How Comparing Spinal Care Practices Between France and Quebec Enhances Clinical Outcomes
November 1, 2025
Addressing Disc Herniations in Sainte-Thérèse: Essential Questions for Your Osteopath and Insights on Neurovertebral Decompression Treatment
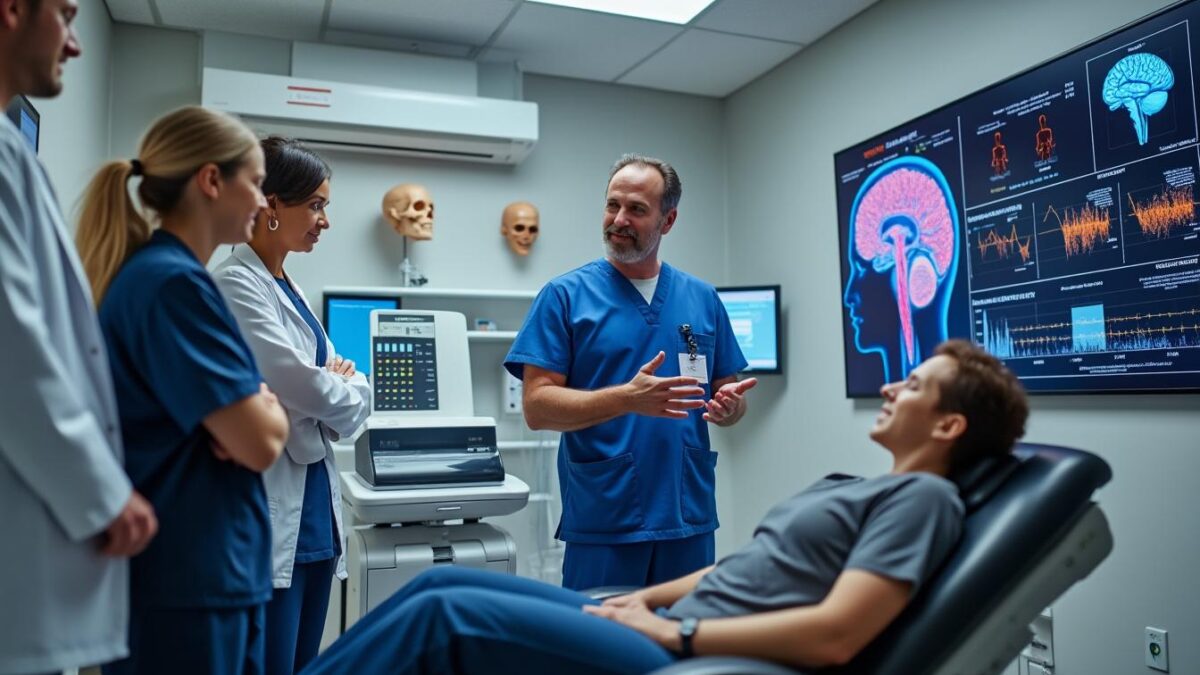
November 1, 2025Advancements in spinal surgery and postoperative care are increasingly shaped by innovative technologies that facilitate patient recovery and enhance outcomes. Among these, repetitive transcranial magnetic stimulation (rTMS) stands out as a non-invasive neuromodulation technique gaining prominence for its role in managing neuropathic pain and supporting neurological rehabilitation post-surgery. This emerging approach not only complements surgical interventions but also contributes substantially to improving patients’ quality of life through enhanced cerebral plasticity and mood regulation.
As surgical techniques evolve swiftly, comprehensive patient care transitions beyond the operating room, integrating therapies like rTMS into the continuum of treatment. Specialists such as Philippe Mazaltarim, director at Neurothérapie Montréal, highlight the synergistic potential of rTMS when combined with coordinated care pathways spanning transatlantic collaboration. This integration offers tailored protocols that address pain, psychological resilience, and functional recovery, especially for complex spinal pathologies treated surgically in France and followed up in Quebec.
This article explores key insights from experts on post-surgery rTMS application, elucidating its impact on recovery trajectories, pain management, and overall rehabilitation. By analyzing clinical protocols, multidisciplinary coordination, and patient experiences, this discussion emphasizes the evolving landscape of neuromodulation in spinal postoperative integration, relevant to clinicians and patients worldwide.
Optimizing Recovery After Spinal Surgery: The Essential Role of rTMS in Postoperative Pain and Neurological Rehabilitation
Spinal surgeries vary drastically in their complexity, from straightforward decompression procedures to motion-preserving artificial disc replacements and arthrodesis (spinal fusion). Each surgical type demands a customized postoperative approach that considers the unique healing and functional restoration requirements. Repetitive transcranial magnetic stimulation (rTMS) emerges as a key adjunctive therapy in this context, addressing both neuropathic pain and neurological recovery.
For simple decompressive surgeries like lumbar decompression without fusion, early mobilization is crucial. Patients often commence walking within two days, with return to work or sports activity planned within four to six weeks. In this recovery window, rTMS serves primarily as a pain modulation tool. By targeting motor cortex regions involved in the transmission and perception of neuropathic pain, it helps reduce reliance on potent analgesics, improving patient comfort and encouraging mobility. Clinical evidence supports this role, as detailed in research authorized by organizations using devices such as Magstim and NeuroStar, which demonstrate effective cortical modulation for pain relief without significant side effects.
Motion preservation surgeries, including cervical and lumbar artificial disc implants, present more intricate challenges. The aim is to maintain vertebral mobility and avoid rigidity, necessitating careful neurological rehabilitation. rTMS protocols tailored for these patients stimulate cerebral plasticity, enhancing neural adaptability and minimizing risks such as ankylosis or functional loss. Such interventions have enabled patients to resume competitive sports in approximately three months. In addition to fostering physical recovery, rTMS’s impact on the prefrontal cortex offers beneficial stress and mood regulation during the psychologically demanding postoperative phase.
Spinal fusion surgeries, however, involve longer and more complex healing processes. Patients experience restricted spinal movement, and many endure chronic pain syndromes such as post-laminectomy syndrome. In these cases, rTMS acts as a non-pharmacological strategy to alleviate persistent neuropathic pain and modulate mood disorders that commonly co-occur postoperatively. According to Philippe Mazaltarim’s clinical practice and the latest guidelines, integrating rTMS significantly improves functional outcomes and psychological well-being, serving as a complement to standard drug regimens.
| Type of Surgery | Key Recovery Phases | Specific rTMS Benefits | Typical Resumption Timeline |
|---|---|---|---|
| Simple Decompression | Early mobilization, neuropathic pain reduction | Pain management, reduced analgesic use, enhanced comfort | Walking: Day 2, Work: 4-6 weeks |
| Motion Preservation (Artificial Discs) | Neurological rehab, mobility maintenance, stress management | Plasticity enhancement, faster recovery, mood support | Return to sports: ~3 months, Work: adapted schedule |
| Arthrodesis (Spinal Fusion) | Fusion protection, chronic pain prevention, long-term follow-up | Post-laminectomy pain reduction, psychological support | Controlled walking: 1-2 weeks, Work: >8 weeks |
- Early initiation of rTMS following clinical stabilization
- Individualized stimulation parameters based on patient response
- Integration with multidisciplinary rehabilitation programs
- Continuous monitoring for pain and psychological symptoms
- Coordination between neurology, surgery, and rehabilitation teams
These strategies collectively underscore how rTMS enhances recovery by targeting specific neurophysiological processes related to pain and neural plasticity, facilitating smoother and quicker postoperative convalescence. Studies found in the Clinical Neurophysiology Journal detail the strength of rTMS in post-surgical contexts, supporting its adoption by centers including Neurothérapie Montréal.

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…
Integrated Postoperative Follow-up Models: The Coordination of Transatlantic Care and Its Impact on rTMS Efficacy
Postoperative care for spinal surgery patients transitioning from France to Quebec exemplifies the importance of seamless international collaboration. Philippe Mazaltarim’s leadership at Neurothérapie Montréal illustrates an integrated model where preoperative evaluation, surgical intervention, and postoperative rehabilitation are connected through coordinated communication and shared protocols.
The patient journey begins with meticulous preoperative preparation in Quebec, including detailed neurofunctional assessments and thorough medical history review by specialists aligned with the current standards in spinal surgery education like those from the French Spine Surgery Diploma curriculum. The partnership with French surgical centers managed through logistics and accommodation by Franchir, and continuous accompaniment provided by SOS Tourisme Médical enhance patient confidence and safety.
Following surgery, the focus shifts to comprehensive rehabilitation incorporating rTMS. This phase is critical as it addresses challenges like chronic pain persistence, postoperative neurological complications, and psychological distress. Customized rTMS protocols administered at Neurothérapie Montréal are adjusted through regular clinical evaluations, combining neuromodulation with physical therapy and psychological support. This model counters the risks of inadequate follow-up that often lead to long-term disability or depression.
| Stakeholder | Role in Patient Journey | Concrete Actions |
|---|---|---|
| Dr. Sylvain Desforges & TAGMED | Initial evaluation and conservative treatments | Neurofunctional assessments, pre-surgery optimization |
| Franchir | Surgical referral and logistical coordination | Selection of surgical center, travel and accommodation planning |
| SOS Tourisme Médical | Administrative support and patient guidance | Information dissemination, assistance with documentation and eligibility |
| Neurothérapie Montréal | Postoperative neuromodulation and rehabilitation | Personalized rTMS protocols, clinical monitoring, psychoeducation |
- Secure, iterative communication channels between French and Canadian teams
- Patient-centric planning addressing individual medical and logistical needs
- Robust data collection to guide therapy adjustments including rTMS doses
- Holistic approach integrating physical and psychological recovery
- Transparent information sharing fostering patient empowerment
This multidisciplinary approach, supported by technology and precise management, optimizes rehabilitation quality while minimizing complications such as persistent neuropathic pain or cognitive decline. Detailed insights on post-surgery integration practices are available through expert articles like those on post-surgery rTMS integration, highlighting the transformative power of combined transatlantic care.

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Enhancing Pain Management After Spinal Surgery: rTMS as a Non-Pharmacological Alternative for Chronic Neuropathic Pain
Persistent neuropathic pain is a common and debilitating sequela of spinal surgeries, including post-laminectomy syndrome. Conventional pharmacologic approaches often provide limited relief and can incur adverse effects, prompting exploration of alternative therapies like rTMS, which has gained traction across international guidelines for its safety and efficacy.
rTMS utilizes focused magnetic pulses to modulate cortical excitability, particularly within motor and prefrontal cortices, thereby disrupting maladaptive pain pathways and promoting endogenous analgesia. Devices from manufacturers such as BrainsWay, MagVenture, and Nexstim have contributed to evolving clinical protocols that provide durable pain relief without the risks of addiction or systemic side effects.
Beyond pain relief, rTMS supports psychological stabilization by influencing neural circuits involved in mood regulation. Patients experiencing post-op depression or anxiety benefit from this neuromodulatory effect, which fosters adherence to rehabilitation programs and improves overall quality of life during recovery.
Clinical reports from Neurothérapie Montréal feature cases such as Paul, who after lumbar arthrodesis experienced a 70% decrease in neuropathic pain within weeks of rTMS treatment initiation. Supporting literature reflects these outcomes, as published in journals emphasizing the therapeutic potential of rTMS after spine surgeries. Details of safety profiles and efficacy are available in comprehensive reviews like the one by the TMS clinical review report.
- Targeted stimulation of motor cortex areas related to pain perception
- Reduction and sometimes elimination of need for strong analgesics
- Improvement in associated psychological symptoms like depression and anxiety
- Adjunctive use alongside physical rehabilitation for enhanced functional gains
- Careful selection of candidates with contraindications screened pre-treatment
| rTMS Application | Evidenced Benefits | Key Devices Involved |
|---|---|---|
| Neuropathic Pain Control | Significant pain reduction, improved comfort, reduced drug dependency | BrainsWay, Magstim, NeuroStar |
| Mood Regulation Post-Surgery | Decreased depressive symptoms, enhanced rehabilitation adherence | Neuronetics, Yiruide Medical |
| Functional Recovery Support | Enhanced motor function and neural plasticity stimulation | MagVenture, Nexstim |
The multidisciplinary approach that combines rTMS with surgical care and psychological support represents a paradigm shift in the management of postoperative spinal patients. Resources like the hidden benefits of integrating rTMS explore how this synergy translates to practical improvements noted by patients and clinicians alike.

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…
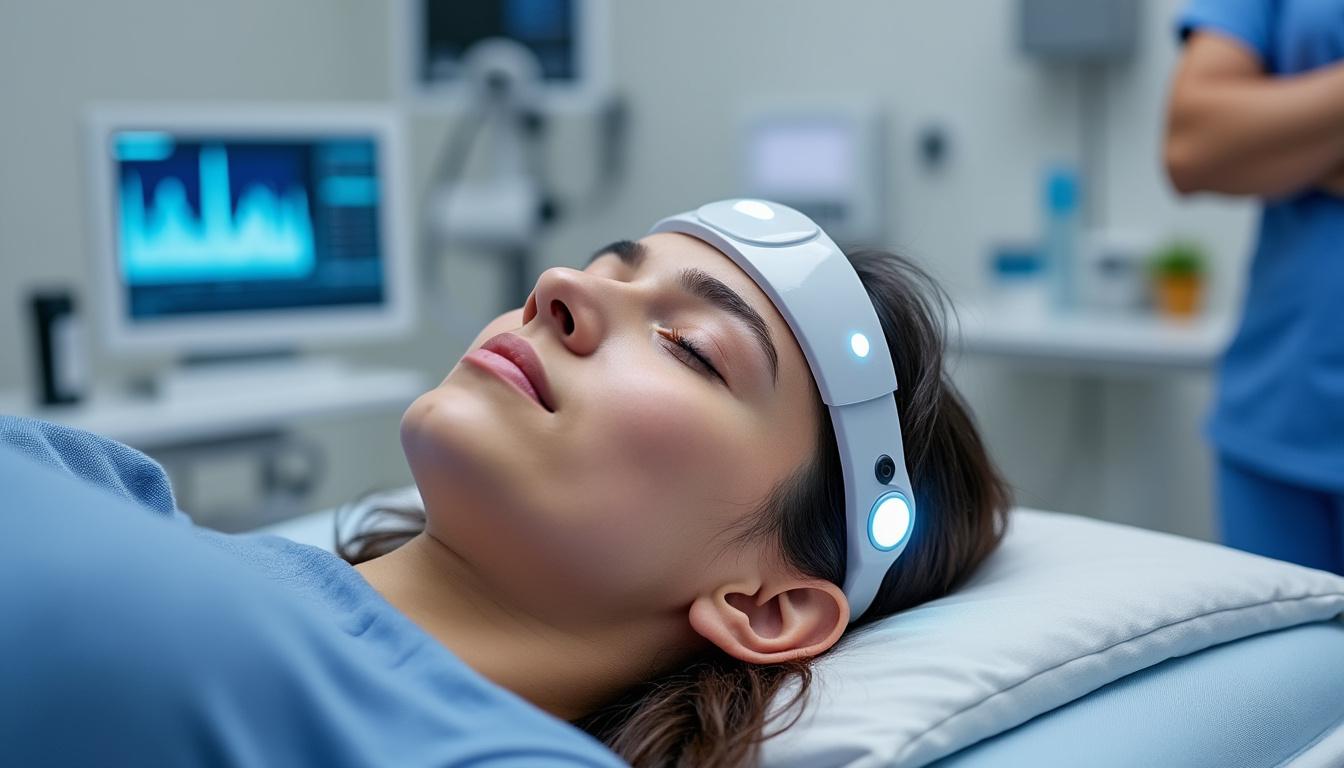
Leveraging Cutting-Edge Neuromodulation Technologies: Devices and Protocols Driving rTMS Effectiveness
The ongoing refinement of rTMS therapies depends significantly on the quality and versatility of neuromodulation devices. Leading manufacturers such as Magstim, NeuroStar, and Yiruide Medical have contributed dynamic platforms that accommodate varied clinical needs through adjustable stimulation parameters, coil designs, and software-guided protocols.
One of the pivotal advances is the incorporation of neuronavigation systems, exemplified by Nexstim’s technology, which ensures precise cortical targeting. This accuracy enhances treatment efficacy and patient comfort, reducing off-target effects. Additionally, MagVenture and BrainsWay have developed stimulators compatible with diverse clinical environments, from inpatient rehabilitation to outpatient clinics.
Protocols evolve to include multi-session frameworks tailored to surgical types and individual symptoms, balancing frequency and intensity to maximize neuromodulatory impact while preserving safety. Innovation also extends to portable devices like eNeura and Remed, which offer patients more accessible maintenance therapy options post-discharge, thus supporting long-term recovery trajectories.
- Neuronavigation-assisted targeting for optimal stimulus delivery
- Personalization of stimulation frequency, intensity, and session duration
- Integration with neuroimaging data to map functional brain areas
- Portable and clinic-friendly device options increasing patient adherence
- Continuous protocol adjustments based on clinical feedback and research
| Device Manufacturer | Technical Features | Clinical Advantages |
|---|---|---|
| Magstim | Transcranial coil design, adjustable pulse parameters | Effective pain modulation, widely used in post-spinal surgery care |
| Nexstim | Neuronavigation-guided stimulation, precise cortical targeting | Enhanced accuracy, reduced adverse effects, tailored treatments |
| BrainsWay | Deep TMS technology, specialized coils for different brain regions | Improves mood and functional recovery, fewer treatment sessions needed |
| Yiruide Medical | Versatile stimulators, clinical software integration | Adaptable protocols, supports psychological rehabilitation |
As research elucidates more precise mechanisms of cortical plasticity, these device innovations are pivotal to expanding rTMS accessibility and effectiveness. For an in-depth review of current technology and clinical application, consult expert literature such as the comprehensive post-surgery rTMS integration guide.

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
Patient Experiences and Clinical Outcomes: Real-World Evidence Supporting rTMS in Postoperative Spine Care
Clinical outcomes associated with postoperative rTMS reveal marked improvements in pain relief, mood enhancement, and functional recuperation. Patients participating in Neurothérapie Montréal’s programs report reduced neuropathic discomfort, less reliance on opioids, and better psychological well-being. These patient-centered results are corroborated by multicenter clinical trials and case studies documented globally.
One illustrative case involves Mélanie, a 42-year-old athlete who underwent lumbar fusion surgery. Traditional concerns regarding permanent mobility loss were mitigated through a specialized rTMS protocol. Over three months, she progressively regained full sporting capacity, achieving pre-injury performance levels. This outcome underscores the potential of rTMS to complement surgical success with enhanced rehabilitation.
| Patient Profile | Surgical Intervention | rTMS Protocol | Outcome |
|---|---|---|---|
| Paul, 55 years | Lumbar arthrodesis | 30 sessions, motor cortex targeting | 70% pain reduction, work resumption within 1 month |
| Mélanie, 42 years | Lumbar fusion (arthrodesis) | 40 sessions, mood and pain modulation | Restored athletic performance in 3 months |
| John, 60 years | Cervical decompression | 20 sessions, neuropathic pain protocol | Reduced analgesic intake, improved quality of life |
- Structured therapy schedules accommodate patient availability and recovery phases
- Adaptations in stimulation focus according to symptom evolution
- Incorporation of psychological support for comprehensive healing
- Use of validated clinical scales to measure functional and emotional improvement
- Continuous feedback loop between patient and care teams
Such outcomes underscore the value of integrating rTMS into postoperative care pathways. They align well with the findings in clinical trials such as those explored in journals like the Trials Journal and real-world insights noted by surgical rehabilitation experts.


International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…
Multidisciplinary Collaboration: Synergizing Surgical Advances and Neuromodulation to Improve Patient Outcomes
Successful postoperative integration of rTMS is contingent upon multidisciplinary teamwork uniting neurosurgeons, neurologists, physiatry specialists, and psychologists. This collaborative approach ensures personalized care plans, constantly refined based on evolving clinical data and patient feedback.
As spinal surgery techniques benefit from innovations such as robotic assistance and 3D imaging platforms demonstrated by eCential Robotics, integrating neuromodulation requires equally sophisticated clinical frameworks. The synergy between surgical precision and rTMS-driven cortical modulation results in superior recovery trajectories, with reduced complications and enhanced wellbeing.
Key elements of an effective multidisciplinary model include:
- Preoperative planning incorporating neurofunctional assessments and risk stratification
- Close communication channels allowing timely adjustments to rehabilitation protocols
- Ongoing education for clinical staff on evolving rTMS evidence and techniques
- Patient engagement strategies fostering active participation in recovery
- Data sharing platforms to monitor longitudinal outcomes and inform future standards
| Team Member | Role in Postoperative Care | Contribution to rTMS Integration |
|---|---|---|
| Neurosurgeons | Perform operations, select candidates | Coordinate timing and surgical data for rTMS initiation |
| Neurologists/Neurotherapists | Design rTMS protocols | Personalize stimulation settings, monitor side effects |
| Physiatrists | Lead physical rehabilitation | Integrate rTMS with locomotion therapies |
| Psychologists | Address mood disorders | Offer cognitive behavioral support complementing neuromodulation |
The efficiency of these coordinated efforts is demonstrated in international initiatives capturing the benefits of rTMS in postoperative spinal surgery, accessible in expert resources such as comparative surgical techniques and motion technologies review.

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
Educational Expansion and Research Frontiers Supporting rTMS Postoperative Adoption
Institutional training programs and scientific studies play critical roles in mainstreaming rTMS within spinal postoperative care. Academic diplomas and certifications such as those provided by the University of Bordeaux and the French Society of Spinal Surgery (SFCR) emphasize neuromodulation as an essential competency for spinal surgeons and rehabilitation specialists.
Research advancing the understanding of rTMS mechanisms informs clinical refinements. Recent clinical trials, systematic reviews, and meta-analyses published in respected journals provide ongoing evidence for its efficacy and tolerability. Additionally, emergent technologies in robotic-assisted surgery and endoscopic spine procedures expand the contexts where rTMS can be integrated effectively.
- Academic diplomas and inter-university certifications fostering neuromodulation expertise
- Clinical trial registries offering transparent records of rTMS application outcomes
- International guideline updates reflecting evolving best practices in rTMS
- Conferences and spinal surgery courses promoting interdisciplinary knowledge exchange
- Collaboration networks ensuring continuous research and clinical feedback
| Institution | Program or Research Focus | Contribution to rTMS Integration |
|---|---|---|
| University of Bordeaux | Diplomas in Medicine and Neuromodulation | Training in cutting-edge neuromodulation techniques |
| SFCR (French Society of Spinal Surgery) | Advanced spinal surgery training and rTMS protocols | Curriculum development and clinical guidelines |
| EuroSpine | Endoscopic spine surgery courses encompassing neuromodulation | International educational collaboration |
| Neurothérapie Montréal | Clinical research & implementation of rTMS post spinal surgery | Integration of scientific advances into practice |
For professionals seeking to deepen understanding and improve postoperative outcomes with rTMS, resources such as the clinical neuropsychology journal on neuromodulation provide comprehensive updates encapsulating current research, protocols, and patient outcomes.
Comparative Table: Post-Surgery rTMS Integration Programs
| Institution | Program | Contribution |
|---|

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…
Psychosocial Impact and Mood Stabilization: rTMS as a Key Factor in Post-Spinal Surgery Mental Health Recovery
Postoperative psychological challenges such as anxiety and depression have significant effects on recovery quality following spinal surgery. Persistent pain, reduced mobility, and uncertainty about outcomes commonly contribute to mood disturbances, which can impede physical rehabilitation and extend convalescence.
rTMS offers a notable advantage in this domain by targeting cortical regions implicated in mood regulation, including the dorsolateral prefrontal cortex. Research illustrates its efficacy in alleviating depressive symptoms post-surgery and improving patients’ emotional resilience. Devices including NeuroStar and Yiruide Medical deliver protocols optimized for this purpose, complementing traditional psychological therapies and pharmacological interventions.
Psychosocial support integrated with rTMS enhances coping strategies, optimizes treatment continuity, and encourages patient adherence to rehabilitation plans. These factors collectively contribute to more favorable physical and emotional outcomes, underscoring the holistic benefit of rTMS in spinal postoperative care.
- Targeting mood regulation centers to reduce postoperative depression
- Supporting anxiety management and emotional resilience
- Complementing psychological counseling and medication
- Improving patient motivation for active rehabilitation participation
- Monitoring emotional progress alongside physical recovery metrics
| Psychosocial Aspect | rTMS Contribution | Device Examples |
|---|---|---|
| Depression Reduction | Alleviates depressive symptoms and improves mood stability | NeuroStar, BrainsWay |
| Anxiety Control | Enhances emotional regulation and stress resilience | Yiruide Medical, Remed |
| Rehabilitation Engagement | Boosts motivation and adherence to therapy programs | Neuronetics, Magstim |
Integrating mental health with the physical recovery journey represents progressive patient-centric care. Further information on rTMS’s psychosocial benefits can be found in specialist publications addressing post-surgical rehabilitation, such as neurological outpatient practice journals.

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…
Future Directions and Innovations for rTMS in Postoperative Spine Surgery Integration
Looking ahead, rTMS will likely expand its role within postoperative spinal surgery protocols. Advancements in neuromodulation technology, including smarter stimulation algorithms and biofeedback integration, promise to refine treatment precision further. Emerging clinical data will continue to inform personalized medicine approaches, balancing efficacy with patient-specific factors.
Integration with telehealth platforms and portable stimulation devices like eNeura allows extended therapy beyond clinical settings, enhancing adherence and convenience. Moreover, combination therapies involving rTMS alongside regenerative medicine and robotics hold potential to revolutionize postoperative care, emphasizing comprehensive functional restoration.
- Development of adaptive rTMS protocols based on real-time patient feedback
- Hybrid models combining neuromodulation with robotic-assisted rehabilitation
- Expanded telemedicine application for remote monitoring and therapy delivery
- Synergistic approaches involving stem cell therapy and neuromodulation
- Continued international collaboration to standardize and optimize treatments
| Innovation Area | Expected Impact | Example Technologies |
|---|---|---|
| Adaptive Protocols | Personalized and responsive stimulation improving outcomes | CloudTMS, MagVenture |
| Robotic Integration | Enhanced functional recovery through multisystem coordination | eCential Robotics |
| Telehealth Expansion | Increased access and adherence via remote treatment | eNeura, Remed |
These anticipated advancements build on current understanding and align with the evolving clinical landscape. Professionals are encouraged to consult ongoing studies and specialty conferences to stay abreast of innovations, such as those highlighted by leading academic centers in 2025.
What specific benefits does rTMS provide after spinal surgery?
rTMS primarily reduces neuropathic pain, supports brain plasticity enhancing neurological recovery, helps stabilize mood disorders, and limits the need for strong analgesics post-surgery.
When is the optimal time to begin rTMS in postoperative care?
rTMS typically starts within the first few weeks after surgery once initial healing is stable, with frequency and intensity tailored to patient’s clinical status and progression.
Are there any contraindications or risks with rTMS after spinal surgery?
While generally safe, rTMS is contraindicated in patients with ferromagnetic implants near the stimulation site; thorough medical evaluation is essential before initiation.
Can rTMS replace physical therapy after spine surgery?
rTMS complements but does not replace physical rehabilitation; it modulates pain and neural pathways to enhance physical therapy outcomes and overall recovery.
How can patients arrange continued rTMS treatment post-surgery in Quebec?
Patients can contact Neurothérapie Montréal directly for personalized evaluations, where care teams design integrated rTMS protocols tailored to each patient’s needs after surgery in France.