
Enhancing Clinical Outcomes: A Comparative Study of Spinal Care between France and Quebec
October 27, 2025
Can Quality and Certification of Medical Devices Help Avoid Surgery?
October 27, 2025Chronic back pain affects millions worldwide, disrupting everyday activities and diminishing quality of life. As spinal conditions grow more prevalent, advances in non-invasive treatments such as spinal decompression therapy have gained significant traction among healthcare professionals and patients alike. This innovative therapy targets the root causes of spinal discomfort by gently relieving pressure on affected nerves and discs, offering renewed hope for lasting relief and improved mobility. With precision technology and established protocols, spinal decompression is reshaping the paradigm of spinal health management and becoming a cornerstone in comprehensive care plans endorsed by leading specialists.
Developed through extensive clinical expertise and refined technological advancements, spinal decompression therapy is no longer considered just an alternative but a primary option for various spinal pathologies. Its ability to restore disc hydration, reduce nerve impingement, and facilitate healing bridges the gap between conservative therapies and invasive surgery. As an organized, evidence-based approach, expert recommendations highlight the critical role spinal decompression plays in preventing progression of degenerative spinal conditions. Universities and specialized clinics around the globe underscore the therapy’s evolving methodologies, reflecting a growing consensus on its widespread applicability and clinical efficacy.
Exploring the Mechanisms Behind Spinal Decompression Therapy and Core Indications
Spinal decompression therapy functions by exerting a controlled mechanical force that gently stretches the spine, alleviating pressure exerted on compressed discs and nerve roots. Unlike traditional traction methods, modern devices such as the DRX9000 and SpineMED systems employ computer-controlled technology enabling precise adjustments tailored to individual patient needs. This targeted traction encourages the rehydration of degenerated discs, which restores their ability to act as cushions between vertebrae effectively.
Patients experiencing herniated discs, spinal stenosis, radiculopathy, or chronic neck and lower back pain often find spinal decompression especially beneficial. A consistent protocol involving 15 to 30 sessions is typically recommended, depending on severity and patient response. By expanding the intervertebral space, nerve irritation decreases, inflammation subsides, and mobility enhancements become evident within weeks of treatment. Other devices like the Axiom DRX and VAX-D also incorporate advanced feedback mechanisms ensuring patient comfort and the minimization of side effects.
The key indications for spinal decompression therapy include:
- Herniated or Bulging Discs: Reduces disc protrusion and nerve root compression, providing significant pain relief.
- Chronic Lumbar and Cervical Pain: Improves flexibility and diminishes inflammation over an extended treatment course.
- Spinal Stenosis Management: Increases foraminal space, alleviating nerve constriction symptoms.
- Radiculopathy: Mitigates radiating pain in the limbs caused by nerve root irritation.
Ensuring proper patient selection through comprehensive medical evaluations is paramount to maximize therapeutic outcomes. Clinics such as those utilizing Chirotouch or Decompression Pro technologies adhere strictly to safety guidelines while personalizing treatment plans.
| Condition | Expected Benefits | Typical Treatment Duration | Potential Side Effects |
|---|---|---|---|
| Herniated Disc | Reduction of nerve compression and pain relief | 15-25 sessions based on severity | Temporary stiffness or mild tenderness |
| Chronic Neck/Back Pain | Enhanced mobility and reduced inflammation | 20-30 sessions | Generally rare; well tolerated |
| Spinal Stenosis | Improved nerve circulation and pain reduction | 18-25 sessions | Possible slight initial discomfort |
| Disc Protrusions | Alleviation of radiating pain and functional improvement | 15-22 sessions | Minimal side effects |
Reliable results are achieved when spinal decompression therapy is integrated within comprehensive treatment frameworks overseen by experienced practitioners. The interplay between technology such as the HillDT system and clinical expertise ensures monitored progress and adjustments tailored for each patient’s evolving condition.
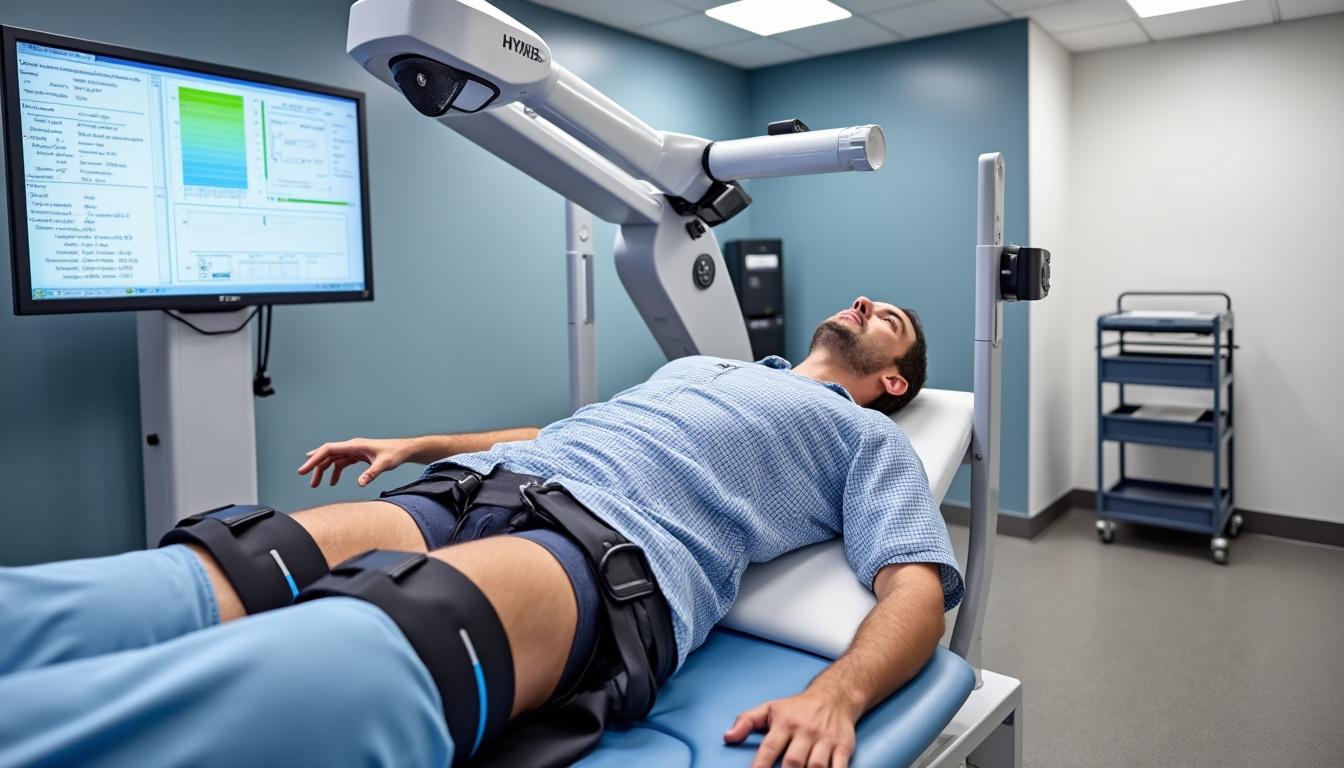

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…
Spinal Decompression As a Crucial Step Within the Multidisciplinary Care Pathway
Spinal decompression should always be incorporated within a larger, patient-centered care pathway that begins with conservative treatments. Leading spinal surgery consultants emphasize that a minimum period of 3-6 months of non-invasive care, including physical therapy, anti-inflammatory interventions, and decompression sessions, is essential before contemplating surgical options. This approach safeguards patient safety and optimizes recovery potential while possibly eliminating the need for invasive procedures.
The standard care sequence involves:
- Comprehensive Evaluation: In-depth review of imaging and clinical history to identify candidates suitable for decompression therapy.
- Customized Decompression and Conservative Management: This includes specialized protocols incorporating devices like Decompression Pro and Hill Laboratories innovations, along with physiotherapy.
- Ongoing Monitoring and Reassessment: Regular clinical assessments allow fine-tuning of therapeutic intensity and complementary treatment incorporation.
- Surgical Coordination (If Required): For cases requiring surgery, a coordinated transatlantic collaboration between Canadian and European centers optimizes treatment timing, technology access, and postoperative care.
- Rehabilitation and Long-Term Follow-Up: Includes both manual therapies and targeted exercises to sustain spinal health and function.
Institutions employing methods aligned with the Lordex Spine Institute emphasize multidisciplinary coordination crucial for outcome optimization. Patients in regions like Quebec benefit from smooth integration of emerging decompression technology with established rehabilitation clinics, facilitating a seamless continuum of care.
| Key Treatment Phase | Responsible Entity | Duration Estimate | Primary Objective |
|---|---|---|---|
| Initial Evaluation | Spinal Surgery Consultant/Clinic TAGMED | 1-2 weeks | Establish eligibility and personalized treatment plan |
| Conservative Treatment Phase | Clinic TAGMED & Associated Facilities | 3-6 months | Symptom relief and mobility restoration |
| Surgical Coordination | Franchir and European Partners | Variable by patient | Plan surgical intervention and logistics |
| Postoperative Care | Neurothérapie Montréal | 6-12 months | Enhance recovery and prevent complications |

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Biomechanical and Psychosocial Benefits of Spinal Decompression for Active Individuals
For patients leading physically active lifestyles, including athletes and manual laborers, spinal decompression therapy represents a scientifically validated option that significantly improves spinal integrity and reduces disability. By targeting the mechanical factors contributing to pain and dysfunction, decompression therapy restores natural spinal biomechanics and physical resilience.
This treatment facilitates:
- Pressure Alleviation: Careful computer-controlled traction reduces disk pressures and nerve impingements precisely.
- Enhanced Mobility: Patients show rapid improvement in flexibility, range of motion, and reduction of stiffness.
- Medication Reduction: The need for analgesic or anti-inflammatory drugs decreases, thereby lessening drug-related side effects.
- Prevention of Secondary Injury: Improved vascularization supports tissue regeneration mitigating progression of degenerative changes.
- Psychological Confidence: Non-surgical nature reduces treatment anxiety and facilitates patient participation in rehabilitation.
Clinical data from peer-reviewed sources affirm that approximately 70% of patients undergoing treatments with devices such as Axiom DRX and VAX-D experience marked symptom improvement. Additional adjunct techniques like Cox Technic improve neuromuscular coordination contributing to sustained functional gains.
| Biomechanical Advantage | Clinical Impact | Patient Outcome |
|---|---|---|
| Controlled Traction | Disc pressure decrease | Rapid pain relief |
| Improved Blood Flow | Enhanced tissue oxygenation | Accelerated healing |
| Neuromodulation (e.g., Pulse Align) | Activated muscle mechanoreceptors | Better muscle coordination and strength |
| Non-invasive Approach | Lower risk profile | Increased patient comfort and compliance |
| Reduced Medication Dependence | Fewer side effects | Improved overall well-being |
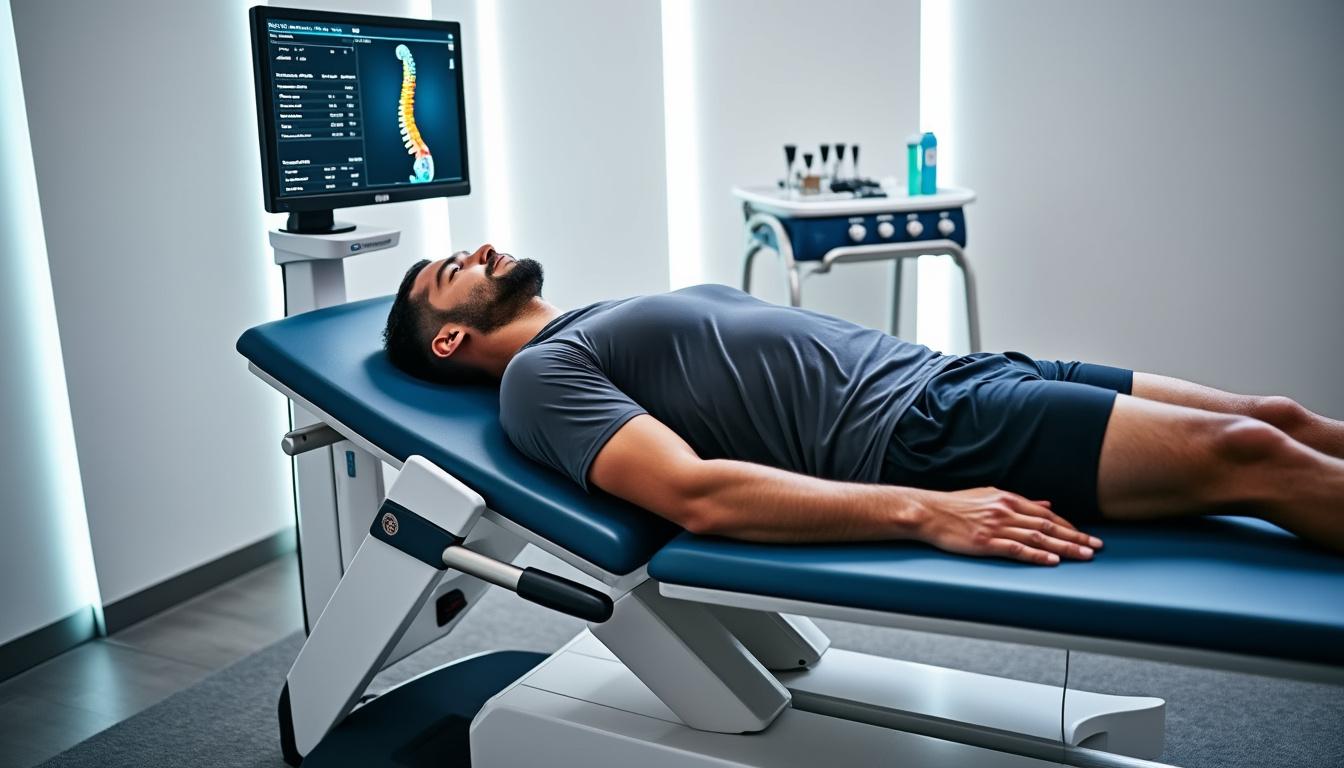

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…
Integrating Spinal Decompression in Postoperative Rehabilitation Regimens
Following spinal operations such as arthrodesis or minimally invasive decompressive surgeries, postoperative rehabilitation is pivotal for lasting success. Spinal decompression serves to complement other therapies by targeting persistent inflammation and enhancing tissue recovery. This phase requires careful timing to avoid compromising the surgical site.
Key benefits in postoperative care:
- Alleviation of Residual Nerve and Tissue Tensions: Helps in minimizing postoperative pain and irritation.
- Improved Local Circulation: Boosts nutrient delivery and healing response.
- Enhanced Mobility Maintenance: Prevents adjacent segment stiffening and preserves spinal flexibility.
- Decreased Complication Rates: Minimizes risk factors associated with mechanical overload and degeneration in treated regions.
Facilities such as Neurothérapie Montréal offer specialized programs combining spinal decompression with manual therapies and functional exercises to expedite recovery. The use of advanced equipment like HillDT and Chirotouch during rehabilitation allows precision monitoring and ensures patient safety.
| Rehabilitation Component | Purpose | Expected Outcome |
|---|---|---|
| Decompression Therapy | Reduce inflammation and nerve tension | Diminished pain, improved comfort |
| Circulatory Enhancement | Promote healing and nutrition | Faster tissue regeneration |
| Mobility Exercises | Maintain and restore range of motion | Prevention of segmental stiffness |
| Manual Therapy | Support structural alignment | Optimized biomechanics |
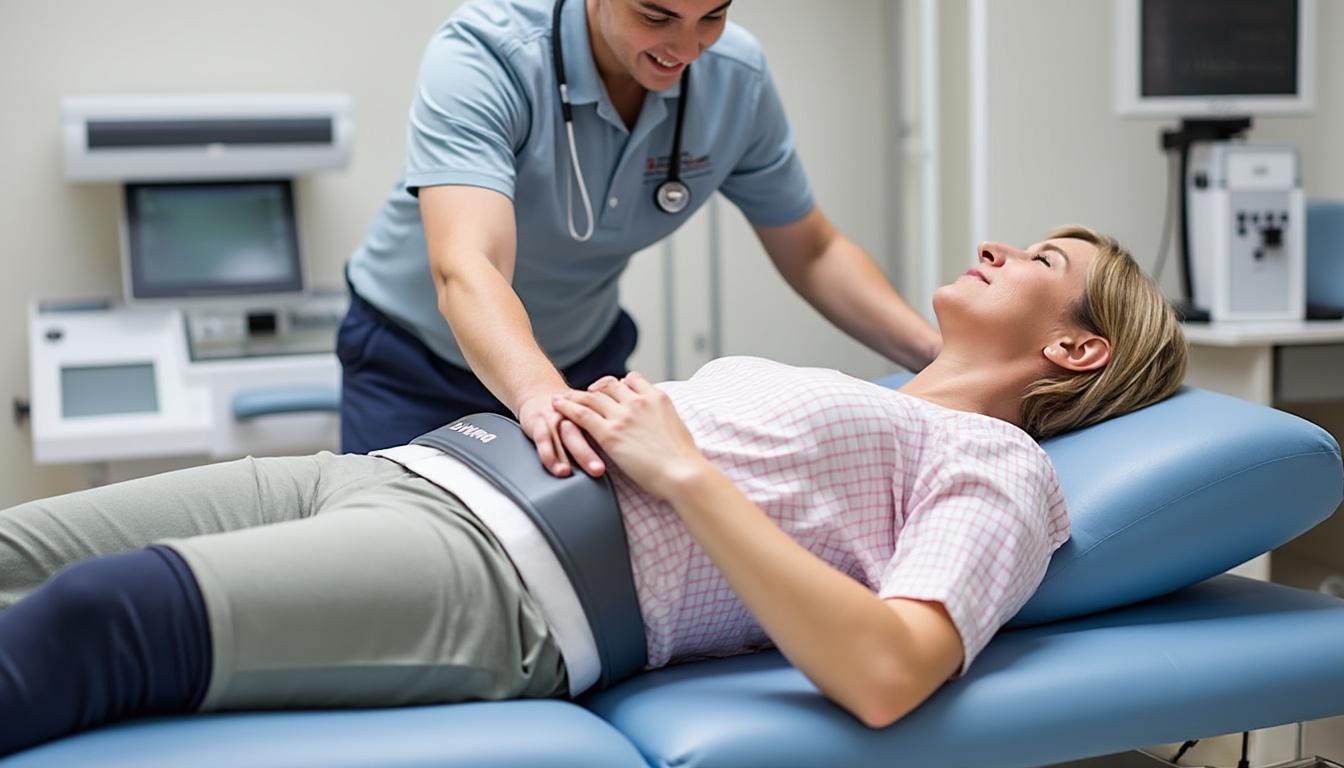

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
International Collaborations Enhancing Surgical Back Care: From Canada to Europe
When conservative care including spinal decompression fails to resolve debilitating spinal conditions, surgical intervention becomes necessary. Today, international collaborations, particularly between Canada and leading European centers, streamline surgical access and postoperative support for complex spine cases.
Coordinated efforts include:
- Preoperative Evaluation by Experts: Canadian clinics like TAGMED work closely with European surgical centers to ensure appropriate patient selection.
- Personalized Surgical Referral and Planning: Collaboration with organizations such as Franchir guarantees matching patients with advanced therapies, including minimally invasive techniques and dynamic implants.
- Patient Logistics Management: Coordination of travel, accommodation, and administrative procedures to ease patient experience abroad.
- Comprehensive Postoperative Follow-up: Neurothérapie Montréal maintains continuity of care upon patient return, focusing on rehabilitation and complication prevention.
This global network fosters access to cutting-edge procedures like the TOPS and Intraspine implants and robotic-assisted spine surgeries. Collaborative expertise dramatically reduces wait times, promoting timely interventions critical for optimal neural and functional outcomes.
| Service | Provider | Description | Benefit to Patient |
|---|---|---|---|
| Initial Evaluation | TAGMED | Candidate assessment and treatment supervision | Optimized treatment plan |
| Surgical Referral | Franchir | Access to European surgical centers with advanced technologies | Reduced delays and expert care |
| Travel Coordination | Franchir | Logistical support for medical travel | Streamlined patient experience |
| Postoperative Follow-up | Neurothérapie Montréal | Comprehensive rehab and monitoring | Sustained recovery and complication prevention |

International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…
Comparing Spinal Decompression Devices: From SpineMED to Cox Technic
Choosing the right spinal decompression device is critical for treatment efficacy and patient comfort. Various manufacturers have introduced innovations that differ in mechanism, precision, and support features.
Highlights of leading devices include:
- SpineMED: Offers patient-specific protocols with advanced computer-controlled traction and feedback systems ensuring safety and optimized outcomes.
- DRX9000: Recognized for precise decompression cycles targeting lower back pain and herniated discs.
- Axiom DRX: Incorporates biofeedback mechanisms enhancing individualized therapy.
- VAX-D: Utilizes computerized traction with automated tension adjustments enhancing patient comfort.
- Cox Technic: A conservative spinal manipulation method complementing decompression by focusing on restoring function and alignment.
Clinics like Lordex Spine Institute and SpinalAid Centers often combine these technologies with manual therapies, delivering holistic care. Patient preferences, clinical indications, and anatomical considerations influence device selection significantly.
| Device | Technology | Primary Use | Special Features |
|---|---|---|---|
| SpineMED | Computer-controlled decompression | Chronic low back pain, disc herniation | Dynamic traction adjustments, patient comfort sensors |
| DRX9000 | Motorized decompression with sensory feedback | Lower back pain, sciatica | Precision cycles, programmable tension |
| Axiom DRX | Biofeedback integrated traction | Disc injuries, nerve impingement | Real-time tension monitoring |
| VAX-D | Automated computerized traction | Various spinal pathologies | Patient comfort focus, customizable protocols |
| Cox Technic | Spinal manipulation and decompression | Chronic pain, functional improvement | Manual therapy combined approach |

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
Guidelines and Best Practices for Safe and Effective Spinal Decompression
Ensuring patient safety and optimizing therapeutic outcomes mandates adherence to established guidelines. Expert healthcare professionals emphasize comprehensive assessments, including imaging and neurological evaluations, before initiating decompression therapy. Contraindications such as spinal instability, infections, or severe osteoporosis must be ruled out.
Recommendations for best practice include:
- Personalized Treatment Planning: Adjusting decompression parameters for each patient’s unique anatomy and symptomatology.
- Monitoring and Feedback Integration: Using devices like Chirotouch for continuous tracking of patient response and early identification of adverse effects.
- Combining Therapies: Incorporating additional modalities such as physical therapy, manual adjustments, and pain management strategies.
- Patient Education: Informational sessions to promote understanding of treatment goals, expected outcomes, and home care instructions.
- Regular Reassessments: Periodic evaluations to refine protocols and decide on modality adjustments or escalation.
Digital resources such as comprehensive guides on spinal decompression and patient-friendly information from institutions actively contribute to informed consent and participation. Safety remains paramount in all clinical settings, with institutions like SpinalAid Centers pioneering integrated care models that prioritize patient well-being.

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…
Spinal Decompression Therapy’s Role in Reducing Healthcare Costs and Improving Quality of Life
The economic burden of chronic back conditions is enormous globally, encompassing direct medical costs and indirect productivity losses. Spinal decompression therapy offers a cost-effective non-surgical alternative that reduces reliance on expensive surgeries, long-term medication use, and disability benefits. Patients report substantial improvement in pain levels, functionality, and overall life satisfaction following treatment courses integrating modalities like HillDT and DRX9000.
Key economic and social benefits include:
- Reduced Surgical Interventions: Many patients delay or avoid surgery altogether.
- Lower Medication Consumption: Decreased dependence on opioids and NSAIDs diminishes side effect risks and healthcare utilization.
- Accelerated Return to Work: Enhanced mobility and pain control facilitate quicker resumption of occupational activities.
- Improved Mental Health: Relief from chronic pain lessens depression and anxiety commonly associated with disability.
- Overall Patient Empowerment: Active engagement in non-invasive therapies fosters a sense of control and resilience.
| Economic Aspect | Impact | Long-Term Patient Benefit |
|---|---|---|
| Surgery Avoidance | Decreased healthcare spending | Less traumatic treatment experience |
| Medication Reduction | Cost savings on pharmaceuticals | Reduced side effect burden |
| Faster Recovery | Lower absenteeism and disability costs | Improved productivity and well-being |
| Psychosocial Gains | Reduced mental health care requirements | Enhanced quality of life |
| Patient Engagement | Better adherence to therapy | Sustained health improvements |
The Importance of Spinal Decompression: Expert Recommendations Explained
Benefits of Spinal Decompression Therapy
Conditions Treated
Typical Treatment Durations
Devices Used
Conservative Care Steps
Frequently Asked Questions
Why is spinal decompression important?
Spinal decompression helps relieve pressure on spinal nerves, promoting healing and reducing pain.
Is the treatment painful?
Most patients experience little to no pain during the therapy, with some reporting a gentle stretching sensation.
How soon will I see results?
Results vary depending on the condition, but many patients notice improvement within weeks.

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…
Frequently Asked Questions About Spinal Decompression Therapy
Is spinal decompression therapy painful?
Spinal decompression is generally painless. Patients typically report a sensation of gentle stretching with most experiencing increased comfort during and after sessions.
How many sessions are required for spinal decompression?
Treatment plans usually consist of 15-30 sessions, adjusted based on the patient’s condition and response. Personalized protocols ensure optimal results.
Are there any contraindications for spinal decompression?
Patients with spinal instability, active infections, or severe osteoporosis should avoid decompression therapy. A thorough evaluation ensures safety before commencing treatment.
Can spinal decompression replace surgery?
While decompression can delay or sometimes obviate the need for surgery, it is not a definitive cure in all cases. It is most effective as part of a comprehensive treatment plan.
Is spinal decompression used alongside other therapies?
Yes, spinal decompression is commonly combined with physical therapy, manual manipulation, and pain management to maximize clinical outcomes.




