
What Research Reveals About Cousin Spine Technology and the Franchir Procedure
November 5, 2025
A Comprehensive Guide to Initial Assessments and Questionnaires
November 6, 2025Amidst a global surge in chronic spinal conditions, neurovertebral decompression emerges as a beacon of hope for millions grappling with debilitating back pain. This innovative, non-invasive treatment, leveraging precision-controlled mechanical traction, promises to alleviate pressure on intervertebral discs and restore mobility without the risks of surgery. As healthcare systems worldwide face challenges of aging populations and rising incidence of spinal ailments, the international adoption and adaptation of neurovertebral decompression reveal remarkable disparities, successes, and collaborative potentials. By investigating the treatment’s diffusion across countries, the technological advancements driving its effectiveness, and the patient-centric approaches shaping its protocols, a comprehensive understanding surfaces on how this therapy reshapes spinal care paradigms globally.
Data from recent international studies reveal significant variations in access and outcomes associated with neurovertebral decompression, influenced heavily by healthcare infrastructure, practitioner expertise, and cultural attitudes toward spinal therapies. Particularly compelling is the cooperative dynamic between Canada and France, where integrated care pathways and shared innovations set benchmarks for patient management. The interplay among major medical device manufacturers—including Medtronic, NuVasive, and DePuy Synthes—further advances technological frontiers, embedding sophisticated imaging and robotic assistance into decompression protocols. This article delves deeply into these global perspectives, elucidating the multifaceted impact of neurovertebral decompression in 2025 across diverse healthcare landscapes.
Innovations in Neurovertebral Decompression: Transforming Spinal Care Worldwide
Neurovertebral decompression has revolutionized the management of chronic disc-related spinal pain by introducing a tailored, mechanical traction methodology that precisely targets nerve root compression. This treatment harnesses computer-assisted protocols to modulate the degree and timing of vertebral distraction, significantly reducing disc pressure and fostering tissue regeneration. The precision of these interventions ensures maximal therapeutic gain while preserving patient comfort and safety.
Among the core technological drivers are devices developed by industry leaders such as Medtronic, NuVasive, and DePuy Synthes. These companies have integrated feedback systems that monitor biomechanical responses in real-time, enabling dynamic adjustments and individualized care. The advantages include:
- Targeted pressure relief: precisely calibrated traction reduces inflammation and nerve root compression
- Enhanced tissue healing: improved local circulation promotes disc hydration and repair
- Non-invasiveness: offering a safer alternative to surgical interventions, minimizing patient risk and recovery time
- Adaptability: protocols are customizable based on patient-specific anatomical and symptomatic data
Clinical evidence supports these benefits robustly: over 70% of patients undergoing neurovertebral decompression report considerable pain reduction and increased spinal function post-treatment. For instance, a comprehensive analysis from international databases highlights that conservative decompression therapy, when integrated into multidisciplinary care, improves outcomes significantly compared to standard physical therapy alone.
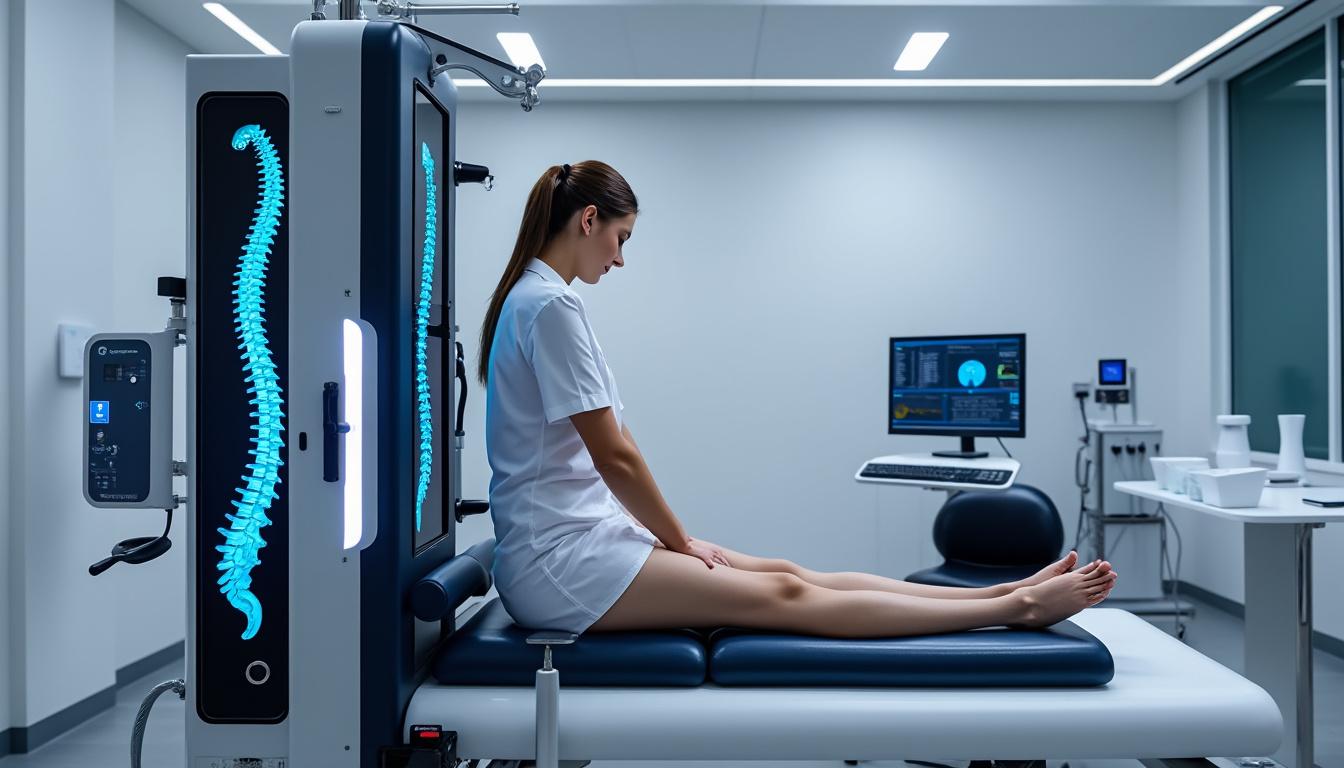
Globally, the impact of such innovations aligns with demographic trends toward aging populations susceptible to degenerative disc disease and vertebral fractures. As detailed in recent literature on spinal cord injuries and vertebral fractures, implementing dynamic decompression systems correlates with lower incidence of progression to invasive surgery, ensuring sustainable healthcare delivery.
| Innovative Features | Clinical Benefit | Technology Provider |
|---|---|---|
| Computer-assisted traction adjustment | Personalized tension control to maximize decompression | Medtronic |
| Real-time biomechanical feedback | Optimized treatment interaction and safety | NuVasive |
| Dynamic vertebral motion preservation | Reduced adjacent segment degeneration | DePuy Synthes |
| Minimally invasive robotic guidance | Precision in treatment delivery | Orthofix |

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Biomechanical Mechanisms Underlying Neurovertebral Decompression Effectiveness
Understanding the biomechanical principles fundamental to neurovertebral decompression is crucial for optimizing its clinical application. The premise centers on the controlled enlargement of intervertebral spaces through gradual axial traction, which alleviates disc pressure and mitigates nerve root impingement. Advanced imaging modalities such as MRI and dynamic radiography are routinely employed to accurately assess spinal segment status and tailor intervention protocols.
The method activates several physiological responses critical to recovery:
- Disc space rehydration: Reduced compression enables water molecules to re-enter the nucleus pulposus, improving cushioning capacity
- Enhanced microcirculation: Traction facilitates blood flow around spinal structures, accelerating nutrient delivery and waste removal
- Inflammation modulation: Mechanical decompression reduces proinflammatory cytokine accumulation, lowering local edema and pain sensation
- Neurological decompression: Decreased mechanical stress on nerve roots improves nerve conductivity and function
Not all decompression systems utilize the same traction dynamics; assisted decompression relies on mechanical devices controlling patient positioning and force application, whereas active decompression integrates patient muscle engagement. Comparative biomechanical analyses reveal that:
| Decompression Type | Biomechanical Mechanism | Clinical Impact |
|---|---|---|
| Assisted Decompression | Precise, consistent traction force applied externally without patient effort | Greater control over disc unloading, ideal for severe cases |
| Active Decompression | Muscle engagement with traction promotes spinal stability and strengthening | Improved muscular support reduces recurrence risk |
Integrating these biomechanical insights into patient assessment and device calibration enhances therapeutic precision. Recent international conferences emphasize training clinicians in both approaches, ensuring judicious application dependent on patient capacity and clinical context.

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
International Collaborative Models: Canada-France Partnership Optimizing Neurovertebral Therapy
Amid escalating wait times and healthcare funding challenges in Canada, innovative international collaborations have emerged to bridge treatment gaps for spinal pathologies. The Canada-France partnership exemplifies a coordinated model offering comprehensive neurovertebral decompression and surgical options through an integrated, cross-border patient journey.
Key components of this collaboration include:
- Pre-treatment evaluation: Canadian specialists conduct thorough diagnostic and conservative treatment phases including neurovertebral decompression at clinics such as TAGMED.
- Organizational logistics: Agencies like Franchir coordinate travel, accommodation, and scheduling for medical interventions in France.
- Advanced surgical interventions: French hospitals provide access to cutting-edge procedures utilizing implants from Zimmer Biomet, Stryker, and Boston Scientific.
- Post-operative care: Follow-up and rehabilitation services in Montreal facilitated by Neurothérapie Montréal ensure continuity and localized support.
This framework optimizes resource utilization across health systems, provides timely access to high-caliber interventions, and fosters a research feedback loop improving practices on both sides. Patient testimonials underscore improved recovery timelines, reduced pain, and enhanced quality of life.
| Stage | Tasks | Stakeholders |
|---|---|---|
| Initial assessment | Comprehensive examination and conservative treatment initiation | Canadian clinicians at TAGMED |
| Cross-border transfer | Travel and medical scheduling | Franchir agency |
| Surgery | Spinal decompression and implant insertion | French medical teams utilizing Zimmer Biomet implants |
| Rehabilitation | Post-surgical recovery and therapy | Neurothérapie Montréal |
The success of this international approach inspires other transnational health partnerships aiming to extend specialized spinal care to underserved regions worldwide.


International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
Dynamic Implants in Spinal Surgery: Advancing Post-Decompression Mobility
Recent surgical innovations have shifted focus from rigid arthrodesis toward dynamic spinal implants that preserve physiological mobility post-intervention. Devices such as TOPS (Total Posterior Solution) and IntraSPINE prostheses exemplify this trend, offering patients enhanced functional outcomes and reduced adjacent segment degeneration compared to traditional fusion techniques.
Advantages of dynamic implants include:
- Maintenance of segmental motion: enabling natural spinal flexibility
- Decreased biomechanical stress: protecting adjacent vertebrae from accelerated degeneration
- Improved postoperative quality of life: facilitating faster return to daily activities
- Compatibility with minimally invasive techniques: reducing surgical morbidity
A detailed comparison highlights the biomechanical and clinical distinctions:
| Implant Type | Post-Op Mobility | Risk of Adjacent Degeneration | Quality of Life Impact |
|---|---|---|---|
| Rigid Fusion | Absent at treated levels | Increased due to altered biomechanics | Restricted movement; potential discomfort |
| Dynamic Implant (e.g., TOPS) | Preserved | Reduced | Enhanced mobility and comfort |
The integration of these devices, provided by manufacturers like Zimmer Biomet and NuVasive, represents a pivotal evolution. Patients benefit from less invasive treatments paired with biomechanical preservation strategies that promote long-term spinal health.

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…
Prioritizing Conservative Treatments: Neurovertebral Decompression as a Cornerstone before Surgery
Before resorting to surgical options, expert consensus underscores the importance of at least three to six months of rigorous conservative management for chronic spinal disorders. Neurovertebral decompression, supported by evidence-based protocols supervised by leading spine specialists, constitutes a central component of this therapeutic phase.
Benefits of conservative neurovertebral decompression include:
- Symptomatic relief: significant reduction of pain and inflammation
- Improved functional capacity: restoration of spinal flexibility and strength
- Reduction of surgical necessity: many patients avoid or delay invasive procedures
- Holistic care approach: integration with osteopathic and naturopathic interventions enhances overall patient well-being
Complementary therapies such as osteopathy focus on correcting muscular imbalances, while naturopathy supports recovery through biological regulation, illustrating the multifaceted nature of pre-surgical care. An effective conservative program is tailored to each patient’s condition and response, ensuring optimal outcomes.
| Therapeutic Modality | Objectives | Expected Outcomes |
|---|---|---|
| Neurovertebral decompression | Relieve disc pressure and nerve compression | Pain reduction, improved mobility |
| Osteopathy | Restore spinal alignment and muscle balance | Improved posture and reduced tension |
| Naturopathy | Enhance systemic recovery and immunity | Optimized healing and stress management |
These integrated strategies led by experts such as those at TAGMED Clinic emphasize cautious progression toward invasive intervention only when necessary.
Global Epidemiological Trends Shaping Demand for Neurovertebral Decompression
Worldwide epidemiological data underscore an upward trajectory in vertebral and spinal disorders, driven largely by demographic aging, sedentary lifestyles, and trauma-related spinal injuries. Comprehensive analyses across 204 countries reveal growing prevalence of vertebral fractures and degenerative conditions requiring innovative treatments like neurovertebral decompression.
Key epidemiological drivers include:
- Population aging: increased incidence of disc degeneration and fractures in older adults
- Urbanization and sedentism: higher risks of spinal strain and injury from prolonged immobility
- Traumatic events: falls and accidents remain leading causes of vertebral fractures globally
- Healthcare accessibility: disparities in treatment availability influence disease burden outcomes
Regional variations map primary challenges: while high-income countries benefit from advanced decompression therapies, low- and middle-income regions face barriers leading to elevated disability rates. The dissemination of knowledge through global spine care networks and educational initiatives—such as those by EuroSpine—aims to bridge gaps.
| Region | Prevalence of Spinal Disorders (%) | Access to Neurovertebral Decompression | Challenges |
|---|---|---|---|
| North America | 18 | Widespread | Cost, wait times |
| Europe | 16 | Comprehensive | Resource variability |
| Asia | 20 | Emerging | Awareness, infrastructure |
| Africa | 22 | Limited | Access, training |
Understanding these dynamics is crucial for policy formulation and resource allocation aimed at expanding effective spinal care modalities globally.
Technological Synergy: The Role of Robotics and Digital Innovations in Neurovertebral Decompression
The integration of robotics, 3D imaging, and artificial intelligence is enhancing neurovertebral decompression treatment precision and personalization. Robotic platforms developed by companies such as Stryker and Globus Medical provide unparalleled navigation capabilities, facilitating minimally invasive procedures and allowing fine-tuned mechanized traction.
Key technological advantages include:
- Enhanced imaging: 3D visualizations aid in precise targeting of decompression zones
- Real-time adjustment: AI algorithms adapt traction forces during sessions based on patient feedback and sensor data
- Improved safety: robotic assistance reduces human error and monitors patient status continuously
- Data-driven outcomes: analytics enable continuous protocol optimization across diverse populations
Collaborations between device innovators and clinical centers, including eCential Robotics, have propelled these advancements, setting new standards for global spinal care. The future suggests a seamless fusion of digital and mechanical therapies, augmented by telemedicine and remote monitoring facilitating decentralized patient management.
| Technology | Functionality | Clinical Benefit | Provider |
|---|---|---|---|
| Robotic Navigation | Precise instrument guidance during decompression | Reduced complications, improved efficacy | Stryker |
| 3D Imaging | Detailed anatomical visualization | Enhanced treatment accuracy | Globus Medical |
| AI-Driven Traction Control | Adaptive feedback integration | Optimized patient comfort and therapeutic outcomes | SpineWave |
| Telemedicine Integration | Remote patient monitoring and consultation | Continuous care and adherence support | Alphatec Spine |
Key Features and Benefits of Neurovertebral Decompression Technologies
Use the dropdown to select column, and input to filter the table.
| Technology ▲▼ | Primary Function ▲▼ | Clinical Advantage ▲▼ | Common Providers ▲▼ |
|---|
What types of spinal conditions benefit most from neurovertebral decompression?
Neurovertebral decompression is particularly effective for herniated discs, degenerative disc disease, and nerve root compression syndromes. Patients with mild to moderate symptoms often experience significant pain relief and functional improvement.
How does the Canada-France medical collaboration improve patient outcomes?
This partnership integrates pre-operative, operative, and post-operative care between Canadian and French medical teams, ensuring timely access to advanced surgical technologies and comprehensive rehabilitation that enhances recovery and quality of life.
Are dynamic spinal implants suitable for all surgical patients?
While dynamic implants offer mobility preservation benefits, their suitability depends on individual patient anatomy, severity of spinal degeneration, and surgeon evaluation. Not all patients qualify, but where applicable, they improve long-term outcomes.
Can conservative neurovertebral decompression replace spinal surgery?
In many cases, neurovertebral decompression as a conservative treatment can alleviate symptoms enough to delay or avoid surgery. However, severe or progressive neurological deficits may still require surgical intervention.
What role do robotics and AI play in enhancing neurovertebral decompression?
Robotics and AI technologies improve precision, optimize traction parameters in real-time, reduce adverse events, and offer personalized care plans, ultimately enhancing efficacy and patient safety during decompression treatments.




