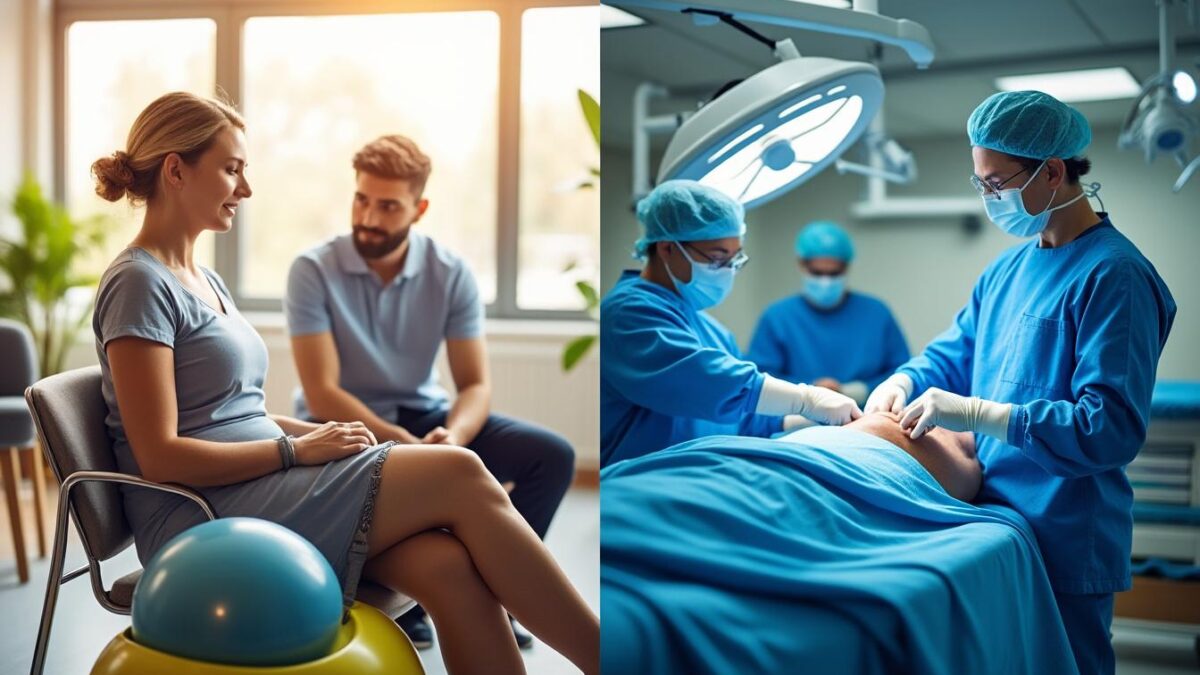
TOPS™ in Gatineau: Ensuring Stability and Enhancing Functionality
November 22, 2025
Comprehensive Guide to Stepwise Functional Recovery: Everything You Need to Know
November 22, 2025Across the globe, patients grappling with musculoskeletal and spinal issues often find themselves at a crossroads—deciding between conservative treatments and surgical interventions. This decision evolution reflects the complex intersection of medical advancements, patient preferences, and healthcare accessibility. With ailments ranging from herniated discs to degenerative spinal conditions becoming increasingly prevalent, the scrutiny on which treatment pathway offers the most optimal patient care intensifies. The dilemma extends beyond pure medical judgment, encompassing factors such as recovery time, risks and benefits, and nuanced treatment options informed by state-of-the-art technologies. Notably, growing interest in transatlantic medical collaborations has introduced innovative pathways where patients can access cutting-edge surgical procedures abroad or leverage advanced conservative therapies locally, embodying a multifaceted approach tailored to individual needs.
In regions like Quebec, challenges such as long surgical waitlists and elevated costs in the private sector amplify the necessity for a thorough understanding of all available modalities. As robotic-assisted neurovertebral decompression and dynamic implant technologies advance, the scope of non-invasive therapy broadens, offering promising alternatives to traditional surgery. Conversely, surgical procedures have evolved with minimally invasive techniques and motion-preservation implants that significantly improve outcomes and shorten recovery times. For patients and healthcare providers alike, nuanced health insights into these evolving modalities are vital for informed medical decisions. This comprehensive exploration unpacks the critical considerations distinguishing conservative treatments from surgical options, shedding light on what every patient should know before embarking on their therapeutic journey.
Fundamentals of Conservative Treatments in Spinal Disorders: Principles and Practices for Patient-Centered Care
Conservative treatments form the cornerstone of initial intervention strategies for spinal pathologies, emphasizing symptom alleviation, functional improvement, and natural healing processes without incurring surgical risks. This approach is rooted in patient-centered care, prioritizing less invasive techniques that encourage the body’s repair mechanisms, aiming to optimize treatment outcomes with minimal disruption.
Key modalities within conservative treatment frameworks include:
- Functional rehabilitation: Engaging in tailored exercises aimed at strengthening paravertebral muscles, improving posture, and restoring joint mobility.
- Physical therapies: Incorporating physiotherapy, kinesitherapy, and therapeutic massages to mitigate pain and enhance functional capacity without exacerbating the condition.
- Pain management strategies: Utilizing judicious medication regimens, target-specific infiltrations, and advanced nerve modulation techniques to control discomfort effectively.
- Neurovertebral decompression, especially robot-assisted: This innovative non-invasive method precisely applies controlled traction to reduce nerve and disc pressure, promoting symptom relief and functional recovery.
- Patient education and prevention: Essential guidance regarding posture, ergonomics, daily activity modifications, and strategies to prevent recurrence is integral to a sustainable care plan.
Consider the example of a patient with a lumbar herniated disc who participates in a structured program combining robotic neurovertebral decompression with supervised rehabilitation. This regimen aims to decompress affected spinal nerves gradually while fortifying the spinal musculature to support long-term benefits.
| Treatment Type | Main Advantages | Limitations |
|---|---|---|
| Robot-assisted Neurovertebral Decompression | Non-invasive, personalized traction; minimal side effects | Varied outcomes depending on condition severity; requires patient commitment over weeks/months |
| Functional Rehabilitation | Enhances muscular strength and mobility | Dependent upon skilled supervision; compliance essential for efficacy |
| Pain Control Medications | Rapid alleviation of discomfort | Potential side effects and addiction risks with prolonged use |
| Patient Education | Empowers patient with preventive knowledge | Requires long-term adherence and lifestyle adjustments |
Recent clinical evidence highlights the critical role of these conservative methods as prerequisites or complements to surgical options. For instance, the analysis on neurovertebral decompression for herniated discs provides compelling support for such carefully tailored non-surgical approaches before considering more invasive interventions. Consequently, many patients can realize significant improvements within a structured 3 to 6-month conservative treatment window, potentially circumventing the need for surgery altogether.
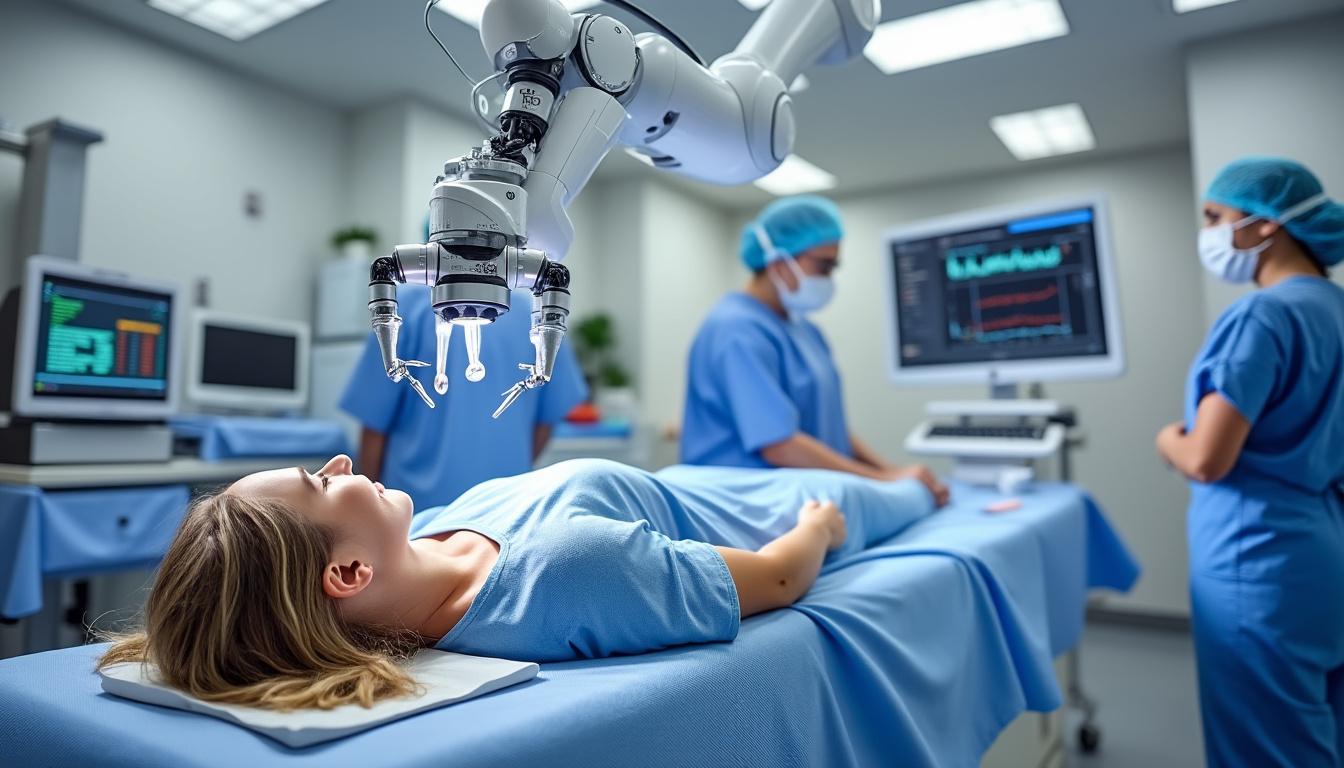

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Extended Conservative Treatment: Why Patience and Rigorous Supervision Are Paramount Before Surgery
A sustained conservative treatment timeline is often indispensable, particularly in degenerative or inflammatory spinal conditions where surgical urgency is low. A 3 to 6-month period of focused non-invasive therapy enables the natural reparative potential of the spine to manifest, while permitting precise evaluation of symptom trajectories.
Significant benefits of this extended approach include:
- Spontaneous improvements: Cases frequently demonstrate symptom attenuation and functional gain, primarily through gradual neural decompression and muscle strengthening.
- Risk mitigation: Deferring surgery lowers the probability of complications such as infections, hemorrhages, or post-anesthetic sequelae.
- Refined patient selection: Allows healthcare providers to discern which patients truly require surgical corrections versus those responding to conservative modalities.
- Pre-surgical optimization: Prepares patients physiologically and psychologically, improving surgical outcomes when operation is necessary.
- Active patient involvement: Promotes informed consent and empowers patients, enhancing satisfaction and adherence.
The treatment pathway unfolds in distinct phases:
| Phase | Objective | Duration | Expected Outcome |
|---|---|---|---|
| Initial Assessment | Comprehensive symptom analysis and personalized care planning | 1 session | Custom treatment protocol formulated |
| Specialized Conservative Therapy | Symptom mitigation and function restoration | 3 to 6 months | Favorable clinical response indicating effectiveness |
| Reassessment | Evaluate need to persist with conservative therapy or consider surgical referral | 1 session | Evidence-based decision-making for next steps |
Success during this interval is frequently correlated with the incorporation of advanced techniques such as the robot-assisted decompression available at centers like TAGMED in Quebec, which uniquely individualizes therapy to patient-specific disc and nerve pathology. The patient-centered coordination led by experts in non-operative care ensures ethics and rigorous standards govern this rehabilitative process.
Discover detailed symptom identification and decompression treatment options that illustrate the critical role of conservative management in preventing unnecessary surgery.

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
Innovative Surgical Techniques in Modern Spine Care: Enhancing Efficacy and Preserving Function
When conservative measures reach their limit, surgery offers definitive solutions with advanced techniques developed primarily within renowned European centers. France, for example, stands at the forefront with a broad spectrum of modern spine surgeries that range from decompression to motion-preserving implantations.
Key surgical options include:
- Simple decompression surgeries: Laminectomy or discectomy to relieve nerve compression without fusion.
- Spinal fusion (arthrodesis): Stabilizes a spinal segment to mitigate severe instability but sacrifices some segmental mobility.
- Dynamic implants such as TOPS or Intraspine: These devices maintain spinal mobility while providing segmental stability and reducing adjacent segment stress.
- Disc prostheses: Artificial disc replacements restore natural disc function and mitigate neurological symptoms.
- Minimal invasive and endoscopic approaches: Employ tiny incisions and endoscopic cameras, reducing post-operative pain and accelerating recovery.
| Procedure | Biomechanical Advantages | Potential Limitations |
|---|---|---|
| Decompression Alone | Less invasive with quicker recovery | Possibility of recurrence or segmental instability over time |
| Spinal Fusion | Provides lasting spinal stabilization | Loss of segmental motion; risk of adjacent segment disease |
| Dynamic Implants (TOPS, Intraspine) | Preservation of range of motion; reduced mechanical stress on adjacent levels | Limited availability and higher cost implications |
| Disc Prostheses | Restores physiological disc mechanics; relieves nerve compression | Specific patient criteria; implant-related complications possible |
| Endoscopic Surgery | Minimized tissue damage; less postoperative discomfort | Technically demanding with strict patient selection |
Access to such state-of-the-art procedures is facilitated by international partnerships, notably between Quebec and France, enabling patients to benefit from surgical expertise and technologies often not locally available. Organizations coordinating these transatlantic care pathways guarantee seamless logistics and continuous follow-up, underscoring patient safety and optimized recovery.
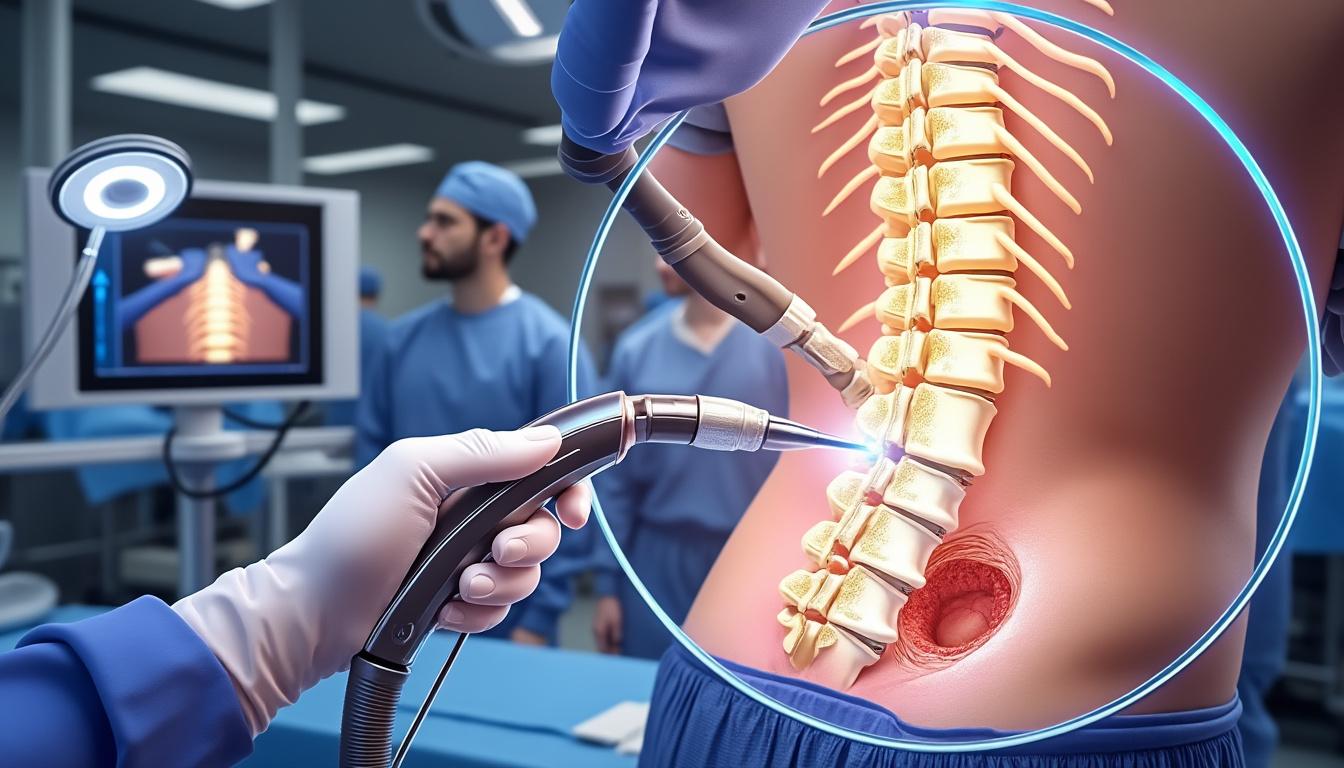

International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
Customized Transatlantic Patient Pathways: Accessing Advanced Spine Surgery Abroad
Innovative transatlantic collaboration exemplifies the integration of conservative and surgical spine treatments, optimizing recovery and care quality. The structured patient journey commonly begins with comprehensive evaluations in Quebec, led by specialists providing conservative care supervision. Based on response, referral and logistical arrangements direct candidates toward France’s exemplary surgical centers.
Phase-specific responsibilities include:
- Conservative management and evaluation by clinicians in Quebec ensures that surgery is reserved for appropriate cases.
- International surgical coordination by organizations specializing in medical travel logistics to select suitable centers and surgeons abroad.
- Postoperative rehabilitation and monitoring upon return, ensuring continuity of care and optimal function restoration.
- Administrative and informational support throughout the journey, smoothing procedural hurdles for patients.
| Stage | Lead Entity | Role |
|---|---|---|
| Initial assessment & conservative care | Specialized clinics and spine experts in Quebec | Tailored treatment planning and monitoring |
| International surgical referral & logistics | Medical travel facilitators organizing access to French centers | Coordination of travel, accommodation, and surgery dates |
| Post-surgical rehabilitation | Rehabilitation centers in Quebec | Reintegrative therapies and support |
| Patient guidance & administration | Patient support agencies | Navigating healthcare systems and insurance procedures |
This international care structure imposes rigorous quality and safety standards aligned with both Canadian and French medical regulations. It is tailored to individual patient profiles, assuring access to innovative treatment options while minimizing risks and recovery times. As such, the model represents a pioneering leap forward in global patient-centered spine care.

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…
Ethical Framework and Innovation in Spine Care: Insights from Leading Practitioners
The nexus between ethical medical practice and the incorporation of innovative therapies underpins the optimal treatment of spinal disorders today. Leaders in the field consistently emphasize evidence-based protocols, patient autonomy, and rigorous adherence to safety standards. By aligning technology adoption with sound ethics, practitioners effectively balance risks and benefits, ensuring patients receive care that is both cutting-edge and conscientious.
Essential principles embraced by ethical spine care include:
- Scientific rigor: Precision in applying validated conservative and surgical treatments.
- Patient safety: Minimizing risk by adhering to strict clinical guidelines.
- Responsible innovation: Gradual integration of robotic decompression, dynamic stabilization implants, and minimally invasive surgery.
- Clear communication and education: Ensuring patients understand treatment possibilities and limitations.
- Humanistic care: Offering empathetic support and fostering patient engagement in decisions.
This commitment to excellence is reflected in ongoing collaborations with international centers of excellence, facilitating access to advanced education such as the Intraspine dynamic stabilization system and endoscopic educational courses. These efforts guarantee up-to-date, ethically sound patient care strategies.
Non-invasive Therapy vs Surgical Procedures: Weighing Risks and Benefits for Optimal Patient Outcomes
The decision to pursue conservative treatments or opt for surgery involves meticulous analysis of risks, benefits, and expected recovery trajectories. Non-invasive therapies tend to offer safer profiles, minimal downtime, and sustainable symptom control, yet might not suffice for advanced disease stages where surgical intervention provides definitive relief.
A summarized comparison of essential factors is outlined below:
| Aspect | Conservative Treatments | Surgical Procedures |
|---|---|---|
| Invasiveness | Non-invasive; includes therapies like neurovertebral decompression and physiotherapy | Invasive, involving tissue dissection and instrumentation |
| Recovery Time | Typically weeks to months, depending on therapy adherence | Varies significantly; minimally invasive surgery reduces time but may still require months for full recovery |
| Risks | Low risk; includes possible minor side effects from medications or therapy discomfort | Higher risk including infections, neurological complications, and anesthesia-related issues |
| Long-term Outcomes | Effective in early to moderate conditions, may limit need for surgery | Potential for lasting resolution but carries risk of complications or reoperations |
Case studies from various orthopedic experiences underline that the choice of treatment should be individualized, balancing patient profiles with clinical indications. Resources such as detailed reviews on the decision-making process between conservative and surgical care for orthopedic injuries provide in-depth frameworks to aid clinicians and patients alike in navigating these complex options.
Role of Patient Education and Engagement in Navigating Treatment Options
Empowering patients through comprehensive education and transparent communication forms a pivotal axis in successful outcomes when choosing between conservative and surgical interventions. Understanding treatment mechanisms, expected benefits, potential risks, and recovery timelines enables patients to actively participate in their care trajectory.
Strategies to enhance patient engagement include:
- Detailed consultations: Explaining in accessible language the pros and cons of each treatment modality.
- Rehabilitation orientation: Teaching the importance of adherence to prescribed exercises and therapy schedules.
- Setting realistic expectations: Clarity on symptom resolution timelines and possible need for future interventions.
- Support networks: Facilitating access to peer groups, counseling, and ongoing medical guidance.
- Use of visual aids and digital platforms: Employing videos, charts, and online resources to reinforce understanding.
Such patient-centric approaches foster trust and encourage a healthier therapeutic alliance, which is instrumental in optimizing recovery and overall satisfaction.
Conservative Treatments vs Surgery: Essential Insights Every Patient Should Know
What are the primary benefits of conservative treatments in spinal care?
Conservative treatments minimize invasiveness, reduce surgical risk, and support natural healing through therapies like neurovertebral decompression and exercise-based rehabilitation.
When should surgery be considered over conservative management?
Surgery is typically recommended when conservative treatments fail over an adequate period, or in cases involving severe neurological impairment or spinal instability requiring structural correction.
How do dynamic implants improve surgical outcomes?
Dynamic implants preserve spinal mobility while stabilizing affected segments, reducing risks of adjacent segment degeneration and improving post-operative function.
Is patient education crucial in choosing between treatment options?
Yes, effective patient education promotes informed decision-making, enhances treatment adherence, and fosters patient engagement critical to successful outcomes.
What role does robotic neurovertebral decompression play in non-invasive therapies?
Robotic decompression provides precise, personalized traction to alleviate nerve and disc pressure, exemplifying an advanced non-invasive treatment modality with promising results.