Saint-Eustache Herniated Disc Relief After Failed Physiotherapy
November 2, 2025
Understanding Disc Herniation in the Southwest: The Top 3 Warning Signs and Neurovertebral Decompression Treatments
November 3, 2025The prevalence of lumbar disc herniation in the Gouin district has led to a growing need for targeted, effective treatment strategies. This spinal condition, known for causing severe pain and mobility issues, affects many residents, significantly impacting their daily lives and work productivity. Advances in contemporary non-invasive treatments are reshaping care paradigms, especially with technologies like neurovertebral decompression offering promising outcomes. Grounded in precise localization of affected spinal zones, these therapies prioritize patient-specific protocols, optimizing recovery and functional restoration. In Gouin, where access to multidisciplinary care and innovative equipment converges, patients find renewed hope through comprehensive evaluations and tailored management plans. Under the expert guidance of Dr. Sylvain Desforges, renowned for pioneering spinal care innovations, management pathways for lumbar disc herniation thoughtfully integrate clinical rigor, ethical standards, and technology-enabled interventions to maximize patient safety and efficacy.
Understanding the complex interplay between spinal anatomy, patient symptomatology, and the biomechanics of herniated discs allows practitioners in Gouin to custom-design decompression treatments. Such an approach ensures that therapeutic energy is delivered precisely to areas identified by sophisticated diagnostics such as MRI and clinical assessment. This chapter discusses the evolution of lumbar disc herniation care, the significance of aligned therapy zones, and how neurovertebral decompression serves not only to relieve symptoms but to foster tissue regeneration and improve long-term spinal health. Additionally, insights into multidisciplinary care coordination, including physiotherapy and osteopathic support, shed light on the holistic patient journey.
Precise Targeting of Herniated Disc Zones in Gouin: Clinical and Radiological Criteria
Accurate identification of the affected vertebral segments is foundational to successful neurovertebral decompression therapy. In Gouin, patients with lumbar disc herniation often present with pain localized at the lumbar or cervical regions, necessitating a meticulous diagnostic pathway that combines in-depth patient history with state-of-the-art imaging techniques. The clinical evaluation managed by Dr. Sylvain Desforges extensively records pain characteristics such as radiation patterns, intensity, and associated neurological symptoms including radiculopathy or muscle weakness.
Magnetic Resonance Imaging (MRI) remains the gold standard to visualize herniated material and its nerve impingement effects. The nuanced classification of disc herniations—protrusive, extrusive, or sequestrated—guides the customization of decompression protocols, ensuring that mechanical unloading is directed where it will be most beneficial. Key factors that shape treatment targeting include:
- Hernia type and size: Larger extrusions may require different therapeutic parameters compared to smaller protrusions.
- Symptom distribution: Radiating sciatic pain versus localized lumbar discomfort influences session targeting.
- Vertebral segments most affected: The L4-L5 and L5-S1 levels are primary culprits in lumbar herniation, dictating decompression focus.
- Surrounding tissue health: Assessment of inflammation and tissue degeneration factors into session intensity and duration.
By combining these clinical and radiological insights, practitioners develop an evidence-based, patient-centric decompression plan. This methodology is aligned with rigorous standards set forth by the Collège des médecins du Québec, reflecting Dr. Desforges’ commitment to scientific integrity.
| Targeted Spinal Zone | Common Symptoms | Therapeutic Focus |
|---|---|---|
| L4-L5 and L5-S1 (Lumbar) | Sciatica, lower back pain, muscle weakness in lower limbs | Segmental traction with adjustable harness, precise inclination angles |
| C5-C6 and C6-C7 (Cervical) | Arm pain, numbness, cervicogenic headaches | Positioning in seated or supine, segment-specific traction force modulation |
| Thoracic (Less common) | Intercostal pain, pelvic radiation | Postural therapy combined with focused decompression protocols |
This targeted strategy ensures maximized efficacy in reducing nerve root pressure and promoting recovery of affected tissues. Patients benefit not only from symptom relief but also from improved spinal stability, which reduces the risk of recurrence.


Disc herniation remains a prevalent and challenging spinal disorder, significantly affecting individuals’ quality of life, particularly in communities like Sainte-Julie. Characterized by a rupture or protrusion of the disc nucleus through the fibrous ring, this condition compresses adjacent nerve roots,…
Biomechanical Foundations of Neurovertebral Decompression in Lumbar Disc Herniation
Neurovertebral decompression therapy is grounded in biomechanical principles designed to neutralize excessive intradiscal pressure, a critical factor in lumbar disc herniation. The excess pressure squeezes the nucleus pulposus through weakened annular fibers, compressing adjacent neural structures and causing pain, inflammation, and neurological dysfunction.
During therapy, sophisticated computer-controlled traction devices apply segmental spinal distraction, creating negative pressure within the disc space. This intra-discal vacuum effect facilitates the retraction of herniated material and encourages fluid and nutrient ingress essential for cellular repair. The therapy further promotes blood circulation around the vertebrae, accelerating anti-inflammatory processes and tissue regeneration.
- Controlled traction precision: Tailored forces prevent damage while maximizing decompression efficacy.
- Negative intradiscal pressure creation: Mechanically withdraws herniated disc components away from nerve roots.
- Disc rehydration: Restoration of disc height and elasticity supports mechanical function.
- Stimulation of vascular flow: Enhanced circulation aids detoxification and repair.
- Reduction of inflammation mediators: Lower neuropeptide levels alleviate chronic pain pathways.
| Biomechanical Parameter | Therapeutic Effect | Impact on Patient |
|---|---|---|
| Segmental Traction Control | Reduces intradiscal pressure | Decreases nerve root compression, alleviates pain |
| Vacuum Effect | Retracts disc herniation | Reduces radiating pain and neurological symptoms |
| Fluid Resupply | Disc rehydration and nutrient delivery | Improves mobility and flexibility over time |
| Enhanced Circulation | Promotes tissue repair and detox | Facilitates sustainable functional recovery |
The precision and control enabled by advanced devices, such as those employed at TAGMED clinics, allow practitioners to tailor sessions perfectly to each patient’s spinal condition. Consequently, the risks of overextension or insufficient decompression are minimized, making this a safe alternative for many patients intolerant of surgery.

IntraSPINE® in Sherbrooke: Protecting and Enhancing Lumbar Function
The prevalence of chronic low back pain has surged globally, profoundly impacting individuals’ quality of life and productivity. Sherbrooke, Quebec, exemplifies this widespread challenge, with numerous patients seeking effective and sustainable relief from lumbar discomfort. Addressing this urgent need, the…
Clinical Benefits of Neurovertebral Decompression for Gouin’s Lumbar Disc Herniation Patients
Patients in Gouin seeking relief from lumbar disc herniation experience numerous clinical advantages through neurovertebral decompression. This approach is especially relevant in comparison to conventional pharmacological and invasive options, which often carry undesirable side effects or risks.
A concise overview of the key benefits includes:
- Effective pain relief: Progressive reduction of nerve compression translates to decreased pain intensity and frequency.
- Functional restoration: Patients regain mobility and reduce stiffness, enabling return to work and daily activities.
- Customized intervention: Therapy is adapted to the individual disc pathology and patient tolerance.
- Non-invasive nature: Absence of surgery eliminates risks like infection, anesthesia complications, or prolonged hospitalization.
- Reduction in medications: Decreased reliance on analgesics and anti-inflammatory drugs minimizes potential adverse effects.
- Integration with complementary therapies: When paired with osteopathy or kinésithérapie, results reinforce.
| Advantage | Detailed Description | Patient Outcome |
|---|---|---|
| Safety | Non-invasive treatment without anesthesia or incisions | Minimized complication rates and outpatient care |
| Personalization | Protocols tailored to hernia type and severity | Improved efficacy and patient comfort |
| Proven effectiveness | Clinical studies report up to 86% patient improvement rates | Enhanced quality of life and functional independence |
Beyond tangible symptom relief, neurovertebral decompression holds preventive value by strengthening vertebral segments and promoting proper posture, thereby lowering the likelihood of recurrence. Its adaptability to various patient needs makes it a preferred treatment at leading clinics in Gouin, like the TAGMED Centers. The therapy aligns with evolving evidence-based protocols found in recent studies on lumbar disc herniation emphasizing conservative yet effective treatments.
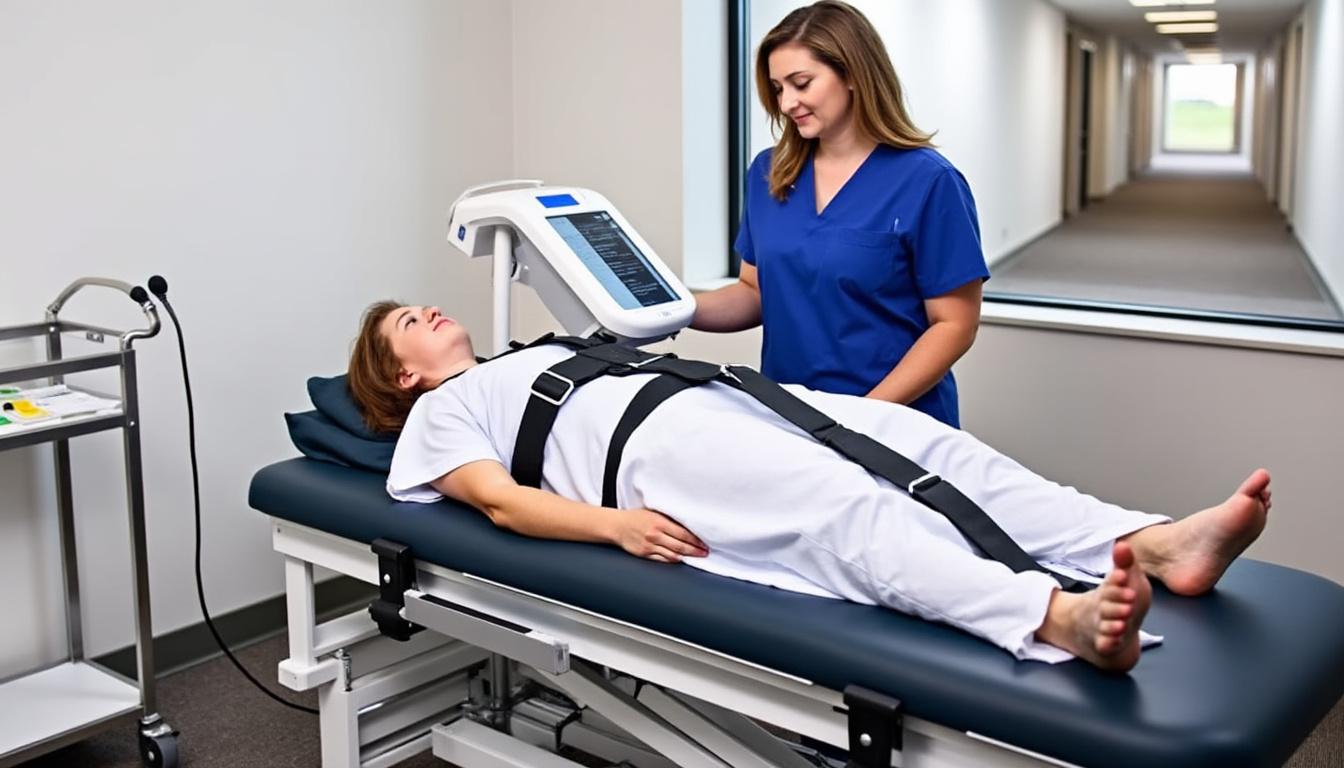
Detailed Neurovertebral Decompression Treatment Protocol Practiced in Gouin Clinics
Therapeutic efficacy depends greatly on the structure and execution of decompression treatment sessions. In Gouin’s specialized facilities, protocols blend state-of-the-art technology with close practitioner oversight. Under Dr. Sylvain Desforges’ expertise, every session is crafted to meet individual patient anatomy and symptom profiles.
The treatment process unfolds through several key phases:
- Initial consultation: Clinical exam coupled with functional and imaging assessments to personalize the approach.
- Patient installation: Comfort and safety ensured with adjustable harnesses and automated spinal traction tables.
- Active decompression: Precise computerized traction induces segmental spinal distraction for 20–30 minutes.
- Post-session care: Recovery guidelines provided alongside therapeutic exercises to consolidate gains between sessions.
| Phase | Typical Duration | Clinical Objective |
|---|---|---|
| Evaluation | 30 to 45 minutes | Accurate diagnosis and individualized treatment planning |
| Setup | 5 to 10 minutes | Optimized positioning for effective therapy delivery |
| Decompression | 20 to 30 minutes | Gradual traction application to relieve disc pressure |
| Recovery | 10 to 15 minutes | Guidance on exercises and lifestyle for stabilization |
A typical regimen consists of 20 to 25 sessions spread over approximately 4 to 6 weeks. This pacing is essential to foster cumulative disc healing while minimizing risks of treatment-related discomfort or stress.
Multidisciplinary Approach Integration to Optimize Patient Outcomes in Gouin
Long-term success in managing lumbar disc herniation demands an integrated, multidisciplinary framework. Neurovertebral decompression acts as a central component, complemented by physical therapy, osteopathic treatment, ergonomic education, and psychological support where needed.
- Physiotherapy: Muscle strengthening and proprioceptive retraining reduce compensatory strain and improve posture.
- Osteopathy and chiropractic care: Manual therapies improve joint mobility and spinal alignment.
- Ergonomic guidance: Patient education to adapt daily activities and maintain spinal health.
- Psychological support: Addressing anxiety and chronic pain coping mechanisms fosters adherence and well-being.
| Discipline | Therapeutic Role | Combined Patient Benefit |
|---|---|---|
| Physiotherapy | Targeted muscle rehabilitation | Improved spinal support and prevention of recurrence |
| Chiropractic Care | Spinal realignment and tension release | Enhanced mobility and overall comfort |
| Ergonomic Counseling | Activity modification and body mechanics education | Reduction of mechanical stress on the spine |
| Psychological Support | Emotional coping and pain management | Improved treatment adherence and quality of life |
Collaborations between neurovertebral decompression centers and allied specialists reinforce the safety and comprehensiveness of care, optimizing patients’ chances for sustained improvement.
Essential Contraindications to Neurovertebral Decompression Therapy in Gouin
While neurovertebral decompression is a valuable treatment, specific health considerations must preclude its use to ensure patient safety. Dr. Sylvain Desforges adheres strictly to contraindication guidelines derived from clinical evidence and regulatory directives.
Key contraindications include:
- Severe osteoporosis or osteomalacia: Fragile bones increase fracture risk under traction.
- Recent or unstable vertebral fractures: Therapy stress could exacerbate injuries.
- Advanced spondylolisthesis or spondylolysis: Mechanical instability contraindicates decompression forces.
- Presence of spinal instrumentation: Hardware like pins or plates may be destabilized.
- Active spinal infections or malignancies: Traction may worsen pathological conditions.
- Severe neurological impairments: Conditions such as cauda equina syndrome require urgent surgical attention.
- Pregnancy: Safety data are insufficient, so therapy is deferred.
| Condition | Risk Associated With Decompression | Recommended Action |
|---|---|---|
| Severe Osteoporosis | Heightened fracture risk | Avoid decompression; consider alternative treatments |
| Active Infection | Spread or aggravation of infection | Treat infection fully before any decompression |
| Pregnancy | Potential risk to fetus | Delay treatment until after childbirth |
| Severe Neurological Conditions | Potential neurological worsening | Immediate referral for surgical or emergency care |
Such precautionary protocols, combined with rigorous patient assessments, uphold the highest standards of care at the TAGMED facilities, ensuring that therapy is only administered when benefits outweigh risks.
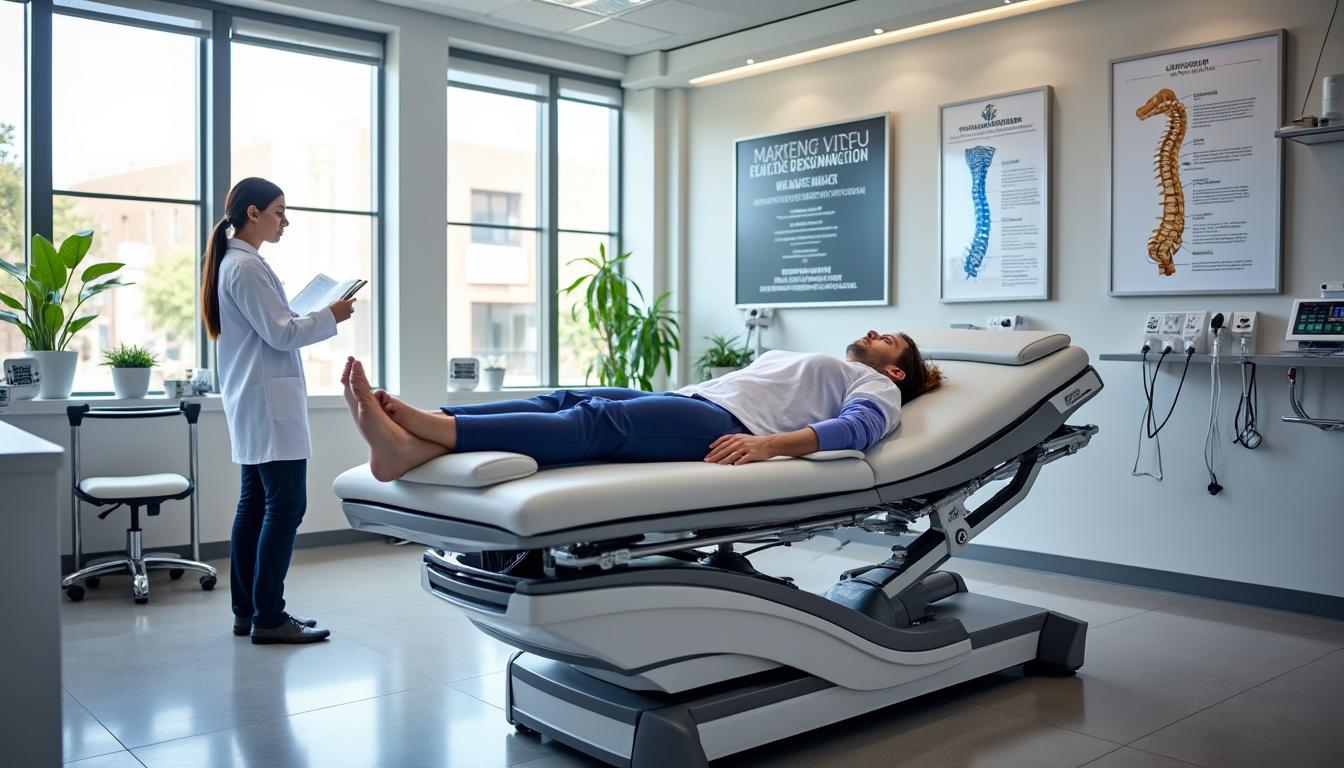
Cutting-Edge Technology Empowering Neurovertebral Decompression in Gouin
Technological innovation is paramount in advancing neurovertebral decompression outcomes. The clinics in Gouin, featuring TAGMED among their leaders, utilize the latest traction systems equipped with computerized feedback loops and precision adjustment software to adapt therapy dynamically to patient responses.
Core technological assets include:
- Computer-assisted segmental traction: Continuously modulates force for optimal decompression without causing discomfort.
- Biometric sensors: Monitor patient physiological responses ensuring safety and effectiveness during sessions.
- Advanced 3D imaging integration: Linkage with MRI allows millimeter-precise targeting of herniation zones.
- Ergonomic harness and tables: Provide patient stability and comfort, reducing muscular strain and anxiety.
Such integrative technology combined with the clinical expertise of Dr. Desforges offers patients unparalleled care quality, aligning with evolving international standards in spine care as supported by studies from several research articles, including the comprehensive reviews found on Pain Physician and MDPI Journal of Clinical Medicine.
The dynamic neighborhood of Mercier–Hochelaga-Maisonneuve has seen a significant rise in cases of herniated disc-related back pain, with many residents facing chronic discomfort that interferes with work and daily activities. This ailment, which involves displacement or protrusion of spinal discs,…
Strategies for Effective Post-Treatment Follow-Up after Neurovertebral Decompression
Ensuring lasting therapeutic benefits after completing decompression therapy involves a structured follow-up program emphasizing reinforcement, prevention, and monitoring. The collaborative care teams in Gouin emphasize patient education, adherence to exercise regimens, and regular reassessment.
The key elements include:
- Structured exercises: Personalized routines to strengthen spinal stabilizer muscles and enhance endurance.
- Postural coaching: Guidance on ergonomic behaviors and daily activity adjustments to reduce mechanical stress.
- Periodic clinical evaluations: Scheduled appointments to promptly detect any signs of recurrence or new symptoms.
- Multidisciplinary engagement: Integration with chiropractic, osteopathy, and physiotherapy providers for ongoing support.
| Follow-up Component | Main Objective | Impact on Patient |
|---|---|---|
| Regular Exercise | Maintain muscle strength and spinal stability | Lower risk of symptom recurrence and injury |
| Ergonomic Advice | Reduce harmful spinal loading | Improved comfort in daily tasks |
| Scheduled Evaluations | Early detection of relapse | Timely intervention to maintain health |
| Holistic Multidisciplinary Care | Comprehensive support | Long-term patient satisfaction and outcomes |
Consistent post-treatment programs greatly reduce the risk of reverting to painful symptoms, underscoring the importance of continued patient engagement alongside their healthcare teams.
Future Directions and Evolving Trends in Lumbar Disc Herniation Management in Gouin
The management of lumbar disc herniation continues to evolve, driven by multidisciplinary research and technological breakthroughs. Gouin remains a hub of spinal care innovation, drawing on the expertise of Dr. Sylvain Desforges and advanced facilities.
Promising developments include:
- Combination therapies: Integration of laser therapy with decompression to enhance cellular regeneration as seen in systems like Smart Laser Therapy.
- Personalized AI-driven protocols: Utilizing artificial intelligence to tailor treatment intensities based on patient-specific biological feedback.
- Telemedicine and remote monitoring: Allowing continuous support and adjustments without demanding frequent clinic visits.
- Advanced dynamic spinal implants: Offering complementary solutions where conservative measures require surgical supplementation.
| Innovation | Expected Impact | Status in Gouin |
|---|---|---|
| Laser-assisted Decompression | Accelerated tissue repair and pain relief | Emerging collaborations with local clinics |
| AI Treatment Customization | Optimized session efficacy and patient comfort | Under research and early implementation |
| Telehealth Follow-up | Enhanced patient accessibility and compliance | Integration in clinic practices |
These forward-thinking approaches embody the philosophy Dr. Desforges champions—an evidence-based, compassionate, and cutting-edge spinal care model offering patients renewed autonomy and relief.
What types of lumbar disc herniations can neurovertebral decompression treat effectively?
Neurovertebral decompression is effective mainly for protrusive, extrusive, and some sequestrated herniations, especially at lumbar levels L4-L5 and L5-S1. Cases requiring surgical opinions include severe neurological deficits or spinal instability.
Is neurovertebral decompression safe for active individuals or athletes?
Yes, this treatment is well-suited for athletes. Its targeted and non-invasive nature allows for rapid symptom relief and facilitates quicker return to physical activity.
How many treatment sessions are generally required to see meaningful improvement?
A protocol of approximately 20 to 25 sessions spread over 4 to 6 weeks typically yields substantial and lasting results. Session intensity and frequency are adjusted for individual tolerance.
Are there any discomforts associated with the decompression therapy sessions?
Most patients report the therapy as comfortable or even relaxing. The system is designed to avoid excessive strain, and real-time monitoring ensures patient comfort throughout the session.
What are the main contraindications for neurovertebral decompression?
Contraindications include severe osteoporosis, recent fractures, active spinal infections or malignancies, advanced spinal instability, pregnancy, and serious neurological conditions such as cauda equina syndrome. Comprehensive evaluation prior to treatment helps identify these risks.