
Understanding Herniated Discs in Rosemont–La Petite-Patrie: Costs, Insurance Coverage, and Neurovertebral Decompression Treatments
October 31, 2025
The Role of Franchir in Supporting Patients Throughout Their Care Journey
October 31, 2025The advances in spinal surgery have prompted innovative approaches to post-operative recovery, among which repetitive Transcranial Magnetic Stimulation (rTMS) plays a pivotal role. This neuromodulatory technique leverages targeted magnetic pulses to promote neural plasticity and alleviate chronic pain, thereby reshaping patient care after complex interventions. Across transatlantic collaborations between Quebec and France, patients benefit from an orchestrated continuum of care integrating rTMS alongside state-of-the-art surgical protocols, ensuring not just structural healing but functional restoration and psychological well-being.
The integration of rTMS as an adjunct in spinal surgery recovery reflects significant progress in non-invasive brain stimulation. Patients undergoing procedures such as laminectomies, discectomies, and spinal fusions are finding their convalescence enhanced by modulation of cortical regions linked to pain processing and motor control. Distinct rTMS devices including Neurostar, BrainsWay, Magstim, MagVenture, CloudTMS, eNeura, Neuronetics, Deymed, Yiruide, and Remed have contributed to refining protocols that are safe, effective, and individually tailored. This multidisciplinary approach blends surgical excellence, neurophysiological insights, and personalized rehabilitation strategies.
Fundamental Principles and Clinical Applications of rTMS for Postoperative Spinal Recovery
Repetitive Transcranial Magnetic Stimulation (rTMS) harnesses electromagnetic induction to non-invasively modulate cortical excitability. The technique employs focused magnetic fields generated by coils placed strategically on the scalp, inducing electric currents that activate neuronal circuits. Particularly, stimulating the sensorimotor cortex, dorsolateral prefrontal cortex, and motor areas influences pain perception, motor function, and emotional regulation—key components in postoperative recovery.
Clinical applications of rTMS after spinal surgery are increasingly diverse:
- Neuropathic Pain Management: Post-laminectomy syndrome often induces persistent neuropathic pain; targeted stimulation of the sensorimotor cortex can reduce pain intensity by over 30%, improving patient comfort and functionality.
- Psychological Support: Postoperative depression and anxiety are frequent; high-frequency stimulation of the left dorsolateral prefrontal cortex has shown efficacy in mood elevation and anxiety reduction, addressing often overlooked dimensions of healing.
- Motor Recovery Enhancement: For patients with motor impairments post spinal trauma or stroke, rTMS improves neuronal plasticity, accelerating rehabilitation outcomes and restoring functional abilities.
Methodologically, sessions usually last 15 to 30 minutes, requiring no anesthesia or hospitalization. Protocols are adapted per patient’s clinical progression and tolerance, optimizing therapeutic effectiveness. Prominent medical centers utilize devices such as MagVenture and Magstim to administer precise stimulation per patient profiles, ensuring safety and maximized benefits.
| Postoperative Indication | Stimulation Target | Expected Clinical Benefits | Typical Protocol Duration |
|---|---|---|---|
| Post-laminectomy Neuropathic Pain | Sensorimotor Cortex | ≥30% reduction in pain intensity | 2 to 4 weeks |
| Postoperative Depressive Symptoms | Left Dorsolateral Prefrontal Cortex | Significant mood improvement, anxiety decline | 3 to 6 weeks |
| Motor Recovery Post-Spinal Injury or Stroke | Motor Cortex | Optimized neural plasticity, faster rehabilitation | 4 to 8 weeks |
Recent clinical investigations have substantiated these benefits. For example, a randomized trial documented noteworthy pain relief and mood stabilization using rTMS following spine surgeries (expert insights on post-surgery rTMS integration). The absence of pharmacological side effects further positions rTMS as a valuable addition to multidisciplinary rehabilitation.
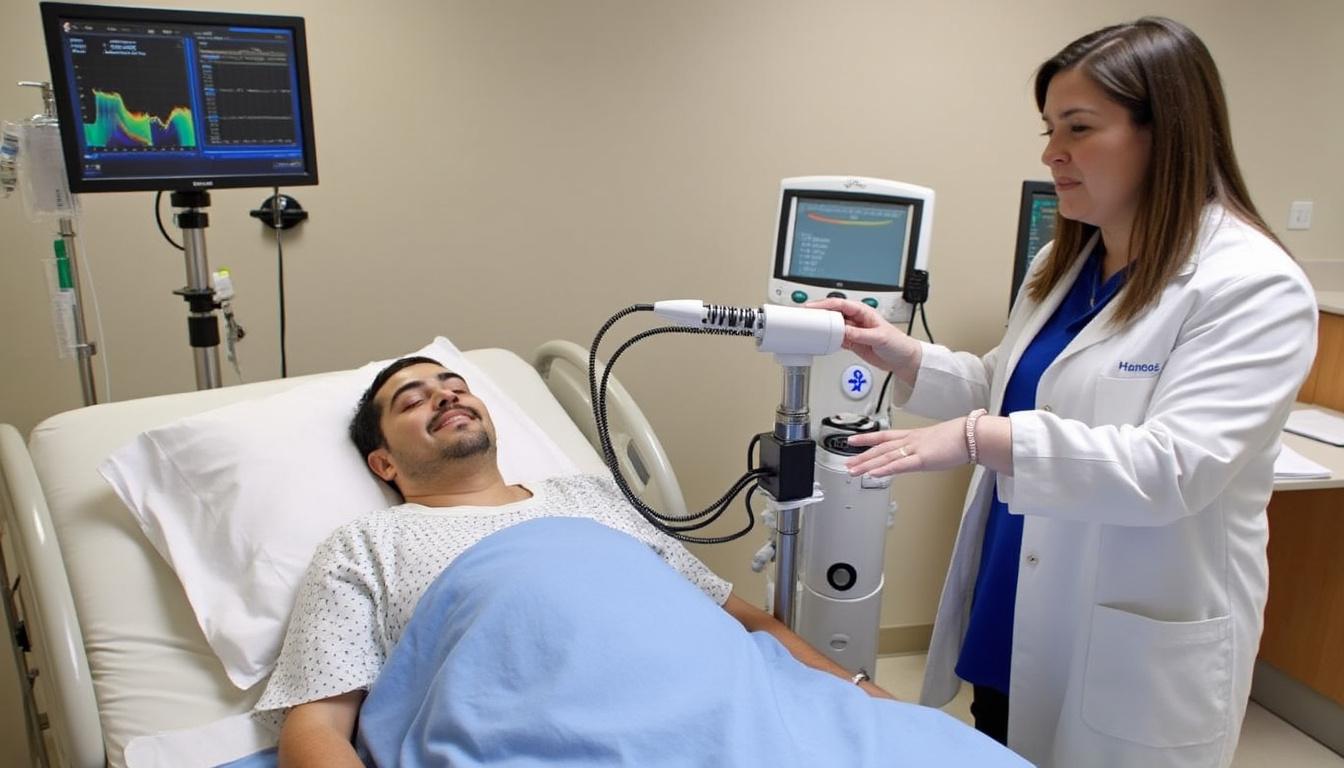

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…
Coordinated Franco-Québécois Patient Management for Enhanced Post-Surgical Outcomes Using rTMS
For patients traveling from Quebec to France for spinal surgery, seamless coordination between healthcare providers across continents is essential. Neurothérapie Montréal plays a pivotal role by orchestrating a comprehensive program beginning pre-operatively and extending through the post-operative phase, integrating rTMS as a cornerstone of neurorehabilitation.
Key actions through the continuum of care include:
- Pre-Operative Preparation: Compilation and transmission of detailed medical records ensure French surgical teams are fully apprised of clinical histories and neurofunctional assessments.
- Neurofunctional Assessment: Evaluations before surgery highlight deficits and guide post-op rTMS programming, customizing each patient’s rehabilitation roadmap.
- Psychophysical Preparation: Preparing patients psychologically and physically enhances resilience and readiness for surgical recovery.
- Real-Time Surgical Support: Continuous communication with French teams supports anticipatory care and post-op planning.
- Postoperative Follow-Up in Quebec: Regular surveillance and adjustment of neuromodulation treatments coupled with integrated physiotherapy maximize recovery.
- Psychological Interventions: Addressing emotional sequelae, often concurrent with spinal operations, ensures holistic care.
| Recovery Phase | Neurothérapie Montréal’s Role | Primary Objective |
|---|---|---|
| Pre-Operative | Neurofunctional evaluation and dossier coordination | Optimize surgical success, prepare for recovery |
| During Surgery | Collaborative support with French teams | Ensure continuity and responsiveness of care |
| Post-Operative | Personalized monitoring and rTMS neuromodulation | Optimize rehab, prevent complications |
Patients consistently report reduced anxiety stemming from coordinated care, underscoring how a well-structured transatlantic partnership effectively bridges the complex challenges of cross-border surgical journeys. The inclusion of rTMS tailored by experts promotes functional milestones and mitigates risks associated with neuropathic pain and mood disorders, as detailed in hidden benefits of integrating rTMS after surgery.

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Strategic Partnerships Facilitating Transatlantic Surgical and Neuromodulatory Care
Effective patient care post-spinal surgery between Quebec and France relies heavily on the integrated efforts of specialized organizations. SOS Tourisme Médical, Franchir, and Neurothérapie Montréal collectively streamline all phases of the patient journey, from initial consultation to full recovery supported by rTMS.
- SOS Tourisme Médical: Provides comprehensive information, eligibility clarification, and administrative assistance, alleviating patient uncertainty regarding surgical technologies and requirements.
- Franchir: Expertly manages site selection, surgeon matching, and logistical arrangements including travel and accommodation, ensuring a smooth surgical stay.
- Neurothérapie Montréal: Ensures long-term postoperative care emphasizing neuromodulation therapy via rTMS, maximizing functional and emotional recovery.
| Partner | Primary Function | Added Value for Patients |
|---|---|---|
| SOS Tourisme Médical | Information dissemination and administrative support | Clarity on options and simplified processes |
| Franchir | Orientation and travel logistics | Tailored surgical choice, stress reduction |
| Neurothérapie Montréal | Post-op monitoring and neuromodulation | Advanced therapeutic support and recovery optimization |
This threefold collaboration exemplifies a patient-centric model designed to overcome distance barriers and deliver innovative post-surgical care. As technologies from leading manufacturers such as Neuronetics and MagVenture continue to evolve, so too does the potential for improving recovery trajectories, representing a synergy of expertise and patient empowerment highlighted in the comprehensive guide to post-surgery rTMS integration.

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…
Advanced Minimally Invasive Spinal Surgery Techniques and Complementary rTMS Role in Functional Recovery
Recent years have seen considerable refinement in spinal surgery methods, prominently within French medical centers renowned for excellence. Techniques incorporating mini-invasive approaches, dynamic stabilization devices such as IntraSPINE prostheses, and cutting-edge implants contribute to enhanced outcomes. Alongside, rTMS acts as a strategic adjunct to these innovations.
The complementary functions of rTMS in this advanced surgical landscape include:
- Accelerated Pain Control: Postoperative neuromodulation reduces acute pain especially after complex interventions such as arthrodesis.
- Syndrome Post-Laminectomy Prevention: Timely rTMS targets maladaptive neural circuits mitigating chronic painful syndromes frequently difficult to treat.
- Functional Reintegration: Enhancing cerebral plasticity supports earlier and safer resumption of physical activity and occupational engagement.
| Surgery Type | rTMS Functional Role | Observed Clinical Impact |
|---|---|---|
| Simple procedures (discectomy, decompression) | Rapid reduction of acute pain | Facilitated walking within 2 weeks, significant pain relief |
| Motion-sparing surgery (disc prosthesis) | Plasticity enhancement, neuropathic pain prevention | Gradual sports resumption in 2-3 months with less pain |
| Fusion/arthrodesis | Extended support for chronic pain management and rehab | Improved endurance and rehab tolerance |
Evidence emerging from institutions employing devices from BrainsWay and Neuronetics corroborates these findings, endorsing rTMS as a transformative complement within comprehensive spinal surgery care. This integration exemplifies the dynamic interplay between technological progress in surgery and non-invasive neuromodulation shaping rehabilitation paradigms.
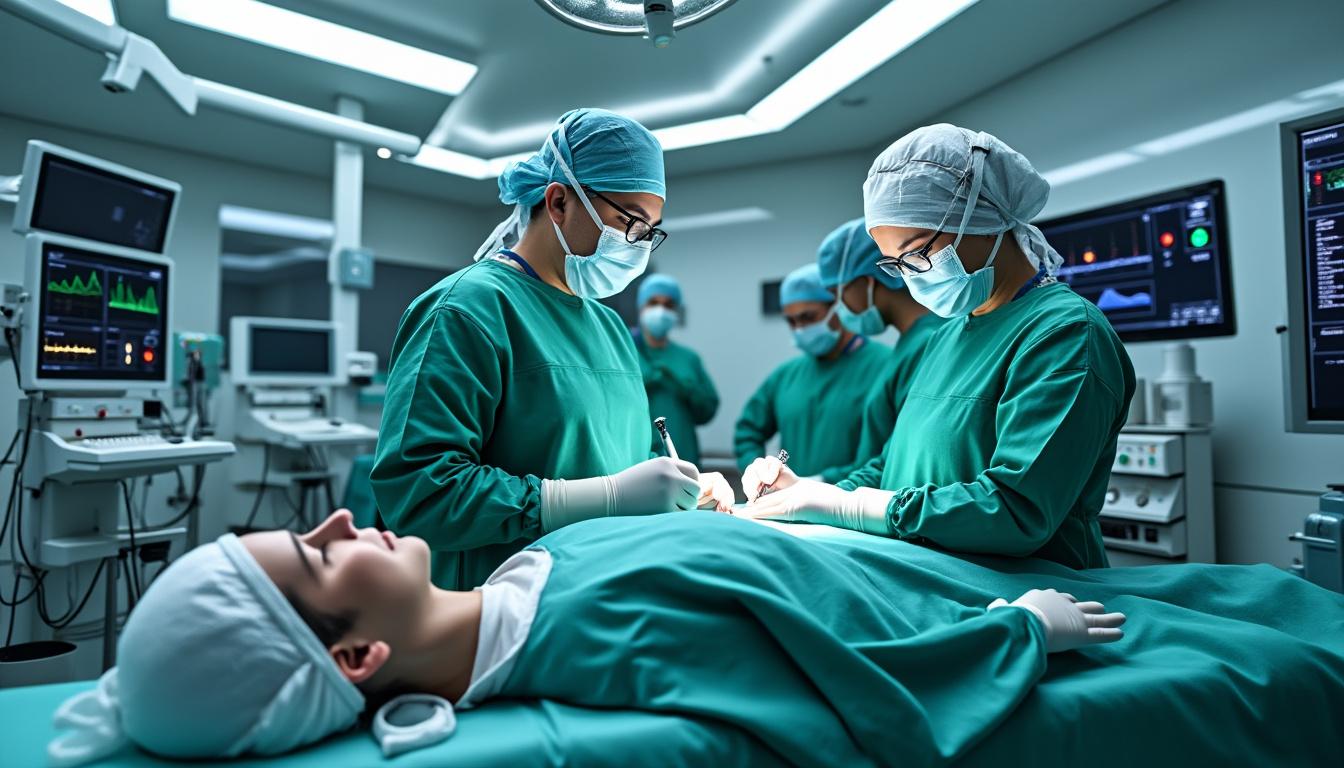

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
Structured Rehabilitation Timelines and Case Studies from Neurothérapie Montréal’s Patient Cohort
Recovery timelines vary considerably depending on surgical complexity and patient health status. Neurothérapie Montréal’s protocols emphasize monitored, staged convalescence supported by both physical therapy and rTMS neuromodulation to promote plasticity and emotional well-being.
An illustrative rehabilitation structure includes:
- Early Ambulation: Initiated during the first or second week for uncomplicated surgeries, progressively increasing activity levels.
- Work Resumption: Typically feasible after 4-6 weeks for minor procedures and extended to 8-12 weeks following extensive fusion surgeries.
- Sporting Activities: Carefully phased comeback starting around 3 months, frequently augmented by rTMS to optimize sensorimotor recovery.
| Surgery Type | Recovery Highlights | Role of rTMS | Estimated Duration |
|---|---|---|---|
| Discectomy | Enhanced mobility and acute pain management | Reduction of pain, neural plasticity stimulation | 6 to 8 weeks |
| Disc prosthesis implantation | Neuropathic pain prevention and functional maintenance | Circuit stimulation, prevention of posterior syndromes | 2 to 3 months |
| Arthrodesis/fusion | Chronic pain management and psychological support | Mitigation of chronic pain, rehab optimization | 4 to 6 months |
Selected patient cases underscore these outcomes:
- Jean, 48 years: Post lumbar fusion, experienced dramatic neuropathic pain relief through combined rTMS and tailored rehab, achieving moderate sports activity within six months.
- Marie, 35 years: Following cervical disc prosthesis surgery complicated by post-laminectomy syndrome and anxiety, benefited from individualized rTMS protocols, experiencing functional and emotional improvement within weeks.

International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…
Exploring Technical Innovations in rTMS Devices Enhancing Postoperative Care
Technological advances by manufacturers including Deymed, Yiruide, Neurostar, and Remed have propelled rTMS devices towards greater precision, ease of use, and patient comfort. Innovations in coil design, integration with brain-computer interfaces, and software algorithms facilitate personalized treatment patterns. These enhancements address challenges such as stimulation targeting, protocol standardization, and session optimization.
Key technological benefits encompass:
- Enhanced Targeting: Focal coil technologies allow stimulation of specific cortical regions implicated in neuropathic pain and functional deficits.
- Adaptive Protocols: Real-time feedback systems align stimulation intensity and frequency to individual neurophysiological responses.
- Increased Patient Tolerance: Noise reduction and ergonomic coil shapes improve comfort during therapy.
| Manufacturer | Device Features | Clinical Advantages |
|---|---|---|
| Deymed | Multichannel coils with adaptive software | Precise modulation of complex cortical networks |
| Yiruide | High-frequency stimulator with patient-friendly design | Improved tolerability and session adherence |
| Neurostar | FDA-cleared system with neuronavigation support | Optimized targeting for depression and pain syndromes |
| Remed | Wearable coil technology with cloud-based programming | Remote monitoring and customization enhancing accessibility |
Continuous integration of software and hardware innovations remain vital for expanding rTMS applications post spinal surgery, establishing a new standard exemplified in recent literature on neuromodulation (neuromodulation advancements).
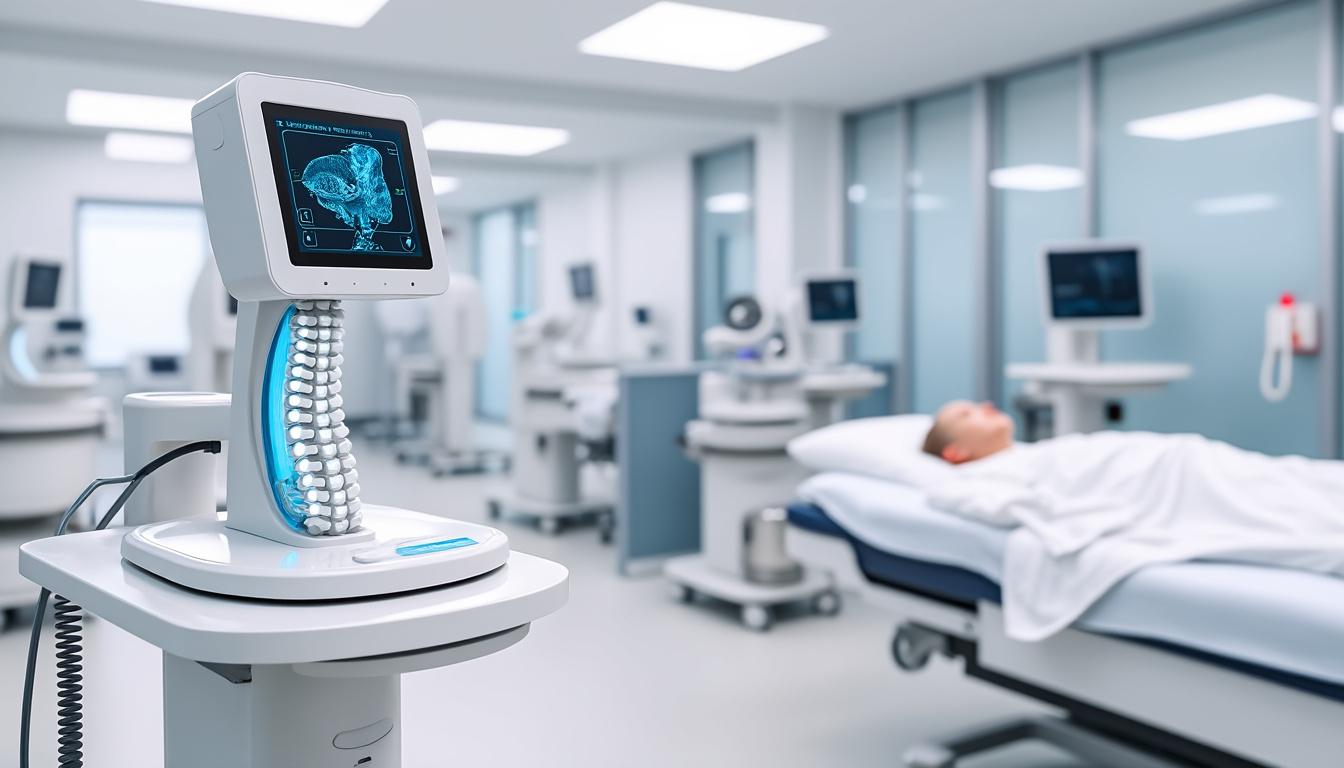
Key Benefits of rTMS in Post-Surgical Spinal Recovery

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
Patient Perspectives on rTMS Integration Following Spine Surgery
Patients embracing rTMS after spinal procedures frequently report enhanced wellbeing. The integration of neuromodulation into recovery protocols addresses the multifaceted impact of spinal pathologies including chronic neuropathic pain and postoperative mood disorders. Patients appreciate non-invasive, drug-free approaches with minimal side effects and flexible session scheduling.
Testimonials highlight:
- Significant pain reduction: Enabling increased activity and daily function.
- Mood stabilization: Improved motivation and reduced postoperative anxiety.
- Rehabilitation synergy: Complementing physiotherapy to expedite progress.
- Personalized treatment plans: Adjusted to individual medical profiles and response patterns.
These patient experiences reinforce the clinical data, illustrating how rTMS yields measurable improvements in recovery speed and quality, achieving outcomes described in benefits of rTMS integration post-surgery.

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…
Challenges and Future Directions in rTMS-Based Postoperative Care
Despite encouraging results, challenges persist in standardizing rTMS protocols across diverse surgical contexts. Protocol optimization requires balancing stimulation parameters, session frequency, and targeting precision. Greater multicenter trials and real-world evidence are needed to establish guidelines for widespread clinical adoption.
Areas warranting further research include:
- Long-term efficacy and maintenance therapy: Identifying sustained benefits and optimal booster session timing.
- Integration with pharmacotherapy: Understanding synergistic or antagonistic effects with analgesics and antidepressants.
- Personalized predictive models: Using neuroimaging and biomarkers to tailor individualized treatment.
- Accessibility improvements: Solutions to increase availability, including telemedicine-supported rTMS.
Clinical trials have begun addressing these gaps, such as a recent study focusing on neurocognitive outcomes post cardiac and spinal surgery, offering promising pathways to expanded applications (recent clinical trials on neurocognitive disorders). Integrative multidisciplinary approaches combining surgical advancements, neurorehabilitation, and neurostimulation technologies herald a new era for optimizing postoperative care.
Is rTMS painful or invasive?
rTMS is a non-invasive, painless procedure using magnetic fields generated by a coil on the scalp. It requires no anesthesia or surgery. Patients might feel mild facial muscle contractions but no significant discomfort.
When can I begin rTMS sessions after my spinal surgery?
Sessions typically start a few weeks post-surgery, aligned with wound healing and rehabilitation progress. Scheduling is personalized based on clinical evaluation.
What concrete benefits does rTMS offer after spinal surgery?
rTMS reduces persistent neuropathic pain, limits post-laminectomy syndrome, enhances motor recovery, and supports mental health including depression and anxiety post-operation.
Does rTMS replace physical rehabilitation sessions?
No, rTMS complements physical therapy by promoting cerebral plasticity, facilitating restoration of sensorimotor functions. It augments but does not replace physiotherapy.
How should I organize my post-surgery follow-up after treatment in France?
Neurothérapie Montréal provides full support in Quebec, working with SOS Tourisme Médical and Franchir for a seamless transition. Contact them through their designated channels for tailored evaluations.

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…




