
Rehabilitation and Returning to Work: Insights from an Expert
November 16, 2025
Hospitals and Surgeon Partnerships: Key Insights, Benefits, and Challenges
November 16, 2025The journey toward considering back surgery is often complex and requires careful evaluation of numerous factors to determine suitability. For patients grappling with spinal conditions, especially in regions where healthcare systems might experience significant wait times, exploring international treatment options has become increasingly viable. This guide provides an in-depth look at the multifaceted eligibility criteria that govern access to back surgery, highlighting how collaborative expert networks and advanced surgical techniques are redefining patient care. In particular, cross-border partnerships between healthcare providers from Quebec and France have been instrumental in facilitating timely and specialized spine surgeries, making cutting-edge interventions more accessible than ever. The role of meticulous patient selection, encompassing medical, psychological, and logistical considerations, emerges as a pivotal theme in ensuring successful outcomes and sustained recovery.
Alongside the clinical evaluation, the psychological readiness and support systems of patients come under scrutiny, reflecting a more holistic approach to spinal care. The integration of state-of-the-art technologies, ranging from minimally invasive endoscopic procedures to innovative dynamic stabilization implants, underscores the rapid evolution in surgical methods available today. Navigating the eligibility landscape demands not only understanding these advancements but also appreciating the organizational frameworks that underpin international surgical pathways. This guide serves as a comprehensive resource for patients, caregivers, and healthcare professionals alike, shedding light on the critical factors that influence access to back surgery and the nuances of individualized treatment planning.
Fundamental Medical Eligibility Criteria for Back Surgery: An Analytical Perspective
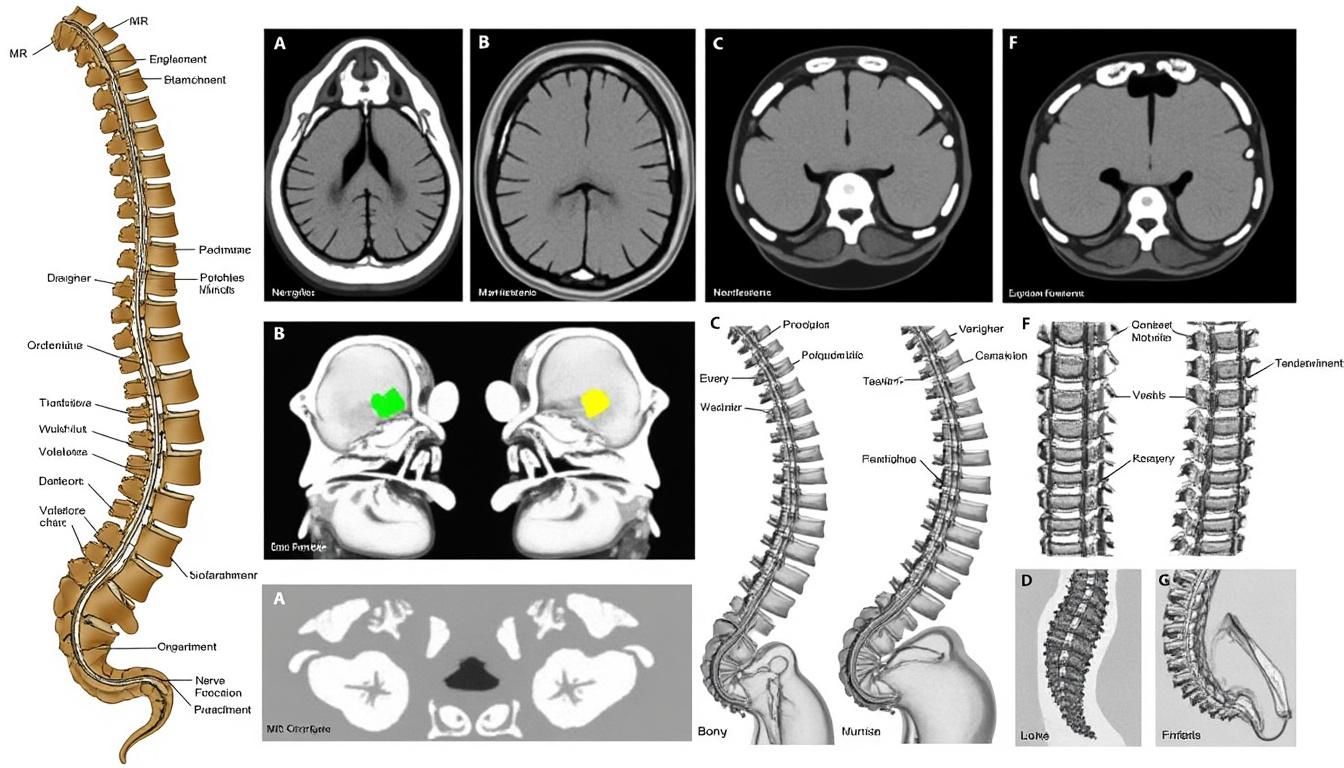
Determining medical eligibility for back surgery involves a thorough evaluation designed to ascertain whether surgical intervention will yield benefits that outweigh associated risks. This assessment is grounded in a detailed review of the patient’s spinal pathology, symptom severity, and prior treatment responses. For example, imaging techniques such as MRI and CT scans play an essential role in confirming diagnoses ranging from herniated discs to spinal canal stenosis or complex deformities like scoliosis and spondylolisthesis. These diagnostic insights inform the surgical approach, whether it be decompression, fusion, or dynamic stabilization.
- Pathology Type: Identification of specific spinal disorders is crucial, as herniated discs and spinal stenosis might warrant different surgical protocols than instability or deformity-induced pain.
- Treatment Failure: Surgery is often considered when conservative treatments such as physical therapy, medications, or injections fail to provide lasting relief over a defined period.
- Functional Impairment: Evaluating the extent to which pain restricts mobility and daily activities helps determine the urgency and necessity of surgical intervention.
- General Health Assessment: Patient comorbidities, anesthesia tolerance, and overall physical condition significantly impact surgical risk and recovery prospects.
- Radiological Evidence: Confirmed findings like nerve compression, disc degeneration, or vertebral instability guide decision-making.
For instance, a patient with a disabling lumbar herniated disc failing to respond to non-surgical decompression might be a strong candidate for a minimally invasive discectomy. Contrastingly, a patient presenting with marked vertebral instability and scoliosis could necessitate an arthrodesis procedure to stabilize and realign the spine. The balance between invasiveness and expected efficacy is central to this decision-making process.
| Eligibility Factor | Criteria or Threshold | Clinical Relevance |
|---|---|---|
| Definitive Pathology | Nerve compression, disc degeneration, vertebral instability | Determines surgical intervention type |
| General Health | Absence of severe comorbidities | Reduces anesthesia and postoperative risks |
| Functional Impact | Significant movement limitation and intense pain | Justifies surgical recommendation |
| Age Considerations | Age-appropriate protocols for recovery | Influences surgical technique choice |
Consulting contemporary resources such as the Comprehensive guide to spine surgery procedures and techniques further emphasizes the importance of tailored interventions based on detailed medical profiling. In clinical practice, aligning diagnosis with patient health and functional needs ensures not only safety but also the optimization of surgical outcomes within frameworks like those described in Selection Criteria 2025 for spine surgery.

Can Rehabilitation and Return to Work Prevent the Need for Surgery?
In the constantly evolving landscape of spinal healthcare, patients and practitioners alike grapple with a pivotal question: can the rigorous pathways of rehabilitation and structured return to work reduce or even eliminate the need for surgical intervention? The answer, as…
Psychological Assessment: A Crucial Dimension in Evaluating Surgery Suitability
The interplay between psychological factors and surgical success has become increasingly acknowledged as a critical element in back surgery candidacy. The patient’s mental preparedness, motivation for rehabilitation, and emotional stability profoundly influence postoperative recovery trajectories and long-term satisfaction. Psychological evaluation complements the medical assessment by identifying potential barriers such as unrealistic expectations, anxiety, or inadequate social support.
- Patient Motivation: A critical driver in adherence to postoperative rehabilitation protocols and lifestyle adjustments.
- Emotional Stability: Ensures resilience in navigating postoperative challenges and reduces psychosomatic complications.
- Expectation Management: Aligning patient hopes with realistic surgical outcomes fosters trust and engagement.
- Support Systems: Family or social support often correlates with improved recovery outcomes and compliance.
- Psychological Screening: Early identification of psychiatric conditions may warrant preoperative interventions to optimize candidacy.
In practical terms, multidisciplinary teams, such as those involving specialists at TAGMED, conduct interviews and assessments to guide the surgical decision process. For example, a patient exhibiting high motivation and stable emotional health is more likely to engage effectively in postoperative physical therapy, crucial for success after complex spine surgeries. Conversely, patients flagged for potential mental health challenges may benefit from tailored psychological support to improve their readiness.
| Psychological Factor | Impact on Eligibility | Recommended Approach |
|---|---|---|
| Motivation | Determines adherence to recovery protocols | Personalized counseling and goal-setting |
| Emotional Stability | Reduces risk of postoperative psychological complications | Psychological support or therapy referrals |
| Expectation Realism | Influences patient satisfaction | Clear communication about surgical outcomes |
| Social Support | Enhances rehabilitation success | Engagement of family or caregivers |
This comprehensive psychological screening process is integral to the high standards of patient care observed in international collaborative models, including preoperative and postoperative services coordinated by experienced teams. Additionally, understanding the psychological dynamics helps optimize resource allocation and improve recovery rates, as discussed in detailed reviews such as Understanding the eligibility criteria for back surgery.

Exploring the Overlooked Benefits of Spine Surgery in France
Spinal disorders are a significant health concern for many patients worldwide, yet the solutions and benefits of spine surgery often remain underappreciated. France, with its advanced healthcare infrastructure and pioneering surgical techniques, has emerged as a noteworthy destination for patients…
Comprehensive International Patient Pathways for Spine Surgery: Coordination and Continuity
International spine surgery programs have carved out specialized pathways that orchestrate the patient journey from initial evaluation to postoperative recovery with precision and patient-centered focus. For individuals from Quebec considering surgery in France, these pathways streamline the complexities usually associated with cross-border medical care, ensuring safety and efficiency.
- Initial Assessment: Conducted in Quebec by specialists such as Dr. Sylvain Desforges and the TAGMED team focusing on confirming diagnosis and administering specialized conservative treatments.
- Surgical Planning: Collaboration with French providers through organizations like Franchir to select surgeons, facilities, and coordinate travel and accommodations.
- Surgical Intervention: Performed at cutting-edge French centers known for their proficiency in spine surgery and innovative implants.
- Postoperative Follow-up: Returned care coordinated by Neurothérapie Montréal, including personalized rehabilitation and neurological assessments.
- Ongoing Support: Psychological and physical monitoring to ensure sustained recovery.
The advantages of such integration include a significant reduction in waiting times and administrative hurdles common in traditional healthcare systems. The collaborative framework between SOS Tourisme Médical and partner clinics represents an exemplary model of international healthcare delivery.
| Care Phase | Responsible Partner | Core Activities |
|---|---|---|
| Initial Evaluation | Dr. Sylvain Desforges / TAGMED | Diagnosis validation and conservative treatment supervision |
| Surgical Coordination | Franchir | Surgeon selection, logistics, travel, and accommodation planning |
| Operative Phase | French Surgical Centers | State-of-the-art surgical intervention with advanced implants |
| Postoperative Care | Neurothérapie Montréal | Rehabilitation and neurological follow-up |
Models like this emphasize the necessity of multidisciplinary collaboration and exemplify how integrated international approaches can improve patient satisfaction and clinical results. Institutions involved maintain rigorous standards without breaching regulatory protocols, ensuring patient safety and therapeutic efficacy. Further insights on organized healthcare pathways for spine surgery can be found in resources such as Spinal surgery in France as a central component of the care pathway.

Cousin Spine Technology and Franchir: Transforming Surgical Decision-Making
In recent years, the integration of advanced medical technologies has dramatically shifted how spinal surgeries are planned, performed, and managed. Among the transformative developments, the alliance between Cousin Spine Technology and Franchir stands out as a pioneering force redefining surgical…
Advanced Surgical Techniques in France and Matching Eligibility Factors
France leads the way in spinal surgery by offering patients access to sophisticated surgical techniques that minimize invasiveness while maximizing recovery prospects. Integrating these advanced options into patient care mandates precise eligibility screening to ensure appropriateness and optimize outcomes.
- Minimally Invasive Endoscopic Surgery: Utilizes high-definition video guidance to minimize soft tissue trauma, yielding quicker recovery and reduced postoperative pain.
- Instrumented Fusion (Arthrodesis): Suitable for patients with significant spinal instability or deformity, securing spinal segments while acknowledging the trade-off in segmental mobility.
- Motion Preservation Implants: Devices like the TOPS and LP-ESP systems aim to maintain spinal segment motion post-surgery, offering an alternative to fusion in select patients.
- Intervertebral Disc Prostheses: Recommended for younger patients with localized disc degeneration, preserving joint function and delaying adjacent segment deterioration.
Successful integration of these technologies with patient-specific pathology enhances satisfaction. Criteria such as spinal segmental stability, prior treatment history, and patient age guide selection. For patients interested in innovative surgery, the minimally invasive surgery options in Quebec offer complementary insights into procedure efficacy and biomechanical preservation.
| Surgical Technique | Main Indications | Key Advantages | Limitations |
|---|---|---|---|
| Minimally Invasive Surgery | Herniated disc, mild stenosis | Reduced pain, smaller scars, faster recovery | Not suitable for complex cases |
| Arthrodesis (Fusion) | Instability, severe deformities | Secure stabilization | Loss of segmental motion |
| Motion Preservation (TOPS, LP-ESP) | Moderate instability requiring mobility maintenance | Preserves joint function, reduces adjacent wear | Strict selection criteria, relative novelty |
| Disc Prosthesis | Young patients with localized degeneration | Maintains range of motion | Less suited for older patients |

Insights from Research on Preventing Post-Laminectomy Syndrome
Post-Laminectomy Syndrome (PLS), a chronic pain condition arising after spinal surgery, remains a formidable challenge in spinal surgery and pain management. Despite advances in surgical techniques, a significant subset of patients continues to experience persistent neuropathic pain and functional limitations,…
Integration of Clinical Guidelines and Insurance Protocols in Eligibility Assessment
Eligibility for back surgery is also shaped by standardized clinical guidelines and insurance policies that aim to ensure patient safety and cost-effective care. Authorities such as Cigna and Blue Shield have developed comprehensive criteria to assist practitioners and reviewers in determining medical necessity and appropriateness of surgical interventions.
- Medical Necessity Guidelines: Clearly define conditions and indications suitable for surgery after failed conservative therapy.
- Imaging and Diagnostic Requirements: Specify the type and timing of imaging studies required to substantiate surgical candidacy.
- Outcome-Based Metrics: Institutions emphasize postoperative outcomes and complication rates to validate patient selection protocols.
- Rehabilitation Expectations: Guidelines highlight the necessity of patient willingness to participate in postoperative rehabilitation.
- Insurance Coverage Policies: Define eligibility in relation to approved surgical types and established evidence.
For providers and patients navigating the complex terrain of healthcare, references such as the Cigna Preface to Spine Surgery Guidelines and the Spine Surgery Appropriate Use Criteria provide practical frameworks for decision-making. Moreover, coverage outlines detailed in Medicare coverage navigation for spine surgery assist patients in understanding their benefits and out-of-pocket expectations.
| Guideline Component | Purpose | Application in Eligibility |
|---|---|---|
| Indication Clarity | Define surgical necessity after conservative treatment failure | Screens patients for appropriateness and timing |
| Imaging Protocols | Standardize required diagnostics | Ensure evidence-based candidacy evaluation |
| Outcome Monitoring | Validate surgical impact and safety | Refines patient selection criteria |
| Rehabilitation Commitment | Assess patient willingness to engage in postoperative care | Influences eligibility decisions |
| Insurance Coverage Rules | Define policy-covered procedures | Aligns clinical decisions with benefit plans |
These integrated systems of clinical and insurance standards serve as a backbone to the SpineCare Solutions framework, which is designed to optimize patient outcomes while maintaining strict adherence to evidence-based practices.

International Comparison: Spotlight on Spine Care Practices Between France and Quebec
The growing emphasis on spine health in Quebec has spotlighted the value of international collaboration in advancing patient care. With the challenges of prolonged wait times and high private care costs in Quebec, France emerges as an attractive alternative, boasting…
Addressing Common Barriers and Contraindications in Back Surgery Eligibility
Despite advances, certain barriers and contraindications limit candidacy for back surgery. These include both medical and systemic factors that must be thoroughly assessed prior to proceeding with surgery to avoid adverse outcomes.
- Active Infections: Patients with ongoing infections pose high risk for surgical complications and are usually deferred until resolution.
- Unstable Medical Conditions: Severe comorbidities such as poorly controlled diabetes, cardiovascular disease, or metabolic disorders may preclude surgery.
- Psychosocial Barriers: Lack of adequate social support or unresolved psychological conditions may impair recovery.
- Non-Compliance Risks: Patients unwilling to commit to the postoperative rehabilitation regimen may be ineligible.
- Structural Limitations: Certain anatomical features or previous surgeries could affect feasibility or success of intervention.
Systematic preoperative screening is critical to identify these risks early. Facilities specialized in spine surgery, like the Center d’Excellence Chirurgie du Dos, implement stringent protocols to mitigate these factors. Understanding these limitations is vital for comprehensive informed consent.
| Contraindication | Rationale | Potential Impact |
|---|---|---|
| Active Infection | Risk of wound contamination and systemic spread | Surgery delay or cancellation |
| Unstable Comorbidities | Increased perioperative morbidity and mortality | Ineligible or need for stabilization first |
| Psychological Barriers | Increased risk of poor postoperative outcomes | Require preoperative psychological intervention |
| Non-Compliance | Higher chance of surgical failure or complications | Exclusion from surgery unless addressed |
| Anatomical Constraints | May complicate or prevent surgical access | Selective surgical candidacy |
Exploring educational materials like Understanding back surgery eligibility: a clear guide for patients in Quebec can bolster patient awareness of these limitations and encourage proactive engagement in the assessment process.

Medical Logistics and Accommodation: Central Pillars in the Patient Care Journey
In the evolving landscape of global healthcare, the interplay between medical logistics and patient accommodation has become a cornerstone for effective and patient-centric care delivery. This synergy is particularly evident in the management of international patient journeys, where cross-border coordination,…
Technological Innovations Elevating the Standard of Spine Surgery Eligibility
Technological progress in spine care is significantly influencing eligibility criteria, expanding the scope for minimally invasive and biomechanically friendly surgical options. Modern tools such as robotic navigation systems, 3D imaging, and dynamic implants afford surgeons unparalleled precision and tailored treatment plans.
- Robotic-Assisted Surgery: Improves accuracy in implant placement and reduces operative time.
- 3D Imaging and Modeling: Enables dynamic visualization of spinal pathology and aids preoperative planning.
- Dynamic Stabilization Devices: Permit preservation of normal motion, offering alternatives to traditional fusion.
- Endoscopic Techniques: Minimize tissue trauma and enhance recovery speed.
- Biomaterials and Custom Implants: Facilitate better integration and durability of surgical constructs.
For example, platforms such as eCential Robotics furnish surgeons with robotic navigation capabilities that are FDA-approved and increasingly integrated into leading French surgical centers. This integration is reflected in improved patient stratification and surgical outcomes, supporting the evolving framework of spine surgery innovation with 3D imaging and robotic navigation.
| Technology | Benefits | Impact on Eligibility |
|---|---|---|
| Robotic Navigation | Enhanced precision and reduced complications | Broadens candidacy, especially for complex cases |
| 3D Imaging | Improved preoperative planning | Refines patient selection accuracy |
| Dynamic Implants | Preserves movement, decreases adjacent segment degeneration | Suitable for younger or moderate instability cases |
| Endoscopic Surgery | Less invasive, quicker recovery | Eligibility expansion for earlier intervention |
| Custom Biomaterials | Better integration and durability | Improves long-term success rates |

Comprehensive Guide to Eligibility Criteria for Back Surgery
The decision to undergo back surgery involves numerous complex considerations that extend beyond the presence of spinal discomfort. Through an international collaboration between healthcare experts in Quebec and France, patients facing severe spine conditions now have access to advanced surgical…
Patient Case Studies Illustrating the Application of Eligibility Criteria
Clinical case studies provide concrete illustrations of how multidisciplinary evaluations apply eligibility criteria in real-world contexts. Consider a patient with chronic radiculopathy linked to a lumbar disc herniation. Despite extensive conservative management, symptoms persist, and imaging confirms nerve root compression. This patient undergoes psychological screening confirming readiness and displays robust social support. After comprehensive assessment coordination between Quebec and French centers, a minimally invasive endoscopic discectomy is performed, followed by a structured rehabilitation program, yielding significant symptom relief and functional restoration.
- Case 1: Middle-aged adult with lumbar herniated disc, eligible for minimally invasive surgery after failed conservative care and positive psychological evaluation.
- Case 2: Elderly patient with scoliosis and vertebral instability, requiring spinal fusion with preoperative optimization of comorbidities.
- Case 3: Younger patient with localized disc degeneration, suitable for disc replacement prosthesis and dynamic implant strategies.
- Case 4: Patient with moderate spinal instability addressed with motion preservation hardware following detailed eligibility confirmation.
- Case 5: Complex patient requiring coordination between multidisciplinary teams to manage psychosocial and medical risk factors concurrently.
These case scenarios exemplify the nuanced decision-making process integral to BackSurgery Navigator platforms, which provide personalized guidance by integrating clinical, psychological, and logistical data to optimize patient outcomes. The success stories and patient insights found in resources like Spinal surgery in France – personal stories and patient insights underscore the pivotal role of eligibility criteria in shaping treatment pathways.
Back Surgery Eligibility Quiz
Welcome to this interactive quiz designed to help you understand some of the eligibility criteria and key concepts related to back surgery. Test your knowledge and explore additional tools to make informed decisions.
Back Surgery Risk Calculator
Estimate your potential risk factors for back surgery based on simple health criteria.
Common Back Surgery Contraindications
Graph showing frequency (simulated data) of common contraindications affecting eligibility.
Did You Know? Medical Fact from Public API
A random medical fact to enrich your knowledge.
Loading fact…
Which examinations are necessary to verify back surgery eligibility?
A comprehensive clinical assessment inclusive of detailed questionnaires and imaging studies such as MRI or CT scans is essential. Coordinated efforts led by specialists like Dr. Sylvain Desforges at TAGMED ensure targeted evaluation to guide surgical decision-making.
How can a patient qualify for dynamic surgical implants like the TOPS system?
Eligibility depends on spinal stability and individual clinical profiles. Neurothérapie Montréal plays a key role in monitoring patient suitability before referring to surgery for such advanced implant procedures.
Is postoperative care received in Quebec after surgery in France?
Yes, Neurothérapie Montréal provides personalized ongoing postoperative rehabilitation and neurological follow-up, ensuring continuity of care and optimal recovery.
What is the typical duration from initial evaluation to surgery?
Thanks to optimized coordination by Franchir and SOS Tourisme Médical, the timeframe from evaluation to operation is markedly shorter compared to conventional waits in Quebec, typically spanning a few months.
What are the common contraindications to back surgery?
Patients with significant medical conditions, unresolved metabolic disorders, or active infections are generally contraindicated; early identification of these factors through thorough evaluation is critical to patient safety.

Unveiling the Hidden Benefits of Neurovertebral Decompression Therapy
Chronic back and neck pain remain pervasive health issues impacting millions, often leading to debilitating effects on daily life and overall well-being. Traditional management strategies frequently fall short due to lengthy wait times, high costs, or invasive procedures. Amid this…




