
International Comparison: Spotlight on Spine Care Practices Between France and Quebec
November 30, 2025
Neck Surgery in Montreal: Maintain Natural Cervical Flexibility
November 30, 2025Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations, complicating recovery and diminishing quality of life. This persistent pain highlights the complex interplay of physiological healing, neural inflammation, and psychosocial factors that influence surgical outcomes. Recent research in 2025 emphasizes a multifaceted approach to prevention—integrating surgical precision, patient education, neuromodulation interventions, and coordinated rehabilitation. This holistic strategy aims not only to mitigate chronic pain but also to enhance overall patient well-being, revealing new frontiers in managing post-operative care through personalized protocols and advanced technologies.
Techniques such as repetitive transcranial magnetic stimulation (rTMS) have gained prominence in modulating neuropathic pain pathways and supporting psycho-emotional recovery following spinal operations. Collaboration across international medical teams and specialized centers, such as Neurothérapie Montréal, exemplifies the trend towards comprehensive care pathways extending from preoperative evaluation to home recovery. Parallel developments in minimally invasive laminectomy and motion-preserving surgical options reduce tissue trauma and decrease fibrotic complications, further preventing PLS. Today’s evidence converges around targeted interventions addressing inflammation, scar formation, mechanical rigidity, and patient-centric factors such as stress and depression, all of which contribute to the syndrome’s pathogenesis.
Understanding Post-Laminectomy Syndrome: Defining the Condition and Identifying Risk Factors for Pain Prevention
Post-Laminectomy Syndrome is characterized by persistent or recurrent back and radicular pain following spinal decompression surgery. Importantly, PLS does not necessarily indicate surgical failure; rather, it underscores the complexity of neuropathic pain and scar tissue formation after the procedure. The inflammation of nerve roots, excessive epidural fibrosis, postoperative mechanical stiffness, and poor vertebral fusion consolidation each independently contribute to pain persistence.
Neuropathic pain in PLS often manifests as allodynia or hyperalgesia, resulting from chronic nerve inflammation that sensitizes pain pathways. Scar tissue that forms around nerve roots can compress these sensitive structures anew, sparking recurrent symptoms. Mechanical rigidity, frequently due to impaired postoperative mobility, exacerbates discomfort by limiting spinal flexibility and aggravating nerve irritation. Furthermore, psychosocial factors — including anxiety, stress, and depressive symptoms — profoundly influence pain perception and the motivation to engage in rehabilitation programs. Addressing these dimensions early in the care continuum is pivotal for effective prevention.
- Chronic nerve inflammation: Elevates neuropathic pain severity and duration.
- Epidural fibrosis: Causes mechanical nerve compression leading to persistent symptoms.
- Postoperative stiffness: Limits mobility, increasing functional disability.
- Poor vertebral fusion: Delays spinal stabilization, prolonging recovery.
- Psychosocial stressors: Heighten pain sensitivity and reduce rehabilitation adherence.
Research insights stress the importance of comprehensive neurofunctional assessments preoperatively to identify individualized risks and tailor surgical and rehabilitative strategies. A comparative study from leading spinal research institutions illustrates that patients with optimized inflammatory and psychosocial profiles demonstrated significantly improved surgical outcomes and reduced incidence of PLS exploring detailed definitions and clinical implications.
| Risk Factor | Preventive Action | Expected Outcome |
|---|---|---|
| Chronic Inflammation | Anti-inflammatory therapies, Early rTMS | Reduced neuropathic pain intensity |
| Epidural Fibrosis | Minimally invasive surgery, Scar tissue monitoring | Lower recurrence of nerve compression |
| Mechanical Stiffness | Early and progressive physical therapy | Improved spinal mobility and function |
| Poor Bone Healing | Orthopedic follow-up, Nutritional support | Enhanced vertebral fusion rate |
| Psychosocial Factors | Psychological support, Neuromodulation | Better pain coping and therapy adherence |
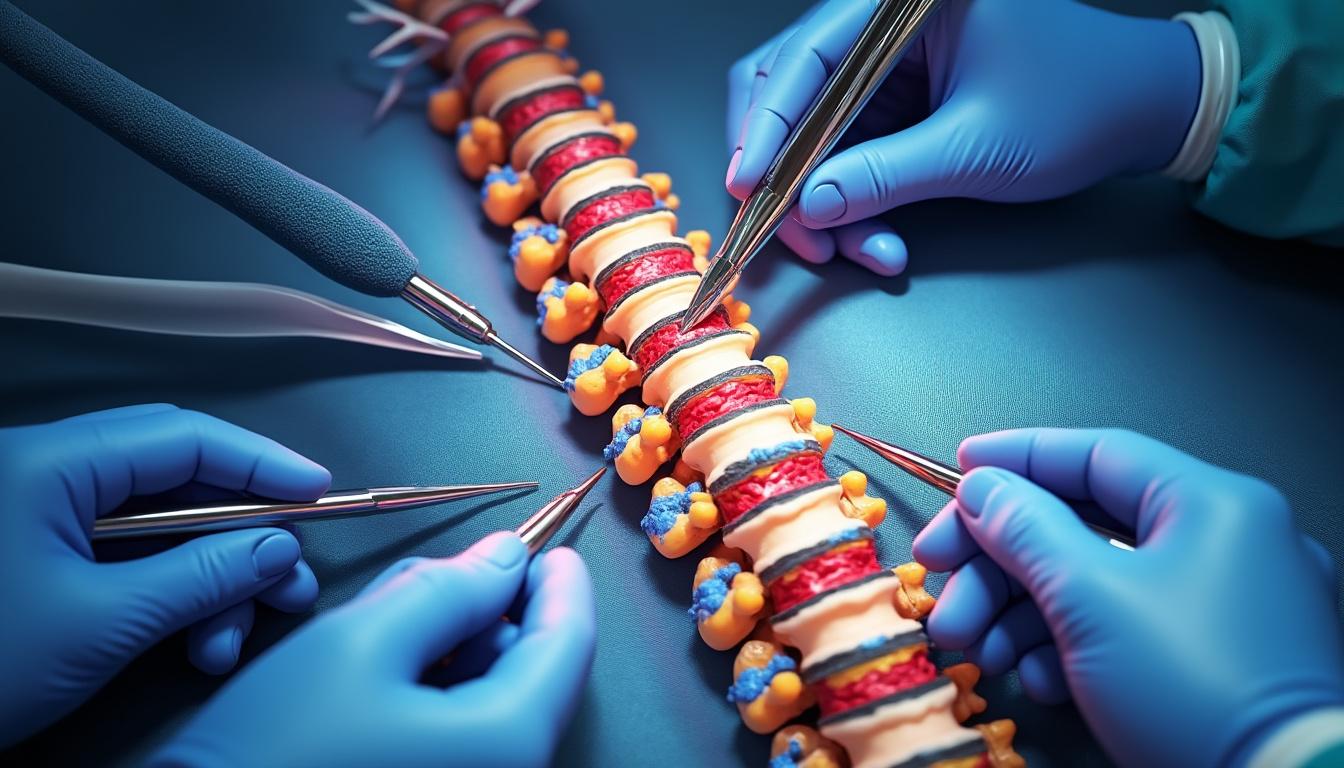

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…
Advancements in Surgical Techniques and Their Role in Minimizing Post-Laminectomy Syndrome
As spinal surgery evolves, technological and procedural innovations have significantly reduced tissue damage and postoperative complications. Minimally invasive laminectomy and motion-sparing surgeries such as dynamic stabilization have become increasingly common alternatives to traditional fusion methods. These techniques focus on preserving spinal anatomy and reducing scar formation, which are key contributors to postoperative chronic pain.
Studies report that patients undergoing endoscopic spine surgery experience a dramatic reduction in surgical trauma, blood loss, and hospital stays, factors which collectively decrease the incidence of post-laminectomy complications. The integration of advanced imaging and robotic navigation platforms in the operating room further enhances precision, allowing surgeons to exactly target the compressed nerve roots while sparing healthy tissues detailed reports on these surgical innovations.
- Endoscopic spinal decompression: Minimizes tissue disruption, reduces fibrosis.
- Robotic-assisted navigation: Enhances surgical accuracy and safety.
- Dynamic stabilization: Preserves spinal kinematics, less post-op stiffness.
- 3D intraoperative imaging: Facilitates optimal implant positioning.
For example, a comparative outcome analysis following minimally invasive versus open laminectomy showed a 30% reduction in PLS symptoms at six months post-surgery. This data signals a clear trajectory toward less invasive modalities coupled with precise perioperative monitoring and tailored rehabilitation protocols.
| Surgical Technique | Advantages | Impact on PLS Prevention |
|---|---|---|
| Endoscopic Laminectomy | Reduced scarring and faster recovery | Lower incidence of neuropathic pain |
| Robotic Navigation Systems | Increased precision and safety | Improved surgical outcomes |
| Dynamic Stabilization | Preserved motion, decreased stiffness | Enhanced functional rehabilitation |
| 3D Imaging | Optimized implant placement | Reduced mechanical complications |

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Neuromodulation Technologies in Postoperative Pain Prevention and Rehabilitation
Emerging neuromodulation therapies, particularly repetitive transcranial magnetic stimulation (rTMS), are gaining widespread acceptance for preventing the development of chronic neuropathic pain following spinal surgery. These non-invasive techniques influence brain circuits governing pain perception and mood regulation, alleviating neuropathic pain and concomitant psychological distress.
Clinical data reveal that integrating rTMS during postoperative recovery can reduce muscle spasms, enhance functional outcomes, and improve patient compliance with rehabilitation regimens. Centers like Neurothérapie Montréal actively implement rTMS alongside conventional care to mitigate adverse pain syndromes and accelerate neural plasticity processes for further insights on rTMS benefits.
- Modulates cortical excitability: Normalizes aberrant pain signaling pathways.
- Reduces neuropathic pain intensity: Targeted stimulation decreases hypersensitivity.
- Improves mood and anxiety: Addresses psychosocial components of chronic pain.
- Facilitates neuroplasticity: Supports functional neural circuit remodeling.
| Neuromodulation Technique | Therapeutic Goal | Observed Benefit |
|---|---|---|
| Repetitive Transcranial Magnetic Stimulation (rTMS) | Reduce neuropathic pain, support psychological health | Significant pain relief, mood stabilization |
| BrainPort Sensory Stimulation | Improve balance and sensorimotor coordination | Enhanced proprioception, better rehabilitation engagement |
| PoNS (Portable Neuromodulation Stimulator) | Boost neuroplasticity, accelerate functional recovery | Faster return to daily activities |
The broader integration of neuromodulation techniques within pain prevention protocols represents a paradigm shift in managing post-laminectomy challenges, aligning with patient-centered care and evidence-based practice.
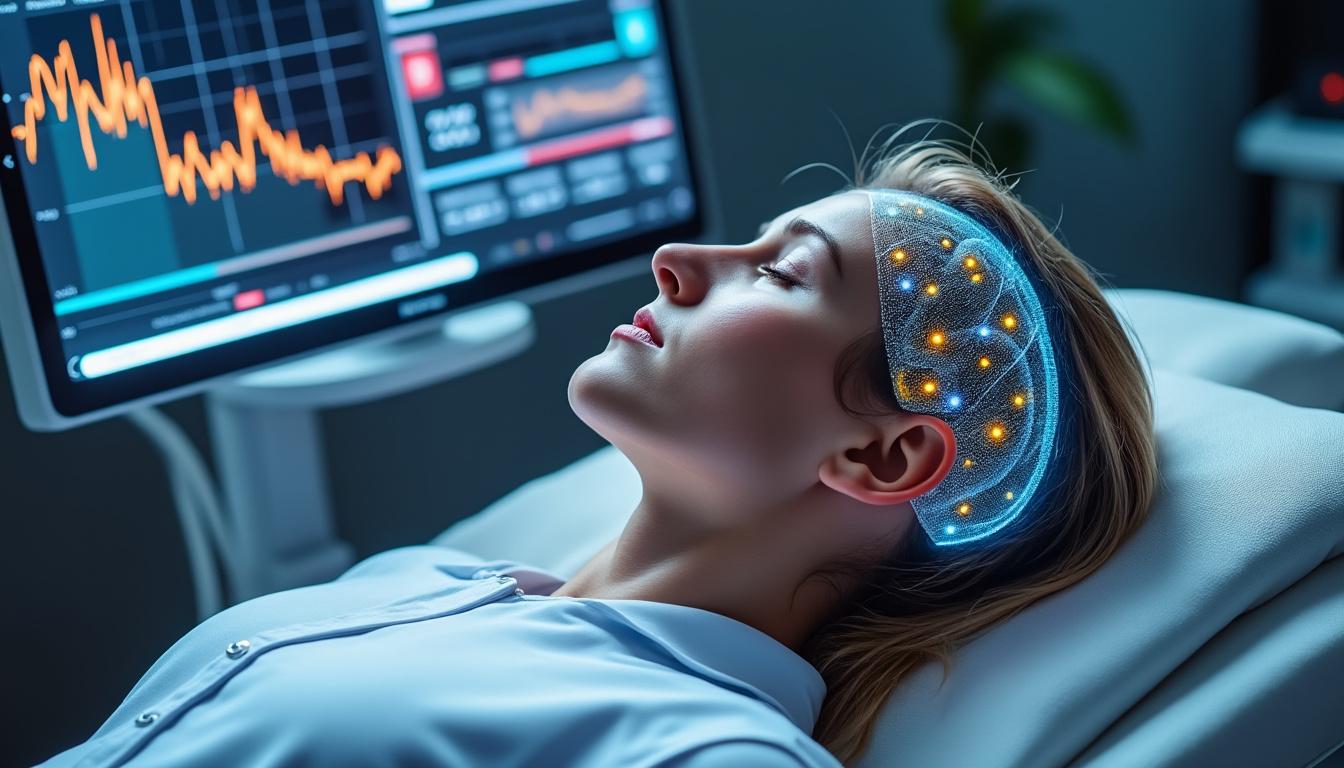

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…
Personalized Recovery Protocols: Tailoring Rehabilitation to Surgical Procedure and Patient Needs
Recovery trajectories significantly vary depending on the surgical approach, patient health status, and postoperative care quality. Coordinated rehabilitation programs customize physical therapy intensity and neuromodulation timing to the individual’s surgical procedure, such as a simple laminectomy, motion-sparing intervention, or vertebral fusion.
The rehabilitation pathway typically encompasses gradual mobilization, pain management, muscle strengthening, and psychosocial support to reduce chronic pain flare-ups. The critical window for initiating therapies like rTMS usually falls within the first three months post-surgery, fostering optimal neural recovery.
- Week 0-1: Relative rest, light walking, pain control.
- Weeks 2-4: Progressive physical therapy, low-impact movement.
- Months 1-3: Increased rehabilitation intensity, commencement of neuromodulation.
- After 3 months: Gradual return to normal activities and sports.
| Recovery Phase | Simple Laminectomy | Motion-Sparing Surgery | Vertebral Fusion |
|---|---|---|---|
| Weeks 0-1 | Rest, light activity | Rest plus early rTMS stimulation | Strict rest, intensive pain management |
| Weeks 2-4 | Increased walking, gentle therapy | Light activity with continued rTMS | Careful mobilization, close monitoring |
| Months 1-3 | Rehabilitation, work resumption | Strengthening, near-normal activity | Physiotherapy, gradual return |
| After 3 months | Full activity resumption | Normal activities without restrictions | Moderate physical activity, enhanced supervision |
Adherence to personalized rehabilitation protocols is essential to maximizing surgical outcomes and preventing the onset of chronic pain syndromes, turning patient education into a cornerstone of this process. Numerous studies support that active patient engagement and clear communication enhance compliance and shorten the convalescence period.

International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…
Implementing Multidisciplinary Coordination for Enhanced Patient Outcomes and Pain Prevention
Multidisciplinary care networks linking surgical teams, rehabilitation specialists, and psychological support providers have demonstrated significant impact in minimizing post-laminectomy syndrome prevalence. Such integration ensures prompt identification of risk factors, customized interventions, and continuous follow-up from hospital discharge to home settings.
International collaboration, such as the partnership among French surgical experts, Canadian neuromodulation specialists, and patient-oriented organizations like SOS Tourisme Médical, exemplifies effective coordination aimed at streamlining surgical logistics and postoperative care. This ensures patients benefit from innovative pain management techniques and receive clear guidance throughout recovery.
- Preoperative neurofunctional assessment: Tailors the surgical plan to patient-specific factors.
- Organized surgical travel: Reduces patient stress through logistical support.
- Postoperative neuromodulation and rehab monitoring: Enhances pain relief and functional recovery.
- Psychological support: Addresses anxiety and depression influencing pain perception.
| Service Provider | Role in Patient Care | Benefit to Patients |
|---|---|---|
| Franchir | Referral to expert surgeons, surgery logistics in France | Safe and streamlined surgical access |
| SOS Tourisme Médical | Patient information, administrative assistance | Clear patient guidance and reduced anxiety |
| Neurothérapie Montréal | Postoperative follow-up, neuromodulation treatment | Optimized recovery, chronic pain management |
Through coordinated multidisciplinary efforts, postoperative complications are substantially diminished, offering greater hope for patients facing PLS. Patients empowered with knowledge and supported by such networks report improved satisfaction and better long-term outcomes further exploring patient compliance and care transformation.

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
Patient Education and Practical Tips for Optimal Postoperative Recovery and Pain Prevention
Educating patients on their surgical procedure, expected recovery timeline, and pain prevention strategies is essential to reduce the incidence of post-laminectomy syndrome. Knowledgeable patients tend to participate more effectively in rehabilitation, recognizing early warning signs of complications and adhering to recommended activity modifications.
Common pitfalls such as premature physical exertion, neglecting neuropathic pain symptoms, or ignoring psychological stress can exacerbate recovery challenges. Therefore, patients are encouraged to follow a progressive activity schedule complemented by anti-inflammatory nutrition rich in omega-3 fatty acids and antioxidants.
- Maintain an anti-inflammatory diet: Incorporate leafy greens, nuts, and fish oil.
- Engage in gentle physical activities: Walking, yoga, and low-impact exercises.
- Attend recommended neuromodulation sessions: For sustained pain control.
- Communicate openly with care teams: Report new or worsening symptoms promptly.
Real-world patient stories emphasize these points. Jean, a 52-year-old golfer, experienced significant pain relief following a simple laminectomy combined with rTMS treatment and returned to his sport within five months. Marie, treated with motion-sparing surgery, regained endurance and work capacity in three and a half months, while Luc, after vertebral fusion, saw a reduction in neuropathic symptoms with neuromodulation support at seven months post-op. These examples confirm the importance of adherence to combined medical and rehabilitative strategies for sustainable outcomes.
| Patient | Type of Surgery | Benefit Observed | Recovery Duration |
|---|---|---|---|
| Jean | Simple laminectomy | Pain relief, return to golf | 5 months |
| Marie | Motion-sparing surgery | Improved endurance, resumed work | 3.5 months |
| Luc | Vertebral fusion | Reduced neuropathic pain with rTMS | 7 months |
These success narratives reinforce evidence from clinical studies on the impact of comprehensive prevention, specialized follow-up, and patient-centered care in reducing chronic pain syndromes.

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…
Emerging Research Directions: Focus on Epidural Fibrosis and Adjacent Segment Disease
Ongoing studies are investigating the role of abnormal epidural scarring and adjacent segment disease as central factors in post-laminectomy syndrome pathogenesis. Abnormal fibrosis can undermine neural decompression and perpetuate pain signals, while degeneration of spinal segments adjacent to surgical sites contributes to additional symptom burden.
Pioneering research prioritizes the development of pharmacotherapies to inhibit fibrosis formation after laminectomy and integrate regenerative techniques to preserve healthy disc and vertebral tissue. The synthesis of these approaches aims to address both mechanical and neurogenic components of persistent pain.
- Anti-fibrotic agents: Drugs targeting scar tissue formation and remodeling.
- Regenerative medicine: Stem cell and tissue engineering for spinal repair.
- Advanced imaging biomarkers: Early detection of adjacent segment degeneration.
- Multimodal treatment: Combining surgical, pharmacological, and rehabilitative strategies.
| Research Area | Objective | Potential Clinical Impact |
|---|---|---|
| Epidural Fibrosis Prevention | Reduce scar adhesion formation | Lower nerve re-compression risk |
| Adj Segment Disease Management | Preserve adjacent spinal segments | Decrease secondary degeneration |
| Pharmacotherapy Development | Effective anti-inflammatory and anti-fibrotic drugs | Improve long-term surgical outcomes |
| Tissue Engineering | Regenerative repair of spinal tissues | Restored spinal function |
New evidence in this domain is periodically reviewed in specialist forums and publications, contributing to evolving clinical guidelines focused on holistic prevention of post-laminectomy complications offering comprehensive surgical insights.

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…
Integration of International Clinical Protocols: A Model for Optimized Care Delivery
International partnerships and standardized clinical protocols facilitate sharing best practices in managing and preventing post-laminectomy syndrome. France and Canada exemplify such a model, where surgical expertise and neuromodulation-based postoperative care are combined into seamless care pathways.
Patients benefit from preoperative neurofunctional assessments, expertly coordinated surgical travel arrangements, and rigorous outpatient monitoring, supported by travel-medical organizations such as SOS Tourisme Médical and specialized surgical referral agencies like Franchir. This trend represents a future where global resources optimize access to expertise and novel rehabilitation options, reducing disparities in spinal surgery outcomes.
- Standardized preoperative evaluation: Facilitates targeted risk mitigation.
- Cross-border surgical coordination: Access to expert surgeons and facilities.
- Postoperative remote monitoring: Enhances early intervention and compliance.
- Telemedicine and patient education: Continuous support beyond hospital discharge.
| Component | Function | Benefit |
|---|---|---|
| Franchir | Chirurgical care coordination in France | Efficient surgical scheduling and logistics |
| SOS Tourisme Médical | Patient information and administrative support | Simplified process and enhanced patient readiness |
| Neurothérapie Montréal | Postoperative neuromodulation and follow-up | Improved pain management, faster recovery |
Infographic: Insights from Research on Preventing Post-Laminectomy Syndrome
Key Terms and Concepts
- Post-Laminectomy Syndrome – chronic pain occurring after back surgery.
- Chronic Pain – persistent pain lasting months or years.
- Neuropathic Pain – pain caused by nerve damage.
- Pain Management – strategies to alleviate pain symptoms.
- Rehabilitation – physical therapy post-surgery to restore function.
- Surgical Outcomes – results following spinal surgery.
- Pain Prevention – research efforts to reduce post-surgery pain.
- Patient Education – informing patients on managing expectations and recovery.
Research Insights Overview
Select a term above to see detailed research insights.
Key Statistics of Post-Laminectomy Syndrome
Data source: Public Research API
Can Post-Laminectomy Syndrome be completely prevented?
Though not all complications can be entirely avoided, rigorous preparation and specialized follow-up significantly reduce the risks.
What is the typical duration for recovery after laminectomy?
Recovery varies by procedure, usually 4 to 6 weeks for light activities and several months for complete healing.
How does repetitive transcranial magnetic stimulation (rTMS) aid post-spinal surgery?
rTMS modulates brain circuits involved in pain and emotion, effectively reducing neuropathic pain and post-operative stress.
When can patients safely resume sports after surgery?
Sports should be resumed gradually under medical supervision, often several months post-operation, starting with gentle activities such as swimming.
What roles do SOS Tourisme Médical and Franchir play?
SOS Tourisme Médical supports patients with information and administrative processes, while Franchir manages surgical referrals and logistic arrangements.

What Research Reveals About Rehabilitation and Returning to Work
Rehabilitation and the process of returning to work form a complex interplay that extends far beyond physical recovery. It is a multifaceted journey involving medical treatment, psychological adaptation, workplace accommodation, and social reintegration. Research in recent years underscores the profound…




