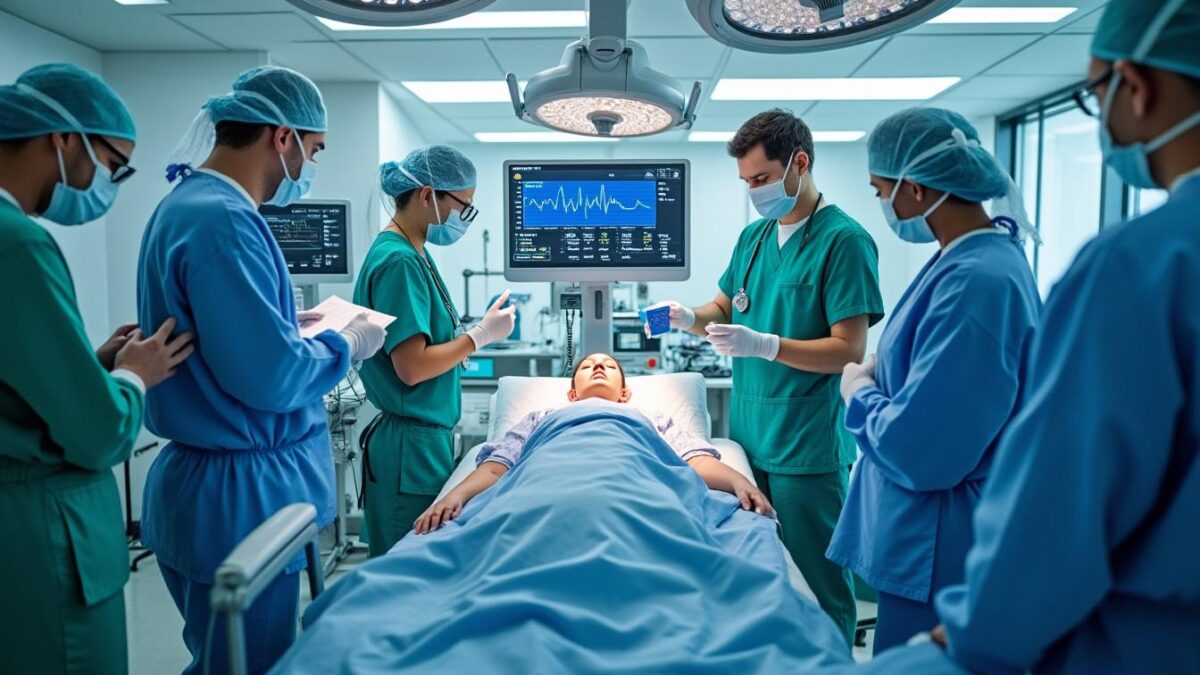
Conservative Treatments vs Surgery: A Clear Guide for Quebec Patients
November 26, 2025
Motion Surgery in Terrebonne: Minimizing Postoperative Complications for Faster Recovery
November 27, 2025The journey to successful spinal surgery is paved with meticulous preparation and comprehensive evaluation. For patients, especially those navigating cross-continental care pathways from Quebec to France, preoperative assessment transcends formalities, embodying a critical, evidence-driven process that shapes surgical outcomes and patient safety. The contemporary landscape of preoperative evaluation integrates advanced clinical assessments, patient-reported outcomes, and tailored multidisciplinary coordination, reflecting state-of-the-art practices in spinal surgical preparation. This approach not only enhances risk stratification and anesthesia planning but also promotes holistic patient evaluation that resonates with modern clinical guidelines. Through an exploration of real-life patient experiences, coupled with healthcare insights and detailed case studies, the intricate dynamics of preoperative pathways reveal their pivotal role in ensuring perioperative management excellence and fostering trust within healthcare teams across borders.
Against a backdrop of technological advances and evolving clinical standards, the importance of a structured preoperative assessment cannot be overstated. It serves as the cornerstone for optimizing patient care, reducing complications, and enabling precise surgical interventions by leveraging both subjective patient input and objective clinical data. This elaborate process, enriched by telemedicine and personalized follow-ups, exemplifies how healthcare systems have adapted to meet increasing expectations for patient-centered care. Highlighted through collaborative models involving specialists such as spinal surgery consultants and multidisciplinary teams, the preoperative phase now functions as an essential safeguard, maximizing therapeutic success and enhancing overall patient quality of life.
Optimizing Surgical Preparation through Comprehensive Preoperative Assessment
Ensuring patient safety and surgical success begins well before the operating room. Comprehensive preoperative assessment plays a vital role in surgical preparation by systematically addressing medical, functional, and psychological factors. It encapsulates strategies for risk stratification—a process that objectively analyzes patient-specific risk factors to tailor anesthesia planning and perioperative management. This dynamic framework considers coexisting conditions, functional capacity, and potential complications, setting the stage for individualized surgical pathways.
Essential components of surgical preparation include thorough clinical examinations, validated questionnaires gauging pain and disability, and specialized imaging analysis. For spinal surgery candidates navigating complex medical profiles, the integration of spinal-specific scoring tools such as the Oswestry Disability Index and Neck Disability Index helps quantify impairment levels and inform decision-making processes.
Successful surgical preparation is facilitated by:
- In-depth medical history and physical exam: Identifies comorbidities impacting anesthesia and surgery risk.
- Patient-reported outcomes: Captured through standardized questionnaires to assess pain, mobility, and quality of life.
- Risk stratification tools: Allow targeted optimization of modifiable factors.
- Collaboration among multidisciplinary teams: Enhances comprehensive case evaluation and perioperative planning.
- Use of telehealth technologies: Improves patient access and follow-up efficiency across geographical barriers.
| Element | Purpose | Impact on Surgical Preparation |
|---|---|---|
| Medical History Review | Identify comorbidities and contraindications | Adjust anesthesia and operative approach |
| Functional Assessments | Evaluate mobility and disability levels | Guide surgical planning and rehabilitation needs |
| Imaging Analysis (MRI, CT) | Confirm diagnosis and lesion characterization | Inform surgical technique and instrumentation choice |
| Psychological Assessment | Identify anxiety, depression, and coping mechanisms | Determine need for psychoeducational support |
| Interdisciplinary Case Conferences | Discuss high-risk or complex cases | Ensure unified surgical and perioperative strategy |
Such an integrative protocol aligns with contemporary clinical guidelines aiming to improve surgical outcomes and patient safety. Detailed insights on these processes can be expanded through specialized literature, for example by consulting respected reviews on preoperative pathways.

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…
Patient Evaluation and the Essential Role of Standardized Questionnaires in Preoperative Settings
Preoperative patient evaluation is a multifaceted process where subjective and objective data converge. A foundation of this approach is the use of rigorous standardized questionnaires, which capture nuances in pain perception, functional impairment, and quality of life essential for tailored surgical planning. These tools enable clinicians to quantify parameters that otherwise evade direct clinical measurement, such as chronic pain intensity and psychosocial impact.
Examples of widely adopted questionnaires include:
- Oswestry Disability Index (ODI): Assesses the degree of disability and functional limitation from lumbar spine-related pain.
- Neck Disability Index (NDI): Targets cervical spine impairment specifically, influencing technique selection.
- SF-36 Health Survey: Offers a holistic view encompassing physical health and emotional wellbeing.
- Visual Analog Scale (VAS): Measures dynamic pain intensity over time.
The deployment of these questionnaires is carefully structured to ensure honest, reliable responses. Patients may complete these independently or with assistance, emphasizing accurate communication over speed. This methodology facilitates a detailed patient profile that underpins objective risk stratification and delineates indications for surgery versus conservative treatments.
| Questionnaire | Main Objective | Influence on Patient Management |
|---|---|---|
| Visual Analog Scale (VAS) | Quantify pain intensity | Guide urgency and intervention type |
| SF-36 Health Survey | Assess general health and quality of life | Inform postoperative rehabilitation planning |
| Neck Disability Index (NDI) | Measure cervical spine functional limitation | Determine fusion or dynamic stabilization need |
| Oswestry Disability Index (ODI) | Evaluate lumbar spine disability scale | Confirm suitability and type of spine surgery |
Integration of these validated tools not only enhances preoperative decision-making but also correlates strongly with postoperative satisfaction and complication rates. Moreover, critical patient feedback has demonstrated better outcomes when these assessments inform adjustment of perioperative and rehabilitation protocols. For a much deeper dive into these assessment measures and their clinical applications, readers can consult dedicated resources such as comprehensive guides on initial assessments.

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Advanced Initial Assessments and Imaging: Foundations of Candidate Eligibility in Spine Surgery
Besides questionnaires, a comprehensive preoperative assessment demands advanced clinical examinations and interpretation of sophisticated imaging studies. These initial assessments validate surgery eligibility by confirming lesion specifics and ruling out contraindications, thereby safeguarding patient outcomes.
Key aspects of initial evaluations include:
- Thorough clinical examination: Detects neurological deficits, evaluates functional capacities, and confirms the absence of systemic risks.
- Imaging review: Expert analysis of patient-supplied imaging (MRI, CT scans, radiographs) identifies disc herniations, stenosis, or vertebral instability.
- Neurofunctional evaluation: Assesses nerve root and spinal cord functionality alongside the autonomic system, adjusting operative and rehabilitative strategies accordingly.
- Multidisciplinary case deliberation: Collaborative review meetings between Canadian and French experts harmonize approaches to complex cases, ensuring a consensus on optimal surgical technique.
- Supplemental testing: Additional investigations ordered for ambiguous cases, tailored to uncover contraindications or refine diagnosis.
| Assessment Component | Specific Objective | Effect on Patient Care Pathway |
|---|---|---|
| Imaging (MRI, CT) | Define pathology localization and characteristics | Guide personalized surgical technique and hardware selection |
| Neurological Evaluation | Measure nerve and spinal cord impairments | Adapt operative planning and rehabilitation protocols |
| Clinical Examination | Identify potential contraindications and comorbidities | Confirm surgical feasibility and safety |
| Multidisciplinary Team Review | Consolidate diagnostic insights and therapeutic decisions | Optimize shared decision-making and interprofessional coordination |
Implementing these initial assessments within a comprehensive workflow mirrors practices recommended by specialized literature. Clinics like those led by the Dr. Sylvain Desforges team at TAGMED emphasize the value of rigorous initial analyses. Contemporary surgical pathways in France increasingly leverage advanced techniques such as dynamic stabilization devices like the IntraSPINE system and TOPS implants, which demand meticulous preoperative planning to ensure optimal patient benefit. Detailed discussions of these techniques and initial assessment protocols are accessible in clinical journals on safe and successful surgery methodologies, for instance key surgical preoperative assessments.

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…
Insights from Real-Life Patient Experiences: Enhancing Multidisciplinary Coordination and Communication
Patient narratives offer invaluable perspectives on the effectiveness and human impact of comprehensive preoperative assessments. Through analysis of experiences from hundreds of patients engaged in a Quebec-France surgical journey, several themes emerge around communication, emotional support, and logistical facilitation. These insights have driven enhancements in perioperative management and patient-centered care models.
Commonly highlighted factors influencing patient satisfaction include:
- Clear and empathetic communication: Transparent explanations about procedures, risks, and expectations.
- Personalized support services: Humanized accompaniment, especially by entities like Neurothérapie Montréal that provide tailored follow-up and emotional reassurance.
- Efficient logistics and coordination: Seamless organization of travel, accommodation, and appointment scheduling coordinated by agencies such as SOS Tourisme Médical.
- Collaborative interdisciplinary teamwork: Harmonized care between Canadian and French surgical teams.
- Use of multimedia educational materials: Videos and guides improving patient understanding and preparedness.
| Experience Aspect | Positive Feedback | Improvement Recommendations |
|---|---|---|
| Communication | Clarity, availability of interlocutors | Enhance preoperative educational communication tailored to individual needs |
| Patient Support | Humanized accompaniment valued | Develop psychoeducational resources to support emotional preparation |
| Logistics | Smooth coordination of travel and appointments | Streamline inter-institutional communications to reduce delays |
| Educational Tools | Usage of guides and videos appreciated | Expand multimedia materials for broader patient access |
| Teamwork | Integrated multidisciplinary management | Ongoing training incorporating patient feedback |
The continuous feedback loop created through patient experiences is a critical driver for quality improvement. It fosters trust in multidisciplinary care teams and refines preoperative and postoperative management protocols. For comprehensive engagement with this topic, explore detailed patient narratives and strategies to enhance healthcare communication at patient-centered preoperative assessment case studies.

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
Statistical Analysis of Patient Outcomes and Continuous Improvement in Preoperative Protocols
Analyzing aggregated data from patient questionnaires and follow-ups provides objective metrics essential for refining preoperative strategies in spinal surgery. This continuous quality improvement model aligns with healthcare insights recommending evidence-based adjustments tailored to reducing complications and maximizing patient satisfaction.
Key performance indicators routinely tracked include:
- Patient satisfaction rates: High satisfaction correlates with effective communication and personalized care.
- Average treatment timelines: Streamlining reduces wait times and associated anxiety.
- Postoperative complications: Incidence decreases with stringent candidate selection and follow-up protocols.
- Rehabilitation customization: Tailored therapy plans promote expedited recovery and functional restoration.
| Indicator | Purpose | Observed Impact |
|---|---|---|
| Patient Satisfaction | Measure care quality and trustworthiness | Improved communication leads to higher scores |
| Treatment Timelines | Assess efficiency of surgical pathways | Reduced delays enhance patient experience |
| Postoperative Complications | Track safety and surgical success | Lower complication rates due to rigorous selection |
| Rehabilitation Personalization | Optimize functional recovery | Faster return to daily activities supported |
The integration of digital follow-up systems further enables real-time monitoring and proactive management, supporting the vision of a data-driven perioperative future. This approach aligns with emerging clinical guidelines emphasizing patient safety through customized care pathways, as discussed comprehensively in recent medical publications on surgical preparation and risk management available at scientific journals focusing on patient safety.
Preoperative Assessment: Steps, Key Components, and Patient Benefits
Interactive infographic to understand the preoperative assessment process and its impact
Steps in Preoperative Assessment
Key Components
Patient Benefits
Estimate Surgery Readiness Score
Adjust the patient parameters below to see an estimated readiness score for surgery.
Real-Life Experiences on Preoperative Assessment
Below is a selection of real anonymous patient quotes fetched from a public API for educational purposes.
Loading patient experiences…

International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…
Preparing Questionnaires and Initial Exams: Effective Strategies for Patient-Driven Preoperative Success
Successful preoperative assessment relies heavily on patient collaboration in preparing initial medical documentation and completing questionnaires with accuracy. This patient-driven preparation ensures timely processing and enables healthcare teams to design safe and appropriate treatment plans.
Important strategies for preparation include:
- Medical record compilation: Collect all spinal imaging (MRI, CT, X-rays) and previous clinical reports.
- Accurate questionnaire completion: Respond sincerely and thoughtfully to items assessing pain, mobility, and mental health.
- Assistance from relatives: Involve relatives to facilitate understanding and response clarity when needed.
- Cooperation with medical teams: Provide additional documents or clarifications promptly upon request.
- Pre-journey logistic planning: Engage with service coordinators to organize travel and accommodation effectively.
| Preparation Step | Patient’s Role | Benefit to Preoperative Process |
|---|---|---|
| Medical Document Collection | Retrieve and organize records | Completeness accelerates assessment |
| Questionnaire Completion | Provide honest and detailed answers | Enables precise clinical evaluation |
| Family Assistance | Support understanding and documentation | Improves response quality and reduces errors |
| Cooperative Communication | Promptly address information requests | Prevents delays and enhances safety |
| Logistical Arrangements | Plan travel, lodging, and appointments | Smooth transition through care phases |
Neurothérapie Montréal and SOS Tourisme Médical play pivotal roles in coaching patients through these preparations, removing stress factors and ensuring readiness for the evaluation phase. This patient-centric guidance exemplifies systems integrating medical expertise with empathetic care management, improving overall perioperative outcomes. Complete details on preparatory recommendations can be found in patient-targeted educational materials at explained preoperative assessment guides.


Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
Emerging Technologies and Innovations Shaping Preoperative Assessment in Spine Surgery
The evolving landscape of spinal surgery preoperative assessment embraces cutting-edge technologies to enhance diagnostic accuracy and surgical precision. Advances in 3D imaging, robotic-assisted navigation, and minimally invasive procedures are revolutionizing how candidates are evaluated and prepared for surgery.
Key technological innovations include:
- 3D Imaging and Modeling: Enables detailed visualization of spinal anatomy and customized surgical planning.
- Robotic Navigation Systems: Provide precise guidance for implant placement and reduce intraoperative risks.
- Minimally Invasive Techniques: Decrease tissue trauma and promote faster recovery.
- Telemedicine Platforms: Facilitate preoperative assessments and postoperative monitoring remotely.
- Dynamic Stabilization Implants: Such as IntraSPINE and TOPS systems allow for motion preservation and tailored stabilization.
| Technology | Purpose | Benefits to Preoperative and Surgical Outcomes |
|---|---|---|
| 3D Imaging | Enhanced anatomical understanding | Improves surgical planning and implant fit |
| Robotic-Assisted Navigation | Precision in instrumentation | Reduces complications and operative time |
| Minimally Invasive Surgery | Less trauma and quicker recovery | Shortens hospital stay and improves satisfaction |
| Telemedicine | Remote assessment and follow-up | Enhances access and continuity of care |
| Dynamic Stabilization Devices | Motion preservation with stability | Improves functional outcomes and durability |
The adoption of these technologies reflects a broader commitment to precision medicine and personalized care in spinal surgery. For practitioners aiming to deepen their knowledge on emerging advancements, specialized training programs such as the Endoscopic Spine Course IRCAD Strasbourg and the Inter-University Diploma in Spine Surgery offer comprehensive educational opportunities that address clinical innovation and evidence-based practice.

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…
Regulatory and Ethical Considerations in Cross-border Preoperative Assessments
Navigating the complexities of international preoperative assessments involves stringent adherence to regulatory standards and ethical principles that safeguard patient autonomy and confidentiality. The unique challenges faced by patients traveling from Quebec to France for spinal surgery highlight the importance of transparent consent processes and data privacy compliance in multiple healthcare environments.
Regulatory considerations include:
- Compliance with data protection laws: Ensuring safe handling of patient records and sensitive information across jurisdictions.
- Informed consent: Clear communication about risks, benefits, and alternatives to ensure voluntary participation.
- Inter-institutional collaboration frameworks: Legal agreements facilitating seamless transfer of medical information and coordinated care.
- Ethical oversight and patient advocacy: Promoting equitable access to care and addressing cultural sensitivities in surgical preparation.
- Transparency in billing and administrative processes: Avoiding hidden costs and clarifying insurance coverage.
| Area | Requirement | Impact on Patient Experience |
|---|---|---|
| Data Protection | Adherence to GDPR and local privacy laws | Builds trust and ensures legal compliance |
| Informed Consent | Comprehensive risk disclosure and documentation | Empowers patient decision-making |
| Collaboration Agreements | Formalize inter-institutional medical data exchange | Enables integrated care pathways |
| Ethical Governance | Prioritize patient welfare and fairness | Supports culturally appropriate care |
| Financial Transparency | Clear billing structures and insurance coordination | Reduces patient anxiety over costs |
This regulatory framework ensures quality and ethical standards underpin patient safety throughout complex cross-border surgical preparation. Detailed insights on regulatory strategies can be found in medical policy literature and reports, such as those covering ethical aspects of preoperative care.

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…
Integrating Perioperative Management and Long-term Follow-up for Enhanced Patient Outcomes
The comprehensive preoperative assessment is but one phase in a continuum of perioperative management designed to improve surgical success and long-term recovery. Coordinated follow-up and rehabilitation programs tailored to individual patient profiles help sustain functional gains and quality of life after spinal surgery.
Key facets of perioperative management include:
- Customized rehabilitation protocols: Incorporating physical therapy, occupational therapy, and neurotherapy.
- Regular clinical evaluations: Monitoring for postoperative complications and neurological recovery.
- Psychosocial support services: Addressing emotional adjustment and pain coping mechanisms.
- Digital monitoring platforms: Remote patient engagement for symptom tracking and early intervention.
- Interdisciplinary collaboration: Facilitating communication between surgeons, therapists, and primary care providers.
| Management Component | Function | Effect on Patient Recovery |
|---|---|---|
| Rehabilitation Protocols | Optimize physical restoration and functional independence | Accelerates return to activities of daily living |
| Clinical Follow-up | Early detection of complications and neurological status | Mitigates adverse events and guides therapy adjustment |
| Psychosocial Support | Manage emotional wellbeing and pain perception | Enhances overall quality of life and reduces distress |
| Telemonitoring | Real-time remote patient assessment | Enables rapid clinical response and supports continuity |
The ongoing coordination within perioperative care amplifies the foundational benefits of thorough preoperative assessment, establishing a holistic patient-centered continuum that defines best practices in spinal surgery care. Readers seeking comprehensive strategies on this integration may benefit from resources like perioperative patient management overviews.
What is the purpose of preoperative questionnaires in spinal surgery?
They systematically capture pain levels, quality of life, and functional limitations critical for personalizing surgical and postoperative care.
Which initial exams are essential before spinal surgery in France?
Reviewing patient-provided imaging (MRI, CT scans), comprehensive neurofunctional evaluation, and multidisciplinary team assessment.
How can patients prepare effectively for preoperative assessment?
Collecting relevant medical records, completing questionnaires truthfully, and coordinating with care teams for additional information or documentation.
What happens after spinal surgery regarding follow-up?
A personalized follow-up with rehabilitative therapy and continuous monitoring to optimize recovery, often coordinated by specialized neurotherapy centers.
How does risk stratification impact anesthesia planning?
By identifying patient-specific risks, anesthesia protocols are tailored to reduce complications and improve perioperative safety.