Mastering Medical Logistics and Accommodation: Essential Tips for Effective Preparation
November 4, 2025
Common Pitfalls to Avoid When Sharing Recovering Patient Testimonials
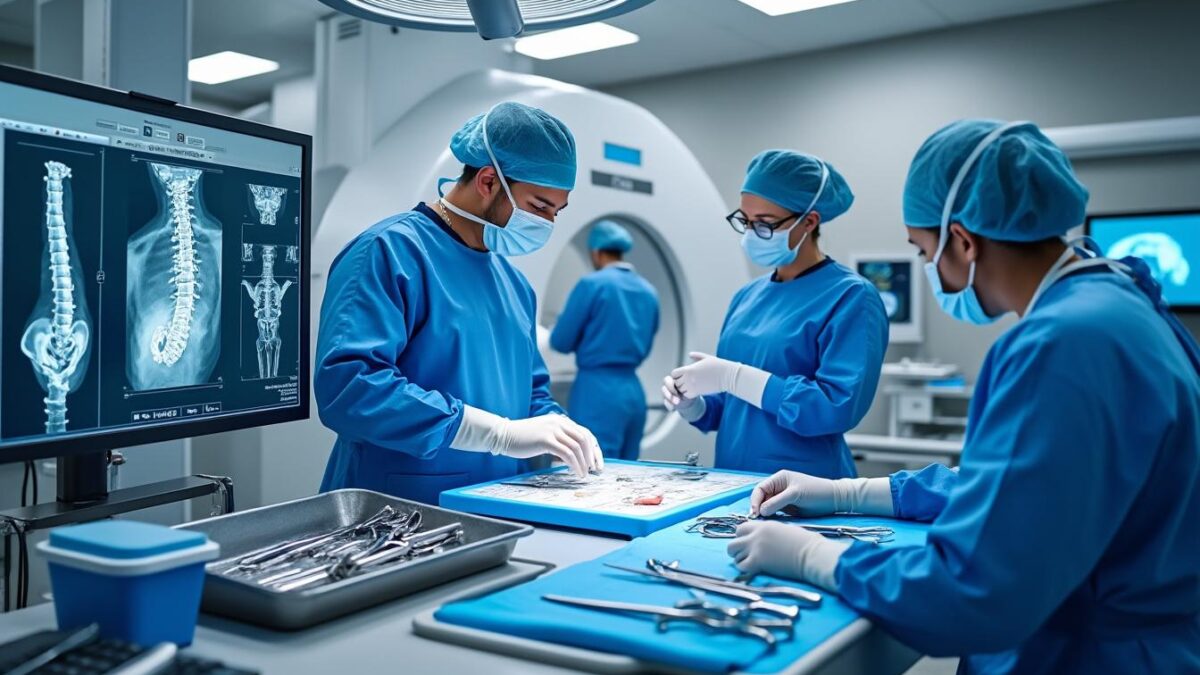
November 5, 2025Addressing spinal surgery—whether involves a simple decompression, vertebral fusion, or motion-preserving operation—often raises numerous questions and concerns for patients and their families alike. The complexity of these procedures, combined with the evolving landscape of surgical technologies and multidisciplinary care pathways, demands rigorous preparation that balances physical conditioning, emotional readiness, and logistical organization. Importantly, the advancements in spinal implants and minimally invasive techniques, pioneered by leading medical technology firms such as Medtronic, Stryker, and DePuy Synthes, contribute to significantly improving outcomes. Yet, success depends not only on cutting-edge devices but on holistic patient preparation and well-coordinated care across the continuum — from initial evaluation through recovery.
In recent years, innovative transatlantic collaborations, such as those between Quebec and France, have enabled patients to access highly specialized spinal surgery services, blending scientific rigor with personalized support. This synergy is exemplified by expert-led programs partnering with entities like SOS Tourisme Médical and neurotherapy centers, providing seamless transitions from conservative treatments through advanced surgical options. Being well-informed on the types of surgical procedures and understanding the preparatory steps can empower patients to navigate their journey confidently and achieve optimal recovery, all while minimizing potential complications.
Comprehensive Overview of Spine Surgery Types: Simple, Fusion, and Motion Preservation Explained
Spinal pathologies vary widely in presentation, severity, and biomechanical impact, necessitating different surgical approaches tailored to individual patient needs. Three principal techniques dominate contemporary spinal surgery: simple procedures, fusion surgeries, and motion preservation interventions. Each technique has unique indications, benefits, and limitations that must be carefully weighed by a multidisciplinary team comprised of spinal surgeons, osteopaths, and rehabilitation specialists.
Simple Spine Surgeries: Targeted, Minimally Invasive Approaches for Focal Lesions
Simple spinal surgeries primarily address localized issues such as herniated discs or foraminal stenosis through decompression. Advances in surgical visualization and instrumentation, including high-definition endoscopes and ultrafine tools developed by Zimmer Biomet and NuVasive, have minimized tissue trauma. These procedures typically involve small incisions or endoscopic access routes that significantly shorten hospital stays and expedite functional recovery.
- Relief of nerve compression symptoms with minimal collateral damage
- Short operative time reduces anesthesia risks
- Lower infection rates and scar tissue formation compared to open surgery
- Often outpatient or brief inpatient stays
Despite these advantages, patient selection is crucial, as extensive or multi-level pathology may limit effectiveness. For detailed patient guidance and recovery tips, resources such as the Mayo Clinic’s surgery preparation guide offer comprehensive insights.
Vertebral Fusion Surgery: Stabilizing the Spine for Lasting Correction
Fusion surgery involves the permanent immobilization of one or more vertebral segments to address instability, deformities, or spondylolisthesis. This approach utilizes state-of-the-art implants such as pedicle screws, rods, and plates—many manufactured by giants like DePuy Synthes and Globus Medical—to achieve biomechanical stability. Coupled with bone grafts, fusion restores spinal alignment and reduces pain.
- Corrects abnormal spinal motion and alignment
- Reduces risk of progressive neurological damage
- Durable pain relief for complex degenerative disorders
- Improved with robotics and navigation systems providing precision implant placement
The trade-offs include loss of segmental mobility and a longer convalescence period. However, ongoing robotic assistance and surgical navigation technologies improve accuracy, safety, and outcomes, underscoring the importance of specialized centers such as those referenced on SPINE SURGERY IN FRANCE ESSENTIAL INSIGHTS.
Motion Preservation Surgery: Innovations to Maintain Spinal Mobility and Reduce Adjacent Segment Disease
Motion preservation techniques revolutionize spinal care by enabling natural movement post-intervention, curtailing degenerative changes seen near fusion levels. Devices like cervical and lumbar disc prostheses and dynamic stabilization implants—such as TOPS by Smith & Nephew and IntraSPINE from Baxter—offer targeted solutions to preserve segmental mobility.
- Prevents compensation stress on adjacent spinal segments
- Improves long-term functional quality of life
- Reduced incidence of secondary degeneration compared to fusion
- Strict patient selection maximizes device effectiveness
These advanced modalities require thorough evaluation of bone quality and lesion scope with multidisciplinary consultation, a process managed expertly by centers like Clinique TAGMED and supported by research highlighted in publications on innovation in motion surgery.
| Technique | Main Indications | Advantages | Limitations |
|---|---|---|---|
| Simple Surgery | Disc herniation, localized stenosis | Minimally invasive, rapid recovery, short hospitalization | Effectiveness varies with lesion severity |
| Fusion Surgery | Spinal instability, deformity, spondylolisthesis | Stable correction, long-term pain relief | Loss of motion, longer recovery, implant risks |
| Motion Preservation | Localized pathology without major instability | Preserved mobility, reduced adjacent segment stress | Strict indications, limited availability |
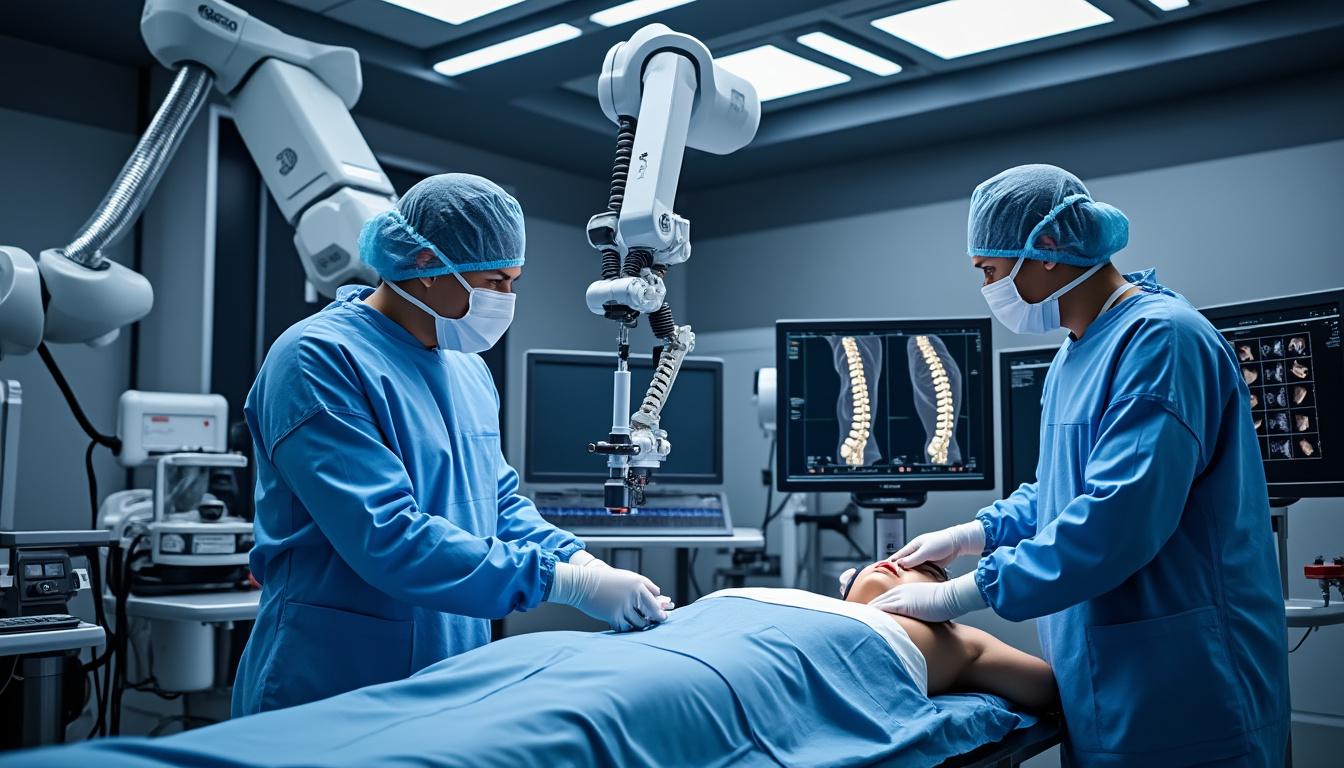

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Optimizing the Transatlantic Patient Journey for Spine Surgery Success
Accessing specialized spinal interventions across borders, particularly in partnerships between Quebec and France, illustrates a sophisticated healthcare navigation system tailored to optimize patient outcomes. Beyond the surgical act itself, success hinges on coordinated evaluation, preoperative care, travel logistics, and postoperative rehabilitation shared between expert teams.
Initial Assessment and Conservative Treatment: Laying the Foundation in Quebec
Before proceeding to surgery, patients typically undergo a comprehensive preoperative evaluation combined with an extended course of conservative therapies. Advanced modalities, including neurovertebral robotic decompression available at centers like Clinique TAGMED, offer non-invasive alleviation of symptoms and can forestall surgical necessity.
- Detailed biomechanical and imaging assessments
- Three to six months of conservative management emphasizing physical therapy and robotic decompression
- Periodic re-evaluations by spinal specialists to track progress
- Significant symptom relief often achieved, redefining surgical candidacy
This preparatory phase embodies principles emphasized by resources such as ReadySetRecover’s guide, advocating for patient empowerment and strategic prehabilitation.
Coordinated Surgical Arrangements and Travel to France
With surgery deemed necessary, logistical orchestration becomes paramount. Collaborations with organizations like Franchir streamline patient selection of expert surgeons and centers, management of appointments, accommodations, and tailored support during the stay in France.
- Precise matching based on pathology and surgeon specialization
- Complete travel and lodging management easing patient burden
- Dedicated patient liaisons facilitating medical communication
- Ensures smooth procedural and perioperative transitions
These arrangements guarantee access to cutting-edge surgical facilities equipped with leading brands such as NuVasive and Integra LifeSciences, ensuring the highest safety and technological standards, as outlined in literature like Willow’s healthcare surgery preparation blog.
Postoperative Monitoring and Local Rehabilitation Support in Quebec
Following surgery abroad, comprehensive postoperative care is crucial to consolidate surgical gains and enable maximal recovery. Centers such as Neurothérapie Montréal coordinate multidisciplinary follow-up encompassing physical therapy, clinical evaluation, and psychological support tailored to the specific surgical technique deployed.
- Individualized physical rehabilitation programs aligned with implants (e.g., Smith & Nephew’s dynamic stabilization)
- Continuous monitoring to detect and mitigate complications early
- Psychosocial support addressing anxiety and adherence challenges
- Regular communication with French surgical teams to harmonize care
| Phase | Key Activities | Responsible Organizations | Patient Benefits |
|---|---|---|---|
| Conservative Treatment | Biomechanical assessment, neurovertebral decompression | Dr. Desforges, Clinique TAGMED | Improved preparation, reduced pain, potential surgery avoidance |
| Surgical Preparation & Travel | Surgeon selection, travel and accommodation coordination | Franchir | Personalized, efficient surgical experience |
| Postoperative Care | Follow-up, rehabilitation, psychosocial support | Neurothérapie Montréal | Optimized recovery and long-term outcomes |

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
Holistic Body and Mind Preparation Techniques Prior to Spinal Surgery
Optimal surgical outcomes are tightly linked not only to procedural precision but equally to the patient’s preoperative physical and psychological condition. Experts stress comprehensive preparation weeks or months before intervention to enhance tissue healing, immune competence, and emotional resilience.
Nutrition Strategies for Structural Strength and Immunity Boost
Dietary optimization encourages tissue repair and counters inflammation through nutrient-dense food choices and avoidance of harmful substances. Bolstering protein intake with lean sources such as chicken, fish, and plant-based alternatives supports collagen synthesis vital for bone and soft tissue healing.
- Increased consumption of antioxidant-rich fruits and vegetables mitigates surgical stress
- Iron and zinc-rich foods foster oxygen transport and cellular repair
- Incorporating omega-3 fatty acids from sources like fatty fish and flaxseed counters inflammatory cascades
- Avoiding processed foods, excessive caffeine, and alcohol prevents immune suppression
Supplementary nutritional counseling as suggested in comprehensive plans like those from Narayana Health can tailor regimes to individual metabolic needs.
Stress Management and Psychological Readiness Approaches
Preoperative anxiety, if unmanaged, may elevate perioperative stress responses and affect pain perception. Adopting relaxation methodologies is thus pivotal, reinforced through mindfulness meditation, controlled breathing exercises, and emotional support.
- Mindfulness techniques facilitate attention regulation reducing intrusive negative thoughts
- Breathwork controls sympathetic nervous system activity, stabilizing heart rate and cortisol profiles
- Engagement with mental health professionals or trusted networks offers essential emotional outlets
Sleep Hygiene and Sensitive Physical Conditioning
Regular, restorative sleep enhances endocrine activity required for anabolic processes and immune function critical to surgical recovery. Recommendations include fixed sleep-wake schedules, reduction of screen exposure before bedtime, and creating a restful sleeping environment.
- Consistency in sleep timings improves circadian regulation
- Dark, cool bedrooms minimize disturbances
- Mild physical activities — such as slow-paced walking, yoga, and targeted stretches — preserve muscular function without exacerbating symptoms
- Supervised light exercises promote circulation and deter disuse atrophy
Such holistic preparedness is instrumental in boosting resilience as supported by organizations like Made for This Moment.


International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
The Indispensable Role of Rigorous Conservative Management Before Electing Surgery
International protocols emphasize that surgery is a last resort after exhaustive conservative efforts. Programs blending robotic decompression, manual therapies, and tailored physical rehabilitation have demonstrated significant symptom mitigation, delaying or entirely preventing the need for invasive interventions.
- Extended conservative therapy periods ensure natural healing mechanisms are maximized
- Procedures such as neurovertebral robotic decompression provide minimally invasive symptom relief
- Surgery is reserved for cases unresponsive to conservative approaches, thereby reducing overtreatment risks
- Preoperative conditioning enhances postoperative recovery trajectories
Patient candidacy and timing decisions rest upon detailed evaluation by experts such as Dr. Sylvain Desforges and collaborations with specialized surgical teams, aligning with evidence highlighted on platforms like essential insights before spinal fusion surgery.

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…
Integrating Cutting-Edge Technologies and Expert Care to Improve Surgical Outcomes
Recent years have witnessed an exponential expansion in the availability and refinement of surgical robotics, navigation, and biomaterials. Pioneering firms including Boston Scientific and Baxter have collaborated closely with renowned clinical centers to deliver interventions characterized by precision, safety, and enhanced recovery profiles.
- Three-dimensional imaging integrated with robotic guidance optimizes implant placement accuracy
- Minimally invasive techniques reduce wound size and postoperative pain intensity
- Dynamically stabilized implants maintain biomechanical function without rigid immobilization
- Standardization and certification of surgical teams assure quality and ethical compliance
Such innovations are extensively covered in medical curricula such as the Diplôme Inter-Universitaire de Chirurgie du Rachis, which updates practitioners on emerging standards. The interplay of technology and expert human-led care epitomizes the current paradigm for spine surgery excellence.
Logistical Recommendations: Practical Steps for a Smooth Surgical Experience
Successful spine surgery depends not only on medical preparedness but also on well-structured logistical arrangements that minimize stress and enable efficient clinical workflows. Key practical considerations for patients include:
- Ensuring clear communication and record sharing with the surgical team and coordinators
- Organizing a comfortable resting environment and securing post-discharge support from family or caregivers
- Adhering strictly to pre-surgical medication and fasting instructions to reduce perioperative risks
- Scheduling preoperative consultations to clarify doubts and set expectations
- Preparing necessary documentation such as health insurance and identification for transatlantic travel
Multiple medical travel facilitators assist patients in this domain to guarantee seamless coordination. Guidance similar to that found in orthopedic surgery preparation checklists ensures nothing crucial is overlooked.
Summary Table of Key Preparation Elements for Different Spine Surgery Types
| Preparation Element | Simple Surgery | Fusion Surgery | Motion Preservation Surgery |
|---|---|---|---|
| Physical Conditioning | Focus on flexibility and nerve decompression readiness | Emphasis on strength and spine stabilization exercises | Balanced mobility with core stabilization |
| Nutrition | Anti-inflammatory, protein-rich diet | High protein and micronutrient optimization | Caloric balance to support bone and tissue repair |
| Psychological Preparation | Stress reduction to ease pain perception | Acceptance of mobility limitations and recovery timelines | Understanding device function and adaptation strategies |
| Postoperative Planning | Short hospital stay and early mobilization | Extended rehabilitation and supervised activity gradually | Continuous motion assessment and implant monitoring |
In conclusion, meticulous preparation addressing both mind and body, alongside innovations in surgical techniques and international collaboration, defines the modern pathway ensuring patients reap the full benefits of spinal interventions while minimizing risks. Leveraging resources from leading healthcare platforms and jurisdictional expertise guarantees informed, safe, and personalized spine care.
Testez vos connaissances : Préparation et savoirs sur les chirurgies du rachis
Répondez aux questions sur la préparation, les types de chirurgies (simple, fusion, préservation du mouvement) et les soins post-opératoires.
What are the fundamental differences between simple, fusion, and motion preservation spinal surgeries?
Simple surgeries usually involve minimally invasive decompression to relieve nerve pressure while preserving structures. Fusion surgeries provide permanent stabilization of spinal segments to correct deformities or instability but sacrifice movement at those levels. Motion preservation techniques aim to maintain segmental mobility, reducing stress on adjacent segments and preserving overall spine function.
Why is conservative treatment important before considering spinal surgery?
Conservative treatment including physical therapy, robotic neurovertebral decompression, and rehabilitation is critical to alleviate symptoms and often avoid or delay surgery. It prepares the patient’s body and mind, ensuring they are in optimal condition for surgery if eventually needed, and reduces surgical risks.
How can patients best prepare physically and psychologically for spinal surgery?
Preparation entails adopting a nutrient-rich anti-inflammatory diet, optimizing sleep hygiene, engaging in tailored physical activity to maintain strength and flexibility, and utilizing stress management techniques such as mindfulness and controlled breathing. Psychological readiness is key to coping with perioperative anxiety and adjusting to postoperative recovery.
What role does technology play in enhancing spinal surgery outcomes?
Technological advancements like robotic surgical assistance, 3D imaging, and dynamic implants from companies such as Medtronic, Smith & Nephew, and NuVasive enhance precision, safety, and functional results. These reduce operative trauma and improve implant positioning, critical factors for successful recovery.
What logistical measures can improve the patient experience during a transatlantic spine surgery journey?
Collaborating with dedicated surgical coordinators, planning travel and accommodation well in advance, maintaining thorough communication with healthcare providers, and ensuring postoperative local rehabilitation support are essential steps. These measures reduce patient stress, streamline clinical processes, and help secure optimal surgical outcomes.