Vaudreuil-Dorion Herniated Disc Success Stories from TAGMED
November 20, 2025
Post-Operative Care After Back Surgery: A Comprehensive Guide for Quebec Patients
November 21, 2025In the vibrant borough of Rosemont–La Petite-Patrie, many individuals face the persistent challenge of back pain often linked to herniated discs. This condition, while common, raises numerous questions regarding available therapies and effective pain management strategies. The increasing interest in neurovertebral decompression as a non-surgical alternative reflects a growing trend toward treatments that respect natural spinal physiology while leveraging cutting-edge technology. As thousands navigate the complex terrain of spinal healthcare, understanding the nuances of treatment options is imperative for those seeking relief without resorting immediately to invasive surgery.
This comprehensive exploration focuses on the current state of spinal treatment in Rosemont–La Petite-Patrie, detailing the anatomy and implications of herniated discs, the principles of neurovertebral decompression, and the multidisciplinary care approach championed by leading experts like Dr. Sylvain Desforges. By weaving clinical insights with patient-centered education, the content highlights pathways for back pain relief that emphasize scientific rigor and personalized care. The article also outlines how international coordination enhances patient journeys and access to innovative therapies not always available locally.
Understanding Herniated Discs in Rosemont–La Petite-Patrie: Anatomy, Causes, and Symptoms
The backbone of spinal health lies in the complex structure of the vertebral column, comprising stacked vertebrae separated by intervertebral discs designed to absorb shock and facilitate flexible movement. When these discs sustain damage, the resulting protrusion of the gelatinous core through the annulus fibrosus constitutes a herniated disc. This condition can exert pressure on nearby spinal nerves, resulting in pain and neurological symptoms.
In Rosemont–La Petite-Patrie, herniated discs predominantly affect the lumbar region, manifesting as localized lower back pain often radiating as sciatica. However, cervical and thoracic herniations, though less frequent, also bring distinct challenges. Typical symptoms include:
- Localized or radiating back pain such as sciatica or cervico-brachial neuralgia
- Numbness or tingling sensations extending into limbs
- Muscle weakness when nerve compression is significant
- Reduced mobility and spinal stiffness
Equally important is recognizing that not all herniated discs cause symptoms; numerous imaging studies reveal asymptomatic cases, which underscores the need for careful clinical correlation before initiating treatment. Understanding these distinctions is essential to customizing care plans in a patient-focused setting.
| Type of Hernia | Common Location | Typical Symptoms | Recommended Treatments |
|---|---|---|---|
| Lumbar Herniated Disc | Lower back (L4-L5, L5-S1) | Lower back pain, sciatica, numbness | Neurovertebral decompression, physiotherapy, medication |
| Cervical Herniated Disc | Neck (C5-C6, C6-C7) | Neck pain, cervico-brachial neuralgia, stiffness | Neurovertebral care, osteopathy, targeted exercises |
| Thoracic Herniated Disc | Mid-back (rare) | Thoracic pain, sometimes radiating | Observation, decompression if indicated |
By comprehensively documenting these scenarios, practitioners in the borough and beyond can better assess patient needs and develop evidence-based plans consistent with the latest scientific recommendations.
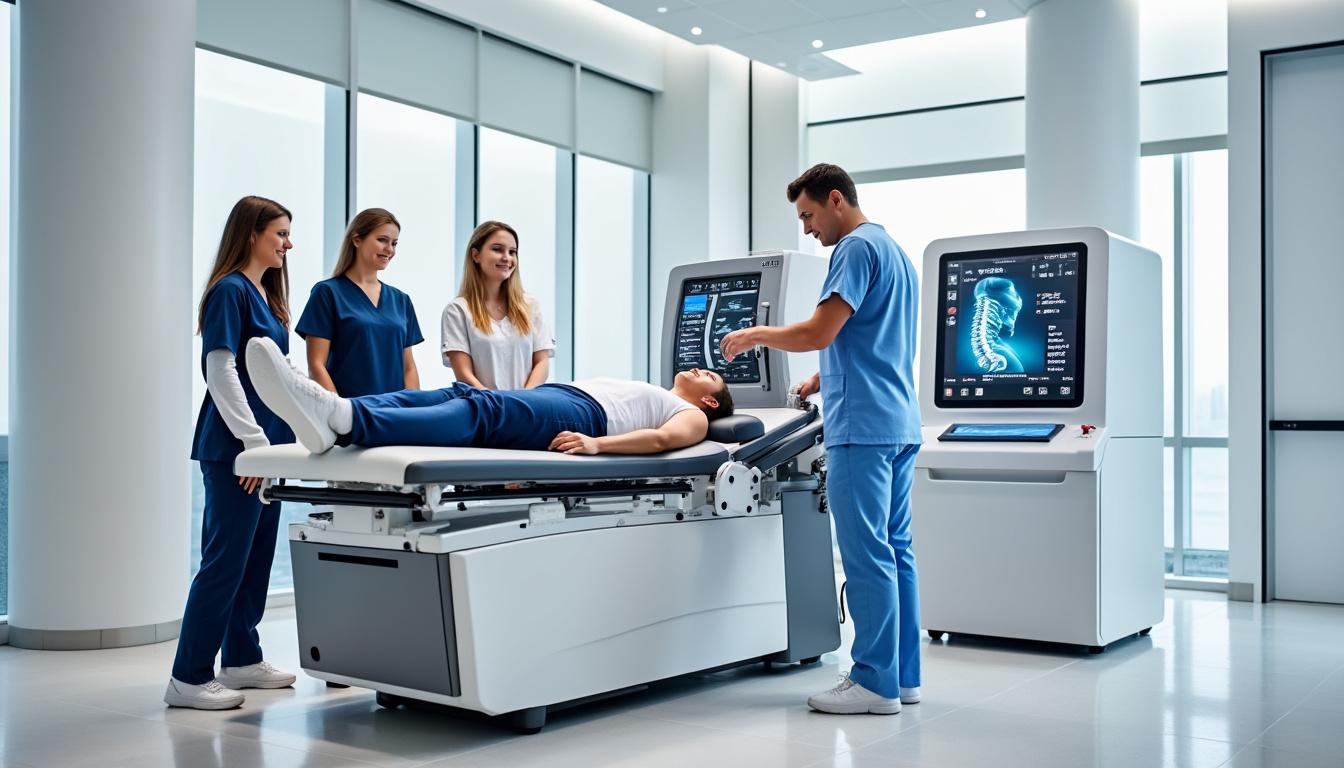

Disc herniation remains a prevalent and challenging spinal disorder, significantly affecting individuals’ quality of life, particularly in communities like Sainte-Julie. Characterized by a rupture or protrusion of the disc nucleus through the fibrous ring, this condition compresses adjacent nerve roots,…
Neurovertebral Decompression: Core Principles and Mechanisms for Herniated Disc Relief
At the forefront of non-invasive back pain solutions, neurovertebral decompression employs controlled spinal traction to alleviate pressure on affected discs and nerve roots. This technique, offered extensively at the TAGMED Clinic in Rosemont–La Petite-Patrie, involves multiple treatment sessions with patients comfortably positioned on specialized decompression tables tailored to their unique anatomical needs.
The mechanism underlying this therapy is twofold: First, the application of intermittent, gentle traction expands the intervertebral space, easing nerve compression. Second, this process facilitates rehydration of the disc nucleus, promoting a natural rebalance and reduction of disc protrusions. Patients commonly experience:
- Significant reduction in back and radiating nerve pain
- Decreased local inflammation and improved blood flow
- Gradual restoration of spinal mobility
- Postural correction and muscular strengthening preventing future episodes
Each session includes carefully monitored stages:
| Session Phase | Action | Expected Outcome |
|---|---|---|
| Patient Positioning | Supine on decompression table, precise adjustments | Optimal comfort and targeted spinal segment focus |
| Traction Application | Intermittent traction with controlled force | Expansion of intervertebral space and disc decompression |
| Recovery Phase | Gradual release, complemented by manual relaxation techniques | Muscle relaxation and enhanced circulation |
This modality, while promising, must be integrated within a broader therapeutic strategy, frequently coupled with osteopathic treatments for optimized spinal health and functionality. Interested readers can further explore this resource on spinal decompression therapy for detailed insights about its indications and outcomes.

IntraSPINE® in Sherbrooke: Protecting and Enhancing Lumbar Function
The prevalence of chronic low back pain has surged globally, profoundly impacting individuals’ quality of life and productivity. Sherbrooke, Quebec, exemplifies this widespread challenge, with numerous patients seeking effective and sustainable relief from lumbar discomfort. Addressing this urgent need, the…
Comprehensive Care in Rosemont–La Petite-Patrie: Integrating Osteopathy and Rehabilitation
Managing herniated discs demands more than isolated decompression sessions; the approach must be multidisciplinary, combining manual therapies, therapeutic exercises, and patient education. The leading expert Dr. Sylvain Desforges has pioneered such integrative care at TAGMED Clinic, emphasizing the synergy of neurovertebral decompression with osteopathy and physiotherapy.
Osteopathic care primarily aims to restore joint mobility and relieve muscular tension, addressing secondary imbalances caused by the herniation. Physiotherapy complements this by focusing on muscle strengthening, postural education, and gradual reconditioning to ensure the spine remains stable and functional over time.
- Osteopathy: Weekly manual therapy sessions targeting vertebral and soft tissue mobilization
- Neurovertebral Decompression: Multiple weekly sessions to reduce nerve pressure
- Physiotherapy & Rehabilitation: Daily exercises for muscle strengthening and flexibility, supported by professional guidance
| Treatment Modality | Objectives | Recommended Frequency |
|---|---|---|
| Neurovertebral Decompression | Reduce nerve compression, expand disc space | 2-3 sessions per week initially |
| Osteopathic Therapy | Restore vertebral mobility, relax muscles | 1 session weekly |
| Rehabilitation Exercises | Muscle strengthening, posture improvement | Daily, with supervised follow-ups |
Such a holistic protocol aligns with scientific best practices and patient safety standards, ensuring durable improvements and minimizing the risk of symptom recurrence. The important role of personalized care cannot be overstated, as each patient has unique triggers and recovery timelines.
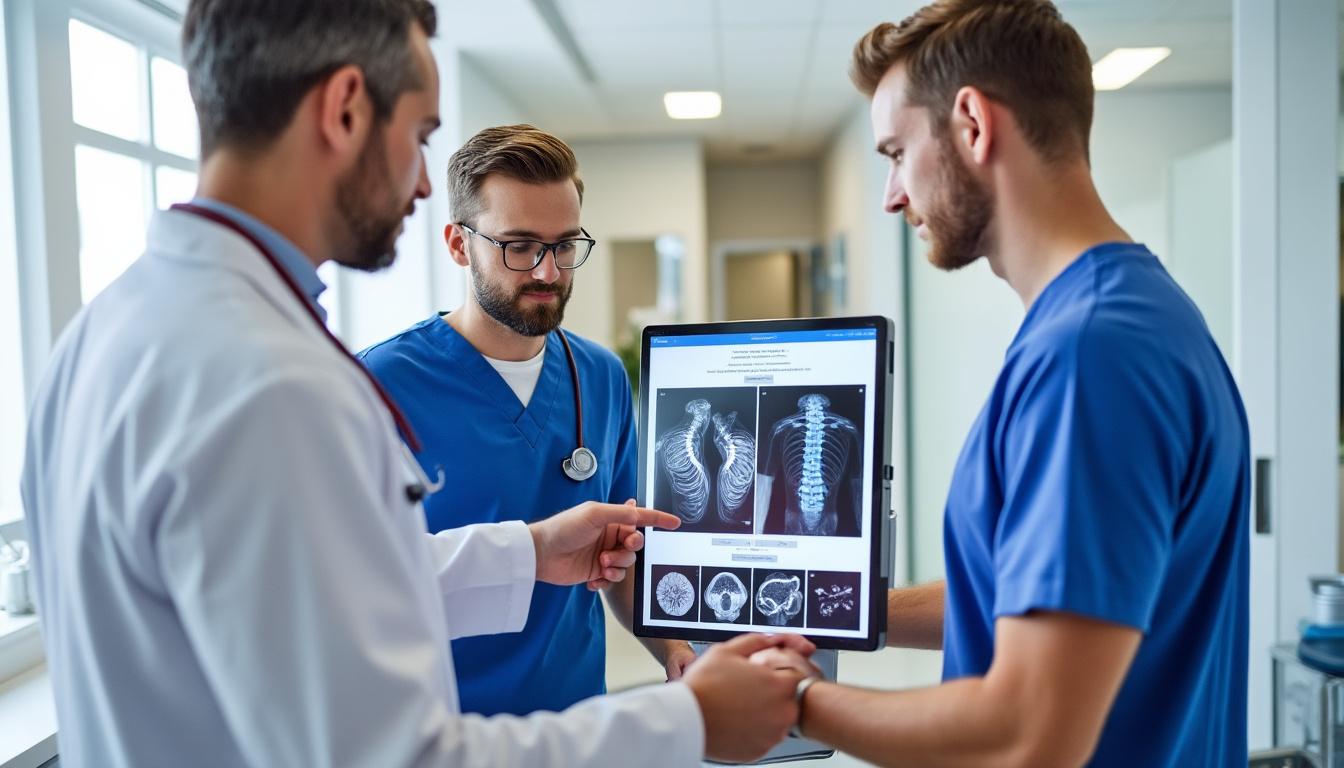
Precision Diagnostics in Rosemont–La Petite-Patrie: Identifying Ideal Candidates for Decompression Therapy
Effective neurovertebral decompression hinges on accurate patient selection. The TAGMED Clinic utilizes comprehensive diagnostic protocols combining clinical examination and advanced imaging like MRI scans to elucidate the hernia’s characteristics and the extent of neural compression.
Key criteria guiding eligibility for decompression include:
- Presence of disc-related pain without severe neurological deficits
- No signs of cauda equina syndrome
- Insufficient response to conservative treatments such as medication and rest
- Patient engagement and ability to adhere to treatment protocols
| Eligibility Criteria | Appropriate for Decompression | Contraindications |
|---|---|---|
| Moderate to severe pain | Yes | No |
| Severe neurological complications | No | Yes (e.g., weakness, cauda equina syndrome) |
| MRI-confirmed herniated disc | Yes | No |
| Ability to participate actively in therapy | Yes | No |
This diagnostic rigor reflects Dr. Sylvain Desforges’ commitment to evidence-based and ethical practice aligned with Quebec medical regulations. By exercising stringent patient selection, the risks of delayed surgical intervention or inappropriate treatment are minimized, preserving patient safety and optimizing outcomes. For further reading on diagnosis and treatment strategies, the Mayo Clinic’s resource on herniated disks offers valuable perspectives.
Weighing Alternatives and Limitations: When Decompression May Not Suffice
Despite its benefits, neurovertebral decompression is not universally effective. Advanced herniations, severe neurological impairment, or certain complications may necessitate alternative interventions. In Rosemont–La Petite-Patrie, the multidisciplinary teams ensure prompt referral to specialists when surgical options, such as minimally invasive discectomy, become necessary.
Other treatment alternatives include:
- Medications: Analgesics and anti-inflammatory drugs for symptomatic relief
- Epidural injections: To reduce localized inflammation
- Physical therapy: Manual techniques or structured rehabilitation programs
- Surgical interventions: Reserved for refractory or complicated cases
| Treatment | Indications | Limitations | Outcomes |
|---|---|---|---|
| Neurovertebral Decompression | Moderate hernia without severe neurological signs | Limited efficacy with massive hernias or cauda equina syndrome | Gradual symptom improvement, not guaranteed cure |
| Medication/Injections | Acute inflammation and pain | Temporary relief, potential side effects | Symptom control, non-curative |
| Minimally Invasive Surgery | Pain refractory to conservative therapies | Risks from anesthesia and scar tissue | Rapid relief, variable recovery |
Patients should approach treatment decisions with realistic expectations, recognizing that pain management often requires adaptive, stepwise strategies and the guidance of experienced caregivers. For detailed patient stories and outcome narratives within Quebec, visit real-life recovery stories that illustrate diverse journeys.
Rehabilitation After Neurovertebral Decompression: Exercises and Lifestyle Adaptations in Rosemont–La Petite-Patrie
Post-treatment rehabilitation is crucial for consolidating gains achieved through decompression therapy. Targeted exercises strengthen spinal musculature, enhance flexibility, and promote better posture, all critical to reducing recurrence risk.
Key rehabilitation components include:
- Strengthening the core and paraspinal muscles to stabilize and support vertebral structures
- Gentle stretching routines to maintain spinal flexibility and reduce stiffness
- Postural corrections based on individual lifestyle and work habits
- Encouraging regular, moderate physical activity to sustain spinal health
| Exercise Type | Benefit | Recommended Frequency |
|---|---|---|
| Muscle Strengthening | Enhanced spinal stability and support | 3-5 times per week |
| Stretching | Reduced stiffness, improved mobility | Daily |
| Movement Mobilization | Prevents rigidity and fosters adaptation | Regularly |
Successful recovery stories in the region affirm that consistent commitment to rehabilitation significantly improves quality of life. Expert supervision and patient education, such as those offered by Dr. Desforges at TAGMED Clinic resources, empower patients during and beyond therapy.

The Socio-Psychological Impact of Back Pain in Rosemont–La Petite-Patrie: Voices and Realities
Back pain, especially when chronic, imposes substantial burdens on daily living, affecting sleep, emotional well-being, and social participation. Residents of Rosemont–La Petite-Patrie frequently recount how persistent pain altered work performance and social interactions. Addressing these challenges requires an empathetic approach that combines therapeutic intervention with psychological support.
Effective management strategies include:
- Medical and rehabilitative treatment to reduce pain intensity
- Education to mitigate anxiety and correct misconceptions about spinal health
- Psychological counseling where needed to prevent chronic pain syndromes
- Community support groups for shared experiences and encouragement
| Influencing Factor | Potential Impact | Recommended Interventions |
|---|---|---|
| Pain Intensity | Activity limitation, fatigue | Medical management, neurovertebral decompression |
| Psychological Perception | Anxiety, increased stress | Therapeutic education, counseling |
| Social Support | Isolation, possible depression | Support groups, community engagement |
The perspectives offered by Dr. Sylvain Desforges emphasize positive communication and reassurance as vital components to empowering patients and promoting recovery. The journey to wellness is as much psychological as it is physical.
The dynamic neighborhood of Mercier–Hochelaga-Maisonneuve has seen a significant rise in cases of herniated disc-related back pain, with many residents facing chronic discomfort that interferes with work and daily activities. This ailment, which involves displacement or protrusion of spinal discs,…
Future Trends in Herniated Disc Management in Rosemont–La Petite-Patrie
Medical innovation continually reshapes the landscape of herniated disc treatment. In 2025, emerging technologies such as dynamic spinal implants like TOPS and Intraspine aim to stabilize without fusion, preserving natural vertebral motion. Telemedicine’s integration facilitates patient follow-up and expands access to expert consultation beyond local boundaries, as championed by pioneering Canadian clinics.
Furthermore, protocols combining targeted osteopathic care and neurovertebral decompression continue setting higher standards for efficacy and patient satisfaction. Emphasizing education and physical activity, these advancements complement a holistic model focused on preventing recurrence and enhancing quality of life.
| Innovative Approach | Expected Benefit | Current Status |
|---|---|---|
| Dynamic Implants (TOPS, Intraspine) | Motion preservation and vertebral stabilization | Clinical trials and development |
| Telemedicine Follow-Up | Improved accessibility and ongoing monitoring | Implemented in select clinics |
| Combined Osteopathic-Decompression Protocol | Enhanced long-term relief and prevention | Standard practice in advanced centers |
Patients in Rosemont–La Petite-Patrie and beyond can look forward to increasingly personalized spinal care, driven by research, technology, and multidisciplinary collaboration. Visit SOS Herniated Disc for ongoing updates and expert analyses.
Is neurovertebral decompression therapy painful?
Most patients find neurovertebral decompression therapy comfortable and non-painful due to precise positioning and controlled traction forces tailored to the individual.
How many sessions of decompression therapy are generally required to see improvement?
Typically, a treatment protocol of 10 to 20 sessions over several weeks is recommended. Results depend on the herniation’s severity and patient adherence.
Can neurovertebral decompression be combined with other treatments?
Yes, it is common practice to combine decompression with osteopathy, physiotherapy, and sometimes medication to enhance overall outcomes.
When does surgery become necessary for a herniated disc?
Surgery is considered a last resort, mainly reserved for patients with severe neurological symptoms or when conservative treatments fail to provide relief.
How can I prevent recurrence after treatment?
Maintaining good posture, continuing strengthening exercises, and managing body weight are crucial to minimizing the risk of herniated disc recurrence.