Unveiling the Hidden Benefits of Comprehensive Preoperative Assessment
November 21, 2025
IntraSPINE® in Laval: Innovative and Approved Intervention
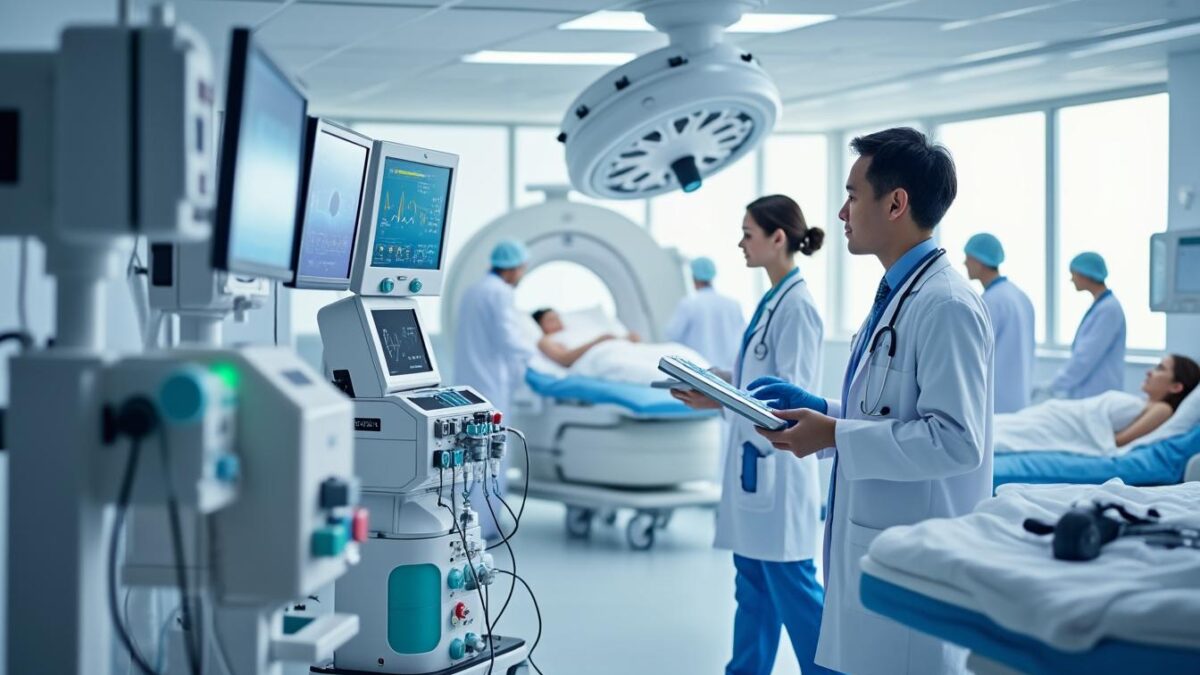
November 21, 2025The rising significance of medical devices in healthcare delivers unprecedented enhancements in diagnosis, treatment, and patient outcomes. However, this progress hinges on rigorous quality assurance, stringent medical device certification, and unwavering adherence to regulatory compliance standards. For complex specialties such as spinal surgery, the integration of certified devices establishes foundational trust between clinicians and patients, ensuring safety and clinical effectiveness. As healthcare systems evolve into more technologically advanced infrastructures, understanding how device quality and institutional certifications influence patient safety, risk management, and product reliability is paramount in amplifying clinical outcomes globally.
Within the dynamic medical landscape of 2025, certified medical devices undergo robust validation processes that encompass patient-centered assessments and long-term performance evaluations. The collateral impact of these measures extends beyond the device alone—enhancing healthcare standards across multidisciplinary teams and strengthening coordinated clinical workflows. Consequently, not only is optimized care realized through innovative implants and surgical techniques, but sustained patient confidence flourishes, fueling healthcare success stories worldwide.
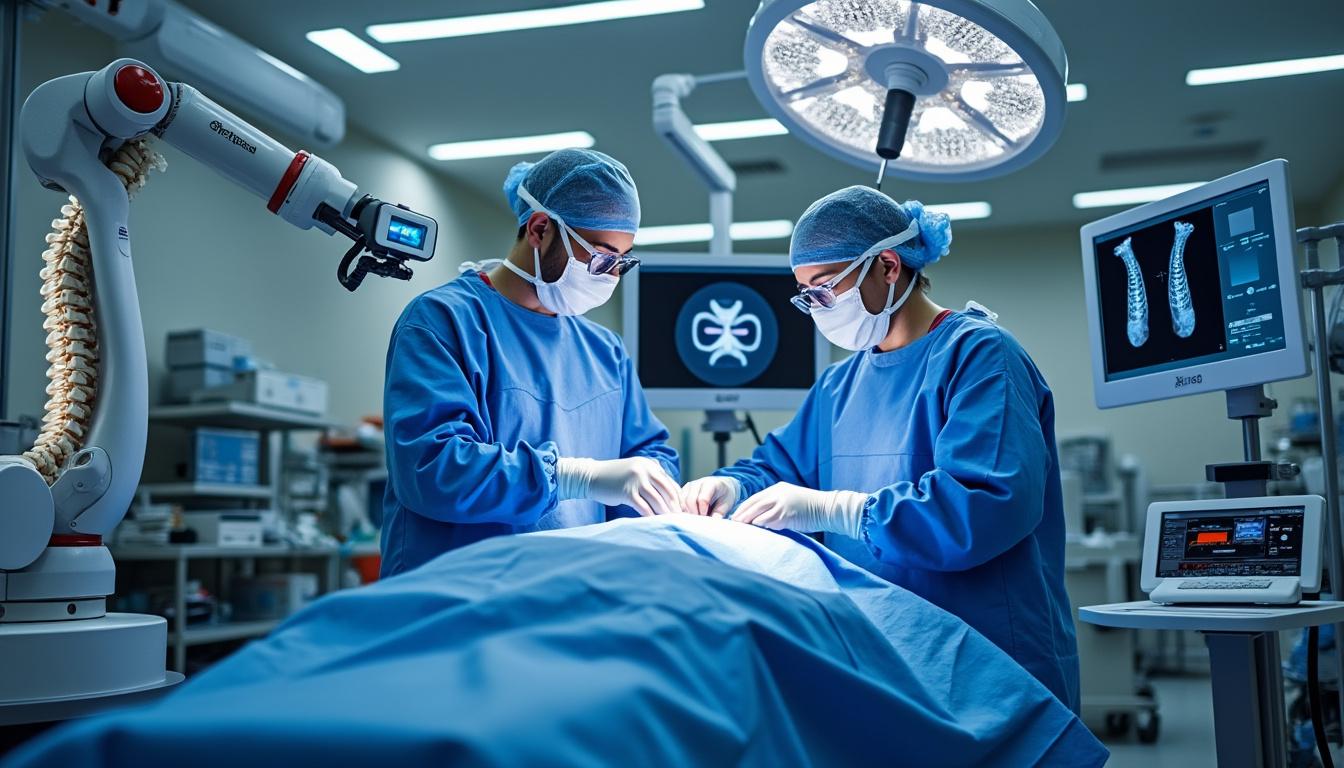
Quality Assurance in Medical Device Manufacturing: A Cornerstone of Clinical Effectiveness
Quality assurance (QA) in the manufacturing of medical devices is indispensable for delivering safe and reliable solutions integral to patient care. The demand for uncompromising quality is heightened in fields like spinal surgery, where devices such as TOPS, Intraspine, and B-DYN implants have transformed therapeutic landscapes.
Robust QA frameworks encompass comprehensive inspection protocols that assess raw materials, production processes, and final product performance. Systematic risk management underpins these processes—identifying potential device failures before clinical use. For instance, the traceability mechanisms embedded in modern devices facilitate post-market surveillance and materiovigilance, providing mechanisms to swiftly address adverse events and device malfunctions. This multi-tiered approach ensures that medical devices meet established healthcare standards, reinforcing clinical outcomes through product reliability.
A crucial facet of QA involves iterative device validation, where prototypes undergo rigorous testing in simulated clinical scenarios. Such procedures include biomechanical assessments, endurance tests, and user feedback under real-world conditions, confirming the device’s durability and compatibility with human anatomy. Research highlights that quality-driven approaches foster continuous improvement cycles, propelling innovations that enhance surgical precision and patient comfort. Consequently, hospitals equipped with certified devices achieve lower rates of complications and superior functional recovery.
- Implementation of ISO 13485 certification for standardized quality management in manufacturing.
- Adoption of rigorous in-line inspection and final device verification practices.
- Regular audits aligning manufacturing processes with evolving regulatory frameworks.
- Investment in advanced materials and precision engineering to meet clinical demands.
- Integration of real-time data analytics for quality performance tracking.
| QA Aspect | Impact on Clinical Outcomes | Examples in Spinal Surgery Devices |
|---|---|---|
| Traceability & Matériovigilance | Enables rapid identification and management of device-related complications | Dynamic implants such as TOPS support detailed tracking for safety monitoring |
| Device Validation Testing | Ensures durability and biomechanical compatibility | Intraspine interspinous devices undergo thorough endurance assessments |
| Risk Management Protocols | Minimizes potential patient hazards through preventive controls | Pre-emptive failure mode analysis in B-DYN spring-based stabilizers |
These structured QA processes, detailed in white papers like those from Siemens, showcase that quality assurance directly correlates with improved patient safety and therapeutic efficiency. Emphasizing product reliability contributes significantly to clinical effectiveness, building a solid framework for ongoing advancements in spinal device technology.

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…
Medical Device Certification and Its Role in Enhancing Patient Safety and Regulatory Compliance
Medical device certification is more than a regulatory checkbox; it represents a rigorous validation process that elevates safety and therapeutic performance. Certification ensures devices fulfill international standards such as CE marking in Europe and FDA approval in the United States, offering clinicians confidence in device functionality and compliance.
Spinal surgery benefits profoundly from this certification process, which demands comprehensive clinical data, risk assessments, and quality management systems documentation. These inclusions foster trust and enable transparent communication regarding device capabilities and limitations. An essential component of certification includes the assessment of clinical outcomes, where patient-reported metrics and clinical outcome assessments (COAs) are integrated to demonstrate real-world efficacy, as supported by FDA guidelines.
Certification also encourages ongoing surveillance post-market authorization, requiring manufacturers to maintain quality systems continuously and report adverse events promptly. Such compliance mechanisms foster a culture of patient safety and risk management, significantly reducing incidences of device-related complications and recalls. Furthermore, institutions incorporating certified devices align their practices with international healthcare standards, generating a safer environment for complex interventions such as spine surgeries.
- Completion of clinical trials demonstrating device safety and efficacy.
- Adherence to ISO 14971 for risk management throughout the device lifecycle.
- Implementation of post-market surveillance plans and materiovigilance reporting.
- Coordination between manufacturers, regulatory bodies, and healthcare providers.
- Education of clinical teams about certified device proper use and limitations.
| Certification Element | Clinical Benefit | Regulatory Impact |
|---|---|---|
| Clinical Outcome Assessments (COAs) | Improves treatment personalization and monitoring | Supports FDA patient-centered development approach |
| Risk Management (ISO 14971) | Reduces adverse events and enhances device reliability | Mandatory compliance for device approval |
| Post-Market Surveillance | Enables rapid intervention for device issues | Maintains certification validity |
With medical tourism gaining momentum, the certification status of devices also informs patient decisions, reassuring individuals seeking advanced spinal care abroad. The partnership between Canadian patients and French certified hospitals exemplifies a model intertwining high safety standards with streamlined clinical pathways to optimize every patient’s journey.
Supporting Resources on Certification and Compliance
Detailed guidance about navigating medical device certification and accreditation can be found through platforms that explore the complexities of these processes, helping healthcare providers understand requirements intricately. These resources facilitate informed choices about device procurement and clinical integration.

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Innovations in Certified Medical Devices: Enhancing Clinical Outcomes in Spinal Surgery
Technological advancements in medical devices are reshaping spinal surgery, enabling motion preservation and minimal invasiveness, thus profoundly influencing clinical outcomes. Certified implants integrate innovative biomechanical features ensuring flexibility without compromising stability.
Devices such as TOPS offer dynamic posterior stabilization that maintains segmental mobility, a significant departure from traditional fusion techniques that often induce adjacent segment degeneration. Intraspine devices, acting as interspinous spacers, alleviate symptoms while minimizing surgical trauma and preserving spinal biomechanics. B-DYN’s spring-based stabilization brings improved vertebral flexibility, a promising alternative whenever fusion can be avoided.
These innovations, validated through clinical trials and abiding by strict quality and certification criteria, enable surgeons to tailor interventions precisely. By supporting movement and reducing adjacent vertebral stress, these implants facilitate better postoperative recovery, pain reduction, and enhanced functional independence.
- Dynamic stabilization preserving spinal motion and preventing stiffness.
- Minimally invasive implantation techniques reducing surgical risk.
- Integration of 4K endoscopic visualization systems improving surgical accuracy.
- Continuous product monitoring to ensure longevity and device integrity.
- Customizable implant options corresponding to patient-specific pathology.
| Device | Key Feature | Clinical Advantage | Certifications |
|---|---|---|---|
| TOPS | Dynamic posterior stabilization maintaining mobility | Reduced postoperative pain and preservation of function | CE, FDA-approved |
| Intraspine | Interspinous device offering minimal surgical impact | Lower adjacent segment pressure and surgical trauma | CE marked |
| B-DYN | Spring-loaded dynamic stabilization | Enhanced vertebral flexibility and recovery | CE certified |
Clinically, the adoption of such certified implants aligns with comprehensive care pathways designed for improved patient outcomes and satisfaction. These devices’ integration with national certification frameworks and quality assurance practices creates a robust ecosystem that supports steady progress in spinal healthcare.

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…
Healthcare Standards and Institutional Certification: Elevating Safety in Spinal Surgery Centers
The certification of healthcare institutions plays a vital role in sustaining a culture of safety and clinical excellence, especially in highly specialized fields like spinal surgery. In France, for example, certification processes harmonize patient care quality, healthcare team coordination, and organizational effectiveness through multi-criteria assessments.
These accreditations, renewed on structured cycles, evaluate hospitals against twelve core objectives emphasizing patient-centered care, team collaboration, and systemic risk management. The inclusion of methodologies such as the patient tracer process facilitates ongoing monitoring of individual care trajectories, mapping strengths and areas for improvement.
Certified institutions exhibit lower postoperative complication rates and shorter hospitalizations, as validated by recent studies, affirming certification’s tangible contribution to clinical outcomes. This translates into enhanced patient safety, more efficient resource use, and higher satisfaction scores. For international patients traveling for surgery, institutional certification reinforces trust and supports seamless integration into transnational care networks.
- Patient-centered quality assessments placing patient experience at the forefront.
- Audit systems evaluating organizational processes and risk mitigation strategies.
- Structured team coordination enhancing continuity of care.
- Incident management systems identifying and addressing safety breaches.
- Regular outcome-based reviews promoting continuous quality improvement.
| Certification Objective | Focus Area | Benefit to Spinal Surgery Care |
|---|---|---|
| Patient Quality | Evaluation of care pathways and safety via patient tracer | Personalized management and reduction of postoperative complications |
| Care Teams | Coordination and multidisciplinary collaboration assessment | Enhanced communication ensuring care continuity |
| Institutional Management | Audit-based process verification and incident handling | Secure and compliant surgical environment |
This certification framework, detailed extensively in resources accessible through healthcare organizations, underscores that institutional accreditation is central to ambitious quality-driven care models. Such rigor elevates the safety net surrounding spinal surgeries, leading to superior clinical outcomes.

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
Structured Patient Pathways Facilitated by Certified Devices and Institutions: A Model for Cross-Border Care
International collaboration amplifies the benefits of certification and quality through well-orchestrated patient pathways spanning continents. Canadian patients, for example, gain expedited access to French spinal surgery centers where certified implants and state-of-the-art facilities converge to optimize care quality and safety.
This model relies on strategic partnerships involving local healthcare providers, logistical coordinators, and post-operative rehabilitation services. For instance, clinics such as TAGMED in Montreal oversee thorough preoperative evaluations and conservative treatments. The organization Franchir coordinates seamless hospital selection, travel arrangements, and administrative tasks, mitigating patient stress associated with medical travel.
Following successful interventions employing certified devices, specialized centers like Neurothérapie Montréal provide tailored post-operative care ensuring recovery continuity. This integrated approach ensures a holistic healthcare experience where quality and certification unify to deliver superior clinical outcomes.
- Comprehensive preoperative evaluations to tailor treatment plans.
- Seamless logistical support including surgery scheduling and accommodation.
- Use of internationally certified implants to assure device safety.
- Personalized postoperative rehabilitation integrated across jurisdictions.
- Monitoring and feedback loops maintaining high standards throughout care.
| Step | Responsible Entity | Role and Description |
|---|---|---|
| Evaluation and Conservative Treatment | TAGMED Team | Assessment of pathology and initial management strategies |
| Orientation and Coordination | Franchir | Selection of certified surgeons and hospitals, travel logistics |
| Hospitalization and Surgery | Certified French Centers | Intervention with certified, quality-controlled devices |
| Postoperative Follow-up | Neurothérapie Montréal | Individualized rehabilitation and clinical monitoring |

International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…
Risk Management and Patient Safety: Integrative Approaches through Quality and Certification
Effective risk management anchored in quality assurance and certification directly translates into increased patient safety in spinal surgical care. By systematically identifying hazards associated with medical devices and healthcare delivery processes, stakeholders can mitigate complications and promote favorable clinical outcomes.
One example includes the utilization of the patient tracer method, facilitating collaborative oversight that involves patients and multidisciplinary teams. This engagement reduces the likelihood of adverse events, streamlines workflows, and fosters a transparent safety culture. Furthermore, device certification mandates require robust post-market vigilance mechanisms detecting emerging risks.
Evidence shows that risk reduction strategies considerably lower rates of surgical site infections, allergic reactions to implant materials, and mechanical failures. These measures not only improve individual patient trajectories but also enrich institutional safety records and enhance overall healthcare quality.
- Pre-implantation risk analyses ensuring device suitability.
- Standardization of surgical and sterile techniques across certified centers.
- Implementation of incident reporting systems to quickly address safety breaches.
- Continuous professional development promoting awareness of device-specific risks.
- Use of interoperable information systems supporting evidence-based decisions.
| Risk Management Practice | Clinical Impact | Certification Linkage |
|---|---|---|
| Patient Tracer Technique | Enhances monitoring of care pathway safety | Embedded in hospital certification audits |
| Incident Reporting & Analysis | Prevents recurrence of adverse events | Supports regulatory compliance |
| Post-Market Surveillance | Enables early detection of device failures | Mandatory under certification frameworks |

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
Continuous Improvement and Future Directions in Quality Standards for Medical Devices and Clinical Outcomes
Quality assurance and certification represent evolving fields, continually adapting to technological progress and clinical feedback. The future trajectory points toward integrated digital systems, including artificial intelligence and real-time device performance monitoring, to further enhance product reliability and patient outcomes.
This evolution includes widening clinical outcome assessments to incorporate patient-reported outcomes more comprehensively. Methodologies such as the FDA’s advice on clinical outcome assessments (COAs) facilitate deeper insights into efficacy and patient satisfaction beyond traditional clinical measures.
Healthcare standards are progressively embracing closed-loop quality management systems, enforcing continuous feedback mechanisms such as CAPA (Corrective and Preventive Actions) frameworks. These ensure medical devices and clinical processes maintain high performance and swiftly adapt to new risks or improvement opportunities.
- Integration of sensor-based monitoring within implants for precision tracking.
- Adoption of AI-driven analytics for predictive risk management.
- Expansion of patient-centered outcome data collection to guide innovation.
- Strengthened collaboration between regulatory bodies for global harmonization.
- Enhanced training programs to disseminate evolving standard practices.
| Emerging Quality Practice | Potential Clinical Benefit | Technological Enabler |
|---|---|---|
| Digital Quality Management Systems | Real-time oversight and error reduction | Cloud computing and IoT sensors |
| Patient-Reported Outcomes Integration | Improved personalization of care | Mobile health apps and telemedicine |
| AI-Powered Risk Assessment Tools | Anticipation and mitigation of complications | Machine learning algorithms |
Quiz : Qualité et certification des dispositifs médicaux

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…
Collaborative Expertise and Patient-Centric Coordination: Foundations of Quality in Spinal Care
Expertise from multidisciplinary teams spearheads the translation of quality certification into tangible clinical benefits. In spinal surgery, the synergy of surgical knowledge, device engineering, and patient coordination creates a dynamic platform for continual advancement.
Consultants and clinical leaders play instrumental roles in selecting appropriate implants, designing individualized surgical plans, and overseeing postoperative regimens. Their collaboration with logistics partners ensures patients receive seamless communication, scheduling, and support throughout their care journey, especially for international patients navigating cross-border procedures.
Emphasizing patient-centric models enhances engagement and compliance, key factors that amplify the success of quality certification programs. This holistic approach aligns with global healthcare standards advocating transparency and participative care, ultimately reinforcing the trust patients place in certified devices and centers.
- Joint decision-making involving surgical teams, engineers, and patients.
- Integration of advanced training programs to upscale clinical skills on certified devices.
- Customized patient education to reinforce compliance and safety.
- Continuous feedback loops between all stakeholders enhancing care coordination.
- Establishing international networks supporting cross-border medical travel.
| Element | Role in Quality Enhancement | Impact on Clinical Outcomes |
|---|---|---|
| Consultant Expertise | Determines best device and surgical approach | Optimizes patient-specific outcomes |
| Multidisciplinary Coordination | Ensures smooth perioperative management | Reduces complication rates and improves satisfaction |
| Patient Engagement | Empowers informed consent and adherence | Supports long-term functional independence |
What are the main benefits of certified medical devices in spinal surgery?
Certified devices ensure compliance with international standards, enhanced safety, validated therapeutic efficacy, and improved traceability enabling rigorous implant management.
How does certification of French healthcare institutions improve patient safety?
Certification mandates regular practice audits, optimal coordination of teams and processes, and active patient involvement, significantly reducing errors and complications.
Are there specific implants designed to maintain spinal mobility?
Yes, implants like TOPS, Intraspine, and B-DYN are engineered to stabilize while conserving segmental mobility, preventing common adverse effects of traditional spinal fusion.
How is postoperative follow-up organized for Canadian patients after surgery in France?
Postoperative follow-up is primarily managed by Neurothérapie Montréal, which provides personalized rehabilitation and maintains direct connections with French medical teams to ensure continuous care.
Who coordinates the surgical journey and surgeon selection in France?
The company Franchir oversees the entire patient pathway including orientation, logistics, accommodation, and administrative support, facilitating a smooth and secure surgical experience.

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…