What Research Reveals About Rehabilitation and Returning to Work
November 29, 2025
Disc Prosthesis in Lévis: Fast and Lasting Results
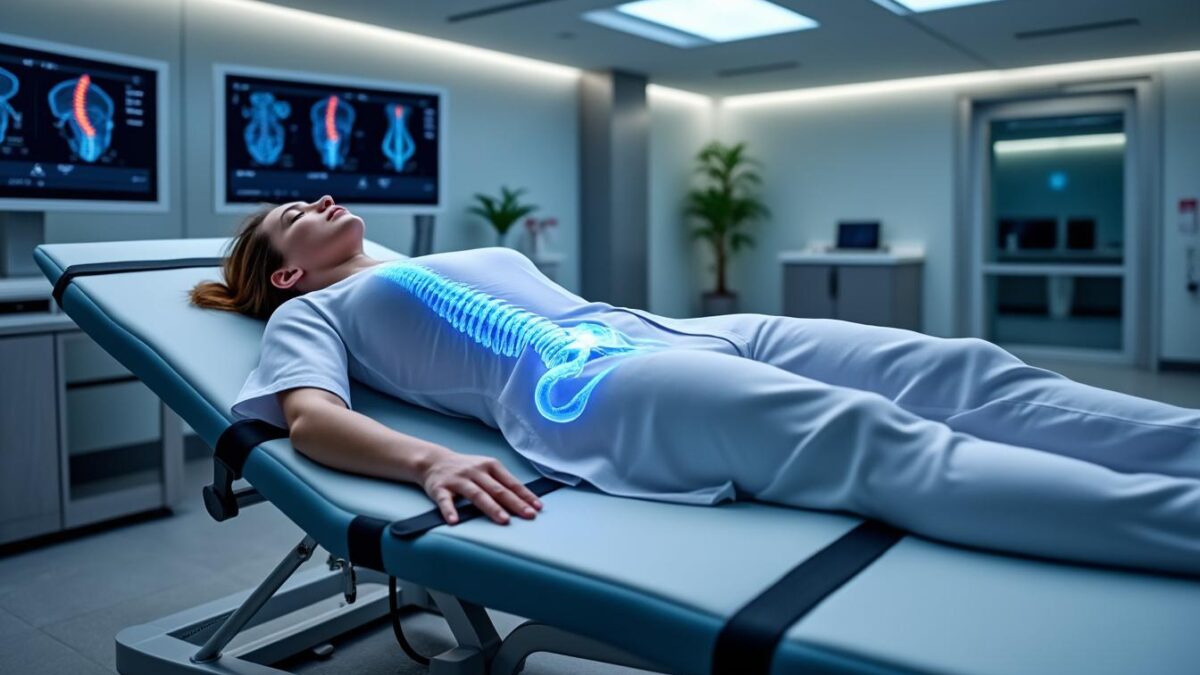
November 29, 2025Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this backdrop, Neurovertebral Decompression Therapy emerges as a groundbreaking non-invasive approach effectively addressing spinal health challenges. This innovative therapy gently relieves pressure on affected discs and nerve roots through controlled mechanical traction, facilitating the body’s natural healing processes. Encompassing advances in robotics and precision medicine, it offers a promising alternative to traditional surgery or prolonged medication regimens, reducing complication risks while enhancing mobility and function.
Endorsed by leading spinal specialists and supported by a growing body of clinical evidence, this therapy integrates tailored treatment plans, patient education, and advanced technology to optimize outcomes. The collaborative healthcare model bridging North America and Europe illustrates the global momentum embracing Neurovertebral Decompression for sustainable back pain relief. With increasing awareness and accessibility, many patients regain pain-free living and restore active lifestyles with this therapeutic modality.
Fundamentals and Therapeutic Advantages of Neurovertebral Decompression
Neurovertebral Decompression Therapy operates on the principle of gently stretching the spine to reduce intradiscal pressure and enhance nutrient flow to affected spinal structures. This controlled, computer-monitored traction is carefully adjusted to patient-specific needs, optimizing decompression without causing discomfort or instability. A key benefit is the creation of an expanded intervertebral space, relieving nerve root compression often associated with herniated discs, sciatica, or spinal stenosis.
Beyond immediate pain relief, the therapy actively contributes to:
- Improved spinal mobility: Relaxing tense paraspinal muscles and restoring normal vertebral alignment significantly enhance flexibility and movement range.
- Enhanced blood circulation: Increased local blood flow supports disc hydration and tissue regeneration, accelerating recovery.
- Prevention of progressive spinal deterioration: Decompression mitigates disc degeneration and foraminal narrowing, preserving spinal integrity.
- Optimized muscular recovery: Reducing inflammation and discomfort allows patients to more effectively engage in complementary rehabilitation exercises.
- Effective non-surgical alternative: Many patients successfully circumvent or delay surgery, benefiting from a conservative approach validated by clinical studies.
Scientific literature and patient testimonials consistently validate these multi-dimensional benefits. This therapy’s capability to address the root causes of spinal dysfunction, rather than merely mask symptoms, aligns with modern pain management’s holistic paradigms. For further understanding on key benefits, detailed explorations can be found via resources like neurovertebral decompression health insights and clinical review articles.
| Therapeutic Component | Clinical Effect | Patient Benefit |
|---|---|---|
| Controlled traction | Reduces nerve root pressure | Rapid pain relief, decreased inflammation |
| Intervertebral space expansion | Facilitates disc rehydration | Improved disc health and spine stability |
| Muscle relaxation | Decreases peripheral tension | Enhanced mobility and posture correction |

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…
Key Indications and Safety Measures in Neurovertebral Decompression Therapy
The success of Neurovertebral Decompression Therapy depends significantly on proper patient selection and adherence to contraindications. Comprehensive assessments by specialized clinicians ensure individualized treatment suitability and safety.
- Primary indications:
- Herniated lumbar and cervical discs causing radiating pain or nerve symptoms.
- Bulging discs with potential to worsen if unaddressed.
- Chronic sciatica and radiculopathies stemming from nerve root compression.
- Spinal foraminal stenosis presenting with functional limitations.
- Mechanical low back pain linked to disc degeneration and poor postural mechanics.
- Contraindications include:
- Severe osteoporosis or other bone-weakening conditions affecting vertebral stability.
- Active spinal infections requiring medical-first interventions.
- High-grade vertebral instability or latest unhealed fractures.
- Pregnancy, unless cleared with specialized medical approval.
These safety parameters allow clinicians to avoid complications while maximizing therapeutic outcomes. The rigorous evaluative process distinguishes Neurovertebral Decompression from less targeted physical rehabilitation techniques. Patients can explore more detailed condition-specific guidance and contraindications through profiles offered by expert providers such as specialized herniated disc care centers.
| Condition | Neurovertebral Decompression Suitability | Notes |
|---|---|---|
| Herniated disc (lumbar/cervical) | High | Excellent outcomes when early and conservative |
| Spinal stenosis | Moderate | Requires careful monitoring and periodic imaging |
| Osteoporosis | Not recommended | Risk of vertebral fracture |
| Active spinal infection | Contraindicated | Treatment delay mandatory |

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Revolutionizing Back Pain Management with Neurovertebral Decompression in Quebec and Beyond
Chronic sufferers of spinal disorders in Quebec often face barriers such as extended wait times and high cost, prompting the healthcare community to innovate accessible treatment paths. Neurovertebral Decompression, spearheaded by experts with decades of experience, integrates advanced robotics with personalized care plans. Operating within specialized clinics like TAGMED, this therapy forgoes conventional generalized physical therapy in favor of precision-targeted intervention supported by interdisciplinary coordination.
A notable innovation is the cross-border treatment pathway connecting Canadian patients with leading surgical centers in France. This transatlantic collaboration, facilitated by logistic partners, allows for seamless surgical referrals when conservative care is insufficient, optimized travel and accommodation arrangements, and coordinated postoperative rehabilitation locally, ensuring continuity and quality of care.
- Advantages of this model include:
- Reduced wait times for evaluation and advanced care.
- Access to cutting-edge surgical techniques and dynamic spinal implants.
- Personalized treatment adjusting conservational and surgical needs.
- Comprehensive post-surgical rehabilitation managed locally.
The integrative approach exemplifies a new standard in chronic back pain management, emphasizing efficient, multidisciplinary collaboration and patient-centered care. Patients interested in details may consult resources detailing how neurovertebral decompression can restore pain-free life.
| Component | Benefit | Provider |
|---|---|---|
| Initial Evaluation | Comprehensive diagnosis and tailored non-invasive care plan | TAGMED Clinic, Quebec |
| Conservative Treatment Phase | Avoid or delay surgery by controlling symptoms and promoting healing | TAGMED Clinic |
| Surgical Referral and Care | Access to innovative surgical techniques and implants in France | French Surgical Centers |
| Postoperative Rehabilitation | Locally coordinated physical therapy and follow-up | Neurotherapy Montreal |

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…
How Neurovertebral Decompression Therapy Supports the Healing Process
The healing process facilitated by Neurovertebral Decompression Therapy involves a cascade of biomechanical and physiological enhancements. By mechanically decompressing spinal segments, the therapy alleviates nerve root irritation and reduces inflammatory mediators responsible for chronic pain sensations. This environment promotes reabsorption of bulging disc material and regeneration of damaged annulus fibers.
Importantly, the therapy improves oxygen and nutrient delivery by increasing local microcirculation, instrumental for cellular repair mechanisms. Improved structural alignment releases compensatory muscle strain, reducing secondary pain patterns. Patients are often better able to participate in complementary rehabilitation, enhancing long-term durability of results.
- Stages contributing to recovery include:
- Immediate pain relief and inflammation reduction.
- Rehydration and morphological restoration of intervertebral discs.
- Normalization of nerve impulse transmission and decreased radicular symptoms.
- Muscle tone restoration and improved posture mechanics.
- Increased mobility and functional independence.
Its scientifically sound mechanisms make Neurovertebral Decompression a pivotal element within conservative back care, supporting not only symptom control but addressing the underlying pathology. More detailed information on the healing effects can be reviewed through materials such as comprehensive spinal decompression therapy guides.
| Healing Phase | Physiological Effect | Patient Outcome |
|---|---|---|
| Decompression | Reduced nerve root compression | Pain relief and nerve symptom reduction |
| Rehydration | Disc regeneration and hydration | Enhanced spinal flexibility and strength |
| Muscle relaxation | Reduced tension and spasms | Better movement and posture |
Integration of Robotic Technology in Neurovertebral Decompression
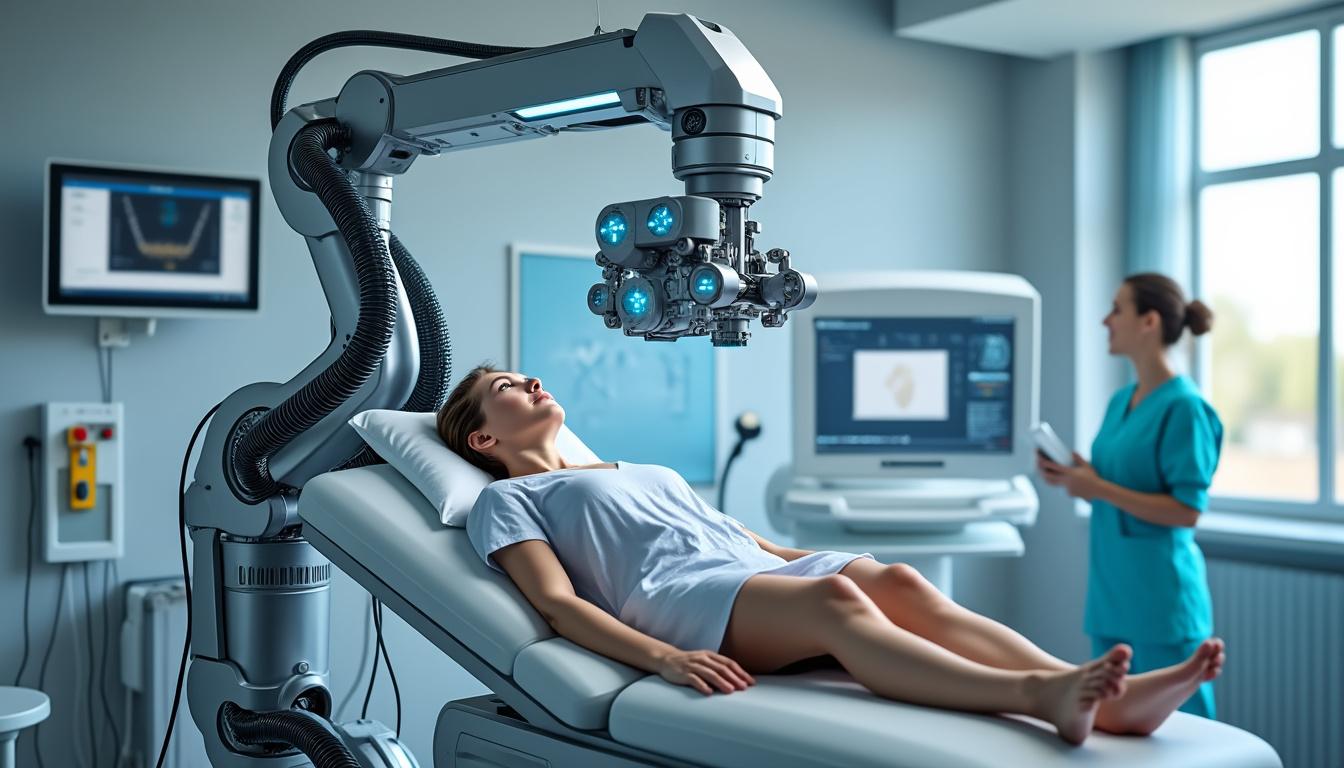
Leveraging advances in robotic assistance and computerized monitoring, modern Neurovertebral Decompression Therapy enhances precision and patient comfort. Robotics enable fine-tuned traction forces tailored in real-time to individual responses, increasing safety and efficacy. These technological advances have been validated by institutions advancing spine surgery, integrating 3D imaging and navigation platforms.
Robotics also significantly reduce manual errors and variability inherent in traditional traction methods, creating consistency across sessions. Patients experience improved outcomes and shorter recovery times, thanks to optimized decompression cycles and better tissue preservation. Institutions like those referenced in recent robotic spine surgery innovations illustrate the promising future of integrating robotics in spinal care.
Comprehensive Patient Education: Empowering Informed Decisions
In the management of chronic back pain, transparent patient education plays a crucial role. Clinicians adopting Neurovertebral Decompression Therapy foster collaborative doctor-patient relationships, simplifying complex medical concepts and clarifying expectations. Clear communication about the treatment’s benefits, possible limitations, and individualized prognosis empowers patients to actively participate in their recovery journey.
- Educational focus areas include:
- Understanding spinal anatomy and pathology.
- Recognizing realistic treatment outcomes.
- Scheduling and adhering to therapy regimens.
- Importance of complementary physical activity and ergonomic adjustments.
- Addressing patient uncertainties and concerns.
Such comprehensive education contributes to enhanced treatment adherence and satisfaction, reducing anxiety and enriching patient engagement. More information on patient-centric education can be explored in clinical articles like how neurovertebral decompression can help regain a pain-free life.

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
Evaluating Neurovertebral Decompression as a Proactive Step Before Surgery
Contemporary spine care increasingly underlines the importance of exhausting conservative treatments before embarking on surgical procedures. A typical protocol recommends a minimum 3 to 6-month course of Neurovertebral Decompression Therapy to assess symptom improvement and functional gains. This approach helps to:
- Confirm the appropriateness of surgical intervention based on treatment response.
- Prepare spinal tissues, reducing perioperative risks and enhancing recovery potential.
- Reduce chronic pain and stiffness, decreasing muscle guarding that could complicate surgery.
- Provide some patients with sufficient relief to avoid surgery altogether.
This strategy aligns with evidence-based practice, emphasizing patient safety, cost-effectiveness, and quality of life improvement. Rigorous monitoring and outcome evaluation during this period ensure adaptive management and minimize unnecessary operations.
| Pre-Surgery Stage | Objective | Expected Outcome |
|---|---|---|
| Neurovertebral Decompression Phase | Pain reduction and functional restoration | Improved mobility, potential avoidance of surgery |
| Surgical Evaluation | Assess necessity based on response | Informed surgical decision with optimized conditions |
| Postoperative Planning | Prepare for enhanced recovery | Faster rehabilitation and lowered complication risks |

International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…
Addressing Common Misconceptions about Neurovertebral Decompression
Despite its clinical success, Neurovertebral Decompression Therapy is often misunderstood, limiting patient access to this beneficial treatment. Common myths include the belief that spinal decompression is painful, invasive, or only suitable for acute injury. Educating the public and healthcare providers plays a vital role in demystifying these misconceptions.
- Myth 1: Decompression causes discomfort or harm – In reality, the controlled mechanical traction is gentle and well tolerated.
- Myth 2: Suitable only for severe spinal conditions – The therapy benefits a wide range of disc and nerve issues including early-stage degeneration.
- Myth 3: Surgery is the only effective solution for chronic back pain – Many patients experience significant improvement without invasive procedures.
- Myth 4: Decompression therapy is a quick fix – It requires dedication to treatment schedules and complementary therapies.
Dispelling these myths improves patient confidence and encourages timely treatment initiation, contributing to better long-term outcomes. Detailed myth-busting discussions are available in articles discussing herniated disc approaches such as those from trusted spinal care resources.

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
Advances in Spinal Surgery Complementing Neurovertebral Decompression Outcomes
When surgery becomes necessary despite conservative approaches, modern minimally invasive techniques and dynamic stabilization implants significantly enhance recovery and function. Access to these innovations adds value to integrated care pathways involving Neurovertebral Decompression as a first-line treatment.
Examples of cutting-edge surgical adjuncts include:
- Mini-invasive and endoscopic procedures reducing tissue trauma.
- Dynamic interlaminar implants, such as IntraSPINE systems, for lumbar stabilization.
- Robotic-assisted navigation platforms improving surgical precision and safety.
- Advanced 3D imaging for tailored operative planning and real-time guidance.
These technologies, showing favorable clinical outcomes, reflect a paradigm shift toward personalized spinal surgery that complements the benefits gained from preceding decompression therapy phases. Medical centers incorporating such advances provide exemplary comprehensive spinal care solutions.
| Innovative Technique | Benefit | Clinical Application |
|---|---|---|
| Mini-invasive surgery | Reduced postoperative pain and recovery time | Herniated disc repair, spinal stenosis |
| Dynamic stabilization implants | Preserve spinal motion and reduce adjacent segment disease | Lumbar degenerative disc disease |
| Robotic-assisted navigation | Enhanced surgical accuracy and safety | Complex spinal surgeries |


Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…
Holistic Approaches Integrating Neurovertebral Decompression and Lifestyle Management
Optimal long-term spinal health incorporates multidisciplinary strategies alongside Neurovertebral Decompression. Lifestyle factors such as ergonomic adjustments, physical activity, nutrition, and stress management synergistically influence recovery and sustain spinal integrity.
- Posture optimization: Education on proper sitting and lifting techniques reduces mechanical stress.
- Targeted physical therapy: Strengthening core musculature supports spine stability.
- Nutrition and hydration: Ensuring adequate micronutrient intake aids tissue repair and disc health.
- Weight management: Limits excess spinal loading, reducing degenerative progression.
- Stress reduction: Minimizes musculoskeletal tension exacerbated by emotional strain.
Patients adhering to such comprehensive programs often experience sustained improvements and reduced recurrence of back pain episodes. Educational resources such as informative guides on spinal decompression and wellness offer valuable insights for integrating lifestyle changes effectively.
| Aspect |
|---|

What Research Reveals About Rehabilitation and Returning to Work
Rehabilitation and the process of returning to work form a complex interplay that extends far beyond physical recovery. It is a multifaceted journey involving medical treatment, psychological adaptation, workplace accommodation, and social reintegration. Research in recent years underscores the profound…
Exploring Neurovertebral Decompression Therapy Benefits in Chronic Pain Relief
For individuals dealing with long-term spinal discomfort, Neurovertebral Decompression Therapy offers a beacon of hope. Chronic back pain limits daily functioning and mental health, often triggering a cycle of reliance on pain medications with unsatisfactory results.
Neurovertebral Decompression addresses the root mechanical causes of chronic pain by decompressing nerve structures and allowing healing processes to occur naturally. Patients typically report:
- Reduction in pain intensity and frequency, enabling better sleep and mood stabilization.
- Increase in spinal flexibility, facilitating activities that were previously limited or painful.
- Decreased dependency on analgesics, reducing potential side effects and improving quality of life.
- Enhanced nerve function, reducing symptoms such as tingling or numbness.
Clinical evidence reinforces these observations, with providers emphasizing the therapy’s role as a natural, non-invasive solution to chronic spinal issues. Patient experiences shared via specialized platforms highlight its transformative impact. Additional insights are presented in comprehensive overviews like expert spinal decompression benefit analyses.
| Benefit | Mechanism | Patient Experience |
|---|---|---|
| Chronic Pain Relief | Reducing nerve root compression and inflammation | Noticeable reduction in pain episodes and medication need |
| Improved Mobility | Increased disc hydration and muscle relaxation | Greater ease in daily activities and exercise tolerance |
| Enhanced Nerve Function | Decompression restoring nerve signaling | Reduction in numbness and tingling sensations |
Personalized Care: Tailoring Neurovertebral Decompression to Patients’ Needs
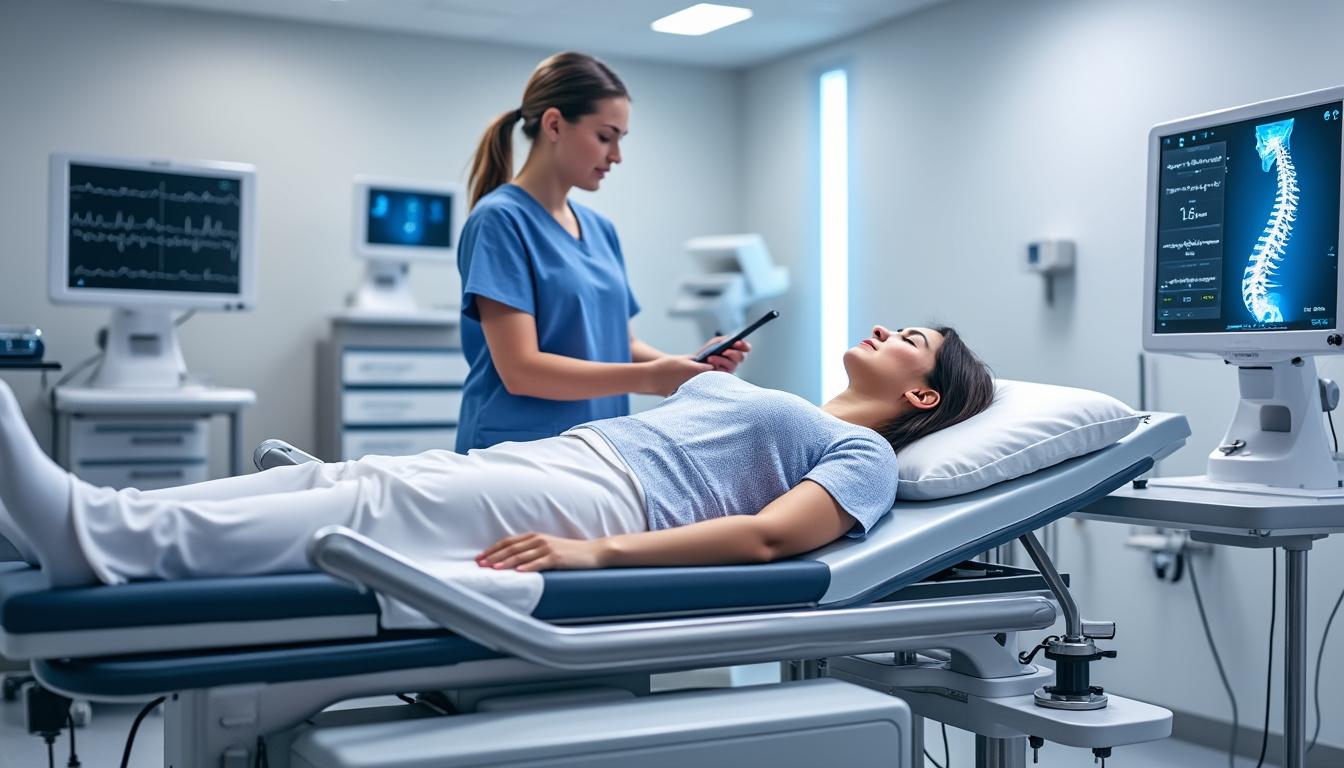
A standout feature of Neurovertebral Decompression Therapy is its capacity for customization. Treatment regimens are adapted to individual anatomical, functional, and symptomatic profiles, enhancing efficacy and patient satisfaction. Advanced diagnostics including MRI and 3D spinal imaging inform intervention strategies.
Clinicians evaluate each patient’s response continually, adjusting traction forces and session frequency. This dynamic approach maximizes therapeutic benefits while minimizing discomfort or adverse effects. Patients actively involved in goal-setting and treatment choices report heightened motivation and compliance.
- Tailoring elements consist of:
- Personalized traction parameters based on disc pathology and symptom severity.
- Integration with rehabilitation therapies for holistic recovery.
- Addressing coexisting conditions such as muscle weakness or postural imbalances.
- Flexible scheduling accommodating individual lifestyle demands.
For further information on personalized neurovertebral decompression care, expert clinics provide detailed insights such as those in patient journey case studies illustrating individualized treatment successes.
Recognizing the Role of Multidisciplinary Teams in Enhancing Therapy Outcomes
Successful Neurovertebral Decompression is often underpinned by collaborative efforts engaging physicians, physical therapists, robotic technicians, and rehabilitation specialists. This multidisciplinary model ensures:
- Comprehensive evaluation and diagnosis integrating diverse expertise for a thorough understanding of spinal pathology.
- Coordinated treatment planning that aligns decompression with physical therapy and lifestyle modification.
- Continuous monitoring and adaptation enhancing safety and maximizing recovery trajectories.
- Patient support and education fostering informed and active participation throughout the journey.
Such integrated care embodies the future of spinal health management, producing superior patient outcomes. Clinics demonstrating successful team-based approaches offer models referenced in training programs and medical literature.
| Team Member | Role | Contribution to Therapy Success |
|---|---|---|
| Spinal Surgeon | Diagnosis and surgical oversight | Ensures appropriate indications and surgical backup |
| Physical Therapist | Rehabilitation and mobility enhancement | Supports functional recovery and exercise guidance |
| Robotic Technician | Operates decompression devices, ensures precision | Maintains safety standards and session customization |
| Patient Educator | Communication and support | Enhances understanding and therapy adherence |
Frequently Asked Questions About Neurovertebral Decompression Therapy
What conditions are best treated with Neurovertebral Decompression?
This therapy is particularly effective for herniated discs, sciatica, spinal stenosis, and chronic mechanical back pain, helping to alleviate nerve compression and improve spinal function.
Is Neurovertebral Decompression Therapy painful or uncomfortable?
The treatment uses gentle, computer-controlled traction to minimize discomfort, with most patients reporting relaxation during sessions.
How long does it take to see results from Neurovertebral Decompression?
Patients often notice pain relief within a few sessions, but a full course of 3 to 6 months ensures optimal healing and lasting benefits.
Can Neurovertebral Decompression replace spinal surgery?
While not all patients can avoid surgery, many experience sufficient relief to postpone or bypass invasive interventions, making it an important conservative option.
Are there any risks or side effects associated with this therapy?
Neurovertebral Decompression is generally safe for appropriately selected patients, with minimal risks when contraindications are observed and treatment is supervised by experienced clinicians.