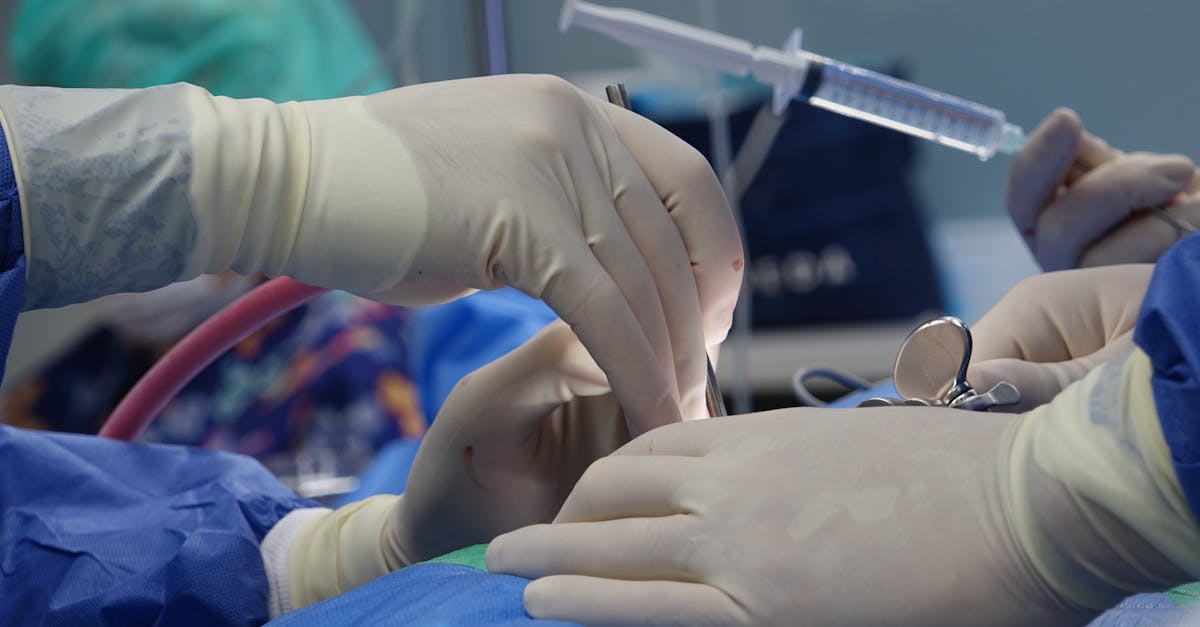
Electrophysiological Tests: Pinpointing Nerve Damage in Herniated Disc Cases
Electrophysiological testing plays an important role in assessing the functional status of spinal nerves and muscles affected by herniation. These tests help determine the extent and pattern of nerve damage, complementing imaging studies for a comprehensive evaluation.
- Nerve Conduction Studies (NCS): Measures the speed and strength of electrical signals traveling along nerves, identifying slowed conduction caused by compression or injury.
- Electromyography (EMG): Involves inserting needle electrodes into muscles to record electrical activity both at rest and during contraction, detecting denervation or impaired nerve input.
- Clinical Relevance: These tests assist in differentiating herniated discs from other neurological disorders and guide prognosis by assessing nerve recovery potential.
Dr. Sylvain Desforges emphasizes that interpretation of these tests requires nuanced clinical insight to correlate findings with symptoms accurately. Electrophysiological outcomes often influence treatment decisions, including candidacy for spinal decompression therapy or the urgency of surgical referral.
| Test | Method | Information Provided |
|---|---|---|
| Nerve Conduction Study | Surface electrodes on skin emit electrical stimuli | Speed and strength of nerve signal conduction |
| Electromyography (EMG) | Needle electrode inserted in muscle | Electrical activity of muscles and nerve-muscle interaction |
Patients considering this form of testing should seek care providers experienced in spinal neurology, ensuring results translate into optimal care pathways. TAGMED Clinics uphold strict compliance with clinical guidelines to maintain high ethical and safety standards in performing these studies.
Customizing Diagnostic Pathways for Individual Patient Needs
In the expert practice of Dr. Sylvain Desforges, a key principle is that each patient’s diagnostic journey is unique. Factors such as symptom severity, comorbidities, and personal preferences influence the selection and timing of diagnostic tests. This personalized approach ensures effective, minimally invasive intervention aligned with the patient’s health goals.
- Initial clinical evaluation: Most patients start with history and physical exam, often sufficient for initial management.
- Early imaging: Indicated in cases of trauma, progressive neurological symptoms, or suspicion of alternative diagnoses.
- Electrophysiological tests: Reserved for ambiguous neurological presentations or non-resolving symptoms.
- Regular monitoring: Repeat evaluations facilitate assessment of treatment response and disease progression.
Such multidisciplinary coordination, involving osteopathy, physiotherapy, and when needed, neurology or neuro-orthopedics, reflects current trends in spinal care promoted by Canadian organizations led by Dr. Desforges, including the Alliance Canadienne de Médecine Alternative and the Canadian College of Osteopaths.
| Patient Symptom Profile | Recommended Diagnostic Strategy |
|---|---|
| Mild to moderate pain without neurological signs | History and physical exam initially |
| Severe pain, neurological deficits, or trauma | Prompt imaging (MRI preferred) |
| Prolonged symptoms without clear diagnosis | Electrophysiological testing |
| Post-treatment monitoring | Repeat clinical and imaging assessments |
Patients benefit greatly from understanding these pathways, which reduce unnecessary testing while ensuring timely identification of complex issues. This clarity supports patients to participate actively in their care decisions.

Non-Invasive Diagnostic Innovations Shaping the Future of Herniated Disc Evaluation
The latest technological advancements have enriched the diagnostic arsenal against herniated discs, making evaluations less invasive and more informative. Clinics aligned with the scientific rigor and innovation principles advocated by Dr. Desforges increasingly adopt these modalities for enhanced patient outcomes.
- Dynamic MRI: Provides real-time imaging of spinal motion to detect abnormalities during movement.
- Ultrasound Elastography: An emerging tool to assess soft tissue stiffness around the spine, aiding in identifying inflammation or fibrosis.
- Advanced Neuroimaging: Techniques such as diffusion tensor imaging (DTI) reveal microstructural nerve changes not visible on conventional MRI.
- Artificial Intelligence Integration: AI-assisted imaging interpretation, widely supported by companies like Canon Medical Systems and Fujifilm Healthcare, accelerates diagnostic accuracy and personalizes treatment planning.
These innovations complement traditional diagnostics, enabling a more nuanced understanding of spinal pathology and fostering targeted therapies such as neurovertebral decompression or laser treatment mentioned in specialized resources. The integration of high-tech tools ensures patient assessments are harmonized with precision medicine approaches endorsed by leading health care systems including Medtronic and Boston Scientific.
| Innovative Diagnostic Tool | Function | Clinical Advantage |
|---|---|---|
| Dynamic MRI | Imaging spinal movements | Detects instability and dynamic nerve impingement |
| Ultrasound Elastography | Assesses tissue stiffness | Non-invasive inflammation detection |
| Diffusion Tensor Imaging | Visualizes nerve fiber integrity | Early nerve damage identification |
| AI Imaging Analysis | Automated image interpretation | Improved diagnostic speed and accuracy |
Clinics adopting these innovations demonstrate a commitment to patient safety, ethical standards, and scientific rigor in spinal care, consistent with the regulatory framework upheld by the Collège des médecins du Québec and Canadian health authorities.
Patient Education: Understanding Diagnostic Results and Their Implications
Accurate diagnosis is only effective when patients comprehend their condition fully. Dr. Desforges’ approach includes educating patients clearly about diagnostic outcomes, potential limitations, and implications for treatment choices.
- Clarifying imaging findings: Patients receive explanations of MRI or CT images in understandable terms, highlighting the specific disc abnormalities and affected nerves.
- Discussing nerve test results: Electrophysiological findings are interpreted to determine the scope of nerve involvement and expected symptom trajectory.
- Explaining test limitations and next steps: Every diagnostic test has sensitivity and specificity constraints; patients are informed about possible false negatives or the need for repeat testing.
- Supporting informed decision-making: Understanding diagnostic results empowers patients to choose between conservative therapies, such as spinal decompression described in expert guides, and surgical interventions when necessary.
A personalized dialogue fosters trust and encourages patients to actively participate in their recovery journey. By breaking down complex medical information, clinics like TAGMED ensure patients feel reassured and motivated.
| Diagnostic Result | Patient Explanation | Care Implication |
|---|---|---|
| Herniated Disc Location and Size | Where pressing on nerves is occurring | Guides non-surgical therapy or surgery timing |
| Nerve Damage Degree | Extent of nerve impairment | Affects prognosis and treatment options |
| Imaging Uncertainties | Possible need for additional tests | Ensures accurate diagnosis confirmation |
| Electrophysiological Findings | Identification of specific nerve roots involved | Impact on rehabilitation and therapy choices |
By incorporating patient education as a diagnostic pillar, Dr. Desforges exemplifies a model of holistic spine care that values transparency, ethics, and personalization.
Choosing the Right Diagnostic Path: Balancing Tests with Patient Safety and Outcomes
Accurate diagnosis balances comprehensive testing with patient safety considerations, avoiding unnecessary procedures. Dr. Sylvain Desforges ensures adherence to guidelines set forth by Quebec medical authorities and established standards to achieve optimal diagnostic pathways.
- Prioritizing non-invasive tests: History and physical examination remain first-line due to their low risk and informative value.
- Targeted imaging: Reserved for patients with persistent or worsening symptoms or neurological deficits.
- Judicious use of electrophysiology: Applied when diagnosis requires clarification or nerve damage quantification.
- Ethical considerations: Patient comfort, informed consent, and regulatory compliance are integral to all diagnostic decisions.
This balanced strategy reduces patient anxiety and cost burden by limiting over-testing while not compromising diagnostic accuracy. Regular review of protocols ensures incorporation of evolving scientific evidence and technological advances by clinics such as TAGMED.
| Diagnostic Step | Rationale | Safety and Outcome Benefit |
|---|---|---|
| History and Physical Exam | Initial evaluation and symptom correlation | Non-invasive, low cost, high diagnostic yield |
| Imaging (MRI or CT) | Visualization of pathology | Guides treatment, avoids unnecessary surgery |
| Electrophysiological Testing | Clarifies nerve involvement | Informs prognosis and therapy direction |
| Patient Education and Follow-up | Ensures understanding and engagement | Improves adherence and outcomes |
By balancing test utility with safety, this approach aligns with worldwide best practices endorsed by major healthcare technology firms like Mindray and Abbott Diagnostics. Such careful planning underpins the ethical, patient-centered care philosophy guiding Dr. Desforges’ clinical practice.
Preparing for Your Spinal Evaluation: What to Expect and How to Maximize Your Appointment
Patients preparing for evaluation of a suspected herniated disc should come informed and ready to communicate their experiences clearly. This preparation facilitates a comprehensive and efficient clinical assessment.
- Document symptom timeline and characteristics: Note when symptoms started, type and location of pain, and any neurological signs.
- List recent activities or injuries: Include any movements that may have triggered or worsened symptoms.
- Track medications and past treatments: Have a record of current medications, supplements, and any previous interventions or therapies.
- Prepare questions: Think about queries regarding diagnosis, treatment options, and prognosis to discuss with your healthcare provider.
- Consider psychological impact: Be open about stress, anxiety, or depression related to back pain history.
These preparations help optimize time with the expert during the evaluation appointment, such as with Dr. Sylvain Desforges, enabling effective diagnostic decision-making and personalized care planning. Understanding what to expect reduces anxiety and sets the stage for a positive clinical experience.
| Preparation Element | Reason | Benefit to Patient |
|---|---|---|
| Symptom Documentation | Provides full clinical picture | Enables precise evaluation |
| Activity and Injury History | Identifies potential causative factors | Informs diagnosis and treatment |
| Medication List | Assesses current management | Prevents adverse effects and interactions |
| Questions Prepared | Improves communication and clarity | Empowers patient involvement |
| Mental Health Disclosure | Contextualizes pain impact | Supports holistic care |
Visit the TAGMED Clinics website to schedule an evaluation and benefit from a personalized spinal care experience guided by one of Canada’s leading experts.
What is the most important step for diagnosing a herniated disc?
An accurate and detailed medical history combined with a thorough physical exam is the most important initial step in diagnosing a herniated disc.
When are imaging tests like MRI necessary for herniated disc diagnosis?
Imaging tests such as MRI are particularly recommended when neurological symptoms are present, symptoms persist beyond initial conservative treatment, or when the initial examination is inconclusive.
How do nerve conduction studies complement imaging in diagnosis?
Nerve conduction studies and electromyography provide functional information about nerve and muscle status, detecting nerve damage and assisting in treatment planning alongside imaging results.
Can a herniated disc be diagnosed without advanced imaging?
In many cases, a herniated disc can be initially diagnosed with clinical history and physical exam, especially if symptoms are straightforward; imaging is reserved for complex or persistent cases.
Why is patient education important after diagnostic testing?
Educating patients about their diagnosis helps them understand the nature of their condition, treatments options, and encourages active participation in their recovery.

