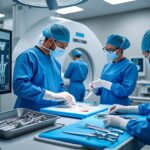
Essential Steps to Prepare for Simple, Fusion, or Motion Surgeries: What You Need to Know
November 5, 2025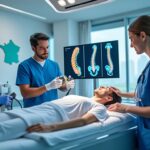
Spine Surgery in Trois-Rivières: Reduce Risk of Complications
November 5, 2025The value of patient testimonials in healthcare cannot be overstated, especially when it comes to sharing stories about recovery. These narratives provide hope, build trust, and create a human connection between prospective patients and healthcare providers. However, the process of sharing recovering patient testimonials is fraught with challenges. Missteps such as breaches in patient confidentiality or misrepresentation can not only undermine trust but also have legal and ethical consequences. In 2025, with evolving regulations and increasing patient awareness, healthcare providers must navigate these pitfalls carefully to maintain authenticity and compliance.
Sharing patient testimonials post-recovery involves several delicate factors including ensuring HIPAA compliance, securing informed consent, and preserving anonymity. Emotional triggers within these stories must be handled sensitively, avoiding language that could retraumatize or mislead. Moreover, testimonials should reflect genuine experiences without any overpromising results, maintaining a balance between optimism and realistic expectations. Third-party verification has also emerged as a valuable measure to enhance credibility and transparency in patient storytelling.
Notably, testimonials are powerful tools when used responsibly. They not only convey the success of treatments but also serve as educative material that encourages patients in their own recovery journeys. This article unpacks common pitfalls to avoid when sharing recovering patient testimonials, exploring aspects of authenticity, patient confidentiality, ethical communication, and effective storytelling. Drawing on current best practices and examples from established healthcare organizations, it offers guidance for healthcare marketers, clinicians, and administrators seeking to optimize the impact of patient stories in a compliant and respectful way.
Ensuring HIPAA Compliance While Sharing Patient Testimonials
One of the foremost challenges in sharing patient testimonials is adhering to HIPAA Compliance regulations. HIPAA (Health Insurance Portability and Accountability Act) mandates strict standards to safeguard patient health information, and testimonials often involve personally identifiable health data.
Healthcare providers must obtain explicit informed consent from patients before using their testimonials. This consent should outline how the patient’s information will be shared, where it will appear, and the scope of the testimonial’s use. Without documented informed consent, sharing any patient information— even anecdotal material—risks violating privacy protections.
Additionally, Anonymity Protection is critical. Redacting identifiable details such as names, locations, or specific treatment dates can help protect patients’ identities while still allowing their stories to inspire others. Sometimes, using pseudonyms or anonymized case studies may be necessary. It’s equally important to avoid sharing sensitive language that could inadvertently reveal patient identity.
Ignoring these safeguards can lead to legal repercussions and damage to patient-provider trust. For example, a healthcare facility posting an unsanctioned testimonial on social media might face complaints or fines. Furthermore, patients may feel exploited if their stories are used without appropriate permissions, undermining the therapeutic alliance.
- Obtain clear, written informed consent before sharing any testimonial.
- Ensure testimonial content complies with HIPAA standards for patient confidentiality.
- Use anonymization techniques when necessary to protect patient identity.
- Train staff on the legal ramifications and correct procedures for collecting testimonials.
- Regularly audit testimonial content for compliance and appropriateness.
| Potential Pitfall | Consequence | Preventive Measure |
|---|---|---|
| Sharing without informed consent | Legal penalties, lost trust | Obtain documented consent detailing usage |
| Including identifiable patient data | Privacy breach, HIPAA violation | Implement strict anonymity protocols |
| Inadvertent disclosure through sensitive language | Patient discomfort, reputational harm | Review testimonials for disclosure risks |
Healthcare organizations looking for detailed legal guidance on this topic will find useful resources, such as your guide to HIPAA-compliant patient reviews. This kind of comprehensive information ensures testimonials are shared responsibly.


Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…
Maintaining Authenticity While Avoiding Overediting Testimonials
Authenticity is a cornerstone of impactful patient testimonials. Patients and prospective clients can easily detect when stories feel scripted or manipulated, which undermines trust in the healthcare provider. Achieving genuine storytelling involves presenting patient voices in their own words without excessive Selective Editing that alters or removes meaningful experiences.
Overpromising results is a common pitfall that can lead to skepticism or disappointment. Testimonials that suggest guaranteed outcomes or overly positive experiences may set unrealistic expectations. Instead, sharing balanced testimonies that acknowledge challenges alongside successes demonstrates integrity and builds lasting credibility in patient communications.
One effective strategy for safeguarding authenticity is allowing patients to tell their story with minimal interference while ensuring Sensitive Language that is respectful and mindful of emotional triggers. This fosters connection without risking retraumatization or misleading messages that exploit patient vulnerabilities.
- Encourage patients to share their own narrative without scripting or heavy editing.
- Avoid exaggerated claims or language implying guaranteed outcomes.
- Be transparent about the variability of recovery experiences.
- Train interviewers to listen actively and probe empathetically.
- Use third-party verification to bolster credibility where feasible.
| Common Authenticity Issue | Impact on Audience Trust | Recommended Practice |
|---|---|---|
| Scripted or overly polished testimonials | Audience doubts sincerity, reduced impact | Use raw patient language and honest emotions |
| Overpromising recovery results | Creates unrealistic expectations, potential backlash | Discuss realistic outcomes and individual variations |
| Selective editing removes critical context | Loss of nuanced perspective, audience mistrust | Preserve key parts that reflect challenges and progress |
Additional insights on authentic healthcare storytelling are explored in resources like Healthcare Storytelling: Building Patient Trust and practical tips in 5 Common Mistakes in Patient Loyalty Testimonials.

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Respecting Patient Confidentiality While Sharing Recovery Experiences
Patient Confidentiality remains paramount when sharing any recovery testimonial. Beyond HIPAA, respecting confidentiality nurtures trust and ensures that patient dignity is preserved. Even well-intentioned sharing can inadvertently reveal sensitive information if controls are not in place.
It is recommended healthcare providers implement strict protocols to vet testimonial content for Confidentiality breaches. This includes reviewing any media, quotes, or images to confirm no personal data or indirect identifiers are disclosed. For instance, combining location details with personal health narratives can make patient identification possible.
Professionals should be alert to pitfalls like Posting Patient Information on public forums without adequate safeguards or responding to reviews with private health details. Adopting a “less is more” approach regarding personal data inclusion can mitigate these risks effectively.
- Conduct compliance checks on all testimonial materials before publication.
- Remove or obscure any information that can lead to patient identification.
- Avoid discussing private patient information in public responses.
- Educate teams on the ethical handling of sensitive patient data.
- Use secure platforms for collecting and managing testimonials.
| Breach Risk | Consequences | Preventive Actions |
|---|---|---|
| Disclosing location and treatment specifics | Patient identification and privacy violation | Omit or generalize geographic and temporal data |
| Improper response referencing private health info | Public privacy breaches, legal actions | Use neutral, non-specific communication |
| Sharing unvetted pictures or videos | Unauthorized exposure of patient identity | Obtain consent and conduct thorough media reviews |
For guidance on responding to patient reviews while preserving confidentiality, exploring the do’s and don’ts of responding to patient reviews may be beneficial.


Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…
Handling Emotional Triggers and Sensitive Language in Patient Testimonials
Sharing recovering patient testimonials must be done with empathy and caution regarding emotional triggers. Testimonies often recount painful or traumatic experiences that can evoke distress if improperly framed. Sensitive Language usage is crucial to avoid exacerbating patients’ psychological distress or alienating prospective patients.
Healthcare professionals must be skilled in identifying potential triggers in narratives and choose phrasing that balances truthful storytelling with compassionate communication. For example, overly graphic descriptions or dramatic language might retraumatize patients or generate anxiety among readers.
This sensitivity extends to the editing and presentation of testimonials, ensuring that stories uplift and encourage without sensationalizing pain or hardship. Training healthcare marketers and interviewers on trauma-informed communication helps prevent common pitfalls in sharing patient voices responsibly.
- Review testimonial drafts for language that may trigger emotional distress.
- Use neutral, supportive wording that shows respect for patient experiences.
- Provide patients with options to review and approve their narratives.
- Offer supportive resources alongside testimonials to aid emotional processing.
- Encourage storytelling that highlights resilience and hope without minimizing challenges.
| Trigger Type | Risk | Mitigation Strategy |
|---|---|---|
| Graphic descriptions of medical procedures | Patient and audience distress | Use clinical but gentle language, limit graphic content |
| Dramatic or sensational wording | Overstimulation, loss of credibility | Focus on balanced, honest storytelling without exaggeration |
| Recounting traumatic events without framing | Re-traumatization, negative emotional impact | Include supportive context and follow-up resources |
For actionable advice on mindful storytelling in healthcare marketing, the do’s and don’ts of patient storytelling provides valuable perspectives.

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
The Importance of Informed Consent Beyond Legal Requirements
Informed Consent is not merely a checkbox or legal formality but a foundational ethical practice that empowers patients when sharing their testimonials. Full disclosure about how their story will be used, potential audiences, and any digital permanence associated with online publication equips patients to make truly informed decisions.
Obtaining informed consent fosters a transparent relationship that respects patient autonomy and mitigates the risk of complaints or withdrawal of permission later. Consent forms should be written in clear, accessible language and offer patients an opportunity to ask questions.
Providers should also clarify whether testimonials will undergo editing and how confidentiality will be maintained. Importantly, patients must be informed about their right to revoke consent at any time, although practical challenges related to removing content from the web after posting should also be explained with transparency.
- Use detailed consent processes that communicate testimonial usage clearly.
- Ensure patients understand the scope and reach of their testimonial’s publication.
- Offer options about anonymity, pseudonyms, or partial disclosure.
- Allow patients to review and approve the final testimonial copy.
- Inform patients about their right to withdraw consent and implications thereof.
| Consent Aspect | Best Practice |
|---|---|
| Scope of use | Clearly define where and how testimonials will be shared |
| Editing disclosure | Inform patients about potential editing and seek approval |
| Right to revoke | Explain withdrawal process and digital permanence limits |
Healthcare organizations can enhance consent protocols by consulting guidelines such as those from experts in patient testimonial compliance and trust building.
Étapes pour obtenir le consentement éclairé des témoignages patients
Interact with each step to get details and avoid common pitfalls!

International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…
Strategies to Avoid Overpromising Results in Recovery Testimonials
Healthcare providers often face the temptation to share exclusively positive recovery testimonials that suggest dramatic or guaranteed healing. This Overpromising Results approach can erode trust when real patient outcomes vary widely due to individual health factors.
To maintain realistic messaging, testimonials must reflect the spectrum of recovery experiences, including setbacks, prolonged healing times, and the need for ongoing care. Such balanced representation avoids misleading potential patients while enabling hope.
Providers should also clearly communicate any innovations or therapies used but with caveats regarding their typical effectiveness range. This transparency helps manage expectations and promotes shared decision-making.
- Include diverse patient experiences reflecting successes and challenges.
- Avoid language implying guaranteed or immediate cures.
- Use testimonials to educate about typical recovery pathways.
- Integrate disclaimers or clarifications alongside success stories.
- Train marketing teams and clinicians on ethical communication principles.
| Risk of Overpromising | Negative Outcome | Mitigation Approach |
|---|---|---|
| Portraying miracles or cures | Patient disappointment and distrust | Present average outcomes and cautionary notes |
| Ignoring possible complications | Unrealistic expectations for care | Discuss risks openly within testimonials |
| Using promotional language | Legal and ethical challenges | Adopt factual, patient-centered storytelling |
Further insights on cautiously framing recovery stories can be found in resources such as How to Share Patient Testimonials on Recovery.

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
The Role of Third-Party Verification in Enhancing Testimonial Credibility
Third-Party Verification refers to the process of having independent bodies or processes validate the authenticity and accuracy of patient testimonials. In an era where digital misinformation proliferates, such verification greatly enhances credibility.
Verification can include confirming that testimonials are based on actual clinical encounters, ensuring the consistency of treatment descriptions, and validating consent processes. This external validation reassures prospective patients that testimonials are trustworthy and not fabricated or overly promotional.
Healthcare providers may partner with unbiased patient advocacy groups or utilize software that manages testimonial authenticity and compliance. While this adds operational layers, the return on trust gained is substantial.
- Engage third parties to audit testimonial collection and approval.
- Include badges or certifications on testimonial pages indicating verification.
- Use digital tools to authenticate patient identities confidentially.
- Maintain transparent records showing compliance and verification outcomes.
- Educate patients about the role and importance of third-party verification.
| Verification Process | Benefit | Implementation Tip |
|---|---|---|
| Independent audits | Improved patient and public trust | Schedule regular external reviews |
| Digital authentication | Reduced risk of fraudulent testimonials | Adopt secure, privacy-compliant software |
| Consent verification | Legal protection and transparency | Maintain comprehensive consent documentation |
Resources such as The power of patient testimonials: Building trust and credibility provide deeper insights into verification strategies.

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…
Ethical Storytelling: Balancing Optimism and Realism in Patient Testimonials
Ethical storytelling in healthcare demands a balance between inspiring optimism and delivering realism. Testimonials should empower patients without minimizing the complexity of recovery or glossing over potential difficulties.
Authentic stories that freely acknowledge both triumphs and hurdles better prepare prospective patients for their own healthcare journeys. This transparency fosters informed choices and builds sustainable trust between patients and providers.
Ethical storytellers focus on presenting testimonials as individual experiences, not universal guarantees, and carefully avoid language that could unwittingly pressure or manipulate vulnerable audiences. Incorporating feedback loops from patients ensures storytelling remains respectful and effective.
- Focus on individual patient journeys, not uniform outcomes.
- Disclose typical recovery challenges alongside successes.
- Avoid dramatic or manipulative narrative tones.
- Support patients in telling their stories with integrity.
- Implement regular reviews to detect potential ethical issues.
| Ethical Risk | Potential Harm | Recommended Safeguard |
|---|---|---|
| Minimizing patient difficulties | False hope and patient disillusionment | Include balanced testimonials with full context |
| Manipulative messaging | Loss of patient autonomy and trust | Use honest, patient-led storytelling |
| Ignoring patient consent nuances | Ethical breaches and legal action | Engage patients continuously throughout process |
For further reading on ethical patient communication, the article Common pitfalls to avoid in patient communication offers useful insights.
Sharing recovering patient testimonials demands vigilance across multiple dimensions: from HIPAA compliance and consent to authenticity and ethical storytelling. By consciously addressing these pitfalls, healthcare providers can harness the full potential of patient stories to foster hope, trust, and informed decision-making in a responsible and legally sound manner.
What constitutes proper HIPAA compliance when sharing patient testimonials?
Proper HIPAA compliance involves obtaining informed consent, ensuring patient confidentiality by removing identifying information, and adhering to legal requirements for the handling and sharing of health information.
How can healthcare providers maintain authenticity in patient testimonials?
By allowing patients to share their experiences in their own words, avoiding scripted or overly polished content, and steering clear of overpromising results that may not be typical.
Why is informed consent more than just a legal formality?
Informed consent respects patient autonomy by clearly communicating how their stories will be used and allows them to make voluntary, knowledgeable decisions, fostering trust and reducing complaints.
What role does third-party verification play in sharing patient testimonials?
It enhances credibility by independently confirming the authenticity and compliance of testimonials, reassuring audiences about their legitimacy.
How should emotional triggers be handled in patient storytelling?
Emotional triggers should be carefully identified and managed by using sensitive language, avoiding graphic or sensational content, and providing supportive context to minimize distress.

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…




