Low back pain (LBP) remains a prevalent and multifactorial health challenge affecting millions globally. It encompasses a range of diagnoses, from mechanical issues like herniated discs to chronic muscular disorders, often impeding daily functioning and quality of life. As the demand for effective, evidence-based interventions grows, the intersection of advanced therapies and personalized care has never been more crucial. In clinical settings, expertise like that of Dr. Sylvain Desforges integrates rigorous diagnosis and cutting-edge non-surgical options, heralding a new frontier in spinal health management. Patients today seek not only relief but also clear guidance, tailored support, and innovative strategies that are backed by science and delivered with empathy.
The evolution of low back pain treatment emphasizes multidisciplinary approaches that blend medication, physical therapy, behavioral interventions, and technological innovation. Understanding pain’s origin, assessing functional impairment, and selecting appropriate interventions demand both experience and patient-centered communication. This comprehensive article explores the myriad options available in 2025 for managing low back pain, highlighting evidence-based practices such as duloxetine usage, acceptance and commitment therapy (ACT), classification-based exercise, and self-management approaches. Moreover, it delves into newer modalities like spinal decompression, minimally invasive procedures, and assistive devices, shedding light on their roles in optimizing patient outcomes.
Comprehensive Clinical Evaluation: The Foundation of Effective Low Back Pain Management
Effective management of low back pain begins with a thorough and nuanced clinical evaluation. Dr. Sylvain Desforges, leveraging over 30 years of osteopathic expertise, implements meticulous assessment protocols that aim to discern the precise causes of a patient’s pain while ruling out critical conditions.
A detailed clinical examination includes observation of posture, gait, and spinal alignment, coupled with functional tests assessing the patient’s ability to sit, stand, walk, and perform leg lifts. Additionally, patients are encouraged to self-report pain intensity using standardized scales such as the 0 to 10 numeric rating scale, alongside descriptions of how pain influences their everyday activities and emotional well-being.
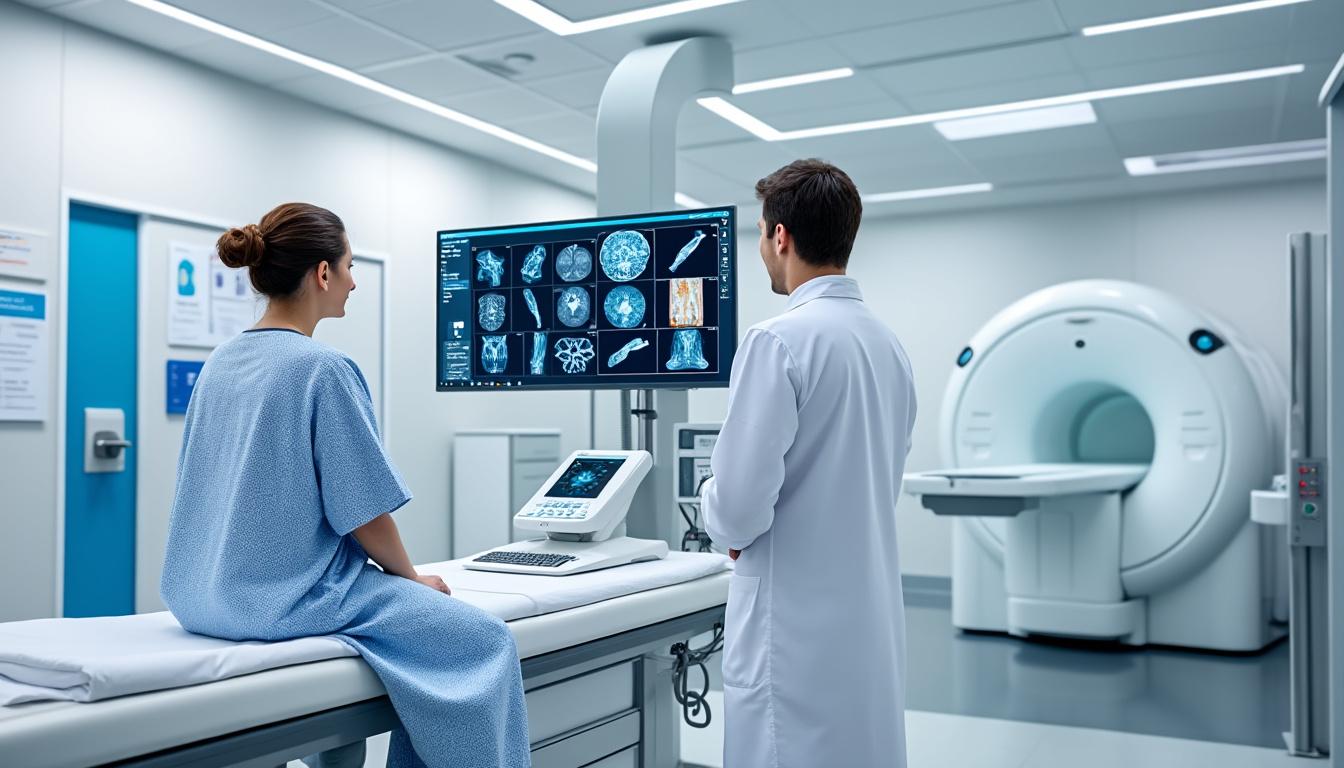
In certain cases, supplementary diagnostics are indispensable to pinpoint sources such as herniated discs or nerve impingement:
- X-rays highlight bony abnormalities, including arthritis or fractures, though they do not visualize soft tissues effectively.
- Magnetic Resonance Imaging (MRI) and CT scans visualize spinal discs, muscles, ligaments, and nerves, essential for identifying herniations or spinal stenosis.
- Blood tests can reveal infections or systemic conditions that might manifest with back pain symptoms.
- Electromyography (EMG) helps evaluate nerve function and muscular responsiveness, confirming nerve compression or dysfunction.
Besides identifying structural abnormalities, the evaluation process by experts like Dr. Desforges emphasizes functional and biopsychosocial factors influencing pain perception and coping mechanisms. This comprehensive approach aligns with modern precision medicine goals, ensuring each patient’s treatment plan is individualized rather than generic.
| Assessment Component | Purpose | Example/Use |
|---|---|---|
| Physical Exam | Evaluate mobility, posture, pain provocation | Assessment of sit-to-stand transitions, leg raise tests |
| Pain Scale Rating | Quantify pain intensity | Numeric Rating Scale 0-10 |
| Imaging (MRI, CT, X-ray) | Visualize bone and soft tissue pathology | Detect disc herniation, spinal stenosis |
| EMG | Evaluate nerve function | Confirm radiculopathy diagnosis |
| Blood tests | Rule out infection or systemic disease | Screen for inflammatory markers |
Patient Engagement and the Role of History
Understanding individual patient history, including previous injuries, lifestyle, and emotional stressors, is integral. A detailed symptom chronology and impact review help clinicians define not only the pathology but the patient’s expectations and readiness for treatment. Dr. Desforges emphasizes clear, compassionate communication throughout this phase, empowering patients to participate actively in their care journey.
Evidence-Based Medications in Low Back Pain: Duloxetine and Beyond
Pharmacological interventions for low back pain constitute a vital component of treatment regimens, especially for moderate to severe symptoms or cases unresponsive to conservative measures. Evidence increasingly supports selective medications that both alleviate pain and address underlying neurochemical imbalances.
Duloxetine, a serotonin-norepinephrine reuptake inhibitor (SNRI), stands out with high-level evidence of efficacy in chronic low back pain. Unlike standard analgesics, duloxetine targets central pain pathways and has a moderate effect in reducing pain intensity as demonstrated through randomized controlled trials. Its use is particularly relevant for patients with chronic symptoms and comorbid depressive tendencies.
- NSAIDs such as ibuprofen (Advil) or naproxen (Aleve) remain first-line agents for acute flare-ups, mitigating inflammation and reducing musculoskeletal pain.
- Muscle relaxants may be considered for short durations to ease muscle spasms but require cautious administration due to sedation risks.
- Topical analgesics like Biofreeze and patches combining menthol or capsaicin offer localized pain relief without systemic side effects.
- Opioids are seldom recommended except for carefully selected, short-term use under strict supervision due to addiction potential.
In conjunction with Dr. Desforges’ rigorous evaluations, medication choices are tailored, factoring in patient-specific contraindications and treatment goals.
| Medication Type | Typical Use | Strength of Evidence | Considerations |
|---|---|---|---|
| Duloxetine (SNRI) | Chronic low back pain with neuropathic features | High | Monitor for mood changes and side effects |
| NSAIDs (Advil, Aleve, Voltaren) | Acute inflammation and pain relief | Moderate | GI and cardiovascular risks with long-term use |
| Muscle Relaxants | Muscle spasm relief | Low to moderate | Caution with sedation and dizziness |
| Topical Agents (Biofreeze, Salonpas, Tiger Balm, Icy Hot) | Localized pain | Low to moderate | Minimal systemic absorption |
| Opioids | Severe acute pain, short-term | Low | Risk of dependence |
Integrating Medication with Non-Pharmacological Therapies
Dr. Desforges advocates a holistic approach where medication use complements physical and behavioral therapies. This strategy aims to optimize functional restoration while minimizing long-term medication dependency.
Classification-Based Exercise and Manual Therapy: Personalized Movement Solutions
Exercise remains the cornerstone of chronic low back pain management. However, research consistently indicates that generic exercise programs offer only moderate benefits. Personalized, classification-based exercise regimens, which tailor therapies based on an individual’s physical presentation and psychological factors, significantly enhance outcomes.
The approach adopted in clinics such as Clinique TAGMED combines motor control exercises with manual therapies practiced by skilled osteopaths. Such interventions help restore spinal stability, relieve nerve impingement, and improve muscular endurance. The evidence supports large treatment effects in pain reduction and functional improvement with this strategy.
- Motor control exercises focus on retraining deep core muscles to enhance spinal support.
- Directional preference exercises tailor movement patterns to patient-specific pain relief positions, like extension or flexion.
- Manual therapy interventions include gentle spinal mobilizations and soft tissue techniques to reduce stiffness and improve mobility.
- Incorporation of cognitive-behavioral elements during therapy sessions supports patient engagement and coping skills.
Clinical experience confirms that this integrated movement therapy and manual approach often reduces the need for more invasive procedures.
| Exercise/Manual Therapy Component | Purpose | Expected Benefit |
|---|---|---|
| Motor Control Exercises | Improve deep core muscle activation | Spinal stability and pain reduction |
| Directional Preference Exercises | Identify and use pain-relieving movements | Symptom modulation |
| Manual Therapy (Osteopathic Techniques) | Restore joint mobility and reduce soft tissue tension | Enhanced flexibility and function |
| Cognitive-Behavioral Elements | Address pain perception and adherence | Improved treatment engagement |
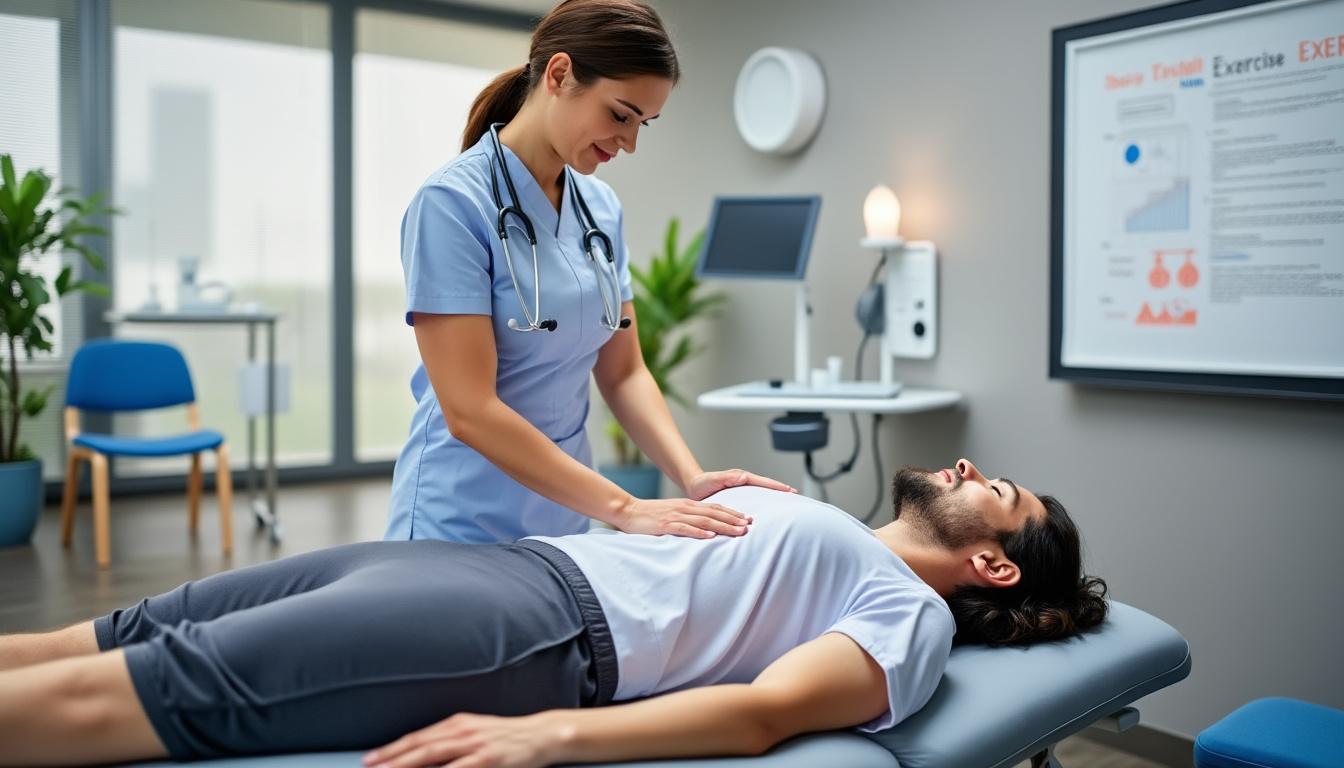
Benefits of Classification-Based Exercise in Clinical Practice
Classification not only guides therapy but promotes patient self-awareness regarding pain triggers and preferred movement patterns. Dr. Desforges highlights that precise tailoring reduces treatment duration and enhances compliance, a key factor in sustained recovery.
Behavioral and Psychological Therapies: Acceptance and Commitment Therapy for Chronic Low Back Pain
Chronic pain is intertwined with psychological and social variables that traditional physical treatments alone cannot address. Acceptance and Commitment Therapy (ACT) has emerged as a high-evidence behavioral intervention aimed at fostering patient acceptance of pain and increasing psychological flexibility.
ACT encourages patients to engage in meaningful activities despite pain, rather than concentrating solely on symptom elimination. This approach has been shown to yield moderate improvements in pain-related disability and quality of life. It may especially benefit older adults or patients with lower educational levels, who sometimes derive less benefit from cognitive behavioral therapy (CBT).
- Teaches mindfulness and present-moment awareness techniques.
- Helps patients commit to behavior aligned with personal values despite pain.
- Provides tools to reduce pain catastrophizing and emotional distress.
- Delivers psychological support either in-person or via digital platforms for accessibility.
Integrating ACT into multidisciplinary care allows patients to perceive pain as a part of their experience without it dominating their lives, leading to better functional outcomes.
| ACT Component | Goal | Clinical Outcome |
|---|---|---|
| Mindfulness Practice | Increase nonjudgmental awareness of pain | Reduced emotional reactivity |
| Values-Based Action | Align behavior with personal goals | Improved life satisfaction |
| Cognitive Defusion | Reduce attachment to pain-related thoughts | Decreased pain catastrophizing |
| Acceptance Techniques | Foster willingness to experience pain | Enhanced coping strategies |
Digital Delivery and Patient Empowerment
With the growing adoption of telemedicine, ACT can be delivered effectively through self-guided digital platforms that complement in-person sessions. This accessibility aligns with Dr. Desforges’ approach of making care understandable and accessible, encouraging patients to take an active role in their therapy journey.
Empowering Self-Management: Education and Tools to Sustain Recovery from Low Back Pain
Self-management education is essential in chronic low back pain care, teaching patients how to independently apply strategies that control symptoms and optimize function. Programs often include a combination of pain neuroscience education, lifestyle modifications, and practical techniques.
Among the best-supported methods for self-management are structured educational initiatives emphasizing:
- Understanding pain mechanisms to reduce fear and catastrophizing.
- Incorporating graded activity and pacing techniques to avoid overexertion.
- Use of appropriate over-the-counter treatments such as NSAIDs (e.g., Aleve, Voltaren), topical agents like Salonpas patches, or devices like the TENS 7000 unit for safe analgesic effects.
- Strategies for posture, ergonomics, and prevention of recurrent injury.
Digital self-management platforms have demonstrated comparable effectiveness to therapist-guided programs, offering scalable, cost-effective access. Dr. Desforges prioritizes patient education delivered in clear, jargon-free language, respecting each patient’s unique context and goals.
| Self-Management Component | Purpose | Examples/Tools |
|---|---|---|
| Pain Neuroscience Education | Reduce fear and promote understanding | Interactive digital modules, counseling sessions |
| Activity Pacing | Balance activity and rest | Personalized activity logs |
| OTC Medications and Topicals | Manage pain with minimal side effects | Voltaren gel, Biofreeze cream, Salonpas patches |
| Electrical Stimulators | Provide non-pharmacological pain relief | TENS 7000, Theragun percussive therapy |
| Postural and Ergonomic Advice | Prevent injury recurrence | Workstation adjustments, back-support braces |
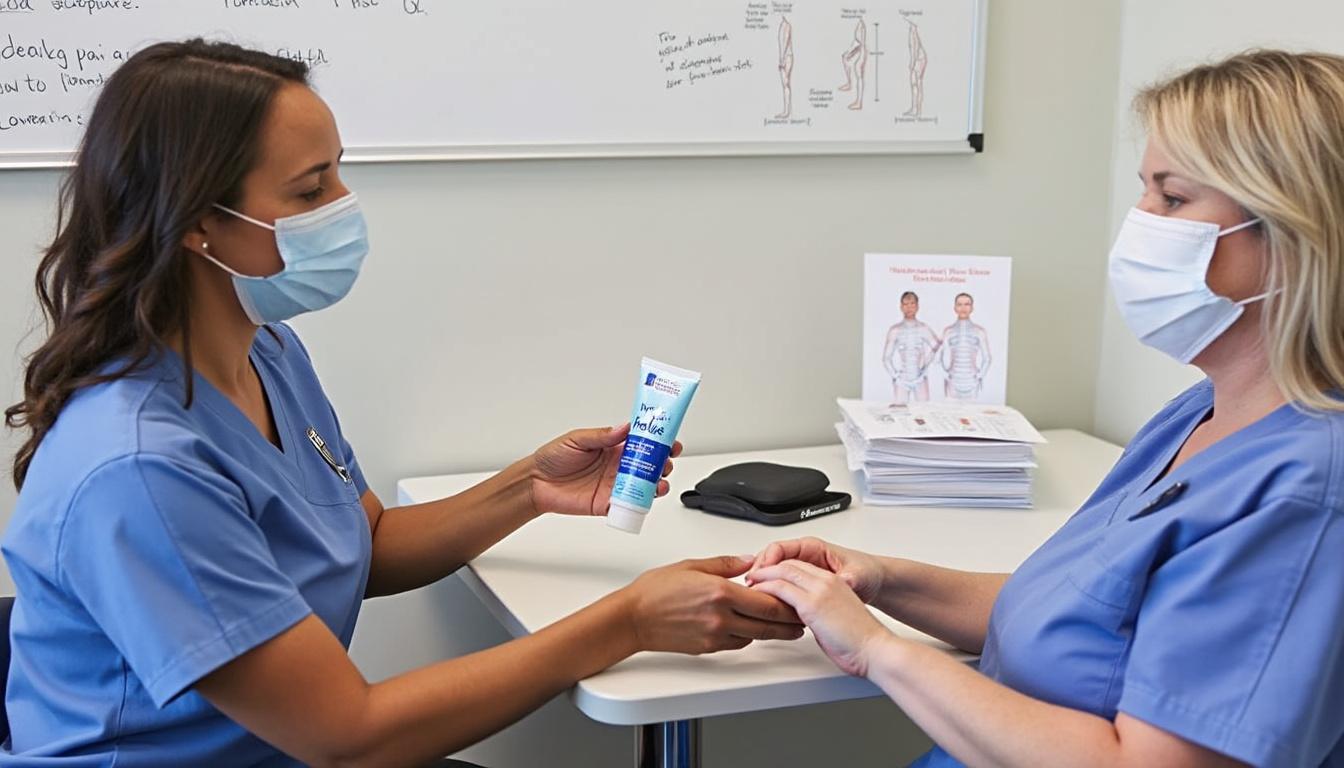
Benefits of Integrating Self-Management Early
Early promotion of self-care builds patient confidence and reduces dependency on clinical visits or medications. This proactive model supports sustainable long-term health and aligns with modern outpatient strategies prioritized by experts such as Dr. Desforges.
Non-Surgical Spinal Decompression: A Scientific Alternative for Chronic Low Back Pain Relief
Non-surgical spinal decompression therapy represents a cutting-edge, evidence-based treatment offering sustained relief from herniated discs and chronic mechanical back pain. This treatment involves mechanical traction under controlled parameters designed to gently stretch the spine, reduce pressure on discs and nerves, and promote disc healing.
Multiple studies, including a prospective randomized controlled study, have demonstrated significant pain reduction and functional improvement with spinal decompression. Dr. Sylvain Desforges incorporates this modality at Clinique TAGMED as part of comprehensive personalized treatment plans that avoid surgery whenever possible.
- Gently relieves nerve pressure through negative intradiscal pressure.
- Enhances nutrient and oxygen exchange within spinal discs.
- Non-invasive, painless sessions typically last 20-30 minutes.
- Can be combined with manual therapy for synergistic effects.
| Feature | Benefit | Clinical Evidence |
|---|---|---|
| Targeted mechanical traction | Disc decompression and pressure relief | Significant reduction in pain scores |
| Repeated treatment sessions | Promotes disc repair and symptom reduction | Improved mobility and function |
| Non-invasive method | Reduced risk compared to surgery | Minimal adverse effects reported |
Patient Selection and Treatment Protocols
Appropriate patient selection following expert evaluation is essential. Patients with herniated discs, nerve root irritation, or chronic discogenic pain derive the most benefit, while those with advanced degenerative changes or instability may require alternative approaches. Treatment plans are tailored in frequency and intensity, ensuring comfort and maximal benefit.
Minimally Invasive Procedures: Innovations in Advanced Low Back Pain Relief
When conservative measures do not fully alleviate symptoms, minimally invasive procedures serve as valuable adjuncts or alternatives to surgery. Among these, techniques like epidural steroid injections, radiofrequency ablation, and basivertebral nerve ablation have gained clinical traction.
Dr. Desforges’ commitment to scientific rigour and patient safety aligns with the adoption of these advanced modalities only when clearly indicated. For example, Intraspine’s minimally invasive therapies allow targeted pain relief with rapid patient recovery times.
- Epidural steroid injections: Reduce local inflammation around irritated nerve roots, offering intermediate-term symptom control.
- Radiofrequency ablation: Uses electromagnetic waves to selectively disrupt nerves transmitting pain, providing lasting relief in some cases.
- Basivertebral nerve ablation: Targets nerves innervating vertebral endplates and is especially useful for patients with Modic type changes on MRI.
| Procedure | Indication | Effect Duration | Considerations |
|---|---|---|---|
| Epidural Steroid Injection | Radicular pain | 1-3 months | May require multiple injections |
| Radiofrequency Ablation | Facet joint pain | 6-12 months | Selective nerve targeting |
| Basivertebral Nerve Ablation | Chronic Modic type 1 or 2 changes | Up to 5 years | Minimally invasive, requires specialized imaging |
Ensuring Safety and Ethics in Interventional Care
For over three decades, Dr. Desforges upholds principles of medical ethics and stringent adherence to Québec and Canadian regulations, including those from the Collège des médecins du Québec. All interventional treatments prioritize comprehensive patient evaluation and informed consent, reinforcing that no single procedure suits all and that conservative care remains foundational.
Future Perspectives: Assistive Technologies and Dynamic Spinal Implants in Low Back Pain Care
Innovations in wearable devices and spinal implants are reshaping possibilities in low back pain management. Passive spinal exoskeletons, such as those studied for industrial workers with back strain, reduce biomechanical loads by 10-40%, potentially mitigating pain and preventing injury exacerbation.
Dynamic spinal implants focus on preserving motion and stability, offering future alternatives to traditional rigid fusion surgeries, although evidence is still evolving. Experts like Dr. Desforges continue to monitor these modalities’ efficacy and integrate them into personalized treatment plans when appropriate.
- Spinal exosuits enhance trunk support and encourage ergonomic postures.
- Implants aim to reduce adjacent segment disease by allowing natural spinal movement.
- Technological advances include integration with real-time biofeedback systems for patient monitoring.
- These emerging treatments complement holistic, non-invasive strategies rather than replace them.
| Technology | Function | Clinical Benefits | Development Status |
|---|---|---|---|
| Passive Spinal Exoskeletons | Reduce musculoskeletal strain | Improved comfort, reduced pain | Prototype and pilot stage |
| Dynamic Spinal Implants | Preserve spinal motion post-surgery | Potential decrease in adjacent segment degeneration | Clinical trials ongoing |
| Real-Time Biofeedback Devices | Monitor posture and movement | Enhanced patient adherence and rehabilitation | Early commercialization |
Tailoring Innovation to Individual Needs
The future of spinal care lies in blending emerging technologies with personalized assessment to address the complex nature of low back pain. Leadership in the field, as modeled by Dr. Desforges, ensures innovations serve patient well-being and uphold the highest standards of care.
Non-Pharmacological Adjuncts: TENS, Percussive Therapy, and Topicals Enhancing Pain Control
Alongside core therapies, adjunct treatments such as transcutaneous electrical nerve stimulation (TENS), percussive therapy devices like Theragun, and topical analgesics contribute to holistic low back pain management. Devices such as the TENS 7000 unit help disrupt pain signaling through safe electrical stimulation, offering well-documented relief with minimal side effects.
Percussive therapy instruments deliver deep muscle vibrations, promoting circulation and reducing muscle stiffness. Meanwhile, topical products such as Tiger Balm, Salonpas, and Icy Hot provide localized chemical stimulation that soothes nerve endings and decreases pain perception.
- TENS 7000: Portable units emitting electrical impulses that reduce neuropathic and musculoskeletal pain.
- Theragun: Percussive massage device that enhances muscle recovery and reduces tension.
- Topical analgesics: Products like Voltaren gel and Biofreeze offer alternative or complementary pain control.
- Safe for continued use alongside other treatment modalities, making them excellent components in multimodal pain management.
| Adjunct Treatment | Mechanism | Clinical Utility |
|---|---|---|
| TENS 7000 | Electrical nerve stimulation | Neuropathic and musculoskeletal pain relief |
| Theragun | Percussive muscle stimulation | Reduced muscle stiffness |
| Voltaren, Biofreeze, Tiger Balm | Topical analgesia | Localized pain reduction |
Complementing Therapy for Improved Outcomes
Integrating these non-pharmaceutical adjuncts with therapies such as manual interventions and digital self-management enhances patients’ control and comfort, making them vital components of modern low back pain treatment protocols.
Strategies for Low Back Pain Prevention: Lifestyle and Ergonomic Considerations
Preventive strategies form the cornerstone of long-term low back health. Patients benefit greatly when clinicians like Dr. Desforges provide tailored guidance on lifestyle and ergonomic factors that mitigate risk and delay symptom progression.
Considerations include:
- Exercise: Regular general physical activity, focusing on core strengthening and flexibility.
- Ergonomics: Optimizing workplace and home environments with supportive seating and lumbar supports.
- Weight management: Reducing load on lumbar structures through healthy diet and physical activity.
- Proper lifting techniques: Educating on body mechanics to prevent acute injury.
- Stress management: Incorporating mindfulness and relaxation practices to prevent pain exacerbation.
| Prevention Strategy | Rationale | Implementation Examples |
|---|---|---|
| Physical Activity | Maintains muscle strength and flexibility | Walking, swimming, yoga |
| Ergonomics | Reduces mechanical stress | Adjustable chairs, lumbar cushions |
| Healthy Weight | Minimizes spinal load | Balanced diet, calorie control |
| Lifting Techniques | Prevents acute injury | Bend knees, keep back straight |
| Stress Management | Reduces pain exacerbation | Meditation, ACT |
Early education on prevention fosters self-efficacy and decreases likelihood of chronic disability. To learn more about prevention strategies and comprehensive management of low back pain, patients are encouraged to consult with clinics such as TAGMED for personalized recommendations.
Creating a Sustainable Health Plan
Aside from physical factors, behavioral components are emphasized, highlighting the importance of a balanced, informed approach to back care that privileges longevity and quality of life.
Explore diagnosis and management details further to equip yourself with comprehensive knowledge enabling optimal care decisions.
What types of low back pain benefit most from non-surgical spinal decompression?
Patients with herniated discs, degenerative disc disease, or nerve root irritation are the primary candidates who experience significant relief from non-surgical spinal decompression therapy.
How does Acceptance and Commitment Therapy (ACT) help chronic low back pain patients?
ACT teaches patients mindfulness and acceptance strategies that reduce pain-related distress and enhance quality of life by encouraging engagement in meaningful activities despite persistent pain.
Which medications are recommended for chronic low back pain management, and what precautions are needed?
Duloxetine (SNRI) is recommended due to strong evidence for moderate improvement, along with NSAIDs for acute flare-ups. Caution is advised regarding side effects and medication interactions.
Can topical analgesics like Biofreeze and Salonpas patches replace oral medication for low back pain?
Topical agents provide localized pain relief and can reduce oral medication usage but usually complement rather than completely replace systemic treatments.
What lifestyle changes are critical for preventing recurrence of low back pain?
Incorporating regular exercise, ergonomic adjustments, proper lifting techniques, weight management, and stress reduction practices are essential for preventing back pain relapse.

